Global Journal of Cancer Therapy
Experiences of women receiving high dose rate brachytherapy for cervical cancer at ocean road cancer institute Dar-es-salaam Tanzania
Francis Kazoba1* and Nazima Dharsee2
2Department of Clinical Oncology, Ocean Road, Cancer Institute (ORCI), P.O Box 3592 Dar es Salaam, Tanzania
Cite this as
Kazoba F, Dharsee N (2020) Experiences of women receiving high dose rate brachytherapy for cervical cancer at ocean road cancer institute Dar-es-salaam Tanzania. Glob J Cancer Ther 6(1): 023-027. DOI: 10.17352/2581-5407.000031The objective of this study was to present a descriptive summary of the experiences of women treated with high dose rate brachytherapy for cervical cancer. A qualitative descriptive study design was used and 50 women who undergo high dose rate brachytherapy at Ocean Road Cancer Institute (ORCI) in Dar-es-salaam were selected. Qualitative interviewer administered questionnaire was used for data collection from cervical cancer patients treated between April 2019 to July 2019 for descriptive and thematic analysis of data. Qualitative interviewer administered questioning was done from which three themes arose: the patient perception, expectation and impressions, informational need, and psychological experiences. Many patients had good perception about brachytherapy although their first impression was bad. The study found the importance of provision of procedure information to patient which seems to improve their treatment experiences. The psychological experiences faced by patients before and during treatment included pain, distress, fear, humiliation and anxiety Pain was a major problem, as the preventative medication participants received had low efficiency in pain prevention hence did not protect them from experiencing pain. Opening and hanging their legs was a humiliating experience aggravated by the presence of doctors and nurses. Their belief that brachytherapy can cure their disease comforted them and gave them courage to endure the treatment, whilst caring staff comforted and supported them. In addition to individualized patient education, nurses should assess the level of pain women experience before, during and after receiving brachytherapy and advice the revision of pain management protocols.
Background of the study
Cervical cancer is a health problem of the developing world, as approximately 84% of all women diagnosed with this disease live in developing regions. According to Denny, it is estimated that 78 897 women living in Africa will be diagnosed with cervical cancer annually, whilst 61 671 (78%) will die from this disease [1,2]. Late presentation and lack of treatment facilities contribute to the high death rate. In the global south, cervical cancer remains the second most common cancer (after breast cancer) among women of reproductive age. Worldwide, it is the third most common carcinoma after breast cancer and colorectal cancer. Unlike other cancers, cervical cancer is almost 100% preventable by ensuring that women receive quality screening and treatment of precancerous lesions [3]. The impact of secondary prevention efforts for cervical cancer prevention in high resource settings is impressive. Despite this, the World Health Organization (WHO) estimates of global cervical cancer rates remain sobering, with more than 500,000 new cases diagnosed each year. Of those cases, more than 85% of women hail from developing countries where access to primary and secondary prevention is far from universal [4]. In these settings, most women diagnosed with cervical cancer in developing countries present at late stages when curative treatments are often no longer possible. East Africa has the highest rate of cervical cancer in the world. In this region, the Age-Standardized Incidence Rate (ASR) is estimated at 42.7 new cases per 100,000 women ASR rates range from Malawi at 75.9/100,000 to Kenya at 40.1/100.000. Tanzania ranks second in the region with an ASR of 54.9/100,000 women. Similar to other East African countries, cervical cancer is the leading cause of cancer and cancer-related death among Tanzanian women. Each year more than 7,300 Tanzanian women are diagnosed with cervical cancer. More than half of these women die as they are diagnosed at a late stage of the disease [5].
