Global Journal of Obesity, Diabetes and Metabolic Syndrome
Nonadherence to dietary recommendation and associated factors among type 2 diabetic patients in Illubabor zone, South West Ethiopia
Rukiya Debalke1*, Beakal Zinab2 and Tefera Belachew2
2Department of Nutrition and Dietetics, Faculty of Public Health, Jimma University, Jimma, Ethiopia
Cite this as
Debalke R, Zinab B, Belachew T (2020) Nonadherence to dietary recommendation and associated factors among type 2 diabetic patients in Illubabor zone, South West Ethiopia. Glob J Obes Diabetes Metab Syndr 7(3): 053-059. DOI: 10.17352/2455-8583.000048Introduction: Dietary adherence, as one of the cornerstones of diabetes self-management, is important to improve glycemic control and preventing diabetes complications, which affect patient’s quality of life as well, impose a large economic burden on health care systems; however most patients have difficulty in adhering to dietary recommendations.
This study assessed the magnitude of non adherence and factors associated with nonadherence to dietary recommendation among type 2 diabetic patients attending follow up at government hospitals in Ilu Abba Bora Zone, south west Ethiopia, 2018
Methods: Institution based cross-sectional study was conducted from March 19 to May 19, 2018 among 422 diabetic patients attending regular follow up at government health facilities in Illuababor Zone, Southwest Ethiopia, participants were selected using systematic random sampling method. Data were collected using pretested interviewer administered semi structured questionnaires. Dietary adherence was assessed using modified version of Morisky medication adherence scale. Multivariable logistic regression was used to identify factors associated with diabetic patient’s non adherence to dietary recommendations. Odds ratio along with 95% confidence interval and p value <0.05 was used to declare significant association.
Results: In the current study more than half (51.8%) of the respondents were found to be non adherent to dietary recommendations.Non-adherence was significantly associated with patients occupation [AOR=5 (95%CI: 2.5, 9.8)], not being diabetic association member [AOR=2.8, (95%CI: 1.6, 4.9)], having low perceived susceptibility [AOR=2 (95%CI: 1.1, 3.7)], and poor emotional support of friends and families [AOR=1.9 (95%CI: 1.2-3.1)].
Conclusion: The rates of non adherence to dietary recommendation were generally found to be high. Model based and family centered educational packages should be delivered, additionally efforts should be taken to engage them to be a member of different membership platforms.
Introduction
Diabetes is a chronic disease which arises when the body is unable to use the insulin it produces effectively (type 2), or when enough insulin is not produced by the pancreas (type 1) [1]. It has become a global health emergency affecting high- middle- and low-income countries. The number of people with type2 diabetes is growing rapidly worldwide. This rise is associated with ageing populations, economic development, increasing urbanization, less healthy diets and reduced physical activity [2].
Being a complex chronic disorder, diabetes requires continuous medical care, predominantly life time patient’s adherence to life style modification recommendations. The management of type 2 diabetes begins with an individualized regimen of diet, exercise, and medical counseling designed to achieve glycemic control [3].
The World Health Organization defines adherence as “the extent to which patients take medications as prescribed by their health care providers, following a diet and/or executing lifestyle changes corresponds with agreed recommendations from a health care provider” [4].
Adherence to dietary recommendation have been shown to improve glucose levels, to lead to decreased blood pressure and to correct lipid abnormalities which are factors associated with the micro and macro-vascular complications of diabetes [3]. Nevertheless, diabetic diet adherence is one of
The most challenging concerns of diabetes self management. Non adherence affects the health care provider and the health care delivery system as well as the patient as the patient has to suffer from the poor quality of life and long duration of hospital stay and increased cost and burden of the disease [5,6]. Non adherence to dietary recommendation is very prevalent in patients with diabetes and there is a variation in different part of the world, findings from study done in Kuwait indicated 63.5% non-adherence to dietary recommendation , Furthermore, the study indicated age, sex, income, duration of disease, social supports to be significantly associated with diet regimen non adherence [7].
There is an urgent need to improve adherence status of recommended healthy life styles to ensure achievement of maximum health benefits to patients and for a quality life because the risk of complications of diabetes can be reduced by proper adherence. However, in Ethiopia lack of data on dietary regimen adherence level and factors influencing the regimen adherence affect the long term management of diabetes,therefore this study aims to give a clear picture of what diabetic patient’s dietary recommendation adherence status looks like and factors affecting non adherence to dietary regimen.
