Global Journal of Medical and Clinical Case Reports
Successful double valve replacement in a pregnant woman with refractory heart failure due to early dysfunction of the biological prosthesis in the aortic valve position
José C Candia1, José F Alderete1, Jorge Martínez1, Oscar A Lovera1, Jorge Jarolín2 and Osmar Antonio Centurión1,3*
2Department of Cardiac Surgery, Clinical Hospital, Asunción National University (UNA), San Lorenzo, Paraguay
3Department of Health Sciences Investigation, Sanatorio Metropolitano, Fernando de la Mora, Paraguay
Cite this as
Candia JC, Alderete JF, Martínez J, Lovera OA, Centurión OA, et al. (2019) Successful double valve replacement in a pregnant woman with refractory heart failure due to early dysfunction of the biological prosthesis in the aortic valve position. Glob J Medical Clin Case Rep 6(1): 003-005. DOI: 10.17352/2455-5282.000067Rheumatic fever continues to be a frequent cause of cardiac valve disease in developing countries. The combination of rheumatic heart disease and pregnancy represents a challenge in the management of these patients. Prevention strategies are often insufficient; this is why we continue to observe complicated cases that demand more complex treatments. We are reporting the case of a 20-year-old woman, with a history of aortic valve replacement and mitral valve repair due to rheumatic heart disease. Two years later after her valve replacement, she attended consultation with signs and symptoms of heart failure in functional class III during a pregnancy of 20 weeks. The echocardiography showed: dysfunctional biological aortic prosthesis with severe stenosis and moderate regurgitation (central and para-valve leak), as well as severe mitral valve insufficiency, eccentric, directed towards the atrial free wall. She was admitted, and received optimal medical treatment for 4 weeks with little response and subsequent worsening. A multidisciplinary committee was formed including cardiologists, cardiac surgeons, obstetricians, neonatologists, and specialists in bioethics. It was decided to proceed with valve replacement surgery during the 21st week of her gestation. Successful double valve replacement (mitral and aortic) was performed, without complications for the patient or the fetus. She was discharged in good health. In her 38th week of gestation, a successful cesarean delivery was performed without any complications.
Introduction
Rheumatic fever consists of a sequela of a pharyngeal infection produced by Streptococcus pyogenes or, A Group beta-hemolytic streptococcus. Of the symptoms associated with this condition, only valve damage or rheumatic heart disease (RHD) can lead to a chronic condition and lead to heart failure, stroke, endocarditis and death [1-4].
Although the incidence and prevalence of rheumatic fever and RHD have decreased in developing countries, they continue to be the cause of significant morbidity and mortality among young people. It is estimated that there are more than 15 million cases with RHD worldwide, with 282,000 new cases and 233,000 deaths annually [1]. A particularly susceptible population consists of pregnant women, who frequently have complications related to this disease. Acute rheumatic fever is a possible complication at this stage, but it is rarely observed. The majority of patients have established valve disease.
In developing countries, cardiac valve disease is present in 80% of patients with pregnancy-related cardiomyopathy, with rheumatic fever being the most common etiology [2]. Pregnancy represents a hyper-dynamic state in which changes occur at the cardiovascular level; increase in cardiac output, expansion of blood volume and reduction of systemic vascular resistance and blood pressure [3]. In with severe cardiac valve disease, these changes are poorly tolerated, especially those associated with stenosis due to the increase in valve gradients, with fetal and neonatal complications reported in up to 25% [4]. Therefore, we are presenting an interesting and ethically challenging case of a patient with rheumatic valve disease, carrying a dysfunctional biological prosthesis in the aortic position who presents refractory heart failure during a pregnancy of 20 weeks.
Case Report
A 20-year-old woman presented for consultation at the Cardiology Department of the Hospital de Clínicas. She complained of episodes of respiratory distress associated with efforts and edema of lower limbs in recent weeks. She reported having undergone aortic valve replacement surgery with a biological prosthesis 2 years earlier, due to severe rheumatic aortic regurgitation. She had an ischemic stroke of cardiac emboli origin one year earlier. She received anticoagulant medication since then. She was also having regular check-ups for a gestation of 20 weeks.
