Global Journal of Allergy
Diagnostic accuracy of skin prick test and specific IgE and their association with Total IgE, AEC and serum cortisol in Indian patients with respiratory allergy
PC Kathuria1*, Manisha Rai2 and Neelam2
2Clinical Assistant, BLK Super Specialty Hospital & National Allergy Centre, New Delhi, India
Cite this as
Kathuria PC, Rai M, Neelam (2021) Diagnostic accuracy of skin prick test and specific IgE and their association with Total IgE, AEC and serum cortisol in Indian patients with respiratory allergy. Glob J Allergy 7(1): 001-006. DOI: 10.17352/2455-8141.000024Background: Indian subcontinent has high burden of patients suffering from respiratory allergy associated with food sensitization. Immune response is different in skin and blood for allergen sensitization. Skin Prick Test (SPT) and Specific IgE (s IgE) allergen positivity is an evidence of sensitization. Both these tests (SPT & sIgE) are often used interchangeably in clinical practice of allergic disorders. In our study the concordance relevance of various tests SPT, sIgE, Total IgE, Absolute Eosinophil Count (AEC) & Serum Cortisol was investigated in 75 patients of respiratory allergy. The aeroallergens were divided into four groups (Dust mite, Pollen, Fungi, Cockroach) & 7 Foods (Milk, Soybean, Wheat, Fish, Peanut, Egg white, Yeast). Total 35 common allergens were tested by SPT. Serum Specific IgE estimation was carried out with 16 allergens (D. pteronyssinus, D. farinae, Alternaria alternata, Candida albicans, Aspergillus fumigatus, mesquite (Prosopis juliflora), common pigweed, goosefoot lamb’s quarter (Chenopodium album), cockroach and seven food allergens (milk, soybean, wheat, fish, peanut, egg white, yeast).
Methods and findings: A retrospective stratified sample of 75 respiratory allergic patients within age group of 05-70 years was included in the study. Serum total IgE and specific IgE levels were estimated by using ImmunoCAP® system and SPT was done by standardized allergens (Allergo Pharma and Greer laboratories Inc.).
Following results were compared to evaluate concordance/ discordance between various markers for respiratory allergy.
1. Sensitizations pattern based on Serum (16 specific IgE >1 kU/ml) with Skin prick tests Positive >4 mm wheal Size (35 aero-allergens)
2. Serum Total IgE levels >250 IU/ml with Sensitizations based on Serum (16 specific IgE >1 kU/ml) with Skin Prick Tests Positive >4 mm wheal Size (35 aero-allergens)
3. Absolute Eosinophil Count >200 cells/uL with Sensitizations based on Serum (16 specific IgE >1 kU/ml) with Skin Prick Tests Positive >4 mm wheal Size (35 aero-allergens)
4. Serum cortisol level <10 mcg/dL with Sensitizations based on Serum (16 specific IgE >1 kU/ml) with Skin Prick Test Positive >4 mm wheal Size (35 aero-allergens).
Introduction
There is a consistent increase in allergic diseases from 10 to 30 % for the last 50 years in India [1]. The global prevalence of Allergic Rhinitis is between 10 to 30 % for adults and as high as 40% for children [2]. SPT and Measurement of sIgE are important tools for diagnosing atopic sensitization and both tests are often used interchangeably. There is no universally acceptable gold standard cut off value for either of these tests associated with allergic diseases, although practice parameter third update guidelines recommends that wheal size threshold of > 3mm cutoff criteria has better clinical accuracy which is based on reproducibility in relation to nasal provocation test. There are several factors which can modify the test such as skill of the tester, the testing device, the color of the skin, skin reactivity on the day of testing, potency and stability of allergen extract reagent [3,4].
The choice of cut off value for blood specific IgE has not been mentioned in guidelines, so Serum specific IgE is often overused and misused for allergic diagnosis. The cut off value for sIgE that distinguishes between an allergic and non-allergic individual has been difficult to define. Serum specific IgE antibody to different allergens have different cut off values depending on the type of the allergens, nature of allergens, concentration of allergen exposure and duration of allergens exposure. Children raised with high exposure to dust mite allergens will have high titers of sIgE antibodies to dust mite allergens [5,6].
