Global Journal of Medical and Clinical Case Reports
Fulminant Reversible Cerebral Vasoconstriction Syndrome: The Other Thunderclap Headache
Keith A Brown1*, James Brady1 and Ammar Alimam2
2Division of Pulmonary and Critical Care, Pulmonary and Sleep Associates of South Jersey, LLC, Cherry Hill, New Jersey, USA
Cite this as
Brown KA, Brady J, Alimam A (2020) Fulminant Reversible Cerebral Vasoconstriction Syndrome: The Other Thunderclap Headache. Glob J Medical Clin Case Rep 7(2): 117-120. DOI: 10.17352/2455-5282.000113Reversible Cerebral Vasoconstriction Syndrome (RCVS) is a rare neurologic clinical syndrome that is often misdiagnosed. The pathophysiology of RCVS is unknown, but oftentimes presents as a thunderclap headache that is commonly overlooked once cerebral hemorrhage is ruled out of the differential. Typically patients follow a benign course and make a full recovery, however, in a small subset of patients RCVS can result in permanent neurologic damage. We present a patient with an uncommon clinical course of RCVS and identify pitfalls in the diagnostic workup.
Introduction
Reversible Cerebral Vasoconstriction Syndrome (RCVS) is a rare phenomenon that is underdiagnosed in clinical practice [1]. Oftentimes the presenting symptom of RCVS is a thunderclap headache leading to evaluation for cerebral hemorrhage. However, blood work and imaging are usually negative which often leave the physician without answers or down an arbitrary path to treat atypical migraine headache [2]. Classically the symptoms of RCVS improve after approximately 2 months, but given the risk of life altering complications which include cerebral infarction, it is important that RCVS be included high in the differential diagnosis [2,3]. We present a case of a 56 year old female with thunderclap headache who was subsequently diagnosed with RCVS after devastating cerebral infarction.
Case report
The patient is a 56 year old female with a history of migraines, gastroesophageal reflux disease, hypertension, and hyperlipidemia that presented to the hospital with a sudden onset headache that started approximately 1 week ago. The patient rates the pain a 10/10 at onset and since then the headache has waxed and waned in intensity. These headaches were described as different from her typical migraine headache as it presented more suddenly and with greater intensity. She presented to multiple urgent care facilities to seek treatment and multiple Computed Tomographies (CT) of the head with CT Angiography (CTA) were performed throughout the previous week, which were only significant for bilateral intracranial internal carotid artery aneurysm. Her surgical history consists of hysterectomy, C3-C4 cervical fusion, and bilateral rotator cuff repair. Her social history was reviewed and she is a 1 pack per day smoker. Her home medication regimen included atorvastatin 80mg daily, clopidogrel 75mg daily, duloxetine 90mg daily, omeprazole 40mg daily, carvedilol 6.25mg daily, and ranitidine 150mg twice daily, and butalbital-acetaminophen-caffeine 50-325-40mg daily as needed.
On arrival to the hospital, the patient’s vital signs revealed a blood pressure of 147/78 mmHg.
Her admission laboratory work was unremarkable with the exception of a glucose of 199 mg/dL. CT of the head and CT angiography of the head and neck were performed promptly upon arrival, which was approximately 1 week after onset of headache, revealing atherosclerotic calcification of the bilateral internal carotid arteries particularly at the level of the cavernous and supraclinoid segments. Two aneurysms measuring 2mm involving the left and right internal carotid arteries were observed. However no other acute intracranial pathology or evidence of large vessel occlusion were demonstrated. The patient was admitted to the hospital under the Internal Medicine Service with presumed diagnosis of intractable migraines and 6mg subcutaneous injection of sumatriptan and 10mg decadron were prescribed upon Neurology evaluation on day 2 of her hospital stay. The patient became more encephalopathic with fevers and Magnetic Resonance Imaging (MRI) and Magnetic Resonance Angiography (MRA) were done on day 2 of her hospital stay, which were unremarkable, and lumbar puncture was completed on day 3 to rule out neurologic infection or autoimmune etiology of her altered mentation which was also negative.
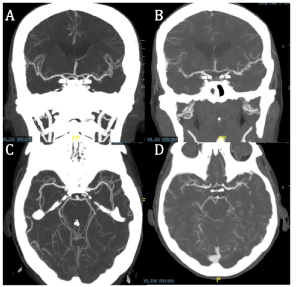
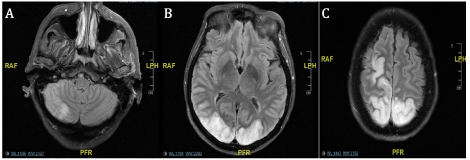
Six days into the patient’s hospitalization a stroke alert was activated as the patient had acute neurologic changes with increased lethargy and was unable to move her left arm. A teleneurology evaluation was done and a CT of the head was performed revealing large subacute appearing infarcts of the right and left posterior frontal, parietal, and occipital lobes, as well as the right cerebellum (Figure 1). CTA revealed mild to moderate stenosis in the cavernous and infraclinoid internal carotid arteries bilaterally with diminutive anterior cerebral arteries and possible occlusion of a distal segment or branch of the left anterior cerebral artery. Moderate stenosis was seen in the distal right vertebral artery, however the posterior cerebral arteries were not well visualized on this imaging study (Figure 2). The patient developed seizures which were refractory to lorazepam and she was intubated and started on versed continuous infusion. Continuous electroencephalogram revealed focal seizures originating the right occipital lobe. She was started on levetiracetam and lacosamide. On day 6, MRI was able to be done at that time revealing infarcts as previously described on CT with petechial hemorrhagic conversion. An echocardiogram was performed and significant for grade I left ventricular diastolic dysfunction consistent with impaired relaxation. In the setting of multiple cerebral infarctions and the ongoing pandemic of coronavirus-2019 (COVID-19), she was tested for the virus and was found to be negative. The patient was transferred to our facility for Neurosurgery evaluation as the admitting facility did not provide neurosurgical services.
