Global Journal of Medical and Clinical Clinical Image
An unusual presentation of a secondary extramedullary plasmacytoma
Mahmoud Nujeidat1*, Yosssi Barshai2, Zamir M3, Novokhatko Galina1, Grisko Olga4, Livoff A4 and Zamir D1*
2Hematology department, Barzilai medical center
3Department of dermatology Hadassah Ein Karem, Jerusalem
4Pathology Institute, Barzilai Medical center Ashkelon
Doron Levi Zamir, Internal Medicine Department D, Barzilai Medical Center, Ashqelon, Israel, Tel: +972537678940; E-mail: prof.doronzamir@gmail.com
Cite this as
Nujeidat M, Barshai Y, Zamir M, Galina N, Olga G, et al. (2022) An unusual presentation of a secondary extramedullary plasmacytoma. Glob J Medical Clin Case Rep 9(4): 068-070. DOI: 10.17352/2455-5282.000163Copyright License
© 2022 Nujeidat M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Introduction
Plasma cell dyscrasias are a group of entities characterized by neoplastic proliferation of a single clone of plasma cells, typically producing a monoclonal Immunoglobulin [1].
Plasmacytoma mostly arises in the bone marrow (intramedullary), presenting as either Multiple Myeloma (MM) or solitary plasmacytoma of bone [2].
In contrast, Extramedullary Plasmacytoma (EMP) is a rare entity, which accounts for about 3% of plasmacytomas [2].
In this case, we report a 76 old Israeli woman with an unusual presentation of extramedullary plasmacytoma.
Case description
Seventy-six-year-old Israel female of Russian origin with recently diagnosed multiple myeloma, diagnosed in the last year (April 2021-august 2021) after an investigation done for progressive renal failure (serum creatinine 3 mg /dl from a baseline of 1.5 mg /dl ) and proteinuria of 1500 mg per 24 hours, serum free light assay is positive for a high amount of lampda chain (5500 mg/l), Bone marrow biopsy revealed plasma cells 10% - 20%, PET scan done before initiation of therapy was negative for bone lesions or soft tissue involvement.
She was treated with CyBorD (Cyclophosphamide + Bortezomib + Dexamethasone) Chemotherapy Regimen for Multiple Myeloma Her response included normalization of serum creatinine (1.5 mg/dl) and a normal PET scan.
Our patient was presented to the emergency room in September 2021 after several days of vomiting and diarrhea.
Vital signs were: BP 126/68, Sat 96% on room air, pulse 91 per minute, Temperature 36.9 c.
On physical examination: diffuse abdominal tenderness was palpable and an abdominal mass was found in the right lower quadrant.
Labs show significant renal failure (creatinine 6 mg/dl, baseline of 1.5 mg/dl) without an increase in inflammatory indices.
An abdominal X-Ray was performed and is presented in Figure 1.
The patient was examined by a surgeon that ruled out an acute abdomen.
At this point the leading diagnosis was gastroenteritis with pre-renal failure therefore the patient was treated with fluids and stool cultures were taken.
Two days later Stool culture grew salmonella and Empiric treatment with ceftriaxone was initiated.
Not improving to supportive therapy (still with a high level of serum creatinine) the patient was scheduled for non-contrast tomography to exclude other etiologies for renal function deterioration.
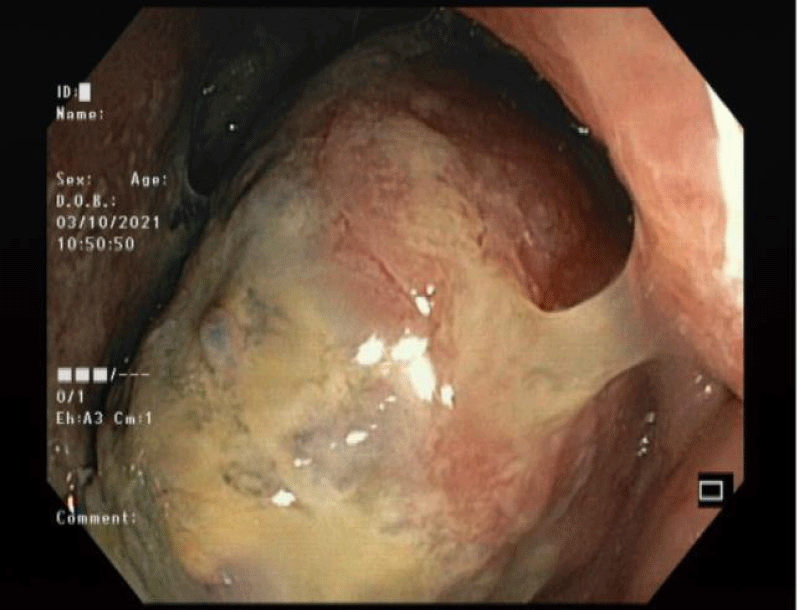
Ct without contrast revealed some unexpected features such as a moderate quantity of ascites and a huge mass in ascending colon with near total bowel obstruction (Figure 2). Colonoscopy was compatible with a large mass in the right colon (Figure 3).
