Global Journal of Medical and Clinical Clinical Image
Muscle strength, level of pain and balance in women with knee osteoarthritis after a sensory-motor exercise program associated to photobiomodulation therapy via cluster: a single-blinded randomized with placebo control trial
Ana Beatriz Balão1, Patricia Gabrielli Vassão1*, Marcela Regina de Camargo2, Victor Zuniga Dourado2, Helga Tatiane Tucci2 and Ana Cláudia Muniz Rennó1
2Department of Human Movement Science of Federal University of São Paulo, Santos, SP, Brazil
Cite this as
Balão AB, Vassão PG, De Camargo MR, Dourado VZ, Tucci HT, et al. (2023) Muscle strength, level of pain and balance in women with knee osteoarthritis after a sensory-motor exercise program associated to photobiomodulation therapy via cluster: a single-blinded randomized with placebo control trial. Glob J Medical Clin Case Rep 10(1): 003-010. DOI: 10.17352/2455-5282.000168Copyright License
© 2023 Balão AB, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Introduction: Osteoarthritis (OA) is the most common chronic condition of the joints that leads to pain, stiffness and disability.
Aim: The aim of this study was to determine the effectiveness of a sensory-motor exercises program and the photobiomodulation on pain, muscle strength, severity of the injury and dynamic balance of women with knee osteoarthritis.
Method and Materials: Thirty-two women were randomized in sensory-motor exercises associated with the placebo photobiomodulation group (SMAG) and sensory-motor exercises with the active photobiomodulation group (SMPG). The pain, knee flexor and extensor peak torque, severity of the injury and dynamic balance were evaluated with the numeric pain rating scale, cell roll, Knee Injury and Osteoarthritis Outcome Score and timed up and go, respectively. Subjects were administered sensory-motor exercises, strengthening exercises and photobiomodulation via cluster applied at the end of each training session for 8 weeks, 2 times/week.
Results: There was no significant improvement in the knee flexor and extensor peak torque, meantime, there was a significant linear positive correlation in the sensory-motor exercises program associated with the placebo photobiomodulation group (p = 0.002) at the end of treatment. A significant improvement in the severity of injury (p = 0.002) and dynamic balance (p = < 0.001) was observed in both groups. Furthermore, the level of pain showed a significant improvement in the sensory-motor exercises program associated with the placebo photobiomodulation group (p = 0.043).
Conclusion: Sensory-motor exercise program promotes beneficial effects on the severity of the injury and dynamic balance and its association with photobiomodulation was able to produce an extra effect in pain relief. However, adding photobiomodulation to routine exercise regimes for subjects with knee osteoarthritis should be investigated.
Introduction
Osteoarthritis (OA) is the most common chronic joint disease and affects approximately 27 million people in United States [1]. A series of morphological modifications in the cartilage occurs that leads to tissue fibrillation, degeneration of the subchondral bone, formation of osteophytes and inflammation of the synovium [2]. The symptoms of OA include an increase in the level of pain, joint stiffness, decreased range of motion (ROM) and an impairment of muscle strength, which leads to physical disability and significant loss of quality of life [3].
OA treatment is based mainly on the use of pharmacological treatments [4], weight control and physical exercise programs (PEPs) [5,6]. PEPs, including both strengthening and aerobic exercise, produce an analgesic effect and an improvement of articular function and muscle strength leading to an increase in general health status in patients with OA [7]. However, there is a lack of studies in the literature investigating the effect of sensory-motor physical exercises program (SMEP) on the symptomatology of OA.
A promising resource intervention that has been showing positive effects on cartilage tissue is low-level laser therapy (LLLT) or photobiomodulation (PBM), mainly due to its analgesic effects and the ability to modulate the inflammatory process [8]. Moreover, the chondroprotective effects of PBM have been observed in several experimental studies of OA in rats [9,10]. Clinical trials have demonstrated that PBM has the ability to reduce pain and knee swelling, increasing the functional activity in this population, mainly in association with PEPs [11,12]. In general, PBM has been applied through the punctual technique, with one point of irradiation each time, which may limit the efficacy of the treatment.
In this context, it was hypothesized that the association of a sensory-motor exercise program (SMEP) and PBM (cluster) may modulate joint inflammatory process and improve strength and balance which may culminate in pain relief and consequent physical and functional capacity improvement in women with knee osteoarthritis (KOA). Thus, the aim of this study was to determine the effectiveness of a SMEP and the PBM, with a cluster device as an alternative to optimize the application, on knee flexor and extensor muscle strength, the severity of the injury, dynamic balance and level of pain in women with KOA.
Materials and methods
The present study is a single-blinded randomized with placebo control trial. The research was approved by the Ethics and Research Committee of the Federal University of São Paulo (CAAE: 87029318.6.0000.5505). Participants signed two copies of the Informed Consent Term (ICT). This study respected the ethical precepts of Resolution CNS 510/2016 and was performed according to the Declaration of Helsinki. This study was registered in the Brazilian Registry of Clinical Trials (ReBEC) under number ID: RBR-33dkw9y, https://ensaiosclinicos.gov.br/rg/RBR-33dkw9y, date of registration: Mar 29, 2022. Volunteers from Santos, SP, Brazil and the region were evaluated by a rheumatologist doctor and invited to participate. A trained physiotherapist carried out and prescribed the treatments. All procedures were conducted at the Federal University of São Paulo between May 2018 to Dec 2019.
