Global Journal of Medical and Clinical Case Reports
Endoscopic removal of bullet lodged in nasal roof
Vanitha Palanisamy* and Prepageran Narayanan
Cite this as
Palanisamy V, Narayanan P (2019) Endoscopic removal of bullet lodged in nasal roof. Glob J Medical Clin Case Rep 6(2): 029-031. DOI: 10.17352/2455-5282.000075Cases of survival after a penetrating firearm injury to the head are very uncommon. In cases where the bullet does not exit the head, it can be lodged anywhere in the cavities of the skull leading to fatal consequences. This case report examines a rare case of a penetrating firearm injury to the face where the victim survived and the bullet was discovered to be lodged at the nasal roof. The victim of this case report is a 25-year-old Somalian lady and the bullet that penetrated her head entered through the right eye laterally and lodged into the midline of the nasal roof. The bullet was successfully removed endoscopically via right nostril without any complications.
Introduction
Survival after a firearm injury that penetrated the head are rarely reported. When a bullet penetrates the head in such an injury, it can get lodged in any of the cavities of the skull. The most common site such foreign body may get lodged reported so far is the maxillary sinus, followed by frontal, ethmoid and sphenoid sinuses [1-4]. The extent of the injuries caused by a bullet penetrating the face is unpredictable due to the complex anatomy of the craniofacial skeleton and can be devastating functionally if not fatal. Removal of the foreign body is often extremely difficult as it may result in further damage to vital sensory organs in the process. Fortunately, the use of endoscopes has remarkably changed the scenario by converting extensive open procedures through external approaches into safe, less damaging, directly visualized approaches of removal.
This is a case report of such an uneventful endoscopic removal of a foreign object, which describes the management of a young lady with bullet lodged in the midline of the nasal roof having penetrated through the right eye laterally.
Case Report
A 25-year-old Somalian woman presented with a bullet in her face. Patient had sustained a gunshot injury to the head at her hometown in Mogadishu in July 2016. The bullet was fired from a distance of only a few metres away, landed on her head while she was sleeping soundly at her home. The bullet entered the right eye laterally and did not exit. She sought emergency treatment at her hometown hospital, where a skull X-ray revealed that the bullet has lodged into the nasal cavity. She was told to go home as the hospital did not have the facilities to perform the surgery and was prescribed with eye drops. At initial presentation patient only had minimal epistaxis which resolved spontaneously.
Patient subsequently travelled to Malaysia to seek further treatment. Initially seen at a private medical centre at Kuala Lumpur where a CT-scan was carried out and subsequently referred to University Malaya Medical Centre (UMMC) Ophthalmology department for the blindness on her right eye and the Ear, Nose and Throat (ENT) department for the removal of the foreign body which was lodged at the roof of the nasal cavity.
Examination revealed a stable patient with a full Glasgow Coma Scale (GCS), right sunken globe and no other external injury to the head or face. No external nasal deformity or swelling were seen (Figure 1).
Rigid nasoendoscopy revealed a smooth bulge at the roof of the right nasal septum with minimal crusting over it. Opthalmology examination revealed ruptured right globe, no external wound around the eye and the blindness of the right eye.