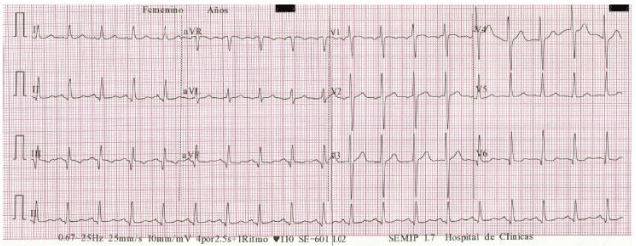
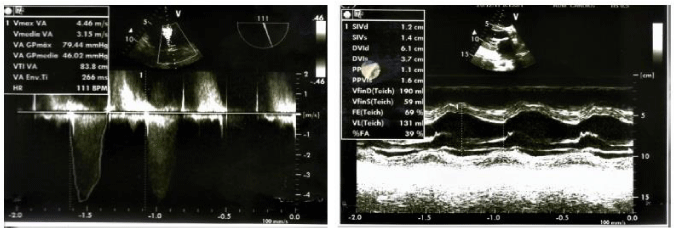
Upon physical examination, she was found with a heart rate of 110 beats per minute with a regular rhythm. The auscultation revealed the presence of systolic murmur in mitral focus IV / VI, as well as systolic murmur in aortic focus III / VI. She had signs of pulmonary congestion and lower limb edema. The electrocardiogram showed a sinus tachycardia with presence of Q waves in inferior leads (Figure 1). Transthoracic echocardiography showed a mitral rheumatic valve disease with severe insufficiency. Thickened aortic biological prosthesis with severe stenosis and moderate insufficiency was also observed with normal systolic function of the left ventricle (Figure 2). For a better characterization of these findings, transesophageal echocardiography was performed, showing the biological valve prosthesis in dysfunctional aortic position with severe stenosis and moderate failure (central and para-valve leak). Severe mitral valve insufficiency, eccentric, directed toward the left atrial free wall, due to poor systolic cooptation due to retraction of the sub-valve apparatus of the posterior leaflet.
The corresponding pharmacological measures for heart failure were initiated. The patient remained hospitalized for four weeks after which she presented a progressive worsening, so valve replacement surgery was proposed. A multidisciplinary committee comprised of cardiologists, cardiac surgeons, gynecologists, neonatologists, and bioethics committee met and finally it was decided to proceed with cardiac surgery.
The surgical technique proceeded as follows: Heparinization, aortic cannulation and cannulation of the superior and inferior vena cava through the right atrium, entry to extracorporeal circulation, aortic clamping. Classical aortotomy was performed, and cardioplegia in both coronary sinuses. The biological valvular prosthesis was found to have severe dysfunction due to calcification and rupture of its leaves. There is no evidence of detachment of the suture. Then, we proceeded to the extraction of the prosthesis which was very difficult due to intense peri and subvalvular fibrosis. We proceeded to place points in U to fix a 19 mm biological prosthesis that fitted very well. Closure of the aortotomy was done. Then we proceeded to the left atriotomy, the left atrium was dilated. Thrombi were not observed inside. Mitral valve was thickened and retracted at its free edges. The anterior leaflet was extracted and the posterior leaflet was preserved. U points were placed on Teflon and a 31 mm biological valvular prosthesis with good settlement was implanted. The atriotomy was closed. Extracorporeal circulation time was 130 min at a temperature of 32 degrees celcius. Aortic clamping time was 110 min.At surgery, it was found that the biological aortic prosthesis was severely dysfunctional (Calcification and rupture of its leaves), there was no evidence of detachment of the suture, nor signs of infection. The patient remained in UCIA for 6 days and in the ward for 12 days, she was finally discharged in good health. In her 38th week of gestation, a successful cesarean delivery was performed without any complications.
Discussion
We are presenting an interesting and ethically challenging case of a patient with rheumatic valve disease, carrying a dysfunctional biological prosthesis in the aortic position who presents refractory heart failure during a pregnancy of 20 weeks. A successful double valve replacement in the aortic and mitral positions was performed, and later on a successful cesarean delivery was performed without any complications.
