International Journal of Clinical Endocrinology and Metabolism
Intrathyroidal thyroglossal duct cyst presenting as chronic thyroiditis: Case report and narrative review of the literature
Arsheed Hussain Hakeem1*, Hassaan Javaid2, Hima Bindu Rallabandi3 and Fozia Jeelani Wani4
2Junior Resident, Department of Trauma Surgery, All India Institute of Medical Sciences, New Delhi, India
3Consultant Department of Pathology, Apollo Hospitals, Hyderabad 500096, India
4Assistant professor, Department of gynecology and obstetrics, Apollo Institute of Medical sciences and research, Hyderabad, 500096 India
Cite this as
Hakeem AH, Javaid H, Rallabandi HB, Wani FJ (2020) Intrathyroidal thyroglossal duct cyst presenting as chronic thyroiditis: Case report and narrative review of the literature. Int J Clin Endocrinol Metab 6(1): 017-021. DOI: 10.17352/ijcem.000047The presence of the thyroglossal duct cyst (TDC) within the thyroid gland is of rare occurrence as only 16 cases have been documented to date. It is even rare for the intrathyroidal TDC to present as infective thyroiditis as only one case has been reported in the scientific literature. We report a case of intrathyroidal TDC which presented as recurrent episodes of thyroiditis in a 13-year-old female. Diagnostic work-up, management, and review of pertinent scientific literature is also presented. To the best of our knowledge, this is the second case of intrathyroidal TDC which has presented as chronic recurrent thyroiditis. It is the first case of the intrathyroidal TDC with chronic thyroiditis reported in the pediatric age group.
Introduction
The involution of the thyroglossal duct typically occurs between 7 and 10 weeks of gestation following migration of the primitive thyroid to its final pre-tracheal position in the inferior neck. Persistence of inferior thyroglossal duct is not uncommon, like presence of the pyramidal lobe of the thyroid gland. Similarly, remnant of upper thyroglossal duct may give rise to cyst formation. Thyroglossal duct cysts are among the most common neck swelling encountered in infancy and childhood. These cysts may develop at any place along the migratory path of the thyroglossal tract of the developing thyroid gland. Most common location is around the hyoid bone superior to the thyroid gland. On review of scientific literature, we found only seventeen documented cases of the TDC within the thyroid gland [1-10]. To the best of our knowledge only one case of intra thyroidal TDC presenting as thyroiditis has been reported [10]. We describe a rare case of intrathyroidal TDC that presented as chronic recurrent pyogenic thyroiditis. According to the PRISMA guidelines, PubMed and Medline were searched for papers from January 1985 to January 2020.In particular, we considered articles with focus on intrathyroidal thyroglossal duct cysts published in English and other languages.
