Global Journal of Medical and Clinical Case Report
Association of ulcerative colitis and IgA nephropathy: A case report
S Boulajaad1*, M Haida1, Ait Errami1, S Oubaha2, Z Samlani1 and K Krati1
2Laboratory of physiology, Faculty of Medicine, University Cadi Marrakech, Morocco
Cite this as
Boulajaad S, Haida M, Errami A, Oubaha S, Samlani Z, et al. (2021) Association of ulcerative colitis and IgA nephropathy: A case report. Glob J Medical Clin Case Rep 8(3): 105-107. DOI: 10.17352/2455-5282.000140Copyright
© 2021 Boulajaad S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.The extradigestive manifestations of chronic inflammatory bowel disease most often affect the articulations, skin, eyes, liver and bile ducts. Renal involvement is rare, and manifests as kidney stones, glomerulonephritis, tubulointerstitial nephritis, and secondary amyloidosis. In this context of chronic inflammatory bowel disease, in particular ulcerative colitis, renal involvement is very often secondary to nephrotoxicity of the basic treatment of digestive pathology, and very rarely an authentic extradigestive manifestation of intestinal disease.
We report a case of IgA nephropathy as an extra-digestive manifestation of ulcerative colitis.
The objective of this study is not to neglect the IgA nephtopathy as an extradigestive manifestation of IBD which, even though rare, remains a condition to be looked for by clinicians during the follow-up of IBD.
Introduction
Chronic Inflammatory Bowel Disease (IBD) is caused by different diseases and manifested of inflammation in different part of the digestive tract. These diseases evolve in inflammatory flares, of varying duration, intensity and frequency depending on the patient, alternating with phases of remission. Extradigestive manifestations can affect virtually any organ. The most frequent attacks are articulations, skin, eye, liver and bile duct damage. They are present in 6 to 46% of patients. Certain genetic, infectious and immunological factors could intervene in their physiopathological mechanism [1,2]. Renal and urinary tract damage represent, according to the authors, 4 to 23% of cases. The most frequent attacks are renal lithiasis, glomerulonephritis, tubulointerstitial nephritis and type AA secondary amyloidosis [3]. We report the case of a 46 years old male followed in the department of gastroenterology of university Hospital Center Mohamed VI of Marrakech for an ulcerative rectocolitis associated with a secondary spondyloarthropathy, put on 5 amino-salicylates and Azathioprine as a basic treatment, who presented an elevated proteinuria during a check-up, with a renal biopsy puncture which is in favor of IgA nephropathy.
Case report
This is a 46-year-old patient, without any particular medical history, followed in the department of gastroenterology of university Hospital Center Mohamed VI of Marrakech since 2014 for ulcerative colitis in pancolitis. The pathology has been revealed by mucous-bloody diarrhea at a rate of 4 stools per day associated with rectal syndrome, and inflammatory polyarthralgia of the large articulations and the sacroiliacs, with inflammatory syndrome on biology and endoscopy.