In the modified classification of risk during pregnancy (WHO) [5], valve prosthesis and severe symptomatic aortic stenosis are found in groups III and IV, representing extremely high mortality and morbidity. Some studies also describe deterioration of the prosthesis during pregnancy [6,7]. It is recommended, if possible, to avoid cardiac surgery during this period of pregnancy because of multiple complications, high morbidity and mortality for the mother and the fetus [8-10]. In our reported case, the cardiac surgery was decided due to the failure of the pharmacological treatment and worsening of her clinical condition, and to the fact that the life of the mother and the fetus were highly compromised. Our case also highlights the early dysfunction (at 2 years) of the biological prosthesis, and the great need to make early diagnoses of these pathologies in order to insist on prenatal counseling [11]. Although unusual, early dysfunction of a biological prosthesis may occur which is a fact that we have to take into account when making a decision to perform cardiac valve replacement. Our case also emphasizes the need for a multidisciplinary team to work together in order to proceed with the best approach and solution for a very complicated and ethically challenging case.
- Carapetis JR, Steer AC, Mulholland EK, Weber M (2005) The global burden of group A streptococcal diseases. Lancet Infect Dis 5: 685-694. Link: https://tinyurl.com/yxwj8aoc
- Watkins DA, Sebitloane M, Engel ME, Mayosi BM (2012) The burden of antenatal heart disease in South Africa: a systematic review. BMC Cardiovasc Disord 12: 23. Link: https://tinyurl.com/y2mwar2a
- Chapman AB, Abraham WT, Zamudio S (1998) Temporal relationships between hormonal and hemodynamic changes in early human pregnancy. Kidney Int 54: 2056-2063. Link: https://tinyurl.com/yxz9d6vs
- Hameed A, Karaalp IS, Tummala PP (2001) The effect of valvular heart disease on maternal and fetal outcome of pregnancy. J Am Coll Cardiol 37: 893-899. Link: https://tinyurl.com/y35mtrxj
- Thorne S, MacGregor A, Nelson-Piercy C (2006) Risks of contraception and pregnancy in heart disease. Heart 92: 1520-1525. Link: https://tinyurl.com/yxuqw9v9
- Badduke BR, Jamieson WR, Miyagishima RT (1991) Pregnancy and childbearing in a population with biologic valvular prostheses. J Thorac Cardiovasc Surg 102: 179-186. Link: https://tinyurl.com/y68pebw9
- Nitsche C, Kammerlander AA, Knechtelsdorfer K, Kraiger JA, Goliasch G, et al. (2019) Determinants of Bioprosthetic Aortic Valve Degeneration. JACC Cardiovasc Imaging pii: S1936-878X(19)30165-2. Link: https://tinyurl.com/yysypsmw
- Weiss BM, von Segesser LK, Alon E (1998) Outcome of cardiovascular surgery and pregnancy: a systematic review of the period 1984-1996. Am J Obstet Gynecol 179: 1643-1653. Link: https://tinyurl.com/yyox8vsd
- Maskell P, Burgess M, MacCarthy-Ofosu B, Harky A (2019) Management of aortic valve disease during pregnancy: A review. J Card Surg 34: 239-249. Link: https://tinyurl.com/y4xsoacr
- Dayan V, Arocena MJ, Fernandez A, Silva E, Zerpa DP (2019) Previous Cardiac Surgery: a Predictor of Mortality in Aortic Valve Replacement? Braz J Cardiovasc Surg 34: 173-178. Link: https://tinyurl.com/yy8y646f
- Rea CW, Wang TKM, Ruygrok PN, Sidhu K, Ramanathan T, et al. (2019) Characteristics and Outcomes of Patients With Severe Aortic Stenosis Discussed by the Multidisciplinary "Heart Team" According to Treatment Allocation. Heart Lung Circ pii: S1443-9506(19)30273-2. Link: https://tinyurl.com/y2bezvwt

Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.
 Save to Mendeley
Save to Mendeley
