International Journal of Dermatology and Clinical Research
Clinical features of Rheumatoid Purpura in adults
El Arabi Yasmina1*, Hali F1, Marnissi F2 and Chiheb S1
2Anatomopathology Department, Ibn Rochd University Hospital Center, Casablanca, Morocco
Cite this as
Yasmina EA, Hali F, Marnissi F, Chiheb S (2022) Clinical features of Rheumatoid Purpura in adults. Int J Dermatol Clin Res 8(1): 001-004. DOI: 10.17352/2455-8605.000042Copyright
© 2022 Yasmina EA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Introduction: Rheumatoid purpura is a systemic vasculitis of small vessels that is more common in children than in adults. The aim of our study was to revise the characteristics of rheumatoid purpura in adults.
Methods: We conducted a retrospective descriptive and analytical study [June 2016 - June 2021], including all the patients hospitalized in the dermatology department of Ibn Rochd University Hospital for rheumatoid purpura. We first described the characteristics of adult patients aged over 18 years old, and then we compared them to those of the children (<18 years old) to determine the clinical features in adults.
Results: A total of 18 adults (15 women/3 Men) and 9 children were collected. Adults had a mean age of 48 years [27-66 years]. Vascular purpura was constant, complicated by necrosis in 12 patients, bullae in 6 patients, and ulceration in 2 patients. Joint involvement was present in 16 patients. Ten patients presented digestive signs: epigastralgia (n= 4), abdominal pain (n= 8), and rectal bleeding (n= 2). Cutaneous biopsy showed leukocytoclastic vasculitis in all patients with IgA and C3 deposition in 13 patients. Renal involvement was present in 6 patients. After comparison with the children group, the particularities in adults were the absence of previous drug intake (p= 0.009), absence of pruritus (p= 0.009), presence of bullae (p= 0.05), presence of severe digestive involvement (p= 0.033), joint involvement (p= 0.003), and presence of anemia (p= 0.017).
Conclusion: Rheumatoid purpura in adults is characterized by its severe clinical features.
Introduction
Rheumatoid purpura is a systemic vasculitis of small vessels that is more common in children than in adults [1]. It is due to the formation of a high level of serum Immunoglobulins A(IgA) then the deposition of circulating immune complexes on the small vessels. This IgA formation could be triggered by several factors (viral and bacterial agents, vaccination, tumor cells). The clinical manifestations concern the skin, joints, kidneys, gastrointestinal tract, and lungs. The disease in children is usually mild but may have many adverse consequences in adults [2]. The aim of our study was to revise the characteristics of rheumatoid purpura in adults.
Materials & methods
Study design and setting
This is a retrospective descriptive and analytical case series study, carried out over a period of five years [June 2016-June 2021], in the Dermatology Department of Ibn Rochd University Hospital of Casablanca.
Study population
Inclusion criteria: We included all the patients hospitalized in the dermatology department for rheumatoid purpura. The diagnosis is based on the EULAR/ PRINTO/PRES classification criteria for rheumatoid purpura, which combines the presence of vascular purpura with at least one of the following signs: abdominal pain, presence of IgA on histology, arthritis, arthralgia, or renal involvement [3]. We first described the characteristics of adult patients aged over 18 years old, and then we compared them to those of the children aged under 18 years old to determine the clinical features in adults.
Exclusion criteria: Patients with incomplete data and those whose final diagnosis wasn’t rheumatoid purpura vasculitis were excluded from the study.
Data collection
Data were collected from the medical records of the patients using an analysis grid. The data collected were: age, gender, the month of hospitalization, known diseases, a previous drug intake or infectious episode, clinical features, paraclinical exams, therapeutic, and evolution.
Statistical analysis
Statistical analysis was performed using SPSS 20 software. Quantitative variables were expressed as means and qualitative variables as frequencies. We used the Chi-2 test for categorical variables. The significance level was set at a p less than 0.05.
Results
A total of 18 adults (15 women/3 Men) and 9 children were collected. The mean age in adults was 48 years [27-66 years]. The annual incidence was 3.6 cases per year with a predilection for winter. Two patients were smokers. No one was known to have neoplasia or an autoimmune disease. Four adults had infectious signs before the onset of symptoms, while no drug use was reported.