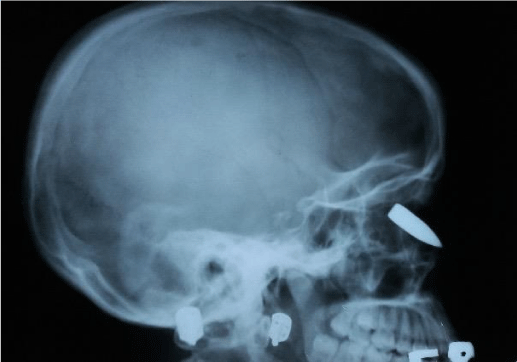
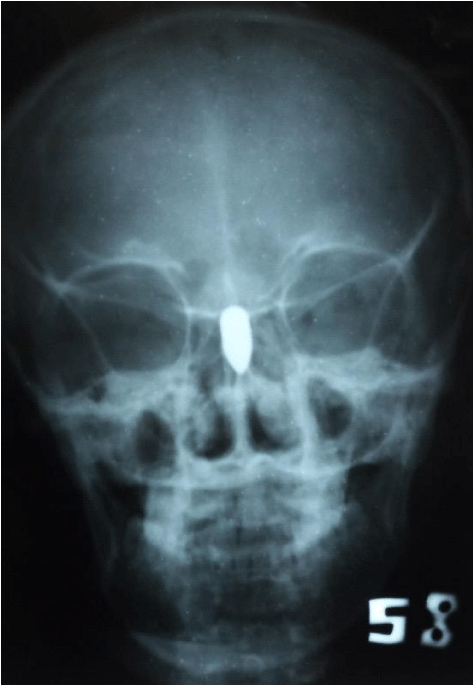
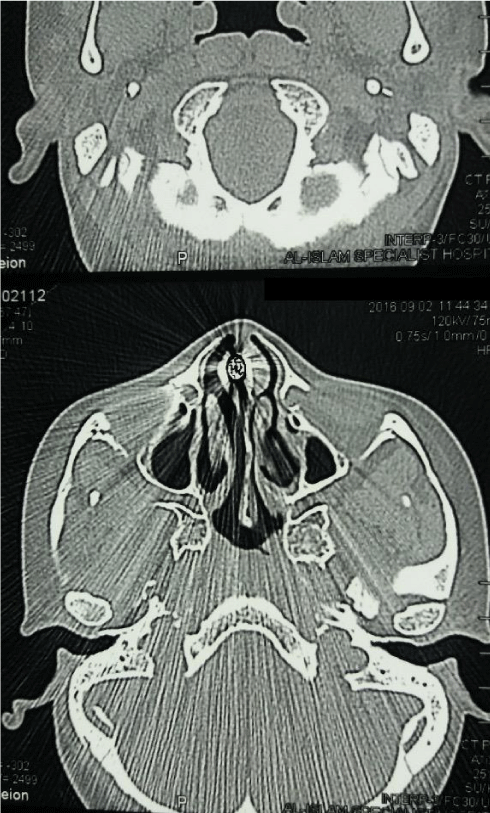
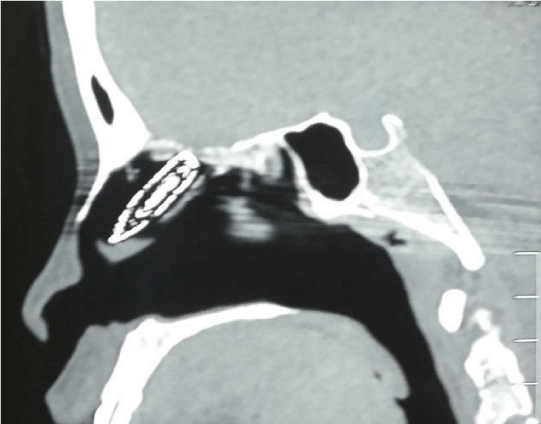
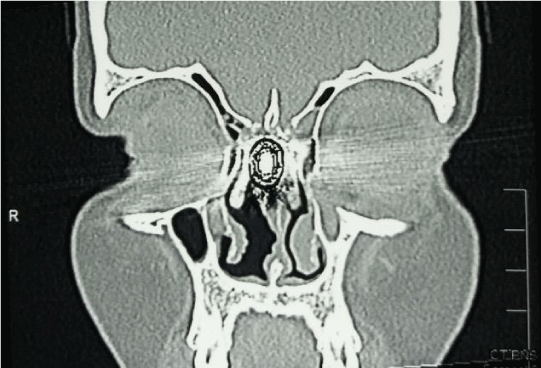
X-ray and computed tomography ( CT) scan examination of the paranasal sinuses revealed the bullet situated in the midline of the nasal cavity roof longitudinally at an angle with the front of the bullet pointing towards the nostril and the base of the bullet just abutting the cribriform plate which it has probably penetrated through (Figures 2-6).
In September 2016 endoscopic removal of the foreign body by the ENT team was performed. This was followed by an evisceration of the eye by the Ophthalmology team. The decision to perform evisceration of the right eye was done to prevent sympathetic opthalmitis to the opposite eye.