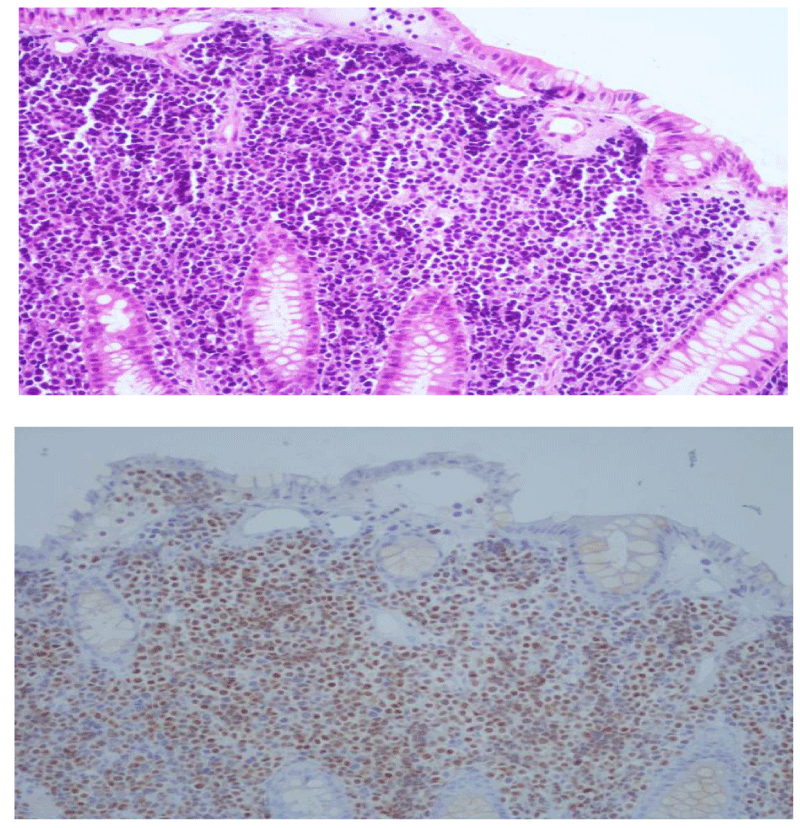
Figure 4 is showing lamina propria expansion by uniform atypical plasma cells, Figure 5 is immunostain plasma cells.
Our patient underwent right hemicolectomy and hemodialysis due to oliguria and high serum creatinine not improving to supportive treatment, unfortunately, we could not investigate more about the reasons for renal function deterioration and exclude renal etiologies such as nephrotic syndrome or tubular injury, renal biopsy was considered but not possible after rapid progress of events and hemodynamic instability due to sepsis resistant to antibiotic therapy which leads to the death of the patient.
Discussion
Multiple Myeloma (MM) represents 1%-2% of all cancers in the USA with an annual incidence of 4.3 per 100,000 [3].
Two-thirds of patients are male [4].
Plasmacytoma is a malignant tumor that is characterized by monoclonal proliferation of plasma cells, mostly arising in the bone marrow (intramedullary), presenting as the multiple myeloma (MM) or solitary plasmacytoma of bone. In contrast, Extramedullary Plasmacytoma (EMP) which arises from soft tissues is a rare entity, accounting for about 3% of the plasmacytoma [2].
The presence of soft-tissue plasmacytomas represents an aggressive form of MM, characterized by the ability of a clone and/or subclone to thrive and grow independent of the bone marrow microenvironment [5].
The etiology of plasmacytoma is unknown. However, it is suggested that EMP may be caused by inhalation of chemicals, chronic stimulation, an overdose of irradiation, viral infection, and genetic disorders in the reticuloendothelial system [6].
The most common sites of EMD occurrence were skin/muscle (24%), pleura (12%), lymph nodes (10%), liver (9%) and CNS (6%) [7].
The involvement of the gastrointestinal tract years after an initial diagnosis of multiple myeloma (MM) is exceptional and, when reported, it is always associated with a poor prognosis [8,9].
The most common site is the small intestine followed by the stomach; the colorectal incidence is very uncommon [10].
Involvement of the colon and rectum is extremely rare and so far only 20 cases of extramedullary plasmacytoma of the colon and rectum have been reported in the literature.
After making systematic inquiries on PubMed from 2010 to now, about 22 case reports of primary gastrointestinal EMPs were reported, including 7 in the stomach, 2 in the duodenum, 1 in the small bowel, 3 in the ileocecum, 1 in the appendix, 6 in the colon and 2 in rectum [11].