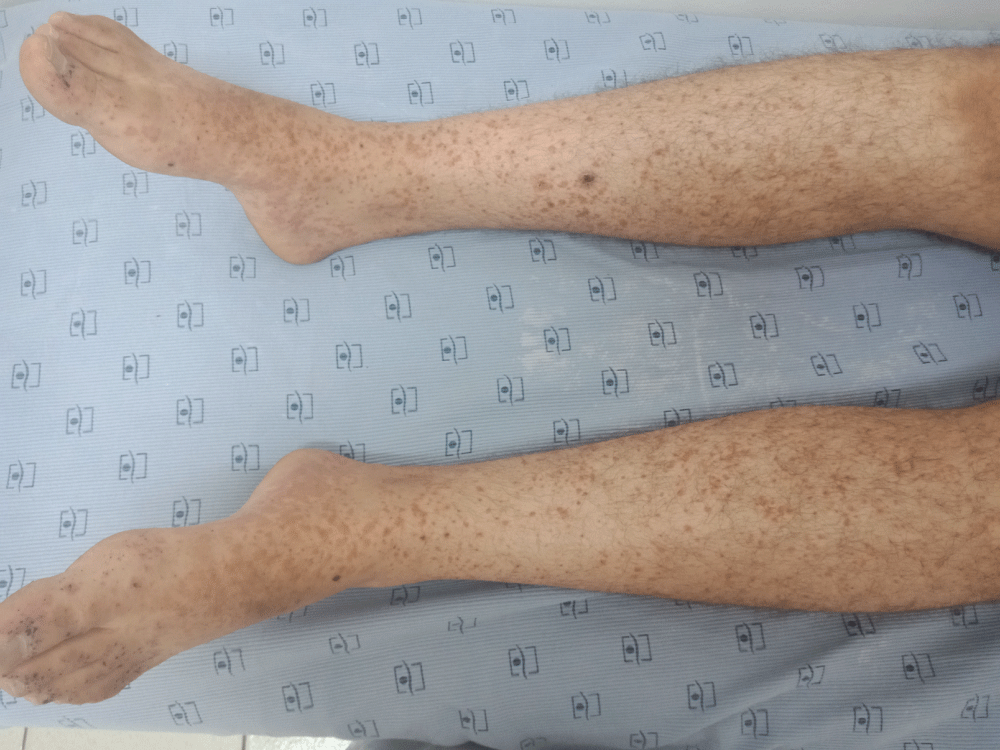
Vascular purpura was constant, complicated by necrosis in 12 patients, bullae in 6 patients, and ulceration in 2 patients (Figure 1). The purpura was located in the extremities in 14 patients and extensive in 4 patients. Two patients presented general signs (fever and asthenia). Sixteen patients had inflammatory polyarthralgia, and eight patients presented edema of the lower limbs. Digestive symptoms were present in 10 patients, including epigastralgia (n= 4), abdominal pain (n= 8), and rectal hemorrhage (n= 2).
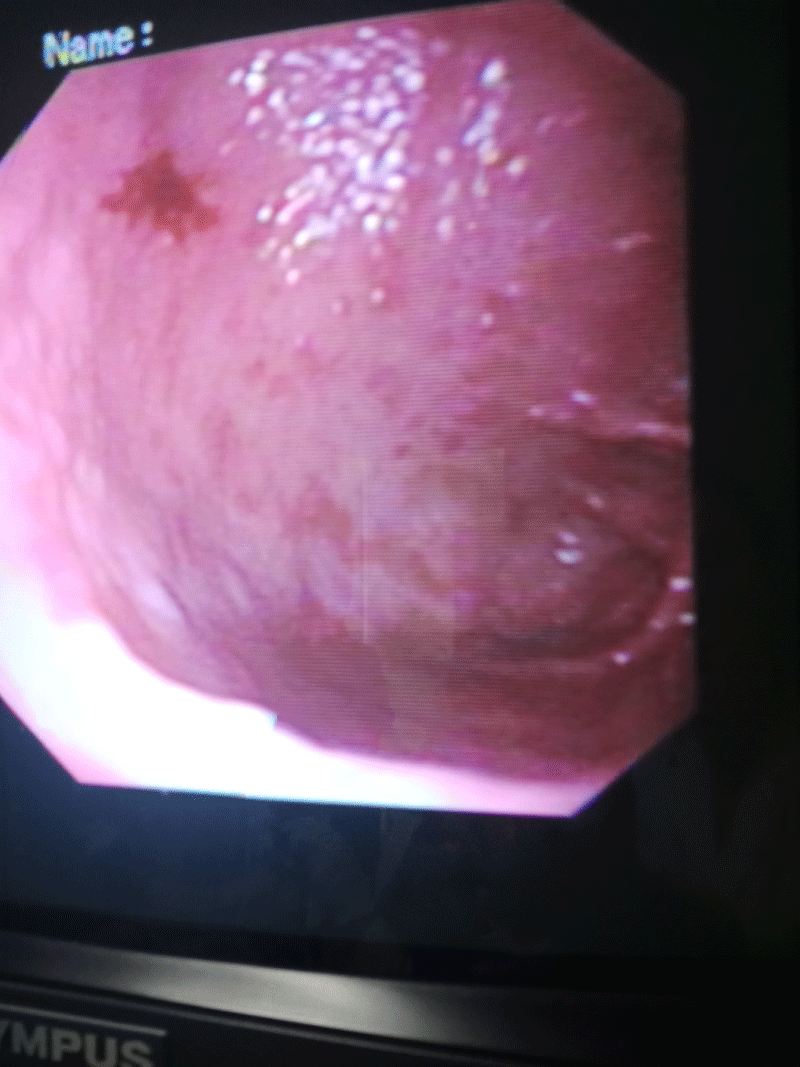
Biology showed anemia (n= 8), neutrophilic leukocytosis (n= 4), or an inflammatory syndrome (n= 18). Cutaneous biopsy showed leukocytoclastic vasculitis in all the patients with IgA and C3 deposition in 13 patients. Abdominal computed tomography showed infiltration of the intestinal wall in 3 patients. Digestive endoscopy showed purpuric lesions of the digestive mucosa in 4 patients with severe digestive symptoms: rectal bleeding and abdominal pain resistant to analgesic treatment (Figure 2). Renal involvement was observed in 6 adults, revealed by positive 24-hour urine protein [0.49-4g/24h], associated with microscopic hematuria and renal failure in two patients. Renal biopsy was indicated in 2 patients and showed diffuse endocapillary proliferative glomerulonephritis with IgA deposition.
Treatment was based on colchicine and vitamin C in all the patients. Oral corticotherapy was indicated in 8 patients due to visceral involvement, and a bolus of methylprednisolone in 4 patients due to severe digestive signs (n= 2) or nephrotic proteinuria (n= 2). Patients also received analgesics and/or antispasmodics if indicated. The evolution was favorable in all our patients.
A comparison between the characteristics of adults and children hospitalized for rheumatoid purpura is represented in Table 1. The clinical particularities in adults were the absence of previous drug intake (p= 0.009), absence of pruritus (p= 0.009), presence of bullae (p= 0.05), presence of severe digestive involvement (p= 0.033), joint involvement (p= 0.003), and presence of anemia (p= 0.017).