Methods
Study setting and participants
The study was conducted in Ilu Abba Bora Zone, South west Ethiopia, there are 2 public hospitals in the zone providing regular follow up care for diabetic patient. These facilitiues provide service in all of the weekdays and patients collect their medication on monthly basis. The diabetic clinics provide services for an average of 20-22 patients per day.
All adult type 2 diabetes patients who were on regular follow up at MKRH and Darimu Hospital NCD follow up clinic were the source populations, while randomly selected adult type 2 diabetic patients who were on regular follow up at MKRH and Darimu Hospital NCD follow up units were study populations. In the current study, patients who were unable to provide required information and newly diagnosed patients (who had less than at least threefollow up visits) were excluded from the study.
Sample size and sampling procedure: Sample size was separately calculated for the outcome (Non- adherence to dietary recommendations) and for each explanatory variable using different parameters taken from previously published researches and finally the largest sample size was taken to ensure a better representativeness. The largest sample size was estimated with the following assumptions,expected proportion of poor dietary practice to be 51.4 % taken from a study in Yekatit 12 Hospital, Addis Ababa city (8), 95% confidence level, 5% margin of error, and 10% non response rate, then the final sample size became 422.
The final sample (422) was proportionally allocated to each hospital based on number of diabetic patients on regular follow up.Accordingly 338 and 187 participants were included from Metu and Darimu Hospitals respectively. Finally study participants were selected using systematic sampling technique.
Data Collection and measurment
Data were collected by interviewing eligible subjects using a pretested structured questionnaire by two trained nurses. The questionnaire contains questions to assess socio demographic information, health profile information, diabetes health beliefs and emotional and active or instrumental family and non family, members support. Dietary adherence status was assessed using the modified form of the eight-item Morisky medication adherence scale (MMAS-8) which was developed in 2008, with a reliability of 0.83 and good concurrent and predictive validity [8,9], it is 12 item scale modified based on the general advice for diabetic diet plan(association SAd: South African diabetes association. In.: South Africa diabetes association 2001). by Almelmal Worku, et al. [8].
Anthropometric measurements was taken by two trained professional nurses at the end of the interview, weight of the participants was measured using a digital scale (SECA), to the nearest 0.1 kg; each participant was asked to remove heavy clothes and the scale was calibrated to zero before and after each measurement. Height was measured to the nearest 0.1cm using stadiometer without shoes, the head of participants at the Frankfurt plane, knees straight and the heels, buttocks, calves and the shoulders blades touching the vertical stand of the stadiometer. BMI was calculated as body weight in kilograms divided by the squared value of body height in meters (kg/m2). Waist circumference (WC): was measured midway between the inferior angle of the ribs and the suprailiac crest at the end of normal expiration to the nearest 1 cm using a non-stretchable rubber measuring tape, participants in an upright position, with arms relaxed at the side, feet evenly spread apart and body weight evenly distributed in accordance with the WHO reccomendation [10].
Data processing and analysis
Data were coded and entered to Epi data version 3.1 and exported to SPSS windows version 20 for cleaning and analyses. Exploratory data analyses and descriptive statistics including proportion, percentage, ratios, frequency distribution, mean and standard deviation were used to describe the data. Wealth index was constructed using the principal component analysis (PCA) form 27 items after checking all assumptions. Bivariate logistic regression analysis was done to see the association between individual explanatory and outcome variables, variables with P-value <0.25 were a candidate for multivariable logistic regression analysis. Odds ratio with 95% C.I was used to measure the strength of association between dependent and independent variables. P value <0.05 was used to declare level of statistical significance. The scores of each diabetic health belief were constructed by summing up the responses to generate a single score for each construct, Participants were labeled to have high or low level of each constructs using mean value as a cutoff, patients social support status was also labeled based on mean value. Patients’ responses for e ach of the 12 questions were summed up and the outcome variable (Patients Adherence status) was dichotomized by taking the mean value as a cutoff.
Operational and standard definitions
Diet: Refers to the recommended diet for people with DM who should ate small meals spread throughout the day (at least 5/day), ate fruits and vegetables daily, and ate foods high in fibers and whole grain but low in fats, sugars and carbohydrates that have high glycemic index
➣ Adherent to dietary recommendation: are those who scored the mean and above the overall dietary recommendation score.