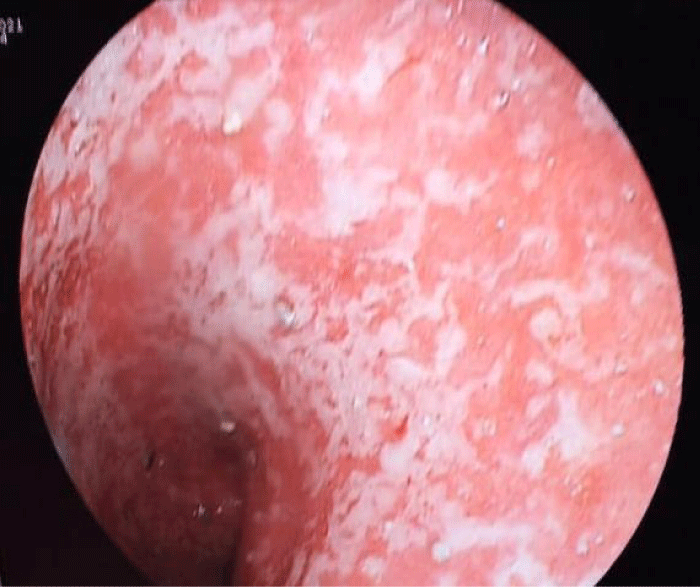
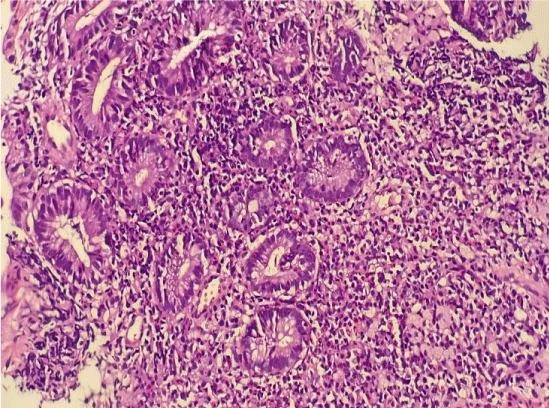
A colonoscopy was performed objectifying a fragile and erythematous mucosa up to the right colic angle, bleeding on contact with rectal ulcerations (Figure 1). Histology revealed an ulcerated surface coating, detached, glandular dedifferentiation, decrease in mucosecretion, cryptic abscess, congestive chorion, inflammatory (Figure 2).
The management consisted of putting the patient initially on oral and rectal 5 amino-salicylates (5 ASA) (Sulfasalazine 3g / day , switched to 6-Mercaptopurine (Purinethol 1.5 mg / kg / day) + 5ASA as treatement of maintenance in the face of non-response to treatment, then to Adalimumab in the face of clinical non-improvement.
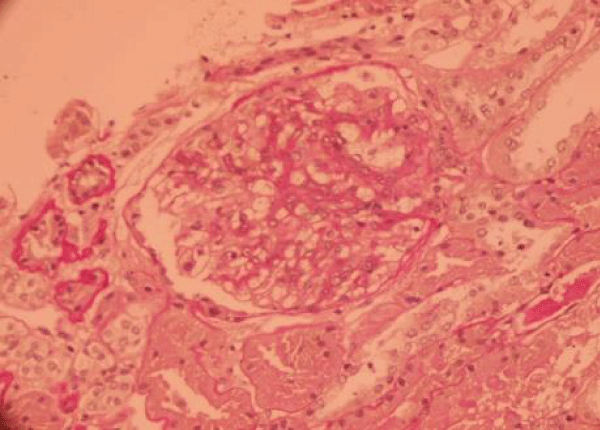
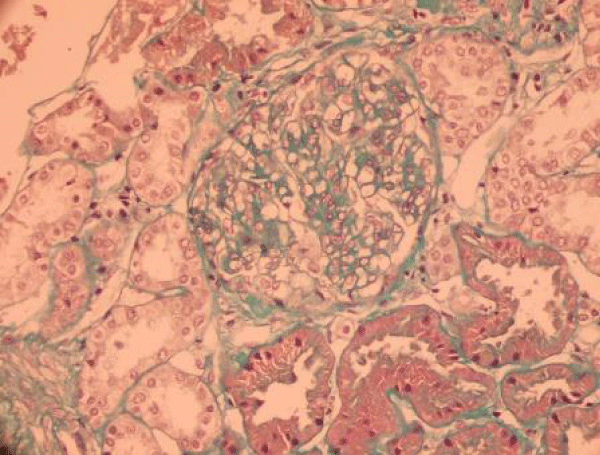
During a check-up of his treatment,the proteinuria was raised to 0.84g/24h, with a correct renal function, a renal puncture biopsy was carried out objectifying deposits of IgA and C3 in moderate number pareto- mesangial, IgA glomerulonephritis with signs of weak chronicity and proliferative glomerulus (Figures 3,4).
