Global Journal of Medical and Clinical Case Reports
Subvesical duct and hepaticocholecystic duct in one patient
Moon Soo Choi* and Heenkenda Kotakadeniya
Cite this as
Choi MS, Kotakadeniya H (2021) Subvesical duct and hepaticocholecystic duct in one patient. Glob J Medical Clin Case Rep 8(1): 028-030. DOI: 10.17352/2455-5282.000121Subvesical bile ducts (formerly known as “Ducts of Luschka”) are a rare entity associated with bile leaks due to their proximity to the gallbladder bed.
Failure to recognise their presence could lead to life-threatening complications to the patient in the form of an abdominal collection, biliary peritonitis and sepsis.
We describe a patient with two abnormal ducts found in the gallbladder fossa which were managed surgically.
Introduction
Laparoscopic cholecystectomies are one the most common operations performed electively and emergently by general surgeons especially in the context of a Western diet and lifestyle. However, it is not without its risks with a reported 0.3% major bile duct injury rate and 1.5% of patients complicated by a bile leak [1].
A significant risk factor for bile leaks is the presence of subvesical bile ducts (or “Ducts of Luschka”) as they are easily damaged and, especially if unrecognised intra-operatively, can lead to biliary peritonitis [2].
Schnelldorfer, et al. in 2012 recommended against the use of the term “Ducts of Luschka” but suggested they should rather be called subvesical ducts and they be classified into 4 types. Type 1 and 2 subvesical bile ducts do not empty into the gallbladder itself but rather superficially or in close proximity to the gallbladder fossa. Type 3 is a bile duct that drain directly into the gallbladder. Type 4 is a network of small bile ducts in the connective tissue of the gallbladder fossa [3].
We describe a case of a patient with two subvesical bile ducts – 1) a type 2 accessory subvesical bile duct draining into the right hepatic duct and 2) a type 3 hepatico-cholecystitic duct draining segment 6 of the liver into the gallbladder.
Case presentation
A 51-year-old lady was referred to the surgical outpatients with an eight-month history of biliary colic. She described having occasional upper abdominal pain with food and an ultrasound showed cholelithiasis but a normal common bile duct calibre. Her liver function tests only mildly deranged with a bilirubin of 33. This was on an unremarkable medical and surgical background.
She underwent an elective laparoscopic cholecystectomy. The patient and the ports were placed in the American-style of cholecystectomy. A critical view of safety was achieved with the cystic duct and common bile duct identified and dissected. A routine intra-operative cholangiogram was done which noted sludge in the common bile duct but no other abnormalities (Figure 1). The sludge was flushed with saline.
The cystic duct and cystic artery were clipped and ligated.
Upon further dissection of the gallbladder bed, two tubular structure were noted. One being on the more right lateral aspect of the gallbladder bed and the other being on the medial aspect of the gallbladder. These two structures did not look to be related in any way.
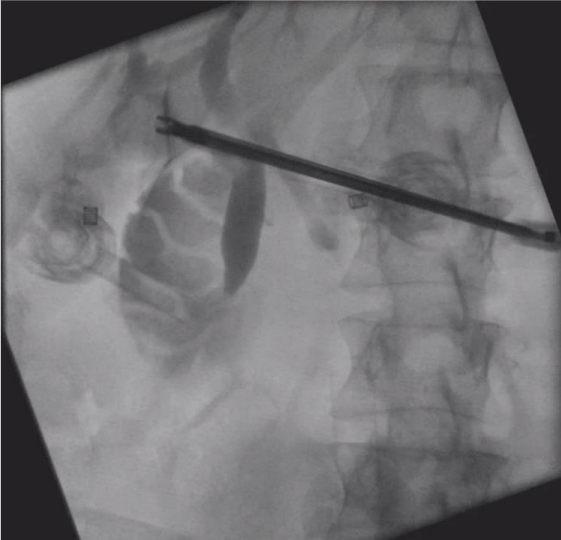
The more lateral tubular structure had inadvertently been damaged. An intra-operative cholangiogram was performed through this damaged structure (Figure 2). This showed this structure was a duct draining segment 6 of the liver.
The decision was made to abandon the operation with a drain in place over the damaged duct Figure 3.
The patient underwent a Magnetic Resonance Cholangiopancreatography (MRCP) the next day which noted the tubular structure on the medial aspect of the gallbladder was an accessory duct draining into the right hepatic duct. The damaged posterior duct was not well-visualised on the MRCP.
There was minimal output from the drain.
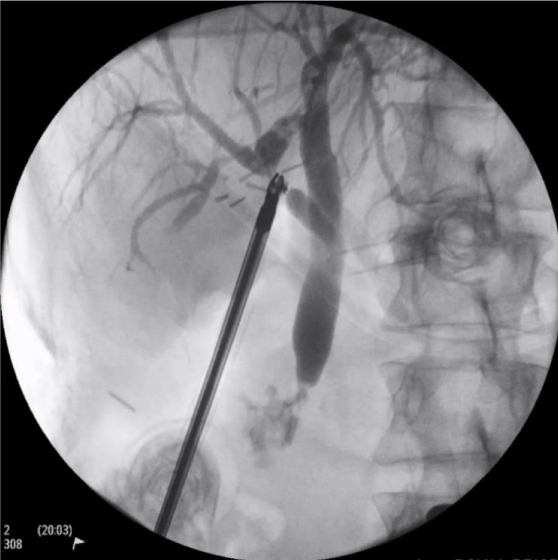
The patient was transferred to a tertiary hepatobiliary surgery unit where the patient underwent a laparoscopy through the same surgical sites as previous. The accessory bile duct on the medial aspect of the gallbladder was identified and a ductotomy and an intra-operative cholangiogram was performed (Figure 4). This confirmed this was an accessory cystic bile duct draining from the right hepatic bile duct at the bifurcation of the anterior and posterior ducts. This was clipped and ligated.
