Imaging Journal of Clinical and Medical Sciences
Cemento-ossifying fibroma
Rida Zainab1*, Imtiaz Ali1, Hina Naseer1, Muhammad Ayub Mansoor1, Aiza Sohail Khan2 and Asad Abbas Jafri3
2Department of Oral and Maxillofacial Surgery, Liaquat National Hospital, and Medical College, Karachi, Sindh, Pakistan
3Department of Histopathology, Liaquat National Hospital, and Medical College, Karachi, Sindh, Pakistan
Cite this as
Zainab R, Ali I, Naseer H, Mansoor MA, Khan AS, et al. (2022) Cemento-ossifying fibroma. Imaging J Clin Medical Sci 9(1): 007-010. DOI: 10.17352/2455-8702.000135Copyright License
© 2022 Zainab R, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Cemento-ossifying fibroma is a rare benign fibro-osseous neoplasm commonly involving the jaws majority of lesions occur in mandible bone. It can be discovered as an incidental finding in radiological imaging. Symptomatic patients are presented with a slowly growing mass involving the jaws commonly in mandible bone and can attain a large size with the passage of time. It can cause facial deformity if left untreated. We present such a case of Cemento-ossifying fibroma involving the right hemi-mandible bone, and its radiological imaging findings, including X-ray (OPG), CT scan, and Histopathology.
Introduction
Cemento-ossifying fibroma or ossifying and cementifying fibroma described as well defined sharply marginated or uncommonly encapsulated benign neoplasms [1-3]. These lesions are predominantly seen in between 2nd to 4th decades of life more commonly in women than men with ratio of (4:1) [4-7]. It consist of fibrous tissue with varying amount of mineralizing or calcified material resembling the bone, cementum or both [1-3]. This lesion is slowly progressive fibro-osseous neoplasm can be originated from bones of face and skull predominantly involving the mandible in molar-premolar region [1,3,4,7]. It is commonly discovered as incidental finding on radiological imaging and asymptomatic [2,3]. However in symptomatic patients it becomes large enough in size and can cause enlargement of the affected bone resulting in clinically apparent swelling of involved region, intra-oral hard mass and disfigurement of face with the passage of time [3,6]. Various investigation are used to diagnose the cemento-ossifying fibroma, these includes orthopantomography (OPG), CT scan, MRI and Histopathology [6,7]. Definitive diagnosis can be made correlation in between clinical history, radiological imaging findings and histopathology [5]. Treatment planning can be made on size, nature and site of lesion [5]. Recommended treatment option for cemento-ossifying fibroma is surgical resection of the lesion with enucleation and curettage of the involved bone [6]. The recurrence of these lesions after surgery is extremely rare [5,6]. Purpose of our case report is to elaborate on the radiological imaging findings of cemento-ossifying fibroma.
Case report
30 years old female presented in the outpatient department of oral and maxillofacial surgery with a complaint of painless swelling in the right lower jaw for 1 year. Initially swelling was small in size and non-palpable gradually increase in size and become clinically visible resulting in asymmetry of the face.