Treatment of cervical cancer involves surgery, chemotherapy and radiation therapy. The treatment involves curative and palliative mode example women with stage IVB cervical cancer receives palliative care. Women with early stage cervical cancer fit for surgery to remove the tumor which is called radical hysterectomy. Patients with advanced stages such as stage IIB to IVA are treated with radiotherapy with or without concurrent chemotherapy. Radiotherapy involves external beam radiotherapy and brachytherapy. According to the Journal of Contemporary Brachytherapy (JCB), Most of cancer treatment involves both External beam radiotherapy and Brachytherapy. Brachytherapy has become a standard treatment for cervical cancer patients either in radical or palliative treatment. Brachytherapy has a potential to deliver a high dose in a short time directly to the affected tissue with the advantage of rapid fall-off in dose hence sparing the adjacent healthy organs [6]. s very effective in treating cancer, as the radiation is delivered with a high level of accuracy has a minimized risk of side effects, due to the targeted and precise nature of delivering the radiotherapy from inside the body, is a minimally invasive technique – i.e. it doesn’t involve extensive surgery, can be performed on an outpatient basis hence avoiding the need for an overnight stay in hospital in many cases, requires very short treatment times (typically from 1 to 5 days), has short recovery times (typically 2 to 5 days) people can usually return to everyday activities very quickly requires fewer visits to the hospital and overnight stays than other options, and the benefits of brachytherapy can enable you to get back to your everyday life sooner with minimal disruption. There is little knowledge about those experiences. Knowing the experiences of women receiving high dose rate brachytherapy improves patient experiences before and during treatment hence good outcome after treatment. Improvement of pain relief drug efficiency could reduce pain during insertion of uterine and vaginal applicators [7,8].
Material and methods
Setting and sample
The setting was an academic and only cancer treatment hospital in Dar-es-salaam city Tanzania. The hospital offers specialist inpatient and outpatient services and serves as referral hospital for cancer patients from a number of regional hospitals. Approximately half of the patients treated at the Department of Radiation therapy suffer from gynecological cancer. Most patients referred to the department are treated on an outpatient basis; those who are too ill to come to the hospital on a daily basis are admitted to the ward. In addition, patients who live far from the hospital and are not able to afford transport costs to and from the hospital are also admitted. The study sample consisted of 50 women, who were to receive high dose rate brachytherapy at Ocean Road Cancer Institute academic and main cancer care hospital in the country. Participants were between 30 and 65 years old, with an average of 47.5. Most of women were married and peasant by occupation. The proportion of Muslims was larger than that of Christians [9].
Methods
Qualitative descriptive study design was used. This study data was collected using Interviewer- Administered questionnaire to obtain the information regarding the experiences and expectations of women receiving high dose rate brachytherapy for cervical cancer. The data collected were on social demographic information, physical experiences, psychological experiences, and disposition towards treatment. The duration of data collection was from April 2019 to July 2019. After obtaining ethical clearance and permission from the university and hospital, approached eligible women scheduled for brachytherapy and invited them to participate in the study. Participation was voluntary and informed consent in writing, was obtained from the volunteers. Interviewer- Administered questionnaires, used to determine individuals’ perceptions and opinions, were conducted in Swahili in a private room, with only the researcher and participant present, for an average of half an hour [10].
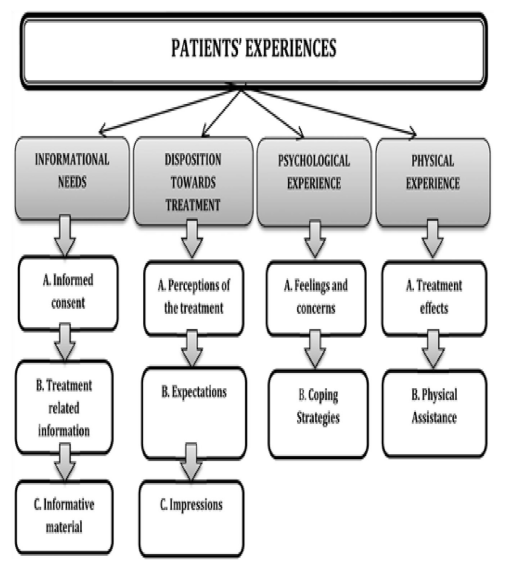
Conceptual framework
Results
Social demographic characteristics
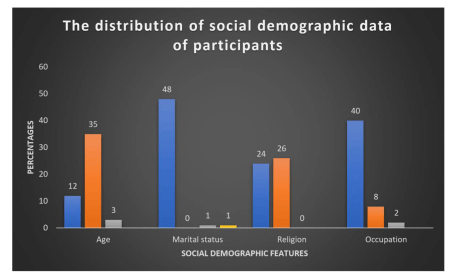
A total of fifty women receiving high dose rate brachytherapy for cervical cancer at Ocean Road Cancer Institute participated in this study in filling of interviewer administered questionnaires. The mean age was 47.5 years and majority of women were married 48 (96%). 40 (80% ) of participants were peasant by occupation and 24 out of 50 women (48%) were Christians and 26 (52&) were Muslims Figure 1.
