Global Journal of Medical and Clinical Short Communications
Acute Flaccid Paralysis surveillance in Gaza Strip, Palestine
Khaled A Abu Ali*
Cite this as
Abu Ali KA (2021) Acute Flaccid Paralysis surveillance in Gaza Strip, Palestine. Glob J Medical Clin Case Rep 8(2): 081-086. DOI: 10.17352/2455-5282.000135Acute Flaccid Paralysis (AFP) is a clinical syndrome characterized by rapid onset of weakness, in the respiratory muscles, swallowing and limbs; and death because of respiratory muscles failure.
AFP surveillance is crucial, the clinicians are required to notify AFP cases among children below 15 years old to the epidemiology department with completion of AFP surveillance form.
In this study, the researcher analyzed AFP surveillance investigation forms to determine the clinical picture, viral etiology and the incidence of AFP among children under 15 years.
Material and method (Study design): The research study conducted through cross sectional study, based on AFP investigation forms in the epidemiology department.
Results: The final diagnosis of the cases were as follow, 71.1% “27 cases” were GBS, 10.5 % were Encephalitis, 7.9% were Neuropathy, 2.6% “ one case only” for each of the following Aseptic meningitis, Transverse myelitis, Tuphus fever and Subspinal muscular atrophy.
The incidence rate among children less than 15 years old which range from 0.58 / 100.000 in 2006 to 1.2 / 100.000 in 2012; Most of the cases 89.5 % had fully vaccinated and 10.5% had not fully vaccinated due to their ages less than one year, 65.8 “25 cases” had residual weakness, all of the cases classified as discarded according to the expert committee decision; no one case dead, all of the samples sent to the Tal-Hashomir laboratory in the occupied land in 1948 for viral isolation; most of the results 81.6% revealed that no virus isolated, 11.8% isolated ECHO virus, 2.6% isolated Coxsachie virus and 4 % isolated NPEV.
Conclusion: No wild polio virus in Palestine which is polio free since 1984 and certified in 2006, our success being attributed to: start of 2 doses of IPV and 5 doses of OPV since 1978, high immunization coverage more than 95% at district level and effective AFP surveillance system in Palestine. The study recommended to encourage polio immunization and all clinicians are required to report all AFP cases and submitting at least two stool samples to the epidemiology department (at least 24 hours apart within 14 days of onset of paralysis).
Introduction
Acute Flaccid Paralysis (AFP) is a clinical syndrome characterized by rapid onset of weakness, in the respiratory muscles, swallowing and limbs; and death because of respiratory muscles failure.
Surveillance for AFP is an important as it consider as a key strategy used by the Global Polio Eradication Initiative by the World Health Organization [1].
According to WHO’s strategy the countries required to survey the AFP cases in order to combat the Poliomyelitis using a standard case definition.
Active AFP cases surveillance in children under 15 years is ongoing till reaching eradication of Poliomyelitis in the globe; so, monitoring of wild polioviruses importation into the non-polio endemic countries is a must.
AFP is caused by many conditions, including viral infections including poliomyelitis, transverse myelitis and Guillain Barre syndrome (GBS) in addition to trauma and metabolic neuropathies.
Non-Polio Enteroviruses (NPEV) causing paralysis, and its` less severe than poliomyelitis.
But in poliomyelitis, anterior horn cells of spinal cord invaded by poliovirus this may lead to limbs asymmetrical weakness and no sensory symptoms.
AFP surveillance is crucial, the clinicians are required to notify AFP cases among children below 15 years old to the epidemiology department with completion of AFP surveillance form.
Two fresh stool specimens to be collected 24 hours apart within 14 days of onset of paralysis and to be sent to the Tal-Hashomir laboratory which accredited by WHO in the occupied land in 1948.
In this study, the researcher analyzed AFP surveillance data from January 2006 to December 2012, to determine the viral etiology, clinical picture and incidence of AFP among children under 15 years old.
Epidemiology of poliomyelitis
Infectious agent: The polioviruses belong to the genus Enterovirus from Picornaviridae family and comprise three related serotypes: types 1, 2, and 3, all of which can cause paralysis. The poliovirus is inactivated by ultraviolet light, chlorine and heat. Poliovirus type 1 causing most of the epidemics.
Occurrence: Daily, more than 1000 paralysis cases among children were reported in 1988, it was primarily in South Asia and Africa.
The disease considered as seasonal disease, commonly occur in summer and early autumn.
In the low immunization coverage countries such as developing countries, the virus led to more significant disability, illness death. As reported, five to ten cases every 1000 cases will develop paralytic disease.
WHO have been certified Palestine polio free in 2006, in Palestine the latest poliomyelitis reported case was in 1984 and in Gaza it was in 1981, this certification was a result of demonstrating the recommended strategies by the WHO.