Case report
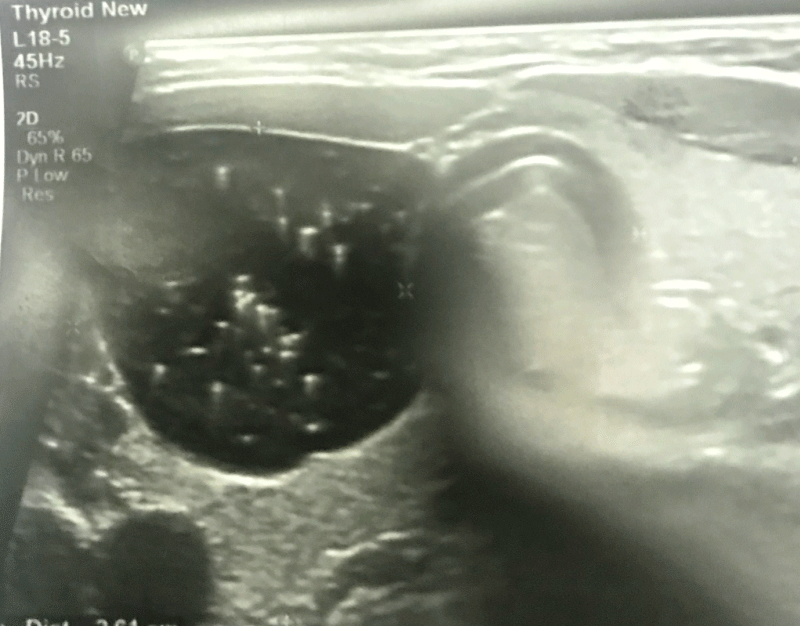
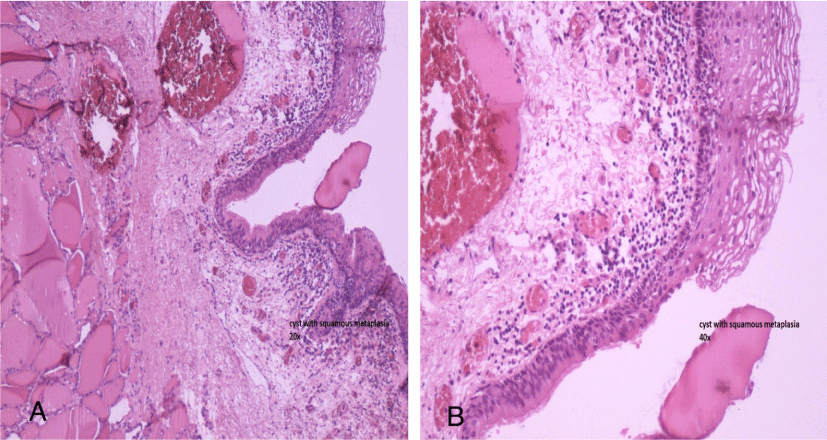
An otherwise healthy 13- year- old female presented to our head and neck clinic with recurrent episodes of lower neck pain and swelling of 2 years duration. It was associated with repeated episodes of fever and chills & rigors. All the recurrent episodes were conservatively managed with antibiotics and anti-pyretic medication. There were no signs and symptoms suggestive of hypo or hyperthyroidism. There is no history of thyroid related disorders in the family. Physical examination revealed a 4×3 cms, palpable, soft cystic mass in the right thyroid lobe region that moved with swallowing. There were no signs of inflammation or fistula formation on local examination. Laboratory results indicated mild leukocytosis with a white blood cell count of 11000 cells/μL (normal range is 4000 to 10,000cells/μL) and her thyroid function tests were in normal range. Her thyroglobulin antibody, thyroid peroxidase antibody, thyrotropin binding inhibitory immunoglobulin, and thyroid stimulating immunoglobulin levels were normal. Ultrasound demonstrated a 4.3×3.5 cms homogenous low echoic cyst with thin capsule involving mainly the right lobe of the thyroid which extended into the isthmus (Figure 1). Comet tail appearances was seen on ultrasonography due to the calcified debris filling the cyst (Figure 1). Fine needle aspiration yielded thick, viscous, dirty white colored fluid. Cytological examination of the aspirated material revealed lympho-histiocytic tangles, and bland-appearing follicular cells. Definitive surgical treatment of right thyroid lobectomy with isthmusectomy was performed. Histopathology reveal a 4.5×3.2 cms cyst involving the right thyroid lobe and isthmus. The cyst was predominantly lined by pseudo-stratified ciliated columnar epithelium with focal squamous metaplasia and mild infiltrate of lymphocytes was seen in the wall (Figure 2 A and B). The TDC was completely surrounded by normal thyroid tissue, with no external tract present. Secondary changes were seen including chronic lympho-histiocytic reaction and dense fibrosis. Histological diagnosis of an intrathyroidal thyroglossal duct cyst was made. Her postoperative period was uneventful. She is being regularly followed up and has not reported any episode of neck pain associated with fever after the surgical procedure.