Inclusion criteria
Women aged between 55 and 70 years, with pain in the knee for at least 6 months (reporting a pain level of more than >2 points on the Numeric Rating Pain Scale (NPRS), unilateral or bilateral KOA diagnosis (based on the criteria established by the American College of Rheumatology and with grades 2 or 3 of the Kellgren & Lawrence [13] classification and observed in the radiographic image by a specialist). Also, volunteers should present BMI between 22 to 35 kg/m2 and should be classified as irregularly active according to Criteria established by the International Physical Activity Questionnaire – Short Version (IPAQ).
Exclusion criteria
Women with lung diseases, cardiologic alterations, uncontrolled hypertension and diabetes mellitus or presenting any kind of previous musculoskeletal injury in the quadriceps femoris and/or hamstring muscles, orthopedic or rheumatic diseases, fibromyalgia, or pain that may prevent the physical exercise.
Randomization
The distribution of the subjects into the experimental groups was established by blind simple randomization by an external researcher through a computer program that created a random table of numbers in which each number corresponded to a specific group. The numbers were inserted into an opaque envelope and were given to the volunteers (consequently, subjects were blinded to the allocation of the treatment- single-blinded).
Subjects
A statistical power of 80% to detect a minimal clinical difference was previously defined for the sample calculation based on the level of pain in our pilot study. The sample size established was 34 subjects (17 subjects per group) and was calculated using 208 R Development Core Team [14] software.
Subjects included in the study were randomized into 2 groups: SMAG – Sensory-motor exercise associated with active PBM group and SMPG – Sensory-motor exercise associated with placebo PBM group.
Experimental procedures
The physical evaluation consisted of weight and height measurements, body mass index (BMI) calculation, assessment of the range of motion of the hip, knee and ankle by goniometry, medical history (diseases and medications) and physical exercise level by International Physical Activity Questionnaire–short version (IPAQ). Moreover, the following evaluations were performed: knee flexor and extensor muscle strength measurement, the severity of the injury, static and dynamic balance and level of pain as described below.
Measurement of knee flexor and extensor muscle strength
Subjects performed 3 series of Maximal Voluntary Isometric Torque (MVIT) in a prone position on a stretcher with the affected joint positioned at approximately 90° to assess knee flexor and extensor muscle strength. For avoiding compensatory movements during the evaluation, the distal segment (ankle) was firmly attached and stabilized by velcro straps connected to an adjustable cuff fixed to the cable [15]. A load cell (Model Miotool, Miotec, Porto Alegre, RS, Brazil) was used to collect force–time traces of the most affected member (firmly attached to an adjustable pole that permitted alignment perpendicular to the tested most affected member). To perform the evaluation, subjects were instructed to produce a movement as fast as can and hard as possible, sustaining the contraction for approximately 2-3 s with 1-min rest intervals between efforts. For analysis, one with the highest peak strength (kg) was used and if value variations were greater than 10% of the mean peak strength, the test was repeated. The peak torque value was calculated by dividing the value peak strength by the body mass value of each subject and multiplying by 100 to normalize. Then, the peak torque percentage was obtained.
Evaluation of the severity of the injury
Knee Injury and Osteoarthritis Outcome Score (KOOS) was used for evaluating the severity of the injury. It is constituted of 42 items, with 5 sub-scales, resulting in a score between 0 and 100 (0 representing extreme knee problems and 100 representing no knee problems). The sub-scales assess aspects such as knee pain, function in daily living, function in sport and recreation and quality of life [16].
Measurement of dynamic balance
The timed up-and-go test (TUG) was used to measure the dynamic balance. The time (seconds) for the subject to stand from a seated position, walk 3 meters, turn around, walk back and sit down was measured [17]. During the test, volunteers were instructed to walk at their regular speed and use a walking aid if necessary [18].
Measurement of the level of pain
The level of pain was assessed using an NPRS. Volunteers were instructed to score their pain on a numeric scale in a range from 0 (absence of pain) to 10 (worst possible pain) [19].
Interventions
Sensory-motor exercise program: SMEP used in this study was based on randomized and controlled studies about the effects of strength, balance, and proprioception exercises in patients with KOA [20]. The sensory-motor exercise program consisted in warming up (5 min on the treadmill), exercises (Standing posture: Retrowalking – 25 m, Walking on their toes – 25 m, Walking with eyes closed – 25 m, Balance with one leg on the floor and on the balancing, Toward the sides, back and front on a single foot with the eyes opened and closed; Lying posture: seated leg raise, seated lateral leg raise; Sitting posture: knee extensors chair, knee flexors chair, and sitting down and standing up from a high chair slowly) and stretching of the major muscle group. For the strength exercises, the subjects realized 3 sets of 10 repetitions each, with 30% (between the first session and forty sessions), 50% (fifth a ninth session) and 70% (tenth and sixteenth sessions) of 1 - RM (repetition maximum) and a rest interval of 2-3 min between sets.