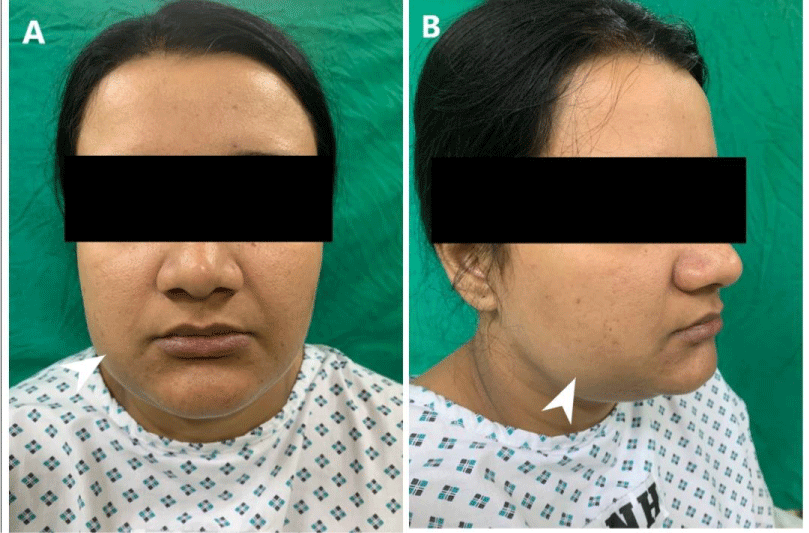
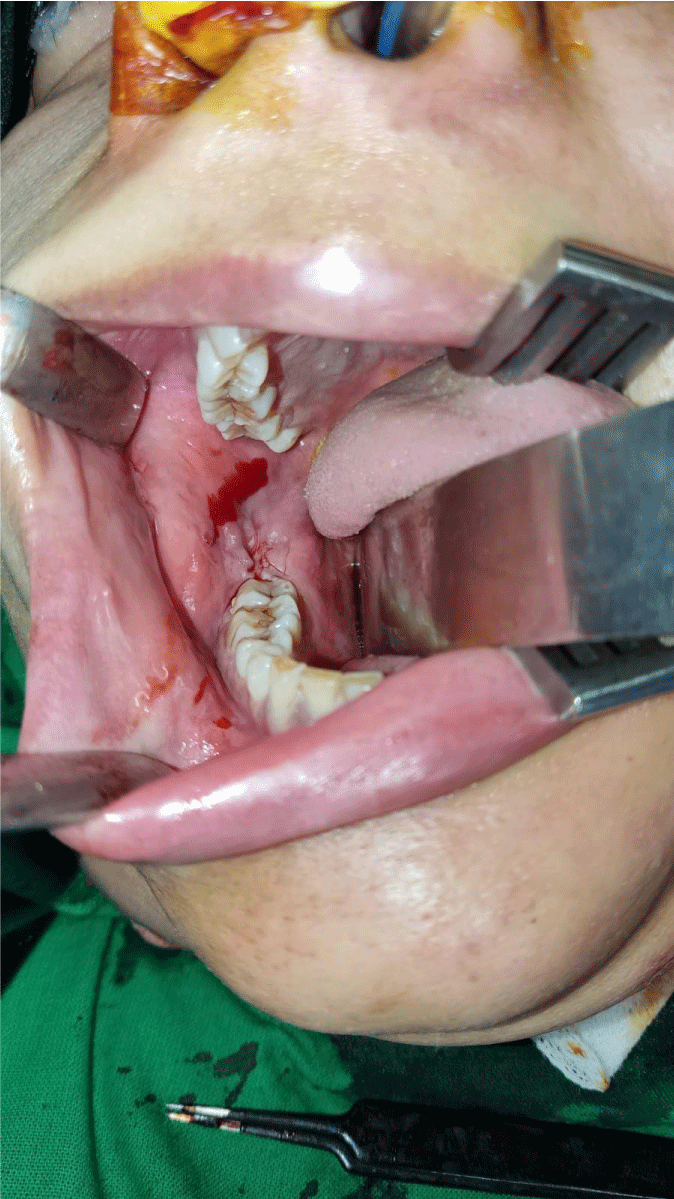
On examination, extra-orally a well-defined swelling on the right side of the face in the region of ramus and body of mandible resulting in facial asymmetry with normal smooth intact overlying skin (Figure 1). It measured about 6.0×4.3 cm hard in consistency and non-tender on palpation. There was no evidence of lymphadenopathy on either side of the neck. On intra-oral examination, there was a significant expansion of ramus and body of right mandible extending up to the right lower molar tooth causing obliteration of buccal vestibule with redness of overlying mucosa. There was no evidence of pussy discharge at the site of swelling (Figure 2).
