International Journal of Clinical Endocrinology and Metabolism
A fatal case of myxedema coma
Fatima Zahra El Bouazzaoui*, Imane Boubagura, Sana Rafi, Ghizlane El Mghari and Nawal El Ansari
Cite this as
El Bouazzaoui FZ, Boubagura I, Rafi S, Mghari GE, Ansari NE (2019) A fatal case of myxedema coma. Int J Clin Endocrinol Metab 5(1): 013-015. DOI: 10.17352/ijcem.000036Myxedema coma is a rare clinical condition that represents severe hypothyroidism decompensation usually occurs in patient with long-standing undiagnosed hypothyroidism and is usually precipitated by infection and discontinuation of supplements treatment. Clinical symptoms are a mental decreased status, hypothermia, bradycardia, hypotension, hypoglycemia and hypoventilation. Thyroid hormone measurement allows the diagnosis. Protocols with rapid intravenous high doses of thyroid hormone, warming and mechanical ventilation may improve the prognosis. The purpose of the present article is to describe a fatal case of myxedema coma in elderly-woman occurring in the context of immunodeficiency.
Introduction
Myxedema coma is a very rare endocrine emergency as a result of a very low synthesis of thyroid hormone due to some precipitating factors such as infections, hypothermia, heart failure, stroke, trauma, digestive bleeding, poor compliance of prescribed thyroid medications and drugs like lithium, sedatives, anesthesia [1]. Elderly patients with cardiovascular diseases, mental problems, sepsis and hypothermia are in highest risk of mortality [2,3]. As the condition is rare and not well recognized, we have only little case reports and series [4]. Intravenous thyroid hormone is the main therapy associated with supportive measures and in case of patient with stress statement and adrenal insufficiency, glucocorticoids must be co-administrated, the rate of mortality in myxedema coma high at 30%-40% [5]. This rare complication of hypothyroidism must be well known by the clinicians to improve management of patient.
Case Presentation
A 61-year-old woman with an end-stage renal failure associated with type 2 diabetes, hypertension, military tuberculosis with pulmonary and peritoneal involvement under anti-bacillary treatment and autoimmune thyroiditis with discontinuation of L-thyroxine since 2 months. She was hospitalized in the emergency department for mental status alteration. At admission, here blood pressure: 120/70 mmhg, bradycardia at 54 bpm, hypothermia at 35 °C.
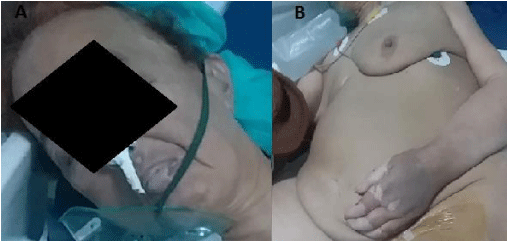
The patient presented with dry depilated skin, Vitiligo and generalized myxedema (Figure 1). The Glasgow Coma Score was 10 (2/3/5) .No goiter or stiffness was found after examination. Her consciousness level worsened and the patient was transferred to intensive care unit.
The initial laboratory test showed a normochromic normocytic anemia without electrolyte disorders. However because of end-stage renal failure level, patient had urea at 1,07g/l and serum creatinine at 73 mg/l. Hepatic encephalopathy was eliminated as the liver function was normal. Thyroid hormones were altered with thyroid-simulating hormone (TSH) of 100 mU/L and free thyroxine (FT4) of 3.9 pmol/l and free thyiodotyronine (FT3) of 1.6 pmol/l. Baseline cortisol level was 133 ug/l. The synacthen test was not performed so the coexisting of adrenal insufficiency was not eliminated.
The alteration of consciousness required the performance of brain tomography to search the possibility of existence of stroke. We should notice that our patient had military tuberculosis that may involve the central nervous system and could justify a part of the symptoms. No stroke or cerebral abnormalities was discovered in the tomography. Spinal fluid analysis also eliminated the hypothesis of meningitis or sepsis with the laboratory findings. ECG showed sinus bradycardia, atrial fibrillation and left ventricular hypertrophy. A chest X-ray showed foci of basal condensation with micronodule.
Myxedema coma’s diagnosis was confirmed and medical treatment was started. The patient was warmed gradually and oxygen was supplied via mask. Levothyrox 300 ug was administered via nasogastric tube on third day after admission. Intravenous injection of bolus hydrocortisone 100 mg was given followed by 50 mg /6H intravenously. The patient was under antibacillary treatment that we had continued and she had received here usual hemodialysis session. The thyroid hormones levels did not be verified since the patient’s clinical condition has not improved and she died 3 days later.
Discussion
Myxedema coma (MC) is an extreme manifestation in patients with untreated hypothyroidism. The typical clinical manifestation includes decreased mental status, hypothermia, hypoventilation, bradycardia, hypotension, and hypoglycemia. Physical findings show myxoedematous face, which is characterized by generalized puffiness, macroglossia, ptosis, and coarse [4]. Very few cases of MC have been reported till date, with the first case reported in London in 1879 [6]. Given the rarity of MC, actual prevalence is unclear with the estimated incidence rate of 0.22 cases per million people per year [7].