Discussion
The onset of renal failure in a patient treated for IBD suggests primarily drug nephrotoxicity. The nephrotoxicity of IBD treatments is known and well described, in particular with 5-ASA, cyclosporin A and antiTNF-alpha. But the pathophysiological mechanism has not yet been elucidated.
The NEPHROPATH group in the United States carried out a study of 33,173 native kidney biopsies taken between March 2001 and June 2012, including 83 in patients with IBD [4]. In these 83 patients with IBD, the main indications for biopsies were: acute renal failure, chronic renal failure and proteinuria. IgA nephropathy was the most common diagnosis, present in 20 patients, followed by interstitial nephritis which affected 16 of 83 patients, and nephroangiosclerosis which affected 10 of 83 patients. AA amyloidosis was diagnosed in one patient, acute tubular necrosis in 7 patients, and other kidney damage ranged from proliferative glomerulonephritis to minimal glomerular damage. Regarding treatment, 28 patients had a history of treatment with 5-ASA and 8 patients with anti-TNF-alpha. In this study, it was not clear whether the occurrence of IgA nephropathy in ulcerative colitis was different from that in Crohn’s disease. Thus the prevalence of IgA nephropathies was significantly higher in patients with IBD than in patients without IBD [5].
The first case of IgA nephropathy associated with IBD was described in 1984 by Hubert, et al. [6]. Data in the literature suggest that the condition manifests as non-nephrotic proteinuria and hematuria. Kidney damage most often occurs during a digestive tract and is, most of the time, regressive after treatment. The pathophysiological mechanisms explaining the association of IBD and IgA nephropathy are not fully understood. However, there appears to be an association between inflammation of the mucosa and dysregulation of IgA synthesis linked to T helper lymphocyte damage.
The pathophysiological link between IgA nephropathies and IBD remains to be elucidated, although some common mechanisms are believed to contribute to their inflammatory conditions. Abnormal helper T lymphocytes have been suggested to stimulate plasma cells in the bone marrow to secrete IgA1 polymers [7]. This claim is supported by Kett, et al. [8].Which showed a significant increase in IgA1-producing cells in colonic tissue from IBD patients.
Thus, the possible involvement of a common genetic factor; in particular the (HLA) -DR1 antigen has been the suspected factor that links IBD to IgA nephropathy [9,10]. However, further experiments are essential for the confirmation of these hypotheses.
With regard to toxic nephropathies, the review by Corica, et al. In 2016, summarizes the different nephrotoxicities of the treatments [11]. Treatment with 5-ASA, the first therapeutic approach in IBD, results in kidney damage in 1% of patients treated, the main lesion of which is tubulointerstitial nephritis, but the exact mechanism is not known. In addition, there was no evidence of an association between the dose, the duration of treatment and the development of renal impairment. Anti-TNF-alpha, also widely used in the management of IBD, known to have good results in the control of the disease on the digestive level, can also cause tubulointerstitial nephritis, the mechanism of which is not unclear, but several cases of interstitial nephritis have been reported in the literature in patients with IBD who lack any treatment. In 2002, Izzedine, et al. were the first to describe the onset of chronic interstitial nephritis in a patient with Crohn’s disease, diagnosed concurrently with his digestive disease [12]. In 2008, Waters, et al. report the case of tubulointerstitial nephritis in a 12-year-old child, newly diagnosed with IBD, not yet treated [13].
In addition, the production of tubular proteinuria is more related to disease activity than to a toxic cause [14].
These examples support the theory of kidney damage as an authentic extradigestive manifestation of IBD, and not secondary to nephrotoxic treatments.
It should be noted that during an outbreak of intestinal disease, IgA nephropathy worsens, in which treatment of intestinal disease with either immunosuppressive therapy or bowel resection is associated with clinical remission of IgA nephropathy [15].
Conclusion
Kidney damage in chronic inflammatory bowel disease is probably underestimated due to its silent and asymptomatic nature. Its screening must be systematic and regular in order to objectify nephropathy at an early stage.