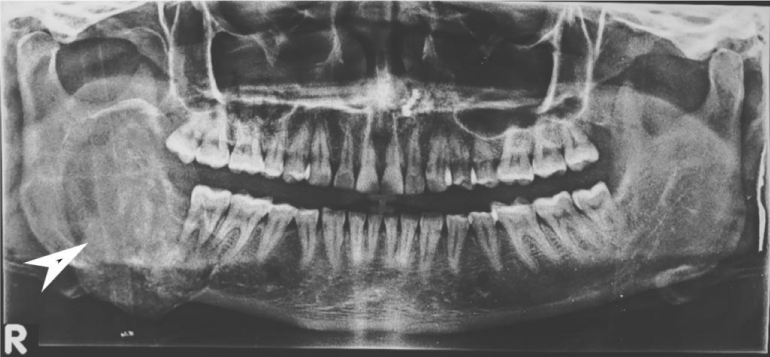
Orthopantomography (OPG) showed a large well-defined mixed density predominantly radiolucent lesion measuring 5.8 x 4.5 cm involving the ramus and body of right hemi-mandible causing their significant expansion reaching up to the root of the right lower molar tooth with no definite evidence of a cortical break. There was no evidence of dislocation, destruction, or erosion of the molar tooth. Few faint ill-defined radio-opaque areas were seen within the lesion representing intra-lesional calcific foci/ cementing material. This was reported as a Fibro-osseous lesion or ameloblastoma (Figure 3).
CT scan with contrast was recommended to elicit the extent of the lesion and to characterize the radiological features. It showed a large well corticated, sharply marginated mixed density expansile lesion involving the ramus and body of mandible reaching up to the root of the right lower molar tooth. There was no evidence of cortical break, destruction, or erosion of involved bone. Few intra-lesional hyperdense areas were seen representing calcific foci/ cementing material (Figures 4-6).
Based on all radiological imaging, a diagnosis of fibro-osseous lesion was made. Her baseline laboratory investigations were within the normal range and were non-contributory to our diagnosis.
The patient underwent the incisional biopsy of the most expansive part of the lesion under local anesthesia. Histopathological examination showed intra-osseous proliferation of spindle cells exhibiting hypercellular stroma with intervening cementum-like calcification. The spindle cells showed elongated hyperchromatic nuclei and eosinophilic cytoplasm. No atypia, necrosis, or mitosis was seen. Features were compatible with cemento-ossifying fibroma (Figure 7).
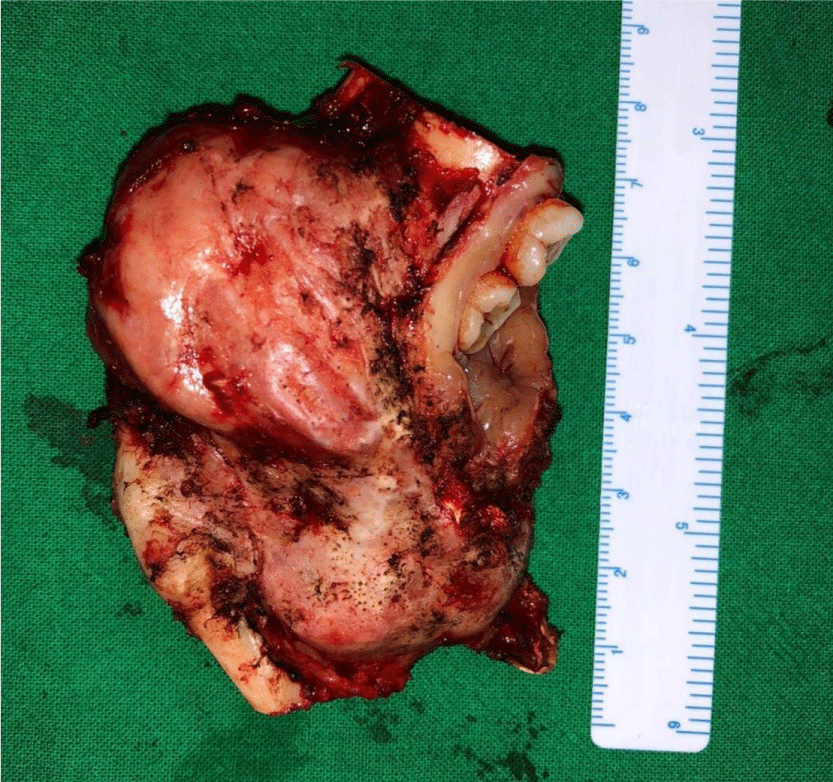
After written and informed consent, baseline investigations, pre-operative workup, and general anesthesia fitness. She was booked for elective intra-oral surgery and shifted to Operation Theater. She underwent the complete surgical resection of the lesion with the extraction of involved teeth, enucleation, and curettage of the involved bone (Figure 8). The patient went through a smooth recovery with no drastic or minor complications on antibiotics and symptomatic treatment in the hospital postoperative course and on a follow-up visit. Post-operative radiological imaging showed no evidence of recurrent or residual lesions.