Transmission
The virus transmitted from person-to-person through the fecal-oral route. Through feces the virus spread after multiplying in the intestines, after infection the virus excreted for two months or more but the maximal amount excreted just before paralysis and during the first fourteen days after paralysis onset. The incubation is seven to ten days with range extended from 4-35 days.
Reservoir
The unique reservoir of the virus is human only. Some studies reveled that small amount of wild poliovirus persist in very cold water for a period extended to months, in tropical climates the virus can survive for a few days only.
Communicability
The Poliovirus considered as one of the high communicable viruses, one week before and 2 weeks after onset of paralysis the infected ones can be highly infectious to all household and close contacts especially in poor sanitation areas.
Immunity
Any non-immunized person considers susceptible to infection. According to literatures any infant born to mother have antibodies against the virus the infant will be protected against paralytic polio naturally for a few weeks.
Infection with wild Poliovirus and/ or the immunization leading to obtaining of immunity against the disease, the vaccination of Oral Polio Vaccine “OPV” resulting in both local intestinal cellular and humoral responses this immunity may persist for years and lead break of chain of infection.
The immunization with inactivated Poliovirus Vaccine “IPV” confers humoral immunity with less intestinal immunity, the IPV does not provide resistance to carriage and spread of wild polio virus in the community.
Immunization: According the national vaccine preventable diseases schedule
Case definition of Acute Flaccid Paralysis & Poliomyelitis
Acute Flaccid Paralysis: Acute onset of a flaccid paralysis of one or more groups of muscles with decreased or absent tendon reflexes in the affected muscles, without other apparent cause, and without sensory or cognitive loss.
All diagnosed cases must be investigated to exclude Poliomyelitis as one of WHO requirements for Poliomyelitis eradication goal.
Poliomyelitis and AFP cases consider from group A diseases in the Palestinian surveillance system and to be immediately to the epidemiology department.
Poliomyelitis
Acute diseases caused by wild poliomyelitis viruses characterized by acute onset of a flaccid paralysis of one or more groups of muscles with decreased or absent tendon reflexes in the affected muscles, without other apparent cause and without sensory or cognitive loss; One confirmed polio case must be considered as an outbreak.
Case definition
Suspected case: Any case of Acute-Onset Flaccid Paralysis (AFP), including Guillain-Barré syndrome, in a person under 15 years of age for any reason other than severe trauma.
Confirmed case: A case with acute paralytic illness, with or without residual paralysis, and isolation of wild poliovirus from the stools of either the case or its contacts.
Polio-compatible case: A case in which one adequate stool specimen was not collected from a case within 2 weeks of the onset of paralysis, and there is either an acute paralytic illness with polio-compatible residual paralysis at 60 days, or death takes place within 60 days, or the case is lost to follow-up.
Vaccine-Associated Paralytic Poliomyelitis case “VAPP”: A case with acute paralytic illness in which vaccine-like poliovirus is isolated from stool samples, and the virus is believed to be the cause of the disease. There are two possible types of Vaccine-Associated Paralytic Poliomyelitis (VAPP):
(A)- Recipient: A person who has onset of AFP 4 to 40 days after receiving OPV and has neurological sequelae compatible with polio 60 days after the paralysis began.
(B)- Contact: A person who has residual paralysis 60 days after the onset of AFP had contact 4 to 40 days before the paralysis began with a person who received OPV somewhere between 4 and 85 days before the contact’s paralysis began.
Discarded (Not Poliomyelitis) case: A case with acute paralytic illness for which one adequate stool specimen was obtained within 2 weeks after onset of paralysis and was negative for poliovirus.
Materials and methods
Study design
The research study conducted through cross sectional study, based on AFP investigation forms in the epidemiology department.
Sample
Between January 2006 and December 2012 Tal-Hashomir laboratory in the occupied land in 1948 received 76 stool specimens from 38 reported AFP cases sent from hospitals throughout Gaza strip.
The specimens were accompanied by an AFP notification form with details of patient personal and clinical history.
All stool specimen kept under deep freezing in the epidemiology department till sent to the laboratory after coordination through WHO.
All AFP reported cases were followed up after 60 days for clinical assessment to ascertain residual paralysis.
Results & discussion
The AFP surveillance system provides a sensitive tool for investigating AFP cases in children, with careful clinical evaluation of the differential diagnosis and expert review of cases. Accurate diagnosis requires a precise knowledge of the etiology and underlying pathophysiology. Analysis of the clinical findings and diagnosis reported for the 38 cases in this study showed that the underlying causes were diverse.
During the period of this study, 38 AFP cases below age 15 years were reported to our department Table 1.
Demographic related variable showing that most of the cases were male 71.1% “27 case” & 28.9 were female.