➣ Non Adherent to dietary recommendation: are those who scored below the overall mean dietary recommendation score.
➣ Adequate glycemic control for DM: FBS measurement 70mg/dL -125 mg/dL.
➣ Inadequate glycemic control for DM: FBS measurement ≥126 mg/dL.
➣ Abdominal obesity: participants with waist circumference >102 cm in men and >88 cm in women.
Ethical consideration
Ethical approval was obtained from the Research and Ethical Committee of Jimma University, Permission letter was written for both Mettu Karl Referral and Darimu Hospital additionally informed consent was obtained from study participants after necessary explanation about the purpose of the study and the respondents’ right to refuse or withdraw at any stage was fully realized. All the interviews with respondents were made under strict privacy.
Results
Sociodemographic characteristics of study participants
A total of 392 respondents participated in the study of which females account for 51.3%. The mean age of respondents were 47 (SD±13). Nearly two third (63.8%) of respondents were married, 37.2% of respondents can’t read and write while 43.1% of them were government employers. Similarly, more than half (58.2%) of respondents were Oromo by ethnicity and one third of the participants were in the lowest wealth Tertiles (Table 1).
Clinical characteristics of study participants
The mean duration of the illness since diagnosis was 6.9 (SD±5.3) years, nearly half of the patients (46.4 %) had family history of DM. Similarly nearly half of the respondents (46.9 %) had additional co- morbidity. More than half of patients (52.3%) used oral hypoglycemic agent to manage their blood glucose level. Hundred sixty nine (43.1%) of patients never missed their diabetic follow up appointment in the past three month.
Additionally, nearly one fourth of participants (26.8%) had not attend diabetic education sessions while (12%) of them attended regularly. It was also observed that one fourth (25.5%) of diabetic patients were member of Ethiopian diabetic association. The mean BMI was 27 (SD±13) and 44.1 % of respondents had normal BMI while 19.6 % of respondents were obese. Likewise (17.3%) of patients had abdominal obesity (Table 2 & Figure 1).
Assesssment of diabetic health beliefs showed that, nearly three fourth (72.7%) of participants had high perceived susceptibility, while proportion of diabetic patients with high perceived severity, perceived barrier and self-efficacy accounts for 54.6, 43.9 and 60.7%, respectively. The study also found poor emotional and active support among 54.3% and 54.8% of respondents, respectively (Table 3).
Adherence status of study participants to dietary recommendation
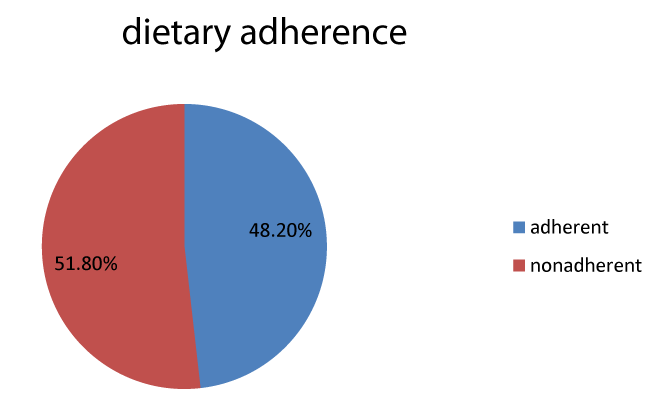
The study indicated, 200(51.8%) of the respondent were non-adherent to dietary recommendation (Table 4 and Figure 2).
Reasons for non adherence to dietary recommendation
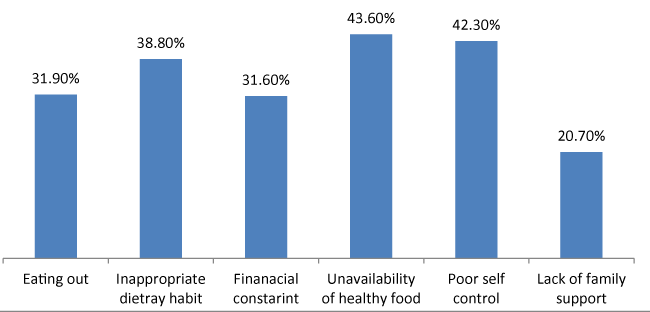
Among the respondents one hundred seventy one (43.9%) answered unavailability of healthy food while166 (42.3%) reported Poor self control and 152 (38.8 %) inappropriate dietary habits as a reason fornot following the recommended diet (Figure 3).