Discussion
Cemento-ossifying fibroma, a rare benign condition, is a slow-growing tumor that occurs between the third to fourth decades and has a female predilection [1-9]. However, in a literature review done by Su, et al. [4] equal predilections were noted in all age groups and female predilection was only seen in the fourth decade. The most usual location for these tumors is the mandible, nonetheless, some studies have also reported the maxilla, paranasal sinuses, and nasal cavities as the less common sites [2,3]. These lesions are slow-growing, and in the majority of the cases patients are asymptomatic and the tumors are found incidentally [1]. By the time these tumors increase in size, they can cause facial asymmetry, and discomfort and can occasionally push the adjacent dental organs [1-3]. Our patient was also a middle-aged female who presented with complaints of facial swelling which was painless and progressed slowly with time.
In the Radiological aspect, initially, the cemento-ossifying fibroma appears as a well-defined radiolucent lesion with no evidence of internal radio densities. As the tumor progresses, there is evidence of calcification so that the radiolucent area opacifies, and eventually, the lesion appears as a lobulated almost complete radiopaque mass in the mature stage. An important diagnostic feature of cemento-ossifying fibroma is the expansion of lesions equally in all directions and present as a round tumor mass. The cortical plate may be expanded, displaced, thinned out, and remains intact. Teeth adjacent to or involved in the lesion may be displaced but resorption is not associated with this tumor [3,4,6,9]. In our case the tumor was large well corticated, sharply marginated mixed density with high densities representing calcific foci/cementing material, expansile lesion with no evidence of bone destruction or cortical break.
In a certain study, done by Pindborg, Waldron, and many other authors, it has been discussed that central ossifying fibroma and central cementifying fibroma show the same clinical, radiological, and histopathological features. The only difference is that in central ossifying fibroma there is the proliferation of osteoblasts with bone formation and cementoblasts with cementum formation in cementifying fibroma. Therefore a collective term cemento-ossifying fibroma was generated [9]. This cemento-ossifying fibroma was classified as a fibro-osseous lesion or non-odontogenic tumor of the jaw according to WHO classification [1,6,9]. According to WHO classification these tumors arise from mesenchymal blast cells of the periodontal ligament, with a potential for fibrous tissue, bone, cement, or a combination of such elements. However, there is still a debate over its origin, since tumors of similar histology have been reported in bone lacking periodontal ligament and not located in the maxillary region, such as ethmoid bone, frontal bone, or even long bones of the body [1,3,8]. The ongoing controversy then led to the need for histopathological evaluation of the disease for final diagnosis [1,8].
Histologically the lesion shows the presence of generally hypercellular fibrous tissue with the occasional presence of bone tissue or cementiform calcifications. The morphology is benign, with very little proliferative activity and the absence of atypia or necrosis [3-9]. Our histopathological examination showed hyper-cellular stroma with intervening cementum-like calcification. No atypia, necrosis, or mitosis was seen. Features were compatible with cemento-ossifying fibroma.