Subjects were administered individual training sessions with a physical therapist for 8 consecutive weeks, twice a week (Monday and Wednesday), following the guidelines of the American Geriatrics Society (2001) [21]. During the study, subjects who developed any musculoskeletal injury did not perform the tests of the experimental procedures, did not perform at least 80% of training sessions, or missed two consecutive training sessions were excluded.
PBM via cluster
Subjects for SMPG and SMAG received, respectively, placebo or active PBM (Cluster; DMC®, São Carlos, SP, Brazil) after the end of each training session, on the medial and lateral region of the knee affected. In the SMAG, the irradiation parameters were: 7 infrared 808 nm wavelength, continuous output, 100mW peak irradiation power, 2 W/cm2 power density, 4J energy per point at seven points each side, the 40s at each application and 56J total energy per knee. To SMPG and SMAG, the same procedure was realized with turned-off equipment. A previous study [22] indicates these parameters for OA.
Statistical analysis
After checking data distribution through the Kolmogorov-Smirnov normality test and homogeneity of variances through the Levène test, the parametric statistic was chosen. For this reason, descriptive statistics were used with central tendency and dispersion measures (means and standard deviations), and three ANOVAs and four MANOVAs were used to compare group and treatment effects. Four additional ANOVAs were applied to analyze possible differences between demographic and anthropometric data. Furthermore, the linear regression test was used for correlated data (Pearson’s correlation test) to verify possible relationships between the peak torque variables through the groups (SMPG and SMAG) and treatment (before and after).
The Bonferroni post hoc test, if necessary, would be used for inter-group multiple comparison adjustments and the Tukey HSD post hoc test was used for possible interaction effects between factors. The level of significance was set at 5% (α = 0.05).
Results
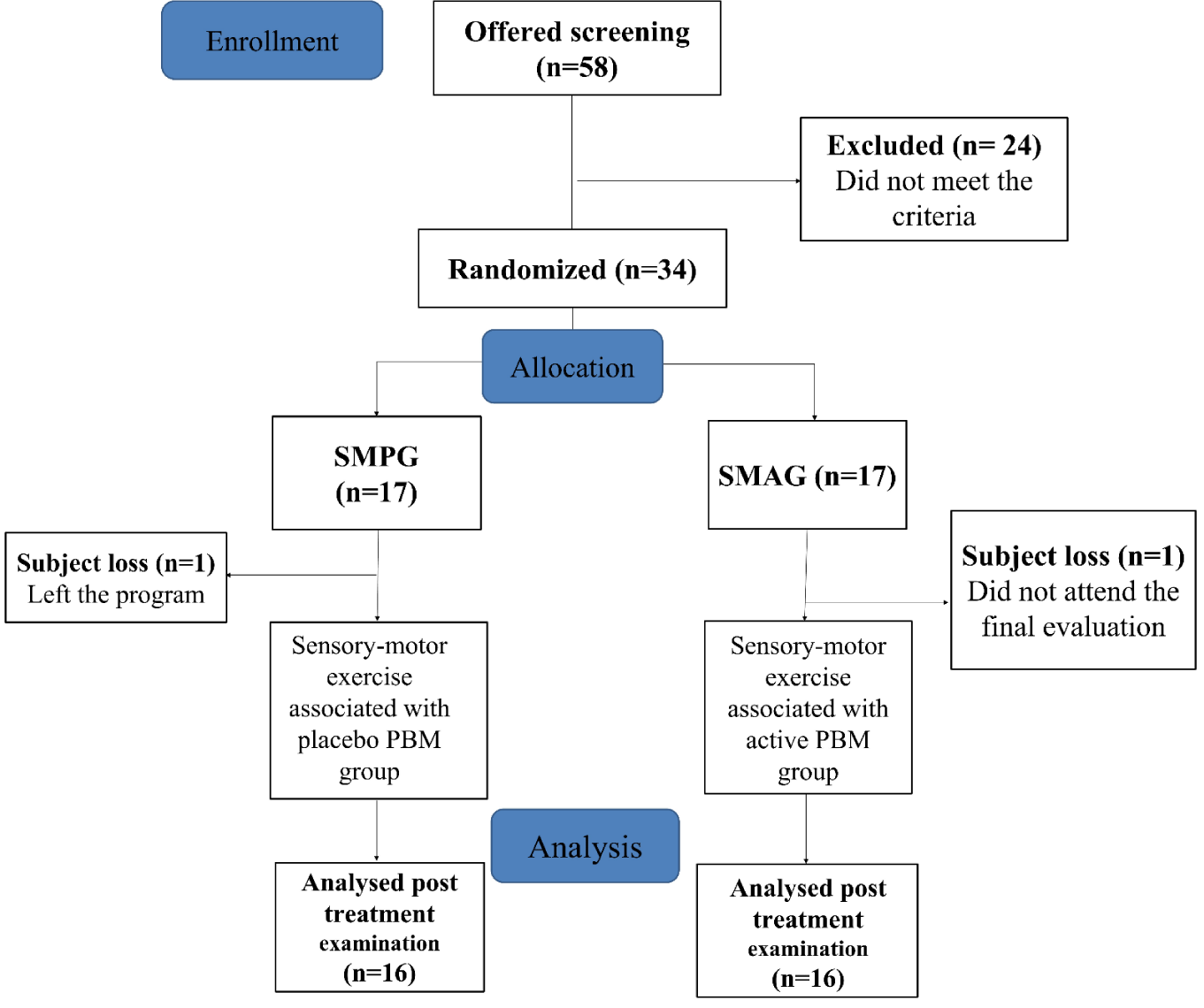
Initially, 58 women were recruited. Among these, 34 fitted the predetermined criteria of inclusion and signed the terms of free and clarified consent, but 32 subjects completed the study (Figure 1).