36.8% “ 14 case” of the cases were living in Gaza governorate, 26.3% “10cases” were living in North Gaza governorate, 21.1% “8cases” were living in Khanyounis and the rest of the case in Rafah & Mid-zone 3 cases for each.
In relation to age category most of the cases 73.7% “28 case” their ages in between 1-9 years, 4 cases “10.5% below one year and 15.8% “6 cases” more than 10 years up to 15 years.
Table “2” showing the clinical related variables in which the primary diagnosis of the cases were 28.9 % “11” cases diagnosed as AFP, 21.1% “8 cases” diagnosed as GBS, and the rest of the cases diagnosed as Inability to walk 16%, Poly neuropathy 2.6% “one case” and Hemiparesis, Quadriparesis, Quadriplegia and paraplegia 7.9% “3 cases” for each;
94.7% “36 case” complained from rapid progression of the paralysis; 92.1 % complained from floppy paralysis; 52.6 % complained from fever with onset of paralysis while 47.4% did not complain.
Most of the cases 71.1 % did not complain from asymmetric paralysis; Most of the cases 81.6 % did not complain from Sensory nerve loss; More than half of the cases 57.9% “22 case” complained from both lower limb paresis & / or plegia.
The final diagnosis of the cases were as follow, 71.1% “27 cases” were GBS, 10.5 % were Encephalitis, 7.9% were Neuropathy, 2.6% “ one case only” for each of the following Aseptic meningitis, Transverse myelitis, Tuphus fever and Subspinal musculae atrophy.
Gullain Barre Syndrome (GBS) accounted for 71.1% “27/38 cases” of AFP cases in this study. In the absence of wild poliovirus induced poliomyelitis, GBS is the most common cause of AFP reported in many parts of the world, accounting for over 50% in many industrialized and developing countries [2].
A study of AFP surveillance in Malaysia, data from 1997 to 2001 showed that GBS was found in 30.2% of AFP cases, with an annual incidence of 0.36% [3].
The majority of GBS cases in the AFP surveillance were diagnosed based on typical clinical features, such as progressive ascending and symmetrical paralysis of the limbs with Table 3.
In this table its` clear that most of the cases 89.5 % “34 case” had fully vaccinated and 10.5% “4 cases only “ had not fully vaccinated due to their ages less than one year Table 4.
This table showing that no one case have travelled abroad one month prior the disease occurrence Table 5.
This table showing the incidence rate per 100.000 among children less than 15 years old which range from 0.58 / 100.000 in 2006 to 1.2 / 100.000 in 2012 Tables 5.1, 5.2.
This may not indicate the actual incidence of AFP, as many cases may not have been reported to epidemiology department for further investigation.
Since AFP notification is part of the poliomyelitis eradication exercise some cases may have been omitted when a definite diagnosis by history, for example trauma, did not indicate the need for laboratory investigation at the time of clinical assessment [4-8].
In this table it appears that about half of the cases 47.4 % “18 /38” notified about the cases to the epidemiology department by El-Nasser pediatric hospital Table 6.
In this table it appear that all of the cases 100% “38 case” were followed up by the epidemiology staff and the clinicians;
65.8 “25 cases” had residual weakness and 34.2 % had no residual weakness;
All of the cases classified as discarded according to the expert committee decision;
No one case died 0.0 % “ 0/38 case” during the disease and the follow up period Table 7.
Table “7” shows that all of the samples 100 % “76/76 sample” sent to the laboratory for viral isolation;
Most of the results 81.6% ‘62 /76 sample” revealed that no virus isolated, 11.8% “9/76 samples” isolated ECHO viruses, 2.6% “2/76 samples” isolated Coxsachie virus and 4 % “3 / 76 sample” isolated NPEV [8-13].
Since 1984, no wild poliovirus has been identified; our success being attributed to: start of 2 doses of IPV and 5 doses of OPV since 1978, high immunization coverage more than 95% at district level and effective AFP surveillance system in Palestine.
High quality of AFP surveillance requires
• The ability to detect at least one case per year of non-polio AFP for every 100,000 children under 15 years of age.
• Two adequate stool specimens collected from at least 80% of cases of AFP.
• All stool specimens should be processed at the Tal-Hashomir laboratory the WHO accredited laboratory in the occupied Palestinian land in 1948.