Due to the good delineation of the tumor, surgical removal and curettage is a treatment of choice [1]. Resection must be complete to prevent a recurrence. In recurrent lesions, successive enucleations or wider resection with or without reconstruction can be carried out [1-9]. Our patient also underwent complete surgical resection. A follow-up of the patient with radiological imaging was done which showed no residual or recurrent lesion.
Conclusion
Cemento-ossifying fibroma is a rare benign fibro-osseous neoplasm that commonly occurs in mandible bone and is usually discovered incidentally on radiological imaging. It can be increased in size over time and may cause disfigurement and asymmetry of the face. Radiologists should aware of radiological features of such lesions for early diagnosis and treatment or follow-up in correlation with histopathology to prevent the progression in size of the lesion, disfigurement of the face and post-operative cosmetic deformity.
Ethical review
This case report was written and images of the patient’s face, scans, and histopathology slides were added after taking consent from the patient, and the patient’s identity is not shown here and will be kept confidential.
- Ram R, Singhal A, Singhal P. Cemento-ossifying fibroma. Contemporary clinical dentistry. 2012. 3(1):83.
- Trijolet JP, Parmentier J, Sury F, Goga D, Mejean N, Laure B. Cemento-ossifying fibroma of the mandible. Eur Ann Otorhinolaryngol Head Neck Dis. 2011 Jan;128(1):30-3. doi: 10.1016/j.anorl.2010.06.005. Epub 2010 Sep 17. PMID: 20846921.
- Peravali RK, Bhat HH, Reddy S. Maxillo-Mandibular Cemento-ossifying Fibroma: A Rare Case Report. J Maxillofac Oral Surg. 2015 Mar;14(Suppl 1):300-7. doi: 10.1007/s12663-013-0507-6. Epub 2013 Apr 2. PMID: 25838714; PMCID: PMC4379219.
- Katti G, Khan MM, Chaubey SS, Amena M. Cemento-ossifying fibroma of the jaw. BMJ Case Rep. 2016 May 12;2016:bcr2015214327. doi: 10.1136/bcr-2015-214327. Erratum in: BMJ Case Rep. 2016;2016. pii: bcr2015214327corr1. doi: 10.1136/bcr-2015-214327corr1. PMID: 27174452; PMCID: PMC4885328.
- Kaur T, Dhawan A, Bhullar RS, Gupta S. Cemento-Ossifying Fibroma in Maxillofacial Region: A Series of 16 Cases. J Maxillofac Oral Surg. 2021 Jun;20(2):240-245. doi: 10.1007/s12663-019-01304-y. Epub 2019 Nov 8. PMID: 33927492; PMCID: PMC8041960.
- Silvestre Rangil J, Silvestre Donat FJ, Requeni Bernal J. Cemento-ossifying fibroma of the mandible: Presentation of a case and review of the literature. J Clin Exp Dent. 2011:3(1):e66-69.
- Brademann G, Werner JA, Jänig U, Mehdorn HM, Rudert H. Cemento-ossifying fibroma of the petromastoid region: case report and review of the literature. J Laryngol Otol. 1997 Feb;111(2):152-5. doi: 10.1017/s0022215100136709. PMID: 9102442.
- Prakash R, Shahid SM, Raj H, Anil KS. Cemento-ossifying fibroma: A diagnostic dilemma. International Journal of Oral Care and Research. 2021 Jan 1;9(1):46.
- Patait M, Chaudhari V, Mathew A, Mangrolia R, Ahire M. Cemento-ossifying fibroma: Case report. Int J Appl Dent Sci. 2020;6(4):215-218.
- Wanzeler AM, Rohden D, Arús NA, Silveira HL, Hildebrand LD. Central cemento-ossifying fibroma: clinical-imaging and histopathological diagnosis. International Journal of Odontostomatology. Temuco. 12: 233-236.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.





 Save to Mendeley
Save to Mendeley