GI manifestations depend on the organ involved but generally result from direct organ invasion leading to perforation in cases of hollow viscus involvement, mechanical mass effects leading to obstruction, and, rarely, the development of ascites [8].
There is still no unified guideline for the treatment of gastrointestinal EMP because of its rarity. Though plasma cell tumors are highly radiosensitive, surgical resection has been proposed as the first choice for gastrointestinal EMP [12].
Conclusion
Plasmacytoma is considered very rare, especially with gastrointestinal involvement and the number of cases mentioned in the medical literature is limited.
The second aspect important to emphasize is that the involvement of the gastrointestinal tract is usually associated with a poor prognosis.
It’s true we could not associate the death of the patient just due to multiple myeloma but we believe that the disease and the rapid progress of events such as surgery and hemodialysis is a very important factor that caused immunocompromising and eventually dying due to sepsis.
- Wahed A, Dasgupta A. Hematology and Coagulation (Second Edition). 2020.
- Strojan P, Soba E, Lamovec J, Munda A. Extramedullary plasmacytoma: clinical and histopathologic study. Int J Radiat Oncol Biol Phys. 2002 Jul 1;53(3):692-701. doi: 10.1016/s0360-3016(02)02780-3. PMID: 12062614.
- Siegel RL, Miller KD, Jemal A. Cancer statistics, 2018. CA Cancer J Clin. 2018 Jan;68(1):7-30. doi: 10.3322/caac.21442. Epub 2018 Jan 4. PMID: 29313949.
- Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2018 Nov;68(6):394-424. doi: 10.3322/caac.21492. Epub 2018 Sep 12. Erratum in: CA Cancer J Clin. 2020 Jul;70(4):313. PMID: 30207593.
- Liu Y, Jelloul F, Zhang Y, Bhavsar T, Ho C, Rao M, Lewis NE, Cimera R, Baik J, Sigler A, Sen F, Yabe M, Roshal M, Landgren O, Dogan A, Xiao W. Genetic Basis of Extramedullary Plasmablastic Transformation of Multiple Myeloma. Am J Surg Pathol. 2020 Jun;44(6):838-848. doi: 10.1097/PAS.0000000000001459. PMID: 32118627; PMCID: PMC7225029.
- Gholizadeh N, Mehdipour M, Rohani B, Esmaeili V. Extramedullary Plasmacytoma of the Oral Cavity in a Young Man: a Case Report. J Dent (Shiraz). 2016 Jun;17(2):155-8. PMID: 27284562; PMCID: PMC4885674.
- Bladé J, Fernández de Larrea C, Rosiñol L, Cibeira MT, Jiménez R, Powles R. Soft-tissue plasmacytomas in multiple myeloma: incidence, mechanisms of extramedullary spread, and treatment approach. J Clin Oncol. 2011 Oct 1;29(28):3805-12. doi: 10.1200/JCO.2011.34.9290. Epub 2011 Sep 6. PMID: 21900099.
- Talamo G, Cavallo F, Zangari M, Barlogie B, Lee CK, Pineda-Roman M, Kiwan E, Krishna S, Tricot G. Clinical and biological features of multiple myeloma involving the gastrointestinal system. Haematologica. 2006 Jul;91(7):964-7. PMID: 16818286.
- Varettoni M, Corso A, Pica G, Mangiacavalli S, Pascutto C, Lazzarino M. Incidence, presenting features and outcome of extramedullary disease in multiple myeloma: a longitudinal study on 1003 consecutive patients. Ann Oncol. 2010 Feb;21(2):325-330. doi: 10.1093/annonc/mdp329. Epub 2009 Jul 24. PMID: 19633044.
- Ding W, Tan Y, Qian Y, Xue W, Wang Y, Xi C, Gu K, Xu Y, Xu X. Primary plasmablastic plasmacytoma in the stomach of an immunocompetent adult: A case report. Medicine (Baltimore). 2019 Jan;98(4):e14235. doi: 10.1097/MD.0000000000014235. PMID: 30681607; PMCID: PMC6358359.
- Lin QT, Cai XR. Extramedullary plasmacytoma involving rectum: A case report and literature review. Radiol Case Rep. 2021 Jan 26;16(4):785-788. doi: 10.1016/j.radcr.2021.01.023. PMID: 33537109; PMCID: PMC7841224.
- Miwa W, Hiratsuka T, Tei S, Sato K, Yo K. Solitary extramedullary plasmacytoma of the rectum complicating ulcerative colitis. Clin J Gastroenterol. 2019 Apr;12(2):160-165. doi: 10.1007/s12328-018-0907-8. Epub 2018 Sep 20. PMID: 30238285.

Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.



 Save to Mendeley
Save to Mendeley