Discussion
Intrathyroidal thyroglossal duct cyst presenting as chronic thyroiditis is a rare event. Our case represents a unique presentation of the thyroglossal duct cyst in more than one way. First, to the best of our knowledge only 16 cases of the true intrathyroidal TDC’s have been documented in the literature (Table 1) [1-10]. This makes our case 17th case of a true intrathyroidal TDC. Second, only 7 cases of intrathyroidal TDC have been reported in the pediatric age group which makes our case 8th documented case [1,6,9]. Last and rarer, only one case has presented as thyroiditis that too in an adult [10]. This makes our case extremely rare presentation, intrathyroidal TDC as chronic thyroiditis in pediatric age. Most common cause of the thyroiditis in the paediatric age is autoimmune thyroiditis. This may present either as a goitrous (Hashimoto’s thyroiditis) and a non-goitrous (atrophic thyroiditis) variant.
Thyroglossal duct cysts present mostly in the pediatric and young adults and only one third present after third decade of life. Our review revealed only 7 cases of intrathyroidal TDC in the pediatric age and 9 cases in the adults (Table 1). Most of the cases of the intrathyroidal TDC presented as asymptomatic anterior neck mass, and only in two cases swelling was associated with cases compressive symptoms like discomfort on swallowing (Table 1) [8,10]. Out of the 16 cases only one case exhibited signs of infection and hyperthyroidism (Table 1) [10]. Similar to our case, Barber et al reported a case with history of neck mass and features ofthyroiditis [10]. In addition they reported dysphagia, fever, sore throat and hyperthyroidism (Table 1) [10]. On ultrasonography, our case had well defined low echoic cystic nodule involving entire right lobe of the thyroid with calcified debris (Figure 1). Most of the authors have reported hypoechoic cystic nodule in thyroid, while only few have reported complex cysts and one case reported calcified debris, similar to our case (Table 2).It is difficult to distinguish intrathyroidal TDC from other causes of cystic lesions of thyroid gland like colloid cyst, lympho-epithelial cyst and branchial cleft cysts clinically or imaging. While Radionuclide thyroid scintigraphy is useful in cases of lingual thyroid and TDC cysts where a normally located thyroid gland cannot be detected, routine use as part of workup is not justified.
Fine needle aspiration cytology in our case revealed normal looking follicular and squamous cells with lympho-histiocytic tangles. Most of the authors who subjected their cases to the fine needle aspiration reported the presence of normal looking follicular/squamous cells (Table 1). Some authors also reported presence of histio-lymphocytic tangles and macrophages along with normal squamous cells (Table 1). Although, cytology has been shown to have only 62% sensitivity and 69% positive predictive value in the diagnosis of TDCs, our review showed most cases lacked sufficient FNA findings to make a definitive diagnosis of intrathyroidal TDC. But FNA was quite useful in ruling out malignancy (Table 1). As completely intrathyroidal TDCs is a rare entity to occur, clinical suspicion is important to arrive at definitive diagnosis. One should also get alerted in the setting of an infected, cystic mass in the anterior neck, as our case presented. The thyroid gland is relatively resistant to infections due to its high degree of vascularity and normal lack of direct communication with surrounding structures. Hence presence of the inflammatory signs and symptoms with finding of an intrathyroidal abscess should mandate further investigation for rare cause Like intrathyroidal TDC.
Surgery remains the standard of care for the intrathyroidal TDC as all the reported cases have been treated successfully with complete excision. Surgery prevents recurrent episodes of infection and gives permanent cure. Different authors have used different procedure for treating intrathyroidal TDC. Some authors have done only cyst excision as used in 5 cases, while some have used hemithyroidectomy as in 4 cases (Table 2). Other authors have used hemithyroidectomy with isthmusectomy as described for 6 cases and only isthmusectomy in one case (Table 2). In our case the cyst was involving entire right thyroid lobe and was extending into the isthmus, we performed right thyroid lobectomy with isthmusectomy to achieve complete removal. We could not find remnant thyroglossal duct tract in our case. Thyroglossal duct tract was seen associated along with the cyst in 4 cases only, while rest of the cases it was not seen. In all the cases where the remnant thyroglossal tract was associated, additional sistrunk’s procedure was also performed (Table 2). The treatment of TDC is surgical excision with the Sistrunk procedure as described in 1920. This requires excision of the tract with the removal of the central portion of the hyoid bone and following the tract to the base of tongue in order to prevent recurrence which may occur with simple excision alone. Sistrunk reported a less than 10% recurrence rate when the lesion is excised as described above. Final histopathology study of the specimen revealed Cyst lined by pseudo stratified ciliated columnar cells with squamous metaplasia surrounded by thyroid follicles. It was also associated with lympho-histiocytic inflammation with dense fibrosis due to chronic infection. Most of the authors have reported similar findings on pathology (Table 2).