Three themes arose from the study which are patient perception, expectation and impressions, informational need and psychological experiences [11].
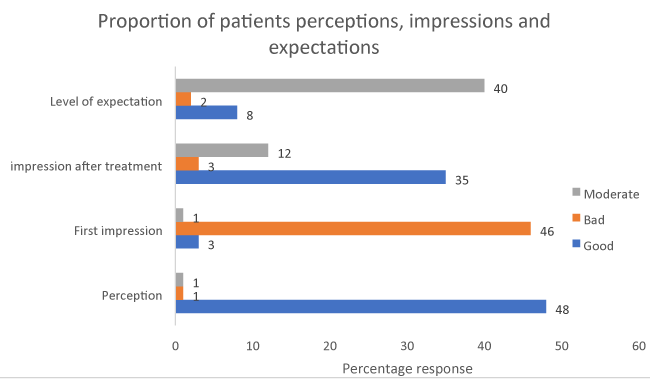
Patient perception, expectation and impressions
Many patients had good perception about brachytherapy treatment before treatment 48 (96%) because they believed it cures their disease although the first impression on brachytherapy was bad for most of patients because of stories about the procedures from other patients who already had brachytherapy. After first treatment many patients had good impression on brachytherapy 38 (76%). Majority of patient expectations was less than expected because they expected brachytherapy to be bad but they found it good after first treatment 40 (80%) Figure 2 [12].
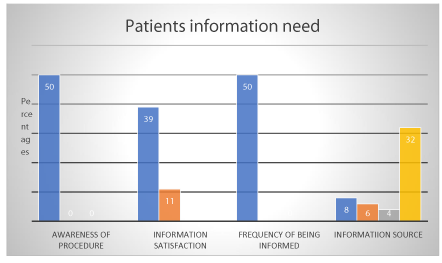
Informational needs
Being provided with information about brachytherapy procedures was another them which arose during the study. Many participants had very few information about the procedure. Regarding the awareness of the procedure, all participants were aware. 39 participants (78%) were slightly satisfied with the information about treatment procedures since they had no enough information. The frequency of being given information about the treatment procedure was once for majority of patients 45 (95%). The information source for most patients were from healthcare workers 44(88%) Figure 3.
Psychological experiences
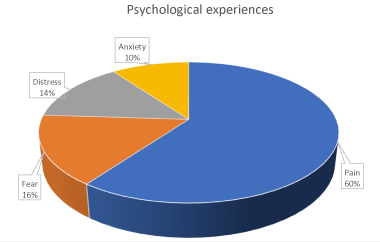
The psychological experiences experienced by the participants in the study were pain, distress, fear humiliation and anxiety. Pain was the major complain especially during the insertion of uterine and vaginal applicators in the cervix. The participants explained that the painful medication given to them was not enough for pain relief. Receiving brachytherapy also caused fear to women due to stories which they were told by their fellow who already had brachytherapy treatment. It was a negative experience to most participants because they experienced emotional distress before, during and after having brachytherapy. Presence of many people in a preparatory room made the participants to consider brachytherapy as humiliating procedure Figure 4.