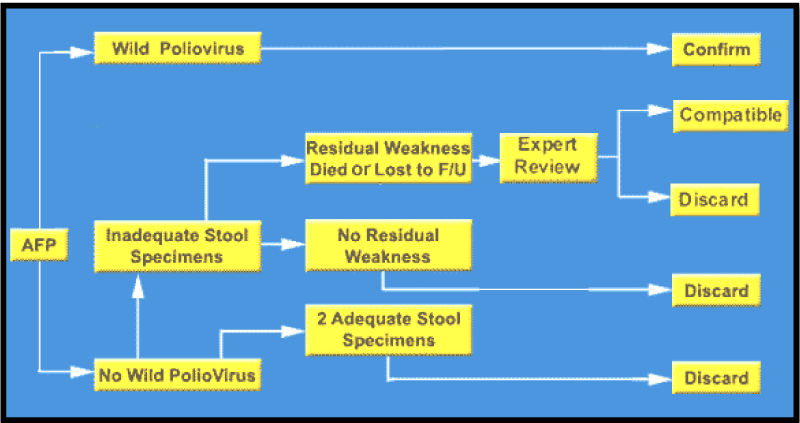
Virologic classification scheme
Conclusion
Despite the global great reduction in the number of poliomyelitis cases following the Global WHO Poliomyelitis Campaign, AFP continues to be an important neurological presentation in children.
The list of underlying causes of AFP is broad and complex. Clinicians need to have a detailed knowledge of the differential diagnosis to ensure effective and timely management. The current surveillance program provides a sensitive tool for investigating AFP cases with careful clinical evaluation of the differential diagnosis and expert review of cases. It is therefore crucial that AFP surveillance be conducted even in the absence of wild poliovirus transmission.
All polio eradication strategies should continue to be effectively implemented if we must preserve the current status of polio eradication in Palestine.
Polio continues to be reported in a number of regions throughout the world specially Easter Mediterranean region countries.
Until polio eradication has been globally achieved polio virus could be imported into Palestine.
Currently, AFP surveillance in Gaza is inadequate (range in between “2006-2012” 0.58-1.2 /100,000 population among children < 15 years of age) which reveal improvement of the surveillance system in 2012 1.2/100.000, which meets WHO standards.
Ensuring high quality AFP surveillance and high immunization coverage rates are necessary to maintain polio-free status, to rapidly identify importation of polio cases and respond quickly in the event that polio importation does occur.
All clinicians are encouraged to
• Report all cases of AFP among children < 15 years of age.
• Submit at least two stool samples to the epidemiology department (at least 24 hours apart within 14 days of onset of paralysis).
• Encourage polio immunization.
No national laboratory for primary poliovirus isolation and identification in Palestine, which consider as obstacle to the Palestinian health care system.
The authors acknowledge and appreciate the assistance of the Palestinian Ministry of Health for their support, assistance and facilitation of data collection.
- World Health Organization (1988) World Health Assembly. Global eradication of poliomyelitis by the year 2000 (WHA resolution no. WHA 41.28). Geneva; World Health Organization. Link: https://bit.ly/2Vwnhjy
- Marx A, Glass JD, Sutter RW (2000) Differential diagnosis of acute flaccid paralysis and its role in poliomyelitis surveillance. Epidemiol Rev 22: 298-316. Link: https://bit.ly/3irE9Rt
- Hussain IHMI, Ali S, Sinniah M, Kurup D, Khoo TB, et al. (2004) Five year surveillance of acute flaccid paralysis in Malaysia. J Ped Child Health40: 127-130. Link: https://bit.ly/3iu2SF0
- Duhair M, Abu Ali K (2011) National Guideline for Communicable Diseases Surveillance. 1ST edition, Palestine.
- MOH (2006) Palestinian Ministry of Health, Health Annual Report. 2006, Gaza Strip. Link: https://bit.ly/3lywMty
- MOH (2007) Palestinian Ministry of Health, Health Annual Report. 2007, Gaza Strip. Link: https://bit.ly/3lxVgTL
- MOH (2008) Palestinian Ministry of Health, Health Annual Report. 2008, Gaza Strip. Link: https://bit.ly/3lzlPrx
- MOH (2009) Palestinian Ministry of Health, Health Annual Report. 2009, Gaza Strip. Link: https://bit.ly/3Cn62C3
- MOH (2010) Palestinian Ministry of Health, Health Annual Report. 2010, Gaza Strip. Link: https://bit.ly/3AhrWFi
- MOH (2011) Annual Epidemiology Report. 2011, Gaza Strip. Link: https://bit.ly/37l3LcB
- Saraswathy TS, Zahrin HN, Apandi MY, Kurup D, Rohani J, et al. (2008) Acute Flaccid Paralysis Surveillance: Looking Beyond The Global Poliomyelitis Eradication Initiatives. Southeast Asian J Trop Med Public Health 39: 1033-1039 Link: https://bit.ly/37lyJkI
- Solomon T, Wilson H (2003) Infectious causes of acute flaccid paralysis. Curr Opin Infect Dis16: 375-381. Link: https://bit.ly/3fxhXnh
- World Health Organization (2008) Global Polio Eradication Initiative Report. Geneva: World health Organization. Link: https://bit.ly/3lDq6ua

Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.
 Save to Mendeley
Save to Mendeley