I would like to thank the staff of Department of Hepato-Gastro-Enterology, CHU Mohammed VI Marrakech, to enable me to write this article.
- Treffel M, Champigneulle J, Meibody F, Laurain E, Frimat L, et al. (2019) Tubulointerstitiel nephritis and Crohn's disease, nephrotoxicity or extraintestinal manifestation of Crohn's disease? About a case. Néphrologie & Thérapeutique 15: 59-62. Link: https://bit.ly/39aCJp1
- Rothfuss KS, Stange EF, Herrlinger KR (2006) Extraintestinal manifestations and complications in inflammatory bowel diseases. World J Gastroenterol 12: 4819–4831. Link: https://bit.ly/2XpbmFI
- Pardi DS, Tremaine WJ, Sandborn WJ, McCarthy JT (1998) Renal and urologic complications of inflammatory bowel disease. Am J Gastroenterol 93: 504–514. Link: https://bit.ly/3AiFr7M
- Ambruzs JM, Walker PD, Larsen CP (2014) The histopathologic spectrum of kidney biopsies in patients with inflammatory bowel disease. Clin J Am Soc Nephrol 9: 265-270. Link: https://bit.ly/3CiETj6
- Ambruzs JM, Walker PD, Larsen CP (2013) The Histopathologic Spectrum of Kidney Biopsies in Patients with Inflammatory Bowel Disease CJASN ePress.
- Hubert D, Beaufils M, Meyrier A (1984) Immunoglobulin A glomerular nephropathy associated with inflammatory colitis. A propos of 2 cases. Presse Med 13: 1083–1085. Link: https://bit.ly/3kfUOZc
- Coppo R (2018) The gut-renal connection in IgA nephropathy. Semin Nephrol 38: 504–512. Link: https://bit.ly/39bEVwM
- Kett K, Brandtzaeg P (1987) Local IgA subclass alterations in ulcerative colitis and Crohn’s disease of the colon. Gut 28: 1013–1021. Link: https://bit.ly/3hCyTJQ
- Friedman BI, Spray BJ, Heise ER (1994) HLA associations in IgA nephropathy and focal and segmental glomerulosclerosis. Am J Kidney Dis 23: 352–357. Link: https://bit.ly/3lsP3XA
- Toyoda H, Wang SJ, Yang HY, Redford A, Magalong D, et al. (1993) Distinct associations of HLA class II genes with inflammatory bowel disease. Gastroenterology 104: 741-748. Link: https://bit.ly/3hzw4tm
- Corica D, Romano C (2016) Renal involvement in inflammatory Bowel diseases. J Crohns Colitis 10: 226–235. Link: https://bit.ly/3tOaNky
- Izzedine H, Simon J, Piette AM, Lucsko M, Baumelou A, et al. (2002) Primary chronic interstitial nephritis in Crohn’s disease. Gastroenterology 123: 1436-1440. Link: https://bit.ly/3nIqJDX
- Waters AM, Zachos M, Herzenberg AM, Harvey E, Rosenblum ND (2008) Tubulointerstitial nephritis as an extraintestinal manifestation of Crohn’s disease. Nat Clin Pract Nephrol 4: 693-697. Link: https://bit.ly/3nDX52E
- Poulou AC, Goumas KE, Dandakis DC, Tyrmpas I, Panagiotaki M, et al. (2006) Microproteinuria in patients with inflammatory bowel disease: is it associated with the disease activity or the treatment with 5-aminosalicylic acid? World J Gastroenterol 12: 739-746. Link: https://bit.ly/3Asu512
- Filiopoulos V, Trompouki S, Hadjiyannakos D, Paraskevakou H, Kamperoglou D, et al. (2010) IgA nephropathy in association with Crohn’s disease: a case report and brief review of the literature. Ren Fail 32: 523-527. Link: https://bit.ly/3hCIsc5

Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.
 Save to Mendeley
Save to Mendeley