There is a strong association between acute episodes of respiratory allergy (Allergic Asthma) with increase in total IgE > 250 IU/Ml). Most individuals have very low level of circulatory serum IgE (< 100 IU/ml where 1 IU = 2.4 ng IgE). Allergen specific IgE should be considered as a marker for atopy and IgE sensitization but it cannot predict clinical severity of reactions and will have to be interpreted on the basis of the individual’s case history [7,8].
There is a complex interaction of neuroendocrine and metabolic immune system. Inhaled corticosteroids are the mainstay treatment for respiratory allergy and there is an increasing concern about their systemic side effects especially adrenal suppression. Basal serum cortisol is an indirect biomarker for detecting suppression of HPAA and the disease severity [9].
Peripheral blood eosinophilia is a hallmark of severe allergic disease and correlates with severity of the disease due to synthesis of IL5-prominent Th2-driven immune response. Infiltrating eosinophils release MBP, ECP, and EPO which in turn injure the nasal epithelial cells and induce hyper responsiveness & chronic remodeling [10,11].
Methods
Data from 75 participants coming to outpatient department of National Allergy Centre, presenting with respiratory allergy was analyzed retrospectively. The patients were without history of food allergy as recorded using a standard questionnaire.
These patients were aged between 05-70 years and comprised of 49 (65.3%) males and 26 (34.7%) females.
All these patients were also sub- categorized into different age groups (Figure 1).
The patients were without any history of food allergy as recorded using a standard questionnaire.
The diagnosis of Respiratory Allergy (allergic asthma with rhinitis) was made based on history and clinical investigations following the criteria of GINA guidelines (2014) [12,13].
Skin Prick Tests (SPT)
Data obtained from SPT tests by various allergens of these patients was recorded. Sensitization to food (7 Allergens) and common environmental allergens (35 standardized): (Pollen/Fungi/Dust mite/ Cockroach) (Allergo Pharma & Greer lab Inc.) were tested. The skin test reactions were tested with standardized allergens and were graded after 20 minutes in comparison to the wheal size of positive control, i.e. histamine diphosphate (10 mg/ml). In which maximum horizontal diameter of wheal >4 mm was considered as immunologically significant positive reaction. Why is there a low level of agreement between SPT & s pIgE in case of fungi & food allergens? It could be because of the presence of different extracts of proteins and Epitopes present in the commercial SPT kits. In our study SPT was done with Alk Lancet which is reliable, tolerable and comparable with other devices [14,15].
Total IgE estimation: Serum total IgE estimation was carried out for each patient by ImmunoCAP® in 75 subjects
Specific IgE estimation: Sera of patients showing marked positive skin reactions were evaluated by ImmunoCAP® for specific IgE against seven food allergens and nine aeroallergens.
Statistical analysis
The statistical analysis was performed using SPSS (Statistical Package for Social Sciences) version 10.5 software. The data was analyzed for all variables using the Chi-square test.
Comparison evaluation
1. Sensitization pattern based on Serum (16 specific IgE >1 kU/ml) with Skin prick tests Positive >4 mm Wheal Size (35 aero-allergens).
2. Serum total IgE levels >250 IU/ml with Sensitizations based on Serum (16 specific IgE >1 kU/ml) with Skin prick tests Positive >4 mm Wheal Size (35 aero-allergens)
3. Absolute eosinophil count >200 cells/uL with Sensitizations based on Serum (16 specific IgE >1 kU/ml) with Skin prick tests Positive >4 mm Wheal Size (35 aero-allergens)
4. Serum cortisol level <10 mcg/dL with Sensitizations based on Serum (16 specific IgE >1 kU/ml) with Skin prick tests Positive >4 mm Wheal Size (35 aero-allergens).
Results
1. Sensitization pattern based on Serum (16 specific IgE >1 kU/ml) with Skin prick tests Positive >4 mm Wheal Size (35 aero-allergens).
75 subjects were analyzed for respiratory allergy against foods & Aero-allergens in which poly-sensitization was seen in maximum patients (n=60, 80%) (Figure 2), we further did analysis for allergen categorization in these patients.