Demographic and anthropometric data of volunteers before the therapeutic interventions showed age (years) of 62.75 ± 4.91, weight (kg) of 73.69 ± 11.82, height (m) 1.59 ± 0.06, BMI of 28.99 ± 4.43 to SMAG, and age (years) of 64.37 ± 4.30, weight (kg) of 68.37 ± 12.59, height (m) 1.59 ± 0.09, BMI (kg/m2) of 27.07 ± 3.75 to SMPG. The statistical analysis showed no significant difference between groups (SMPG and SMAG).
For peak torque variables, there was no treatment effect (Wilks’ Lambda= 0.913; F(29,2) = 1.377; p = 0.268), neither of the group (Wilks’ Lambda = 0.889; F(29,2) = 1.803; p = 0.183) nor the interaction between treatment and group (Wilks’ Lambda = 0.945; F(29,2) = 0.850; p = 0.438) (Figure 2).
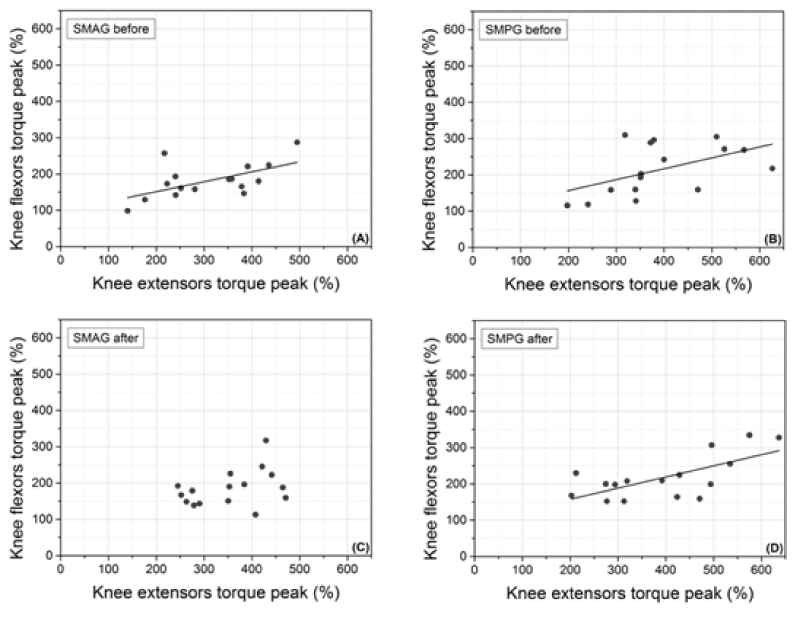
Linear regression tests showed positive and significant moderate correlations between peak torque of knee extensors and flexors to SMPG (r = 0.563; p = 0.023, Figure 3A) and SMAG (r = 0.589; p = 0.016, Figure 3B) before treatment. However, after treatment, there was a linear positive and significant high correlation only SMPG (r = 0.718; p = 0.002, Figure 3D).
KOOS variables showed treatment effect (Wilks’ Lambda = 0.466; F(25,6) = 4.782; p = 0.002), however, no-showed group effect (Wilks’ Lambda = 0.950; F(25,6) = 0.217; p = 0.968) and neither interaction between treatment and group (Wilks’ Lambda = 0.906; F(25,6) = 0.434; p = 0.849). Furthermore, a significant decrease for all variables evaluated (comparing the evaluation and reevaluation) through KOOS items was observed for both groups (symptoms F(30,1) = 8.159; p = 0.008; stiffness – F(30,1) = 4.343; p = 0.046; pain – F(30,1) = 12.895; p = 0.001; function/daily living – F(30,1) = 20.048; p < 0.001; sports and recreational activities – F(30,1) = 24.777; p < 0.001 and quality of life – F(30,1) = 16.289; p < 0.001) (Figure 4). However, no difference between groups after the intervention was observed.