Factors associated with dietary recommendation adherence
On multivariable logistic regression analysis it was observed that patient’s occupation, receiving dietary written instruction, diabetes association membership, abdominal obesity, perceived susceptibility, self efficacy and emotional support for dietary regimen were the independent predictors of dietary adherence status.
Self employed patients had five times higher odds of non adherence than house wives, [AOR=5 (95% CI: 2.56,9.85)] ,patients who did not received dietary written instruction were 1.8 times more likely non adherent [AOR =1.837 (95% CI: 1.06,3.18)]. Patients who were not meber of diabetic association were 2.8 times, more likely non adherent to diatary recommendation than their counterparts [AOR = 2.8 (95% CI: 1.58, 4.95)]. Further more, patients who had abdominal obesity were 2.7 times more likely non adherent [AOR = 2.69 (95% CI: 1.4, 5.19)]. Diabetic patients who had low perceived susceptibility to diabetic complication [AOR = 2.067(95% CI: 1.14, 3.77)], and low self efficacy to follow the recommended dietary and physical activity regimens [AOR = 3.448 (95% CI: 1.96, 6)], were 2 times and 3.4 times more likely to be non adherent to dietary recommendation compared to their counterparts. Similarly patients who had poor emotional support were 1.9 times more likely to be non adherent to dietary recommendation as compared to those with good support [AOR=1.919 (95% CI: 1.176,3.131)] (Table5).
Discussion
In the current study 51.8.2% of the participants were non adherent to dietary recommendation. This finding is comparable with studies done in Addis Ababa, Yekatit12 medical college Hospital and Dilla University Referral Hospital, which non adherence was reported in slightly more than half of the respondents [8,11]. However, it is lower than the studies done in Harar, Nepal, and Surat city India, which indicated 58.7% ,59 % and 66% non adherence to dietary recommendation respectively [12–14], and higher than studies done in Yemen and Ghana, which showed 21% and 34.9% non adherence to dietary recommendation respectively [15,16].
The variation can be explained by difference in the setting, measurement tool, sample size or patient’s socio economic and educational level, seasonal availability of fruits and vegetables or patients difficulty to differentiate the recommended diet. The study area is cash crop area, thus there is very little and seasonal production of vegetables and fruits.
According to different literatures, supporting local food outlets (farmers) and growing food in community garden or back yard will contribute towards peoples food consumption decision, since food price and availability are major factors influencing food choice [17]. Since there is no one set of nutritional recommendation that apply to all diabetes patients dietary recommendation had to be based on individuals habit, preference and availability of food by thoroughly discussing with their physicians [8].
According to the current study, being house wife was associated with dietary recommendation adherence status which is consistent to the studies done in Yemen and India, this may be due to housewives mostly eat at home or cooking in Ethiopian society is exclusively done by housewive, giving them the chance to prepare foods in accordance with their diet plan. Furthermore, decisions about food and nutrition are often made by women and are based on culture and traditional diets. Recommendations and diet plans should therefore be sensitive to such differences [13,15].
The current study also showed that not receiving detailed written instruction regarding dietary recommendation was associated with dietary recommendation non adherence. Lack of dietary written instruction have been stated as most common reason for non adhering to dietary recommendation in a qualitative study done in Belgium and study done in Botswana in 2013 [18,19]. Providing written instructions for diet is helpful because it aids patients to remind recommendations as patients may not remember all the details of discussions during follow up [6].
Diabetic association membership was as well significantly associated with dietary recommendation adherence status, the finding is also supported by findings from Bahirdar Felegehiwot Hospital [20]. This might be due to the association’s monthly regular diabetic education, or it may be because the association provides a chance to learn from each other’s experience, a forum for sharing of information and resources. However according to this study only 25.5 % of the participants were members of a diabetic association, which may be due to the associations’ poor promotion and/or health professionals’ negligence to aware importance of the diabetic association.
This study also indicated that emotional support for dietary regimen was associated with dietary recommendation adherence status, this finding is in line with study done in Nigeria, which reported practical and emotional family involvement are strong factors in diabetes diet regimen and study done in China, also showed social support to be positively associated with overall diabetic self management [21,22]. Social support is required for dietary practice change especially in Ethiopia, where, extended family arrangement is frequently found and families usually share a dish, family members and friends provide encouragement and appraisal support and hence contribute to dietary recommendation adherence. Considering family based approaches as central to the management of diabetes will ensure better adherence level to diabetic self management.