Discussion
Treatment of cervical cancer patients by brachytherapy is a mandatory procedure if the intent of patient is curative. Despite of it being a significant treatment for cervical cancer patients with stage II to stage IV, it can be a worst experience due to the complexity nature of the procedure. In this study participants were associated with pain, distress, fear, anxiety and considered as humiliation. The study categorized the experiences into four parts as patients’ perceptions, expectations and impression, informational needs, and psychological experiences. Pain was a major negative experience for most women in this study as compared to the study done by AD Dzaka and JE Maree (2016) in south Africa which showed that pain is a major problem for women receiving high dose rate brachytherapy for cervical cancer. The study by AD Dzaka and JE Maree also explained the informational need by patients that they should be provided with enough information regarding their treatment which can help to improve their experiences. This study also revealed distress, humiliation and fear as the psychological experiences which were also found in the study by AD Dzaka and JE Maree in south Africa. Some participants felt unprepared and uninformed and experienced the health professionals as uncaring. In addition, having more than the essential staff present when they were at their most vulnerable, lying on their backs with their legs ‘wide open’, added to their emotional distress. Velji and Fitch [13] who investigated the experiences of Canadian women who received brachytherapy, found the information that women received prior to the treatment and the care they received from nurses during the procedure shaped their experience positively or negatively. In addition, Brand [14] found a significant relationship between the fear and anxiety women experience before brachytherapy and hence information needs. Considering these factors, it is not surprising that the women in the study feared brachytherapy and considered it a negative experience. However, to conclude that the negative experiences of the participants were caused by their information needs and the lack of care they expected would be over-simplifying a complex issue and should be investigated before definite deductions can be made. In contrast with the findings of Velji and Fitch [13,14], who found that the treatment modality itself did not play an important role in how women experience this treatment, the nature of the procedure expressed as ‘shoving stuff in your vagina’ played a major role in how our participants experienced brachytherapy. The participants experienced both physical and emotional pain. Participants feared the procedure before they had been treated and even the follow-up treatments. Andersen, Karlsson, Anderson and Tewfik [15,16], when exploring survivorship issues in women diagnosed with gynaecological cancer, found levels of anxiety and distress in women remained high before, during and after brachytherapy. Kwekkeboom, Dendaas, Straub and collegues16 found that pre-treatment distress was significantly higher than that experienced before the second brachytherapy. It is unclear whether the distress levels of women in the current study decreased after the first treatment as the number of treatments was not taken into consideration and distress levels were not measured. However, distress after the first treatment was still a reality for the women in our study. The severe pain participants experienced, described as ‘cutting’ and ‘I could not take the pain’, added to their suffering. According to Arnold, Lee and Stuart [17] and Chapman [18] pain is a common symptom amongst persons receiving any form of cancer treatment and is a reality for about 50–53% of patients at all disease stages and about 62–88% of patients with advanced disease. Nail [19] found most women diagnosed with gynaecological cancer experience varying degrees of pain during brachytherapy, which, according to Kwekkeboom, Dendaas, Straub, et al. [16], ranges from mild to moderate. In addition, Rollison and Strang [20] found more than half (13 of 20) of the patients in their study experienced moderate to severe pain during this procedure. Although the current study did not assess the levels of pain, it provides evidence of the experience of severe pain during brachytherapy procedures. As evident by ‘that pill and injection didn’t drug me’, the conscious sedation participants received did not prevent them from experiencing pain. The way pain is managed does not seem to be best practice as, according to Puntillo, Wild, Morris, et al. [21] and Gordon, Dahl, Miaskowski and colleagues [22], unlike other forms of cancer pain, procedural pain can be anticipated and prevented. As described by ‘I couldn’t sleep, I’m thinking of the agony I’m gonna go through’, women experienced high levels of anxiety. Warnock [23], on investigating experiences of gynaecological cancer patients treated with brachytherapy, found a relationship between pain and anxiety and difficulty coping during the procedure. However, it was unclear whether the pain was raised by the anxiety or the anxiety resulted in pain. The emotional pain of having to lie in the lithotomy position with your legs wide open adds to the complexity of the pain experience. In addition, it was interesting to find the participants preferred childbirth, described by Simkin [24], as the ultimate painful, emotionally distressing, vulnerable and exhausting event in a woman’s life, to having to undergo brachytherapy. It can only be concluded, as supported by Velji and Fitch [14] and Kwekkeboom Dendaas, Straub and colleagues [16], that brachytherapy is a very unpleasant and the study also had similar findings as the study done by Deirdre Long, Hester Sophia Friedrich- Nel and Georgina Joubert in 2012 South Africa that explained the importance of provision of information regarding treatment procedures and overall treatment to patients. The study showed the importance of providing information to patients regarding disease, treatment and possible side effects that reduce the feeling of fear and anxiety toward their treatment. Patient expectations, perception and impression were found to be negative before treatment but after the first treatment the negativity changed and patient considered brachytherapy as a excellent and necessary treatment [25].