Conclusions
Intra thyroidal TDCs are a rare cause of anterior neck mass, but can present with chronic inflammation and infection. The possibility should be considered in patients with an infected cyst or thyroid nodule along the midline of the neck. Definitive treatment with surgical excision can prevent recurrent episodes infection.
Learning points
- Recurrent episodes of pain and fever associated with swelling in the thyroid region can be signs of intrathyroidal thyroglossal duct cyst.
- Preoperative clinical examination, imaging, FNA are not conclusive of intrathyroidal thyroglossal duct cyst.
- Surgery gives the long term cure by avoiding recurrent infections in the cyst.
Author contributions
Arsheed Hakeem conceived and drafted the manuscript and prepared the figures. Hassaan Javaid carried out the clinical assessment of the patients. Hima Bindu Rallabandi did the pathology and Fozia wani revised the manuscript for intellectual content.
Competing interests
The funding organization(s) played no role in the study design; in the collection, analysis, and interpretation of data; in the writing of the report; or in the decision to submit the report for publication.
Ethical statement
The patient provided written informed consent for publication of the case details and analysis.
- Sonnino RE, Spigland N, Laberge JM, Desjardins J, Guttman FM (1989) Unusual patterns of congenital neck masses in children. J Pediatr Surg 24: 966-969. Link: https://bit.ly/31nKzJk
- McHenry CR, Danish R, Murphy T, Marty JJ (1993) Atypical thyroglossal duct cyst: a rare cause for a solitary cold thyroid nodule in childhood. Am Surg 59: 223-238. Link: https://bit.ly/3g4Xlk8
- North LJH, Foley AM, Hamill RL (1998) Intrathyroid cysts of thyroglossal duct origin. Am Surg 64: 886-888. Link: https://bit.ly/2A8E7e5
- Hatada T, Ichii S, Sagayama K, Ishii H, Sugihara A, et al. (2000) Intrathyroid thyroglossal duct cyst simulating a thyroid nodule. Tumori 86: 250-252. Link: https://bit.ly/3dGFCOa
- Johnston R, Wei JL (2003) Intra-thyroid thyroglossal duct cyst as a differential diagnosis of thyroid. Int J Pediatr Otorhinolaryngol 67: 1027-1030. Link: https://bit.ly/2Z7hyyE
- Roy D, Roy PG, Malik VK, Seenu V (2003) Intrathyroidal thyroglosduct cyst presenting as thyroid nodule. Int J Clin Pract 57: 637-638. Link: https://bit.ly/3i3A2ca
- Perez-Martinez A, Bento-Bravo L, Martinez-Bermejo MA, Conde-Cortes J, de Miguel-Medina C (2005) An intra-thyroid thyroglossal duct cyst. Eur J Pediatr Surg 15: 428-430. Link: https://bit.ly/388sMHe
- Choi HJ, Jung JH, Yoo J (2007) Intra-thyroid thyroglossal duct cyst: A case report. Korean J Pathol 41: 132-134.
- Alvarez Garcia N, Burgues Prades P, Gonzalez Martinez- Pardo N, Simon Portero S, Fernandez Atuan R (2015) The intra-thyroid thyroglossal cyst in the differential diagnosis of the solitary thyroid nodule: A presentation of 2 cases. An Pediatr (Barc) 82: 360-361. Link: https://bit.ly/2CNdxrR
- Barber J, Martinez DS, Diaz FP, Stark AP, Masha J (2018) Intrathyroidal thyroglossal duct cyst: a rare cause of thyroiditis in an adult. AACE Clinical Case Reports 4: e90-e93.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