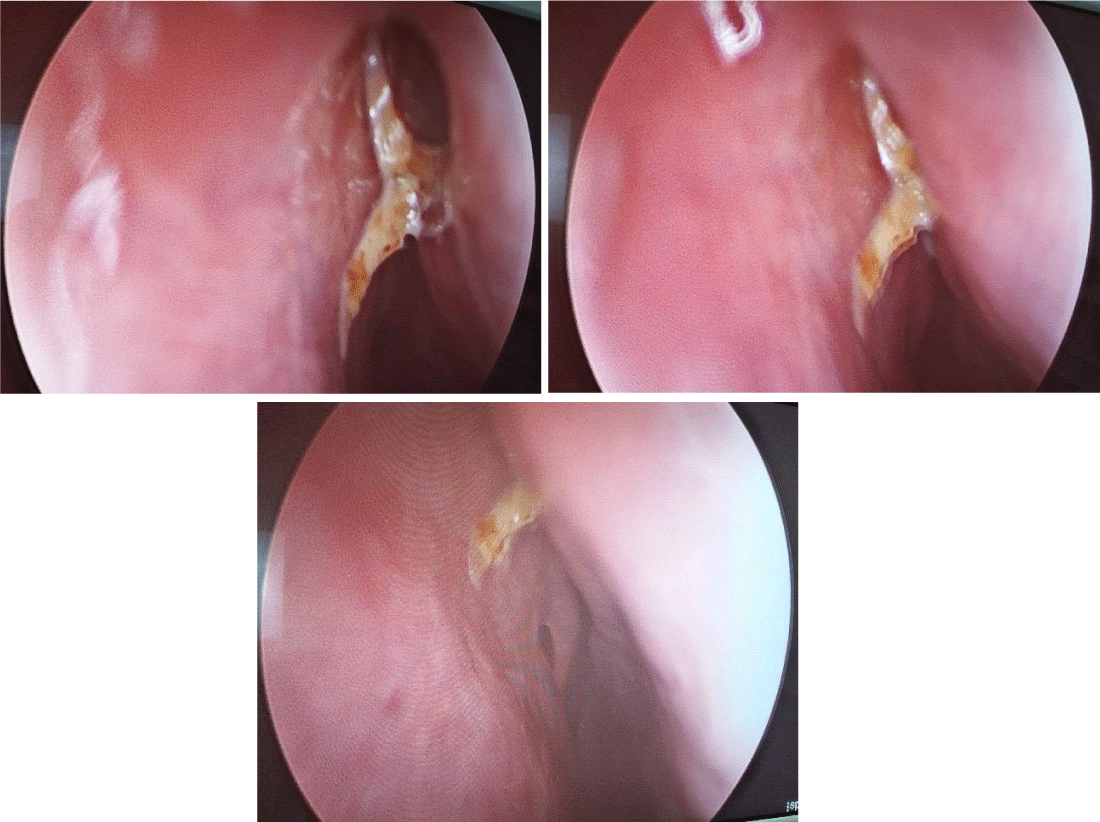
Intraoperative findings of the bullet position was correlated with the CT scan findings. Removal of the bullet was done by initially laterialising the right middle turbinate. A freer was inserted between the septum and right middle turbinate up to the nasal roof. Minimal crusting was seen at the roof of the nose at the level of anterior end of right middle turbinate. On retracting the mucosa of the septum at the roof the bullet was seen embedded. Bullet was dislodged using a freer. Minimal bleeding was seen at the roof which was covered by minimal granulation tissue. No cerebrospinal fluid leak was observed (Figures 7,8).
This was followed by the evisceration of the right eye by the ophthalmology team. The patient recovered well in the hospital ward and was discharged after two days of monitoring. No evidence of cerebrospinal fluid leak or epistaxis noted during this monitoring period.
During the review after 2 weeks in the clinic, it was noted that the patient did not have any nasal symptoms. Nasoendoscopy showed clear nasal cavity with no blood clots nor cerebrospinal fluid leak or any signs of infection. Subsequent review 4 weeks was also uneventful and patient was discharged.