Data observed for Monosensitized and Poly-sensitized patterns demonstrated that maximum allergic cases were of dust mites (n=10, 66.6%) & both mites and cockroach (n=57, 95%) respectively (Figure 3).
The combined results for both tests (SPT>4 mm and sIgE >1 kU/ml) demonstrated a significantly higher sensitivity. Data below showed a high level of agreement between SPT and sIgE Figures 4-8.
Below Graphs summarizes correlation of sensitization based on specific IgE and SPT
Total IgE estimation distribution
Total serum IgE estimation was carried out from the available data, cut off range was taken as > 250.0 IU/mL
Following distribution was derived from this data Figures 9-11.
Discussion of data analysis
Immune response for sIgE is different in skin & blood for allergen sensitization. Skin Allergen testing has a higher specificity & sensitivity than sIgE (with a cut off of 0.35 kU/ml) regardless of the type of allergic diseases. Food sensitization in Respiratory Disorders by SPT or sIgE must be interpreted with caution because of the presence of cross reactivity of food allergens with pollens, fungi, & dust mites etc. Some studies have compared the cut-off level of both sIgE & SPT sensitization to aeroallergens or food allergens in respiratory allergy. In one study of “PASTURE” (protection against allergy study in rural environment), cohort has suggested that there is a disagreement between SPT & sIgE in the first six years of life. In another study 12.1 % of patients would have been misdiagnosed, if only sIgE had been performed, while 45.2 % would have been misdiagnosed if only SPT had been performed. It is still controversial to comment as to which of these tests (SPT & sIgE) is better than the other? Will both the tests in combination (SPT & sIgE) improve sensitivity & specificity? [17-19].
SPT wheal size threshold of > 3 mm cut off criteria has better clinical accuracy which is based on reproducibility in relation to nasal provocation test rather than clinical relevance in considering several co-factors such as skill of the tester, the testing device, color of the skin, the skin reactivity potency & stability of allergen extracts reagents. But the level of accuracy of spIgE cut off value for various groups of allergens has not been well defined in guidelines. Sampson H, et al. [20] have given variable cut off values of sp IgE serum level for different food allergens that can predict clinical reactivity in (90-95) % of group studies. In our study we have considered >4 mm SPT and spIgE > 1 kU/ml criteria as reasonably accurate in identifying sensitization in physician based diagnosis of respiratory allergy which differs from the International threshold cut off criteria of SPT >3 mm based on nasal provocation test [4,21].
In the current study of 75 subjects of respiratory allergy both SPT & sIgE were carried out to detect the level of agreement (Concordance Vs. Discordance), and their relevance with Total IgE, AEC and S. Cortisol.
Sensitization was considered immunologically significant, if SPT showed >4mm wheal size & sIgE was >1 kU/ml and a higher percentage of sensitivity and PPV was observed (Average Percentage: Sensitivity – 89.3%, PPV – 69.28%) on combining both the tests.
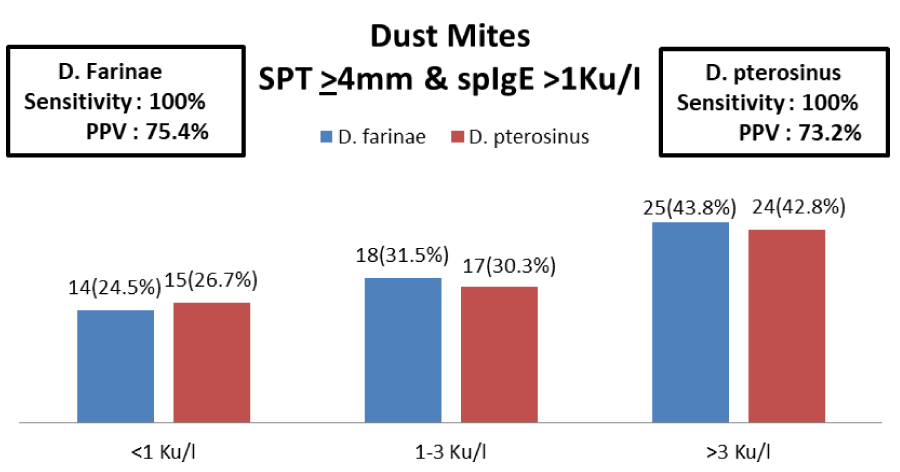
House Dust Mite (D. pteronyssinus, D. farinae) (n=67, 89.33%) was observed to have high sensitivity 100% & Positive predictive value (PPV) 74.3% which displayed a high level of agreement between SPT & sIgE.