Upon arrival to our facility the patient was intubated and sedated on versed and propofol and admitted to the Critical Care Service with Neurology and Neurosurgery consultation. Sedation was weaned and she was able to be extubated. The patient was provisionally diagnosed with RCVS at this time and 4 grams (g) of Intravenous (IV) magnesium and oral amlodipine 10mg were prescribed and her previous levetiracetam and lacosamide were continued. A repeat CTA of the head and neck were done on day 7 revealing known findings of bilateral occipital lobe infarcts, however arteries were patent with no findings of significant stenosis or occlusion. After starting the patient on this regimen she became progressively more awake, alert, and oriented after several days of treatment. However she was found to be blind bilaterally, with ⅗ strength in the right upper and lower extremities with left sided hemiplegia. Over the course of her hospital stay she received amlodipine 10mg daily and 2g of magnesium daily for 7 days. The patient continued to work with physical therapy to optimize her physical mobility and strength. At the conclusion of her 21 day hospitalization, her vision did improve significantly and she only required reading glasses for correction of her vision. Unfortunately, she remained with residual left sided hemineglect. She was discharged to an acute rehabilitation facility and will continue to follow up with her Neurology specialist for ongoing evaluation and management.
Discussion
In 2007, multiple unexplained vasculopathies and vasoconstriction syndromes to include CallFleming syndrome, postpartum angiopathy, and acute benign cerebral angiopathy were unified as one clinical syndrome called RCVS [4,5]. Since this time few cases have been reported in the literature of patients with RCVS with poor outcomes and death as it is generally observed to have a self-limiting course [5]. RCVS appears to predominantly affect young females between the ages of 20 to 50 years of age, but according to a single cohort study, men who present with RCVS are significantly younger and symptoms are often associated with sexual activity [6]. The hallmark of the disease is thunderclap headache as well as reports of photophobia and phonophobia leading the physician to a diagnosis of migraine after cerebral hemorrhage has been ruled out [1,7]. The exact mechanism for this clinical syndrome is unknown, but susceptibility to developing RCVS may be influenced by genetics or a potential trigger [8]. Common triggers have been reported to include alcohol, sexual intercourse, triptans, postpartum states, and Valsalva maneuver; however, many patients are diagnosed without a known trigger [2]. Specific attention should be paid to the use of triptans as patients are often prescribed this for migraine, which this clinical syndrome is often mistaken for. Previous case reports have linked triptans to induce or at the very least exacerbate RCVS [8]. Our patient was also prescribed triptans which may have contributed to her rapid neurologic decline after hospitalization.
Clinical presentation is misleading as thunderclap headache is the most common clinical presentation of RCVS although it is not specific for the syndrome [1,4]. In fact, when physicians encounter thunderclap headache the differential is often limited to subarachnoid hemorrhage, migrainous headache disorder, Primary Angiitis of the Central Nervous System (PACNS), and cervical arterial dissection. More specific characteristics of thunderclap headache that are associated with RCVS include a waxing and waning course often that repeats over 1 to 3 weeks [4]. This distinction is particularly important to consider during initial examination in a patient with RCVS as presentation of subarachnoid hemorrhage presents with more abrupt onset. Seizures can be present at onset as well, but their recurrence is rare [9]. Rapid progression of the disease is very unusual in RCVS [5], but our patient did develop rapid neurological decline after she was hospitalized. This type of fulminant course is encountered in 5-10% of patients with RCVS resulting in permanent disability and death [10].
Diagnostic criteria for RCVS include acute and severe onset headache, with or without additional neurologic signs or symptoms that are uniphasic without new symptoms after 1 month of onset. On cerebrovascular imaging there is evidence of multifocal segmental cerebral artery vasoconstriction without evidence of aneurysmal SAH [4,9]. A clinical and radiologic distinction must be made between RCVS and PRES. MRI with diffuse weighted imaging and cerebral angiographic imaging remains the radiologic test of choice for both clinical entities and in RCVS lesions are typically asymmetric while in PRES lesions are more symmetric. MRI should be performed when CT are non diagnostic and do not adequately explain the patients symptoms. In RCVS there are also ischemic lesions noted bilaterally while ischemic lesions are uncommon in PRES. In RCVS vasoconstriction on vascular imaging is a distinctive finding 6. Our patient demonstrated findings of asymmetric lesions with associated ischemia with vasoconstriction on vascular imaging which is more typical with RCVS. Given results of imaging, a lumbar puncture was performed to exclude pleocytosis in the setting of headache. Infectious workup to include CSF analysis was unremarkable, which was done to exclude infectious as well as paraneoplastic and autoimmune etiology. Most importantly there is reversibility of angiographic abnormalities within 12 weeks after onset of disease, separating it from the etiology and findings in acute ischemia secondary to vascular occlusion from thrombosis or progressive atherosclerosis [4,9]. Infarction on baseline imaging, use of intra-arterial vasodilator therapy, and glucocorticoid therapy may be associated with poor outcomes [10].