Dynamic balance was better after treatment – F(30,1) = 22.555; p < 0.001; however, it did not show group effect – F(30,1) = 0.895; p = 0.352, nor the interaction between treatment and group – F (30,1) = 0.291; p = 0.594 (Figure 5). No difference between groups was observed after the therapeutic interventions.
The level of pain was lower after treatment – F(30,1) = 26.212; p < 0.001; however no group effect was observed – F(30,1) = 0.011; p = 0.916. There was also an interaction effect between treatment and group – F(30,1) = 4,478; p = 0.043. Post hoc tests showed that the pain in the SMAG was lower after treatment, which did not occur in the SMPG (Figure 6).
Discussion
As far as we know, there is no previous study investigating the association of both therapeutical interventions, SMEP and PBM, in women with KOA. The main findings demonstrated that all treated volunteers (with and without PBM) presented a significant improvement in balance and KOOS variables. Interesting exercised and irradiated volunteers demonstrated a reduced level of pain. No effect on muscle strength was observed after the treatments.
In the present study, the lack of increase in muscle strength after the therapeutical interventions may be related to the type of exercise performed. It is well known that sensory-motor exercises are important because they work in a weight-bearing position, emphasizing the quality of movement and corporal alignment [23]. Due to these effects, this type of exercise is involved in the reduction of the overload in the joint compartments, culminating in the improvement of pain, balance and function in patients with KOA. However, this regime of training lacks exercises focusing on the increase of strength, which may explain the present results. Likewise, PBM did not have any effect on these variables. PBM stimulates microcirculation and mitochondrial function and enhances ATP synthesis [24]. Considering these facts, it may be hypothesized that the contradictory results of the present study may be related to the type of exercise used and, consequently, the concomitant use of PBM did not have any effect on the increase in muscle strength.
Interestingly, the linear regression tests showed significant correlations between the peak torque of knee extensor and flexor muscles in both groups before treatment. It is known that one of the mechanisms capable of interfering with submaximal strength is the atherogenic muscle inhibition (AMI) process inevitable in patients with KOA [25]. This fact occurs because the articular pain and swelling activate abnormal afferent information in the local, leading to a decreased activation of the muscles acting on the joint (quadriceps and hamstrings in the case of the knee) due to inhibition of alpha motoneurons [25]. Curiously, after treatment only the irradiated volunteers maintained this correlation, being a possible explanation for the analgesic effect of PBM.
All volunteers presented significant improvement in balance with no extra effect of the association of PBM. It is well known that changes occur in articular and periarticular tissues of patients with OA that lead to a decrease in muscle strength related knee, which culminate in impairment in proprioception and poor balance control [26]. Thus, proper balance control is crucial to improve the functional capacity with consequence improvement of activities of daily living (ADL) in this patients [27]. Possibly, the positive outcomes can be explained by the type of exercise program performed, once, SMEP works out proprioception skills and muscle activation, improving sensorimotor system control and culminating in a better balance. Interestingly, PBM could not optimize the positive effects of SMEP on balance and, possibly related to the parameters used.
The KOOS variables were also improved after both therapeutic interventions but with no difference in the irradiated volunteers. These results corroborate the results found by Chaipinyo and Karoonsupcharoen [28] who found significant improvements in all domains of KOOS after home-based balance training in patients with OA. In the present study, the repetitive movements used in SMEP increase the ability the control joint movements and might have contributed to the improvement of pain relief, increased quality of life and function improvement of women with knee OA. In contrast, PBM could not optimize the positive effects of SMEP in KOOS variables. Possibly, the cluster device used in this study (7 diodes, 100mW each, dose of 4J per point and 56 J total per knee) [22] was high and did not provide extra improvements in these variables.
The most remarkable finding of the present study is the significant decrease in the level of pain only in the exercised and irradiated volunteers. The literature already evidenced that exercise programs and PBM is effective in improving pain in this population. In a clinical study performed by Alghadir, et al. [29], PBM was able to promote pain relief at rest and movement in patients with chronic knee OA. These results indicate that the association of the SMEP with laser energy offered by the cluster had a positive effect on this parameter.
It is important to highlight that the type of exercise used in this study, SMEP, promoted improvement in balance and KOOS variables. These results can be justified by the anti-inflammatory and antioxidant effects of PEPs on the autonomic nervous system [30]. However, according to the one guideline on exercise therapy for KOA, it’s necessary to discuss patient screening, evaluation during exercise sessions and adherence to the treatment [31]. Thus, approaching these topics may be useful for future studies.
More studies developing the association of therapies should be carried out. The literature has demonstrated that multi-modal physiotherapy (transcutaneous electrical nerve stimulation, low-level laser therapy, ultrasound, physical exercise and cryotherapy), when associated with an intra-articularl injection with the viscoelastic hyaluronic acid product, also promotes effective reduction of pain, stiffness, and improve ROM value and quality of life of patients with mild KOA [32].
As far as the authors know, this is the first study to verify the impact of a SMEP associated with PBM (via a cluster device) in women with knee OA. Cluster devices permit irradiation using many different spots at the same time with the aim of optimizing the PBM application (however, the ideal parameters for PBM application remain unclear) [27]. As this study was limited to a relatively short-term evaluation of the performance of physical exercise and PBM, information on the long-term performance of this therapeutic modality remains to be provided.