This was similar as the study done by Alicia Ehlers and Chandra Rekha Makanjee in 2017 about Exploration of gynaecological cancer high dose rate brachytherapy treatment which findings showed that brachytherapy was considered as a sensitive procedure which requires better preparation and treatment procedures information to patients.
The study also found that the efficiency of drug used for pain relief during insertion of uterine and vaginal applicators is very low. This finding is similar to the study done by Theresa N Elumela and Abbas A.Abdus –Salam on the topical anaesthesia for pain relief during high dose rate brachytherapy in 2014. The study suggested the addition of local vaginal anaesthesia with 10% xylocaine spray to conscious sedation. Some of study limitation included limited budget and time and only few studies explain about the experiences of women receiving high dose rate brachytherapy [26].
Conclusion
Within Tanzania this is one of few studies that explains the experiences of women receiving high dose rate brachytherapy for cervical cancer. The study explained the perception, expectations and impressions toward brachytherapy, informational need by patients and psychological experiences.
Being treated with brachytherapy was a negative experience causing fear, pain and humiliation. The participants feared the procedure, before receiving the first treatment. Having many people in the preparatory room made the participants feel like they are humiliated – lying on their backs with their legs wide open-was a humiliating experience. The pain participants experienced was severe some could not help but cry out, as the preventative medication they received did not stop the pain completely. The dysuria they experienced after the treatment added to their suffering. However, their belief that brachytherapy can cure their disease comforted them and gave them courage to endure the treatment, whilst caring staff also comforted and supported them. Patients should receive individualized education regarding the procedure, and the rotation of doctors and presence of observers could be minimized. In addition, doctors could explain the procedure and inform patients what the next step would be so that they are prepared for what would be happening to them. Nurses should assess the level of pain women experience before, during and after receiving brachytherapy and, based on the findings, advice the revision of pain management protocols. Non-drug options used in pain management could also be considered to complement pharmacological interventions.
- International Agency for Research on Cancer and World Health Organization (2015). Globocan 2012: estimated cancer incidence, mortality and prevalence worldwide in 2012. Link: https://bit.ly/2PZO7dJ
- Denny L (2010) Cervical cancer in South Africa: an overview of current status and prevention strategies. Cont Med Ed 28: 70-73. Link: https://bit.ly/322XCi8
- Moodley J, Harries J, Barone M (2009) Misinformation and lack of knowledge hinder cervical cancer prevention. SAMJ 99: 128. Link: https://bit.ly/2PYdA7A
- National Health Laboratory Service (2015) Cancer in South Africa 2010: full report. The National Institute for Occupational Health. Link: https://bit.ly/2Fr9nHk
- International Atomic Energy Agency (2012) Management of cervical cancer: Strategies for limited-resource centres: a guide for radiation oncologists. Vienna: IAEA.
- Sandelowski M (2000) Whatever happened to qualitative description? Res Nurs Health 23: 334-340. Link: https://bit.ly/348Js1u
- McCarthy G, O’Sullivan D (2008) Evaluating the literature. In: Watson R, McKenna H, Cowman S, Keady J, editors. Nursing research. Designs and methods. Edinburgh: Churchill Livingstone 113-123.