Discussion
Firearm injuries in the craniofacial region often cause damage to vital organs leading to irreversible and uncompensated loss leading to fatal consequences. When a bullet penetrates the head from a gunshot incident, the course of bullet is unpredictable as the bullet may traverse in any direction and get lodged in any of the compartments or cavities of the skull. If the bullet does not exit the head, the most likely site of lodgement are the paranasal sinuses [1-4]. The bullet may also be lodged in the cranial cavity [5,6]. Nevertheless, in such an event, it is very rare to find the bullet lodged in the nasal roof without life-threatening damage, as presented in this case.
While plain radiology is helpful in localizing the foreign body, a computer tomography scan not only helps determine a more precise location of the bullet, but it essentially provides the roadmap for safe and accurate endoscopic removal.
Employment of conventional open methods of removal of the foreign body would lead to increased morbidity, scaring, disfigurement and potentially other complications. In general, trans-nasal endoscopic removal is safer, less damaging and easier alternative. provided that the foreign body is approachable endoscopically, the endoscopic procedure offers surgeons with a more direct visualization. Furthermore, endoscopic removal of bullet and pellets from maxillary sinus, frontal sinus, sphenoid sinus and anterior cranial fossa have previously been reported with high degree of success [3-10]. Crucially, the approach for the removal of the foreign body would need to be tailored based on the exact site of foreign body. In some cases, the criticality of site may contraindicate surgery due to the risk of removal outweighing the benefits [10,11]. Conclusively, in arriving at the decision to remove a bullet in firearm injuries, several key factors need to considered, including the its location, the extent of the resulting injuries and the associated risks, facilities available and the experience of the surgeon.
In the case presented in this report, examinations revealed the site of the bullet as lodged in the midline of the nasal roof area. The strong nasal bone had likely stopped the bullet from progressing to the other side of the face that could have caused blindness of both eyes. The bullet was successfully and uneventfully removed by trans-nasal endoscopic approach through the nasal cavity at the midline nasal roof. The procedure caused much less morbidity when compared to the likely outcome of employing an external approach. In conclusion, this approach is recommended in such cases where the foreign body is lodged in the cranio-facial region provided that it is approachable through endoscope and where the required expertise and facilities are readily available.
- Rahman AC (1982) Foreign bodies in the maxillary antrum. Br Dental J 153:108-109. Link: http://bit.ly/309la2G
- Holmes A (1987) Sewing needle as an antral foreign body. Br Dental J 162: 153-154. Link: http://bit.ly/31A3Jsm
- Raik SM (1995) An unusual foreign body in the frontal sinus. Indian Journal of Otolaryngology and Head and Neck Surgery 1: 38-39. Link: http://bit.ly/303dwqq
- Ramdas T, Prabhakaran M, Kumar VS (1996) Air riffle bullet in the sphenoid sinus. Indian Journal of Otolaryngology and Head and Neck Surgery 1: 51-52. Link: http://bit.ly/2z1fr2V
- Dodson KM, Bridges MA, Reitur ER (2004) Endoscopic transnasal management of intracranial foreign bodies. Arch Otolaryngol Head Neck Surg 130: 985-988. Link: http://bit.ly/2H7oK60
- Cetinkaya EA, Okan C, Pelink (2006) Transnasal, intracranial penetrating injury treated endoscopically. J Laryngol Otol 120: 325-326. Link: http://bit.ly/2MjTzbK
- Dutta A, Awasthi SK, Kaul A (2006) A bullet in the maxillary sinus. Indian J Otolaryngol Head Neck Surg 58: 307-319. Link: http://bit.ly/31KQvJw
- Kapil D, Amit KJ, Hemant C, Bajwa GS, Jaspal S (2007) Endoscopic removal of unusual foreign bodies from maxillary sinus. Pak J Otolaryngol. Head Neck Surg 23 :52-53.
- Jones NS (2001)The risks and benefits of endoscopic removal of a foreign body from the anterior cranial fossa; a case report. BMJ 322: 122-123.
- Thomas S, Daudia A, Jones NS (2007) Endoscopic removal of foreign body from the anterior cranial fossa. J Laryngol Otol 121: 794-795. Link: http://bit.ly/2z61zUU
- Muhammad Khyani IA, Hafeez A, Farooq MU, Alam J (2008) Endoscopic Removal of Bullet from Orbital Apex. J Coll Physicians Surg Pak 18: 646-648. Link: http://bit.ly/2Ml1hCe

Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