Conclusion
In the present study, sensory-motor exercises had beneficial effects on the severity of the injury and dynamic balance. The addition of PBM into SMEP produced an extra effect in pain relief. Nevertheless, more studies with long-term follow-up and using different methods of dynamic balance accuracy are needed. Adding PBM to routine exercise regimes for patients with knee OA should be investigated. Ultimately, it might be feasible to investigate different parameters of PBM in exercise regimes for this specific population.
Availability of data and materials: The dataset used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Authorship
PGV, ACMR, ABB, VZD and HTT are responsible for the concept and development of the study protocols. PGV and ABB are responsible for the interventions, implementation of the study and data collection. MRC was responsible for collation and analysis. PGV, ACMR and MRC were responsible for drafting the manuscript. All authors contributed to and approved the final manuscript.
Funding Information
Fundação de Amparo à Pesquisa do Estado de São Paulo (2018/18049-4)- Ana Beatriz Balão.
- Martel-Pelletier J, Barr AJ, Cicuttini FM, Conaghan PG, Cooper C, Goldring MB, Goldring SR, Jones G, Teichtahl AJ, Pelletier JP. Osteoarthritis. Nat Rev Dis Primers. 2016 Oct 13;2:16072. doi: 10.1038/nrdp.2016.72. PMID: 27734845.
- McAlindon TE, Driban JB, Henrotin Y, Hunter DJ, Jiang GL, Skou ST, Wang S, Schnitzer T. OARSI Clinical Trials Recommendations: Design, conduct, and reporting of clinical trials for knee osteoarthritis. Osteoarthritis Cartilage. 2015 May;23(5):747-60. doi: 10.1016/j.joca.2015.03.005. PMID: 25952346.
- Waller B, Ogonowska-Slodownik A, Vitor M, Lambeck J, Daly D, Kujala UM, Heinonen A. Effect of therapeutic aquatic exercise on symptoms and function associated with lower limb osteoarthritis: systematic review with meta-analysis. Phys Ther. 2014 Oct;94(10):1383-95. doi: 10.2522/ptj.20130417. Epub 2014 Jun 5. PMID: 24903110.
- Bartels EM, Henrotin Y, Bliddal H, Centonze P, Henriksen M. Relationship between weight loss in obese knee osteoarthritis patients and serum biomarkers of cartilage breakdown: secondary analyses of a randomised trial. Osteoarthritis Cartilage. 2017 Oct;25(10):1641-1646. doi: 10.1016/j.joca.2017.06.009. Epub 2017 Jul 6. PMID: 28689920.
- Braghin RMB, Libardi EC, Junqueira C, Nogueira-Barbosa MH, de Abreu DCC. Exercise on balance and function for knee osteoarthritis: A randomized controlled trial. J Bodyw Mov Ther. 2018 Jan;22(1):76-82. doi: 10.1016/j.jbmt.2017.04.006. Epub 2017 Apr 7. PMID: 29332761.
- Ferraz RB, Gualano B, Rodrigues R, Kurimori CO, Fuller R, Lima FR, DE Sá-Pinto AL, Roschel H. Benefits of Resistance Training with Blood Flow Restriction in Knee Osteoarthritis. Med Sci Sports Exerc. 2018 May;50(5):897-905. doi: 10.1249/MSS.0000000000001530. PMID: 29266093.
- Riis RGC, Henriksen M, Klokker L, Bartholdy C, Ellegaard K, Bandak E, Hansen BB, Bliddal H, Boesen M. The effects of intra-articular glucocorticoids and exercise on pain and synovitis assessed on static and dynamic magnetic resonance imaging in knee osteoarthritis: exploratory outcomes from a randomized controlled trial. Osteoarthritis Cartilage. 2017 Apr;25(4):481-491. doi: 10.1016/j.joca.2016.10.009. Epub 2016 Oct 13. PMID: 27746377.
- Sommer AP. Revisiting the Photon/Cell Interaction Mechanism in Low-Level Light Therapy. Photobiomodul Photomed Laser Surg. 2019 Jun;37(6):336-341. doi: 10.1089/photob.2018.4606. Epub 2019 May 20. PMID: 31107170.
- Sanches M, Assis L, Criniti C, Fernandes D, Tim C, Renno ACM. Chondroitin sulfate and glucosamine sulfate associated to photobiomodulation prevents degenerative morphological changes in an experimental model of osteoarthritis in rats. Lasers Med Sci. 2018 Apr;33(3):549-557. doi: 10.1007/s10103-017-2401-9. Epub 2017 Dec 1. PMID: 29196833.
- Assis L, Tim C, Magri A, Fernandes KR, Vassão PG, Renno ACM. Interleukin-10 and collagen type II immunoexpression are modulated by photobiomodulation associated to aerobic and aquatic exercises in an experimental model of osteoarthritis. Lasers Med Sci. 2018 Dec;33(9):1875-1882. doi: 10.1007/s10103-018-2541-6. Epub 2018 May 24. PMID: 29797102.