Discussion
The particularity of our study is that it confirms the severity of the clinical features of rheumatoid purpura in adults. Indeed, purpura is often bullous and the systemic involvement is more severe. Our study was able to highlight the severity of the digestive and joint involvement. Nevertheless, we couldn’t highlight the renal involvement as it is commonly known, given the hospitalization of these patients in the nephrology department.
Only few studies have been interested in rheumatoid purpura in adults. It is characterized by its low incidence compared to children (1/1000000 versus 150-200/1000000) and by the severity of its clinical signs. The disease is more frequent in male patients, and its incidence increases in winter [4]. Our incidence is similar to that of Ben Abdelghani (14 cases) [5], Loukil (14 cases) [6] and Kupfer (17 cases) [7], which remain lower than those of Lasseur (40 cases) [8] and Van de Perre (85 cases) [9]. In our series, we note a female predominance contrary to what is known. The low prevalence of hospitalized children in our structure is due to their hospitalization in the pediatric department.
The pathophysiology of rheumatoid purpura is explained by an increased production of IgA that can be triggered by several microorganisms (viruses and bacteria) or by tumor antigens. These Immunoglobulins are deposited on small vessels in the skin, glomeruli, joints, and gastrointestinal tract, activating the alternative complement pathway. An inflammatory response is triggered by the production of the Vascular Endothelial Growth Factor, cytokines, and platelet-activating factors. These mediators increase capillary permeability and lead to endothelial destruction with neutrophil migration. In the presence of a triggering factor, IgA production in adults is higher than in children, which explains the severity of the clinical manifestations [10].