The diagnosis could be delayed because diagnostic laboratory data may not be available in a timely manner during emergency presentation. Our patient was also reported to have delayed diagnostic despite she was presented with all common features of MC, because she has other medical history as miliary tuberculosis and end-stage renal failure that make the first diagnostic suspected of a decreased mental status secondary to hyper uremia or central nervous system tuberculosis.
MC is a lethal endocrine emergency. Administration of thyroid hormone replacement is mainstay therapy. It is recommended that initial replacement should be levothyroxine given intravenously at a loading dosage of 200 to 400 ug. The replacement dosage reduced to 1.6 ug/kg/d thereafter [8]. The therapy should be introduced without delay [8]. It is suggested that this hormone started intravenously because gastrointestinal absorption may be impaired in severe cases [9]. Some authors show beneficial effects of combinaison of enteral levothyroxine and liothyronine and reported that this patient had a lower mortality rate than those who received levothyroxine alone [10,11]. However, levothyroxine injection and Liothyronine are currently unavailable in Morocco. Our patient was treated with gastric levothyroxine at a dosage of 300 ug/d.
Increased cortisol clearance and aggravation of adrenal deficiency could be secondary to thyroid hormone administration. If the facilities for hypothalamic-pituitary axis evaluation are not available on emergency, steroid therapy can be introduced and a formal evaluation of axis should be done later when the patient is stable. Hydrocortisone I.V administration is preferred at a rate 50 mg every six hours [4]. On account of the highest risk of adrenal insufficiency in our case because she had auto immune thyroiditis, vitiligo, we have started the replacement of corticosteroids with hydrocortisone at 50 mg/6H.
Generally patient with Myxedema coma has a bad evolution even with the adequate and early treatment. Aggravating factors like elderly age, multiple comorbid states may impair myocardial function after fast normalization of serum thyroid hormone levels [12].
We can conclude that the clinician should routinely control the thyroid function to looking for dysthyroidism. Myxedema coma can be fatal when it’s not well recognized. Intravenous administration of Levothyroxine is the best option due to lower risk of enteric absorption which is inherent to the syndrome. Others supportive measures including treatment in the intensive care unit, cardiovascular and ventilator support, passive rewarming, treatment of any concurrent infection and correction of electrolyte imbalance are very important in the treatment of this threatening illness.
- Klubo-Gwiezdzinska J, Wartofsky L (2012) Thyroid emergencies. Med Clin North Am 96: 385-403. Link: https://tinyurl.com/yxko4hnp
- Dutta P, Bhansali A, Masoodi SR, Bhadada S, Sharma N, at al. (2008) Predictors of outcome in myxoedema coma: A study from a tertiary care centre. Crit Care 12: R1. Link: https://tinyurl.com/y2jo5pt9
- Yamamoto T, Fukuyama J, Fujiyoshi A (1999) Factors associated with mortality of myxedema coma: report of eight cases and literature survey. Thyroid 9: 1167-1174. Link: https://tinyurl.com/y5b2lj8f
- Mathew V, Misgar RA, Ghosh S, Mukhopadhyay P, Roychowdhury P, et al. (2011) Myxedema Coma: A New Look into an Old Crisis. Journal of Thyroid Research 2011: ID 493462-7. Link: https://tinyurl.com/y32j2xsr
- Lklouka MA (2013) Myxoedema Coma: A Very Rare Presentation of Severe Hypothyroidism. J Med Cases 4: 715-718. Link: https://tinyurl.com/y5qe6xvv
- Kwaku MP, Burman KD (2007) Myxedema coma. J Intensive Care Med 22: 224-231. Link: https://tinyurl.com/yxvlpj98
- Hampton J (2013) Thyroid gland disorder emergencies: thyroid storm and myxedema coma. AACN Adv Crit Care 24: 325-332. Link: https://tinyurl.com/y2g9tauh
- Jonklaas J, Bianco AC, Bauer AJ (2014) Guidelines for the treatment of hypothyroidism: prepared by the american thyroid association task force on thyroid hormone replacement. Thyroid 24: 1670-1751. Link: https://tinyurl.com/y25yhgeq
- Wiersinga WM, De Groot LJ, Chrousos G, Dungan K, Feingold KR, et al. (2000) Myxedema coma (severe hypothyroidism). Endotext MDText.com, Inc., South Dartmouth (MA): 2000. Link: https://tinyurl.com/y55z5uvj
- Ono Y, Ono S, Yasunaga H, Matsui H, Fushimi K, et al. (2017) Clinical characteristics and outcomes of myxedema coma: analysis of a national inpatient database in Japan. J Epidemiol 27: 117-122. Link: https://tinyurl.com/y4goetsu
- Ueda K, Kiyota A, Tsuchida M, Okazaki M, Ozaki N (2019) Successful treatment of myxedema coma with a combination of levothyroxine and liothyronine. Endocr J EJ18-0469. Link: https://tinyurl.com/yypap5a5
- Yamamoto T, FukuyamaJ, Fujiyoshi A (1999) Factors Associated with Mortality of Myxedema Coma: Report of Eight Cases and Literature Survey. Thyroid 9: 1167-1174. Link: https://tinyurl.com/y5b2lj8f
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