- de Paula Gomes CAF, Leal-Junior ECP, Dibai-Filho AV, de Oliveira AR, Bley AS, Biasotto-Gonzalez DA, de Tarso Camillo de Carvalho P. Incorporation of photobiomodulation therapy into a therapeutic exercise program for knee osteoarthritis: A placebo-controlled, randomized, clinical trial. Lasers Surg Med. 2018 Oct;50(8):819-828. doi: 10.1002/lsm.22939. Epub 2018 May 7. PMID: 29733117.
- de Matos Brunelli Braghin R, Libardi EC, Junqueira C, Rodrigues NC, Nogueira-Barbosa MH, Renno ACM, Carvalho de Abreu DC. The effect of low-level laser therapy and physical exercise on pain, stiffness, function, and spatiotemporal gait variables in subjects with bilateral knee osteoarthritis: a blind randomized clinical trial. Disabil Rehabil. 2019 Dec;41(26):3165-3172. doi: 10.1080/09638288.2018.1493160. Epub 2018 Oct 16. PMID: 30324827.
- KELLGREN JH, LAWRENCE JS. Radiological assessment of rheumatoid arthritis. Ann Rheum Dis. 1957 Dec;16(4):485-93. doi: 10.1136/ard.16.4.485. PMID: 13498603; PMCID: PMC1006994.
- R Core Team R: a language and environment for statistical computing. R Foundation for Statistical Computing, Vienna. 2016.
- Góes SM, Leite N, Shay BL, Homann D, Stefanello JM, Rodacki AL. Functional capacity, muscle strength and falls in women with fibromyalgia. Clin Biomech (Bristol, Avon). 2012 Jul;27(6):578-83. doi: 10.1016/j.clinbiomech.2011.12.009. Epub 2012 Jan 9. PMID: 22230426.
- Ross F, Triggs E, Cadbury H, Axford J, Victor C. Evaluation of education for people with osteoarthritis of the knee: recruitment and retention issues in study design. Nurse Res. 1998 Oct 1;6(1):49-59. doi: 10.7748/nr.6.1.49.s5. PMID: 27702162.
- Alfieri FM, Riberto M, Abril-Carreres A, Boldó-Alcaine M, Rusca-Castellet E, Garreta-Figuera R, Battistella LR. Effectiveness of an exercise program on postural control in frail older adults. Clin Interv Aging. 2012;7:593-8. doi: 10.2147/CIA.S36027. Epub 2012 Dec 18. PMID: 23269865; PMCID: PMC3529636.
- Dobson F, Hinman RS, Roos EM, Abbott JH, Stratford P, Davis AM, Buchbinder R, Snyder-Mackler L, Henrotin Y, Thumboo J, Hansen P, Bennell KL. OARSI recommended performance-based tests to assess physical function in people diagnosed with hip or knee osteoarthritis. Osteoarthritis Cartilage. 2013 Aug;21(8):1042-52. doi: 10.1016/j.joca.2013.05.002. Epub 2013 May 13. PMID: 23680877.
- Ferreira-Valente MA, Pais-Ribeiro JL, Jensen MP. Validity of four pain intensity rating scales. Pain. 2011 Oct;152(10):2399-2404. doi: 10.1016/j.pain.2011.07.005. PMID: 21856077.
- Diracoglu D, Aydin R, Baskent A, Celik A. Effects of kinesthesia and balance exercises in knee osteoarthritis. J Clin Rheumatol. 2005 Dec;11(6):303-10. doi: 10.1097/01.rhu.0000191213.37853.3d. PMID: 16371799.
- American Geriatrics Society Panel on Exercise and Osteoarthritis. Exercise prescription for older adults with osteoarthritis pain: consensus practice recommendations. A supplement to the AGS Clinical Practice Guidelines on the management of chronic pain in older adults. J Am Geriatr Soc. 2001 Jun;49(6):808-23. doi: 10.1046/j.1532-5415.2001.00496.x. Erratum in: J Am Geriatr Soc 2001 Oct;49(10):1400. PMID: 11480416.
- Hegedus B, Viharos L, Gervain M, Gálfi M. The effect of low-level laser in knee osteoarthritis: a double-blind, randomized, placebo-controlled trial. Photomed Laser Surg. 2009 Aug;27(4):577-84. doi: 10.1089/pho.2008.2297. PMID: 19530911; PMCID: PMC2957068.
- Bennell KL, Egerton T, Wrigley TV, Hodges PW, Hunt M, Roos EM, Kyriakides M, Metcalf B, Forbes A, Ageberg E, Hinman RS. Comparison of neuromuscular and quadriceps strengthening exercise in the treatment of varus malaligned knees with medial knee osteoarthritis: a randomised controlled trial protocol. BMC Musculoskelet Disord. 2011 Dec 5;12:276. doi: 10.1186/1471-2474-12-276. PMID: 22141334; PMCID: PMC3247187.