Digestive involvement is common in adults. Its incidence varies in the different series. It consists of moderate to severe spasmodic pain, sometimes associated with exteriorized hemorrhage, justifying an exploratory laparotomy revealing no abnormalities, or a digestive endoscopy showing purpuric lesions of the digestive mucosa. Joint manifestations are seen in 2/3 of cases: arthralgia of the knees and ankles rapidly resolving, or non-destructive synovitis. The frequency of renal involvement varies from 45 to 85% according to the series. Its low incidence in our study is justified by the hospitalization of these patients in the nephrology department. It often appears during the first month and conditions the long-term prognosis. Indeed, several cases of chronic renal failure have persisted after IgA vasculitis. Neurological, pulmonary, cardiac, or urogenital manifestations may rarely be observed [4].
Treatment is based on colchicine which has an anti-inflammatory action and decreases chemotaxis and the production of lysozymes and peroxides. Dapsone can also be used for its anti-inflammatory action which decreases cytokines, free radical synthesis, and cell migration. In case of visceral involvement, the use of prednisone (1 mg/kg/day) is indicated, or even a bolus of methylprednisolone in case of severe manifestations. Intravenous Immunoglobulins or Cyclophosphamide may be used in case of severe renal involvement. Rituximab is used in refractory forms [10].
The limitations of our study were its retrospective nature and thus the unavailability of some data, but also the small sample given the hospitalization of patients with rheumatoid purpura in the different hospital departments. A study including all the departments that can be involved (dermatology, internal medicine, gastroenterology, nephrology, pediatrics) would be desirable.
Conclusion
Our study confirmed the severity of the cutaneous, digestive, and joint involvement of rheumatoid purpura in adults compared to children. It should be thought of in the case of bullous or necrotic purpura in adults, especially if associated with digestive symptoms.
- Maritati F, Canzian A, Fenaroli P, Vaglio A (2020) Adult-onset IgA vasculitis (Henoch-Schönlein): Update on therapy. Presse Med 49: 104035. Link: https://bit.ly/3tYICQh
- Konieczniak K, Rekowski FW, Gladys A, Zugajb P, Rymarz A, et al. (2021) Schönlein-Henoch purpura - single-center, retrospective analysis of the diagnostic process, treatment and course in adults. Pol Merkur Lekarski 49: 99-102. Link: https://bit.ly/3KQRFcD
- Ozen S, Pistorio A, Iusan SM, Bakkaloglu A, Herlin T, et al. (2010) EULAR/ PRINTO/PRES criteria for Henoch-Schönlein purpura, childhood polyarteritis nodosa, childhood Wegener granulomatosis and childhood Takayasu arteritis: Ankara 2008, Part II: final classification criteria. Ann Rheum Dis 69: 798-806. Link: https://bit.ly/36mx3Ko
- Pillebout E (2018) Vascularite à IgA (purpura rhumatoïde) de l’adulte. Méd Intensive Réa 27: 291-299.
- Ben Abdelghani K, Maghrbi I, Ben Assi W, Boussetta N, Boubaker S, et al. (2008) Purpura rhumatoïde de l’adulte. À propos de 14 observations. Rev med int 29: 170-171. Link: https://bit.ly/3JgZGHH
- Loukil H, Snoussi M, Frikha F, Jallouli M, Damak C, et al. (2019) Purpura rhumatoïde de l’adulte dans le sud tunisien: une série de 14 cas. Pan Afr Med J 34: 107. Link: https://bit.ly/34M0pSf
- Kupfer I, Joly P, Courville P, Balguerie X, Jouen-Beades F, et al. (2000) Purpura rhumatoïde de l'adulte: évaluation de l'atteinte rénale à moyen terme. Ann dermatol venerol 127: 818. Link: https://bit.ly/3idmIDq
- Lasseur C, Rispal P, Combe C, Pellegrin JL, De Precigout V, et al. (1996) Purpura rhumatoïde de l'adulte. À propos de 40 observations. Rev Med Int 17: 381-389. Link: https://bit.ly/3w76ns9
- Van de Perre E, Jones RB, Jayne D (2021) IgA vasculitis (Henoch-Schönlein purpura): refractory and relapsing disease course in the adult population. Clin Kidney J 14: 1953-1960. Link: https://bit.ly/3tY8JqE
- Sugino H, Sawada Y, Nakamura M (2021) IgA Vasculitis: Etiology, Treatment, Biomarkers and Epigenetic Changes. Int J Mol Sci 22: 7538. Link: https://bit.ly/3CNaBq7
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