In line with the assumption of health belief model this study indicated that patients perceived susceptibility to diabetic complication is associated with dietary adherence, which was in contrast with study done in Harar which indicated perceived susceptibility as poor predictor of self care practice. Participants’ who had high self efficacy were 3.4 times more likely to adhere to dietary recommendation , this result is consistent with a meta analysis done in China, there was a consistent strong association between increased self-efficacy level and better diabetic self management behaviors [22-24]. This finding is in line with Bandura’s theory of self efficacy, those who had high self efficacy are confident in keeping up with their daily dietary plan because they believe they can control their diabetes. It seems that focus on self–efficacy is the most influential element in the success of such health promotion programs.
Despite the fact that most participants perceived diet as important to achieve and maintain good glycaemic control, majority still reported a range of reasons for not adhering. The most frequent reasons for not adhering to dietary recommendations are unavailability of healthy foods, poor self control, in-appropriate dietary habits, eating out (especially, social gathering, restaurant, and family and friends “homes). The above mentioned reasons are consistent with study done in Botswana, India and Bahrain [13,19,25].
Patterns of diets differ according to sex, culture and age. National strategies should therefore be culturally appropriate and able to challenge cultural influences and to respond to changes over time.
The study has practical significance. Given the emergence of chronic non-communicable diseases in Ethiopia and lack of preventive efforts, the level of non-adherence indentified by this studies calls for arguments to fortify policy and programmatic actions for the change of life styles including adherence to diet. Short of this, the economic and human cost of non-communicable dieases will be eminent.
Since the study is institution based the study participants were patients on regular follow up and therefore might not be truly representative for the entire Diabetic patients.
Conclusion
The current study found dietry recommendation nonadherence among more than half of study participants. Patient’s dietary non adherence was significantly affected by patient’s occupation, receiving dietary written instruction, diabetic association membership, perceived susceptibility, emotional support to dietary regime and self efficacy. The health care system needs to advocate and support dietary regimen adherence through patients family centered model based diabetic education that consider educational status, gender and different age group and providing detailed written instruction like handouts/ leaflets and audio visuals as preferred by the patients.
The authors wish to acknowledge Jimma University for their financial assistance. We are also grateful to the respondents for their participation.
Authors’ contributions
R.D., T.B., and B.Z. (Jimma University) were involved in the design, results analysis and writing of the manuscript.
- WHO (2016) Global Report On Diabetes. World Heal Organ 20 Ave Appia, 1211 Geneva 27, Switz. Link: https://bit.ly/2GOah1c
- Edition S (2015) IDF DIABETES ATLAS Seventh Edition 2015. seventh ed. Link: https://bit.ly/2GKCYMD
- American Diabetes Association (2017) Standards of Medical Care in Diabetes. J Cinical Appl Res Educ 40.
- Sabaté E (2003) Adherence to long term therapies ,World Health Organization 2003. World Heal Organ Ave Appia 20, CH-1211 Geneva 27 [Internet]. Link: https://bit.ly/3jCaseJ
- Warren RE (2007) The stepwise approach to the management of type 2 diabetes. Lancet 370: 1283. Link: https://bit.ly/2GHhTCN
- Delamater AM (2006) Improving Patient Adherence. cliniclal diabetes 24: 71-77. Link: https://bit.ly/3jIeKRU
- Al-ibrahim AA (2012) Factors associated with compliance to diabetes self care behaviors and glycemic control among Kuwaiti people withtype 2diabetes. University of Maryland 2012. Link: https://bit.ly/2SyUVAy
- Abebe S (2015) Dietary practice and associated factors among type 2 diabetic patients : a cross sectional hospital based study, Addis Ababa .Springer Plus 4: 15.
- Morisky DE, DiMatteo MR (2011) Improving the measurement of self-reported medication nonadherence. Response to Authors. J Clin Epidemiol 64: 255-263. Link: https://bit.ly/3ntnmOm
- WHO (2000) Obesity : Preventing and Managing The Global Epidemic Report of a. World Heal Organ Geneva.