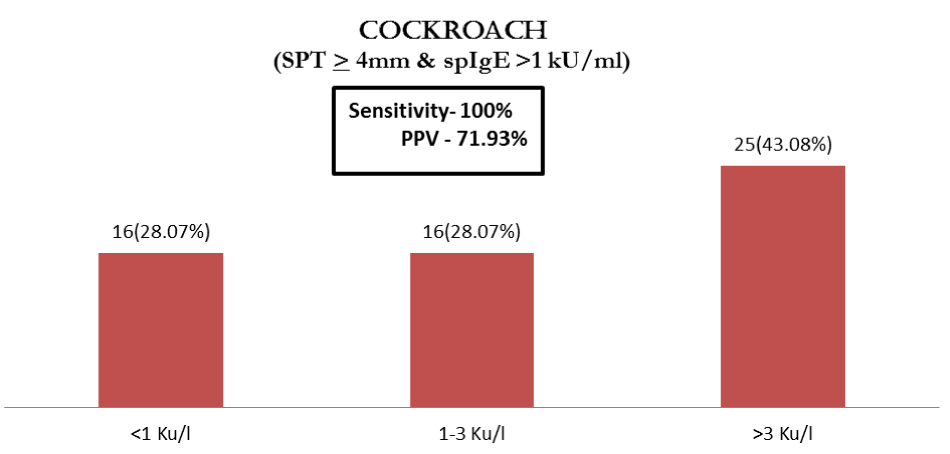
Cockroach (n=57, 76%) also showed a high level of agreement between SPT & sIgE with sensitivity up to 100% & PPV up to 71.93%
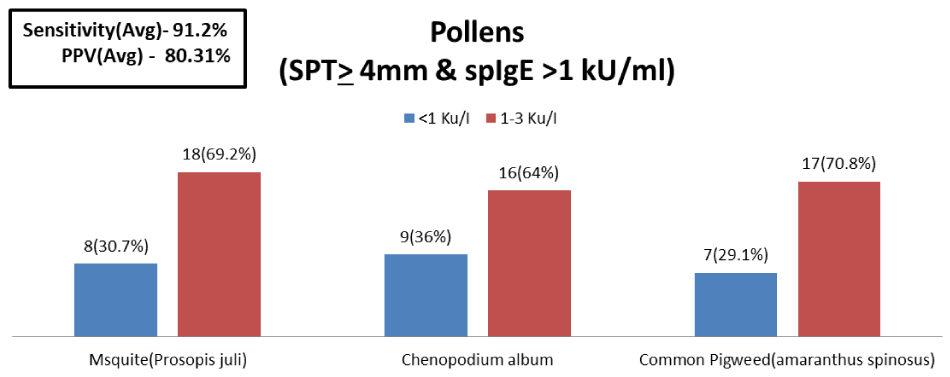
Pollens (n=56, 74.6%), showed a high level of agreement between SPT & sIgE with sensitivity as high as 91.2% & PPV as 80.31%.
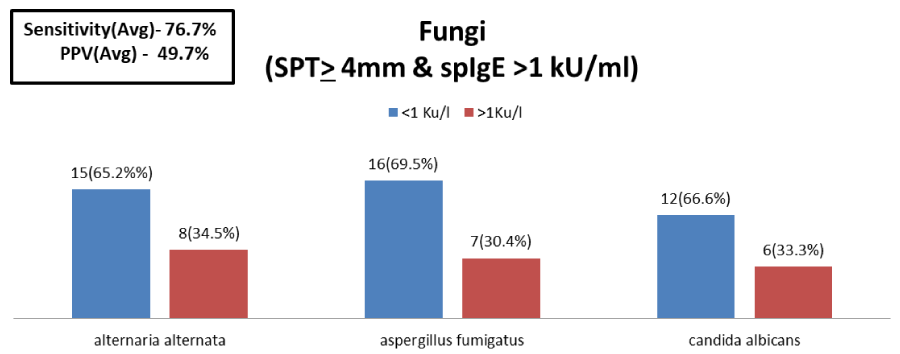
Fungi (n=21, 28%), showed low level of agreement between SPT & sIgE low level of sensitivity 76.7% & low level of PPV 49.7%, with a high NPV Negative Predictive Value 55.71%.