There are no clear treatment modalities for the treatment of RCVS and specific treatment is based on observational studies and clinical experience. Like any clinical entity with potential triggers, these offending agents must be discontinued [9], such as sumatriptan in our patient. Other pharmacologic agents thought to be potential precipitating factors are triptans, ergotamines, pseudoephedrine, amphetamines, cannabis, cocaine, and bromocriptine [1]. Treatment of the vasospasm should be considered for cerebral vasoconstriction with calcium channel blockers and continued for 4-12 weeks. Our patient was treated with amlodipine and magnesium upon diagnosis which has been used as well in the treatment of acute RCVS with success. The decision to use amlodipine opposed to nimodipine, nicardipine, or verapamil was arbitrary and based off of the attending physician preference. There are no evidence based guidelines regarding calcium channel blockers although nimodipine and verapamil are most common reported in previous cases. Intra-arterial administration of epoprostenol, milrinone, and nimodipine as well balloon angioplasty have all been reported in more severe cases with variable success. However, this intervention should be utilized based on access to intervention and operator experience as this procedure is higher risk [1,9]. Although magnesium and calcium channel blockers have been used in previous reported cases of RCVS, no standard treatment regimen has been established [1]. However, long term management with neurologic specialists is imperative as symptom recurrence and complications until death may rarely occur [10].
Conclusion
RCVS presents a diagnostic challenge in physicians as it is not a commonly encountered clinical syndrome. However, given the life altering complications such as cerebral hemorrhage and infarction, it is imperative to be aware of this clinical entity. Patients who present with thunderclap headache without significant findings on neuroimaging are often diagnosed with migraines even if the clinical history does not fit properly. Unfortunately, this leads to prescription of vasoconstrictive drugs which can often worsen RCVS. Through this case it is our goal to bring awareness to RCVS and bring the condition into physicians’ differential diagnosis as the other thunderclap headache.
Institutional financial and material support were not provided for the creation of this manuscript.
- Ba F, Giuliani F, Camicioli R, Saqqur M (2012) A reversible cerebral vasoconstriction syndrome. BMJ Case Reports. Link: https://bit.ly/39ykTO5
- Ji JY, Jung HS, Yoo SH, Son HD, Kim AJ (2019) Reversible cerebral vasoconstriction with thunderclap headache: A case report. Medicine 98. Link: https://bit.ly/3luZWpF
- Mijalski C, Dakay K, Miller-Patterson C, Saad A, Silver B, et al. (2016) Magnesium for treatment of reversible cerebral vasoconstriction syndrome: Case series. Neurohospitalist 6: 111-113. Link: https://bit.ly/3luGlpJ
- Miller TR, Shivashankar R, Mossa-Basha M, Gandhi D (2015) Reversible cerebral vasoconstriction syndrome, part 1: Epidemiology, pathogenesis, and clinical course. Am J Neuroradiol 36: 1392-1399. Link: https://bit.ly/3qkjSiH
- Suchdev K, Norris G, Zak I, Mohamed W, Ibrahim M (2018) Fulminant Reversible Cerebral Vasoconstriction Syndrome. Neurohospitalist 8: NP5-NP8. Link: https://bit.ly/33zXdoY
- Topcuoglu MA, McKee KE, Singhal AB (2016) Gender and hormonal influences in reversible cerebral vasoconstriction syndrome. Eur Stroke J 1: 199-204. Link: https://bit.ly/36vGHYI
- Rao P, McCollough MF, Stevens J, Edwardson M (2020) Grief-induced reversible cerebral vasoconstriction syndrome (RCVS). BMJ Case Rep 13: e232204. Link: https://bit.ly/2VqqH41
- Kato Y, Hayashi T, Mizuno S, Horiuchi Y, Ohira M, et al. (2016) Triptaninduced reversible cerebral vasoconstriction syndrome: Two case reports with a literature review. Intern Med 55: 3525-3528 Link: https://bit.ly/3qmXbub
- Santos L, Azevedo E (2016) Reversible cerebral vasoconstriction syndrome - a narrative revision of the literature. Porto Biomed J 1: 65-71. Link: https://bit.ly/2JvhJ33
- Pilato F, Distefano M, Calandrelli R (2020) Posterior reversible encephalopathy syndrome and reversible cerebral vasoconstriction syndrome: Clinical and radiological considerations. Front Neurol 11: 34. Link: https://bit.ly/3ofjv79

Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.
 Save to Mendeley
Save to Mendeley