The damaged abnormal duct on the lateral aspect of the gallbladder draining segment 6 was clipped and ligated. The gallbladder was dissected off the gallbladder bed with no further abnormal structures being found. The subhepatic drain did not produce any bilious content so the drain was removed, and the patient was discharged.
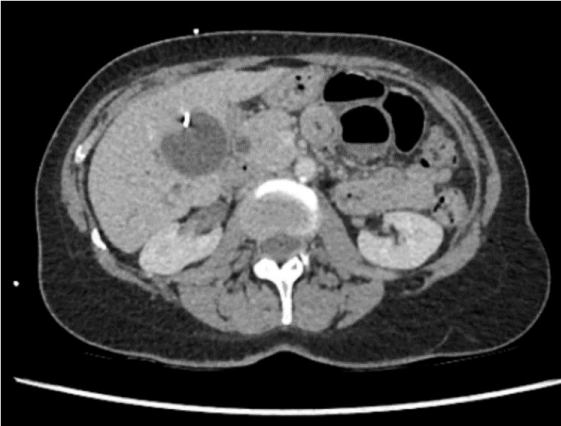
Four weeks after the index operation, the patient re-presented to the hospital with similar upper abdominal pain. On examination, the patient was tender at the right upper quadrant of the abdomen, but she did not have signs of peritonitis. Her liver functions tests were deranged. A CT scan of her abdomen revealed a biloma at gallbladder bed (Figure 5).
It was thought that segment 6 of the liver would likely atrophy or there would be alternate pathways for the bile to drain and the biloma would eventually resolve. The patient was discharged when her pain settled with plans to repeat imaging to check the progress of the biloma. Her liver function tests on subsequent testing showed improvement and follow up CT found resolution of the biloma.
Discussion
First described by Luschka in 1863 [4], subvesical bile ducts are rare but significant anatomic variations found during laparoscopic cholecystectomies that could have dire consequences.
Technical factors involved in minimizing harm were dissecting the gallbladder close to its wall [5]. in the subserosal plane as this would minimise chance of harm to the subvesical ducts which run deeper [6].
Also, the judicious use of intra-operative cholangiogram to define the anatomy was recommended though there is no evidence to show this reduces the rate of bile duct injury [7].
Early recognition of bile leak and bile duct injury is important in reducing the risk of biliary peritonitis and sepsis. Case reports in the medical literature of late presentations (4 and 8 days) of subvesical duct injuries presented with biliary sepsis [8,9]. Leaving a drain when there was suspicion of bile duct injury or during a difficult gallbladder bed dissection can help facilitate this [10].
An early referral to a tertiary hepato-biliary surgery unit also proved useful.
Conclusion
We present a case with two abnormal ducts in the gallbladder fossa managed surgically.
We would like to thank American Journal Experts for editing the manuscript.
- Pucher PH, Brunt LM, Davies N, Linsk A, Munshi A, et al. (2018) Outcome trends and safety measures after 30 years of laparoscopic cholecystectomy: a systematic review and pooled data analysis. Surg Endosc 32: 2175–2183. Link: https://bit.ly/3qR1yNg
- Spanos CP, Syrakos T (2006) Bile leaks from the duct of Luschka (subvesical duct): a review. Langenbecks Arch Surg 391: 441-447 Link: https://bit.ly/3tpxDNK
- Schnelldorfer T, Sarr MG, Adams DB (2012) What is the Duct of Luschka?-A Systematic Review. J Gastrointest Surg 16: 656-662. Link: http://bit.ly/3eN3fc7
- Luschka H (1863) Die Anatomie des Menschen in Rücksicht auf die Bedürfnisse der praktischen Heilkunde bearbeitet. Die Anatomie des menschlichen Bauches. Tübingen: Laupp 2: 235-263. Link: https://bit.ly/2NkKjpO
- Society of American Gastrointestinal and Endoscopic Surgeons. The SAGES safe cholecystectomy program. Link: http://bit.ly/3qR85r9
- Honda G, Hasegawa H, Umezawa A (2016) Universal safe procedure of laparoscopic cholecystectomy standardized by exposing the inner layer of the subserosal layer (with2016 video). J Hepatobiliary Pancreat Sci 23: E14- E19. Link: http://bit.ly/3vwuFsA
- Donnellan E, Coulter J, Mathew C, Choynowski M, Flanagan L, et al. (2021) A Meta-Analysis of the Use of Intraoperative Cholangiography; Time to Revisit Our Approach to Cholecystectomy?. Surgery Open Science 3: 8-15. Link: http://bit.ly/3rQmXY8
- Majumder S, Habibi H, Garcia CM (2013) Subvesical Bile Duct Injury: An Often Missed Cause of Postcholecystectomy Bile Leak. Surg Laparosc Endosc Percutan Tech 23: e168–e169. Link: http://bit.ly/3cvnbO0
- Pineño-Flores C, Segura-Sampedro JJ, García-Pérez JM, Soldevila-Verdeguer C, Palma-Zamora E, et al. (2018) Subvesical Duct Injury Resolved by Percutaneous Drainage. Gastroenterol Hepatol 41: 172-174. Link: http://bit.ly/38GTQ28
- Ahmad F, Saunders RN, Lloyd GM, Lloyd DM, Robertson GSM (2007) An algorithm for the management of bile leak following laparoscopic cholecystectomy. Ann R Coll Surg Engl 89: 51-56. Link: http://bit.ly/3ll5iW1

Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