- Addisu Y, Eshete A, Hailu E (2014) Assessment of Diabetic Patient Perception on Diabetic Disease and Self-Care. J Metab Syndr 3: 4–11. Link: https://bit.ly/2GMO6J2
- Ayele K, Tesfa B, Abebe L, Tilahun T, Girma E (2012) Self Care Behavior among Patients with Diabetes in Harari , Eastern Ethiopia : The Health Belief Model Perspective. PLoS One 7: e35515. Link: https://bit.ly/33ESBy1
- Jadawala HD, Pawar AB, Patel PB, Patel KG, Patel SB, et al. (2017) Factors Associated With Non Adherence to Diet and Physical Activity among Diabetes Patients : A Cross Sectional Study. Ntl J Community Med 8: 68-73.
- Ghimire S (2017) Barriers to Diet and Exercise among Nepalese Type 2 Diabetic Patients. Int Sch Res Not 2017: 9. Link: https://www.researchgate.net/publication/321062658_Barriers_to_Diet_and_Exercise_among_Nepalese_Type_2_Diabetic_Patients
- Alhariri A, Daud F, Almaiman A, Ayesh S, Saghir M (2017) Factors associated with adherence to diet and exercise among type 2 diabetes patients in Hodeidah city, Yemen. Diabetes Manag 7: 264-271. Link: https://bit.ly/2I9WYZR
- Owusu-akyem S, Agyapong GO, Fataw P (2017) Barriers to Adherence to Diet and Exercise Recommendation amongst Type 2 Diabetes Mellitus Patients. J Heal Med Nurs 39: 48-53.
- Castellanos DC, Downey L, Graham-Kresge S, Yadrick K, Zoellner J, et al. (2013) Examining the diet of post-migrant hispanic males using the precede-proceed model: predisposing, reinforcing, and enabling dietary factors. J Nutr Educ Behav 45: 109-118. Link: https://bit.ly/36Kuobx
- Wens J, Vermeire E, Royen PV, Sabbe B, Denekens J (2005) GPs ’ perspectives of type 2 diabetes patients ’ adherence to treatment : A qualitative analysis of barriers and solutions. BMC Fam Pract 10: 1-10. Link: https://bit.ly/3jHROSO
- Ganiyu AB, Mabuza LH, Malete NH, Govender I, Ogunbanjo GA (2013) Non- adherence to life style modification recommendation (diet and exercise)amongst type 2 dibaetic patients, Botswana. Afr J Prim Heal Care Fam Med 5: 457. Link: https://bit.ly/36HnuDY
- Feleke SA, Alemayehu CM, Adane HT (2013) Assessment of the level and associated factors with knowledge and practice of Diabetes Mellitus among Diabetic Patients attending at FelegeHiwot Hospital, Northwest Ethiopia. Clin Med Res 2: 110-120. Link: https://bit.ly/30Fi9cH
- Haastrup EA, Daki LO, Tijani A (2014) Family Support as Predictor of Adhernce to Diet Regimen among People with Type II Diabetes in Lagos State. IOSR J Nurs Heal Sci 3: 15-21. Link: https://bit.ly/2GJtRvQ
- Luo X, Liu T, Yuan X, Ge S, Yang J, et al. (2015) Factors Influencing Self-Management in Chinese Adults with Type 2 Diabetes : A Systematic Review and Meta-Analysis. Int J EnvironResPublic Heal 12: 11304-11327. Link: https://bit.ly/2SBjH2P
- Dixon JB, Browne JL, Mosely KG, Rice TL Jones KM, et al. (2013) Severe obesity and diabetes self-care attitudes, behaviours and burden: Implications for weight management from a matched case-controlled study. Results from Diabetes MILES-Australia. J Br Diabet Assoc 31: 111. Link: https://bit.ly/2GExmUz
- Mogre V, Abanga ZO, Tzelepis F, Johnson NA, Paul C (2017) Adherence to and factors associated with self-care behaviours in type 2 diabetes patients in Ghana. BMC Endocr Disord 17: 1-8. Link: https://bit.ly/2SBg8K5
- Shamsi N, Shehab Z, AlNahash AZ, AlMuhanadi S, Al-Nasir F, et al. (2013) Factors Influencing Dietary Practice Among Type 2 Diabetics. Bahrain Med Bull 35: 1-14. Link: https://bit.ly/36Gr5lS
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