- Grove S, Bruns N, Gray J (2013) The practice of nursing research. Appraisal, synthesis and generation of evidence. 7th ed. St Louis (MI): Elsevier. Link: https://bit.ly/3h2a4ou
- Polit D, Beck C (2010) Essentials of nursing research. Appraising evidence for nursing practice. 7th ed. Philadelphia, PA: Lippincott Williams & Wilkins. Link: https://bit.ly/2Q4jkwE
- Shenton A (2004) Strategies for ensuring trustworthiness in qualitative research projects. Ed Inform 63-75. Link: https://bit.ly/3geCTgt
- Malterud K (2001) Qualitative research: standards, challenges, and guidelines. Lancet 358: 483-488. Link: https://bit.ly/349H6zy
- Pillow W (2003) Confession, catharsis, or cure? Rethinking the uses of reflexivity as methodological power in qualitative research. Int J Qual Stud Educ 16: 175-196. Link: https://bit.ly/2Q1BW07
- Velji K, Fitch M (2001) The experience of women receiving brachytherapy for gynecologic cancer. Onc Nurs Forum 28: 743-751. Link: https://bit.ly/2Yb5PzL
- Brandt B (1991) Informational needs and selected variables in patients receiving brachytherapy. Onc Nurs Forum 18: 1221-1227. Link: https://bit.ly/2DTtiyw
- Andersen BL, Karlsson JA, Anderson B, Tewfik HH (1984) Anxiety and cancer treatment: response to stressful radiotherapy. Health Psychol 3: 535. Link: https://bit.ly/2Q2ia4G
- Kwekkeboom KL, Dendaas NR, Straub M, Bradley KA (2009) Patterns of pain and distress during high-dose-rate intracavity brachytherapy for cervical cancer. J Support Oncol 7: 108–114. Link: https://bit.ly/3iMZYIH
- Arnold G, Lee J, Stuart P (2007) Pain in palliative care. In: McGann K, editor. Fundamental aspects of pain assessment & management. London: Mark Allen 77–93.
- Chapman S (2012) Cancer pain part 1: causes and classification. Nurs Stand 26: 42-46. Link: https://bit.ly/3495TDD
- Nail L (1990) Involving clinicians in nursing research. Onc Nurs Forum 17: 621-623.
- Rollison B, Strang P (1995) Pain, nausea and anxiety during intra-uterine brachytherapy of cervical carcinomas. Supp Care Cancer 3: 205-207. Link: https://bit.ly/3iP2HkF
- Puntillo KA, Wild LR, Morris AB, Stanik-Hutt J, Thompson CL, et al. (2002) Practices and predictors of analgesic interventions for adults undergoing painful procedures. Am J Critic Care 11: 415-429. Link: https://bit.ly/2CBFjb7
- Gordon DB, Dahl JL, Miaskowski C (2005) American Pain Society recommendations for improving the quality of acute and cancer pain management. Arch Inter Med 165: 1574-1580. Link: https://bit.ly/3azjdlX
- Warnock C (2005) Patients’ experiences of intracavity brachytherapy treatment for gynaecological cancer. Eur J Oncol Nurs 9: 44-55. Link: https://bit.ly/3azQAFj
- Simkin P (1996) The experience of maternity in a woman’s life. J Obstet Gynecol Neonatal Nurs 25: 247-252. Link: https://bit.ly/2E5NUDs
- Wachholtz AB, Pearce MJ, Koenig H (2007) Exploring the relationship between spirituality, coping, and pain. J Behav Med 30: 311-318. Link: https://bit.ly/348Bcyt
- Attree M (2001) Patients’ and relatives’ experiences and perspectives of ‘Good’ and ‘Not so Good’ quality care. J Advance Nurs 33: 456-466. Link: https://bit.ly/2Q2VXU0

Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.
 Save to Mendeley
Save to Mendeley