- Hamblin MR. Mechanisms and Mitochondrial Redox Signaling in Photobiomodulation. Photochem Photobiol. 2018 Mar;94(2):199-212. doi: 10.1111/php.12864. Epub 2018 Jan 19. PMID: 29164625; PMCID: PMC5844808.
- Rafsanjani H, Khademi-Kalantari K, Rezasoltani A, Naimi SS, Ghasemi M, Jaberzadeh S. Immediate effect of common peroneal nerve electrical stimulation on quadriceps muscle arthrogenic inhibition in patients with knee osteoarthritis. J Bodyw Mov Ther. 2017 Oct;21(4):879-883. doi: 10.1016/j.jbmt.2017.03.003. Epub 2017 Mar 4. PMID: 29037643.
- van der Esch M, Steultjens M, Harlaar J, Knol D, Lems W, Dekker J. Joint proprioception, muscle strength, and functional ability in patients with osteoarthritis of the knee. Arthritis Rheum. 2007 Jun 15;57(5):787-93. doi: 10.1002/art.22779. PMID: 17530678.
- Duman I, Taskaynatan MA, Mohur H, Tan AK. Assessment of the impact of proprioceptive exercises on balance and proprioception in patients with advanced knee osteoarthritis. Rheumatol Int. 2012 Dec;32(12):3793-8. doi: 10.1007/s00296-011-2272-5. Epub 2011 Dec 21. PMID: 22187058.
- Chaipinyo K, Karoonsupcharoen O. No difference between home-based strength training and home-based balance training on pain in patients with knee osteoarthritis: a randomised trial. Aust J Physiother. 2009;55(1):25-30. doi: 10.1016/s0004-9514(09)70057-1. PMID: 19226239.
- Alghadir A, Omar MT, Al-Askar AB, Al-Muteri NK. Effect of low-level laser therapy in patients with chronic knee osteoarthritis: a single-blinded randomized clinical study. Lasers Med Sci. 2014 Mar;29(2):749-55. doi: 10.1007/s10103-013-1393-3. Epub 2013 Aug 3. PMID: 23912778.
- Daniela M, Catalina L, Ilie O, Paula M, Daniel-Andrei I, Ioana B. Effects of Exercise Training on the Autonomic Nervous System with a Focus on Anti-Inflammatory and Antioxidants Effects. Antioxidants (Basel). 2022 Feb 10;11(2):350. doi: 10.3390/antiox11020350. PMID: 35204231; PMCID: PMC8868289.
- Shallwani SM, King J, Thomas R, Thevenot O, De Angelis G, Aburub AS, Brosseau L. Methodological quality of clinical practice guidelines with physical activity recommendations for people diagnosed with cancer: A systematic critical appraisal using the AGREE II tool. PLoS One. 2019 Apr 10;14(4):e0214846. doi: 10.1371/journal.pone.0214846. PMID: 30969981; PMCID: PMC6457630.
- Onu I, Matei D, Sardaru DP, Cascaval D, Onu A, Gherghel R, Serban IL, Mocanu GD, Iordan DA, Murariu G, Galaction AI. Rehabilitation of Patients with Moderate Knee Osteoarthritis Using Hyaluronic Acid Viscosupplementation and Physiotherapy. Appl. Sci. 2022; 12:3165. https://doi.org/10.3390/app12063165

Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.



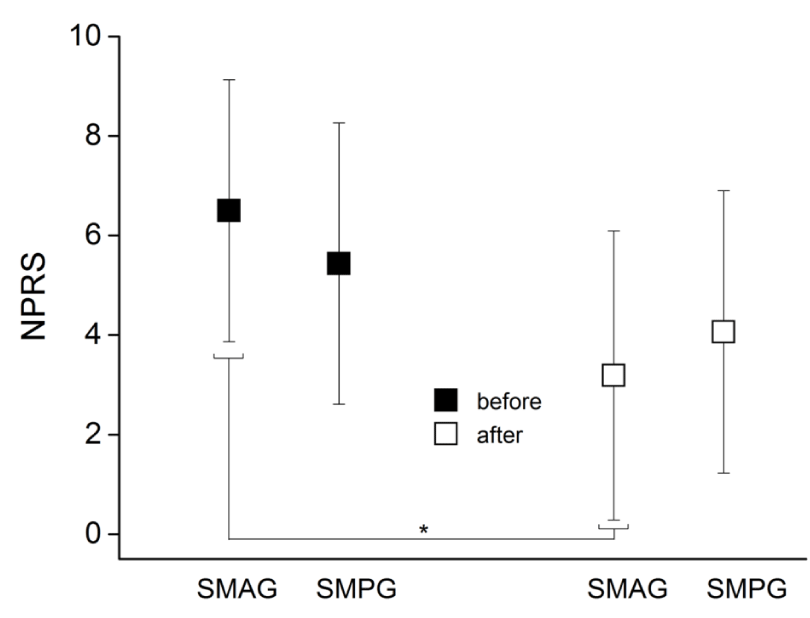

 Save to Mendeley
Save to Mendeley