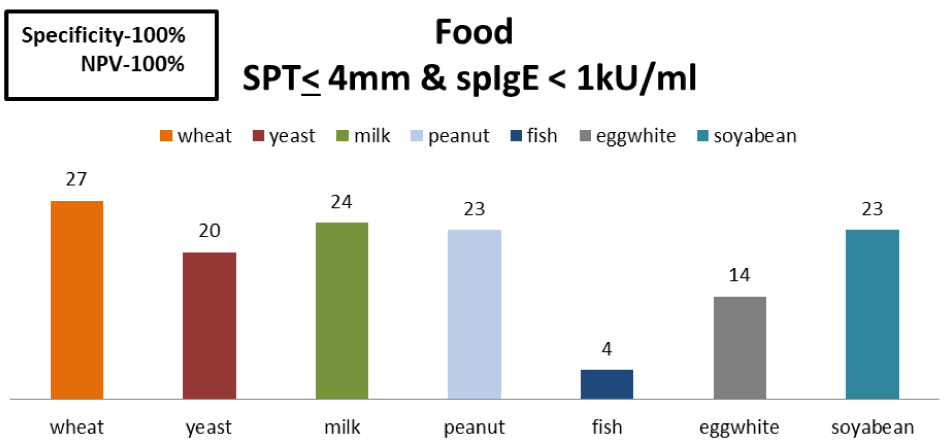
In case of food allergens there was no agreement between SPT & sIgE with high specificity of 100% & Negative predictive value (NPV) of 100% for detection of respiratory allergy.
In our study both SPT >4 mm sIgE >1 kU/ml have high level of agreement between House Dust Mite, Cockroach & Pollens, but low level of agreement between fungi & food allergens. Our results verify that cut off value of wheal size of >3 mm & sp IgE > 0.35 kU/ml cannot explain the clinical sensitivity of patients from respiratory allergy.
Discussion on data analysis- Relevance to total IgE, AEC & S. cortisol
In our current study of 75 subjects (n=60, 80%) were poly-sensitized, among which (n=67, 89.33%) (Figure 4) were found to be significant positive with House Dust Mites (D. farinae, D. pteronyssinus), Cockroach (n=57, 76%) (Figure 7) & Pollens (n=56, 74.6%) (Figure 6). This explains the increase in exposure to the different aero allergens suggestive of severity of the disease.
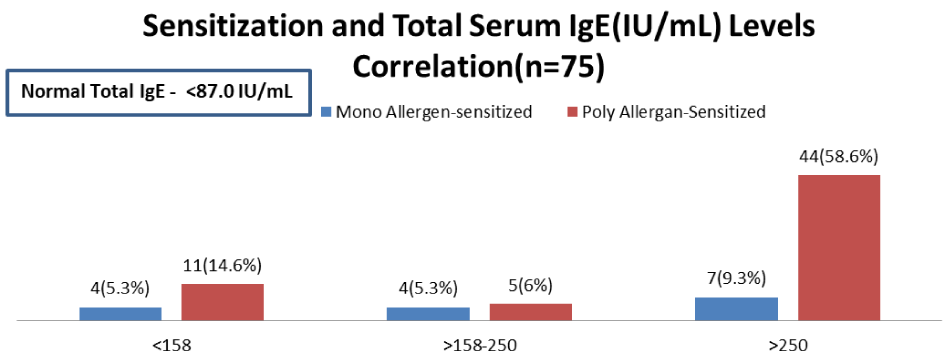
High titer >250 IU/ml of Total IgE was found in 58.6% of subjects (Figure 9). This verifies strong association between elevated S. Total IgE & Respiratory allergy (allergic rhinitis & Asthma) in Indian patients. Similar observation was found in various studies.
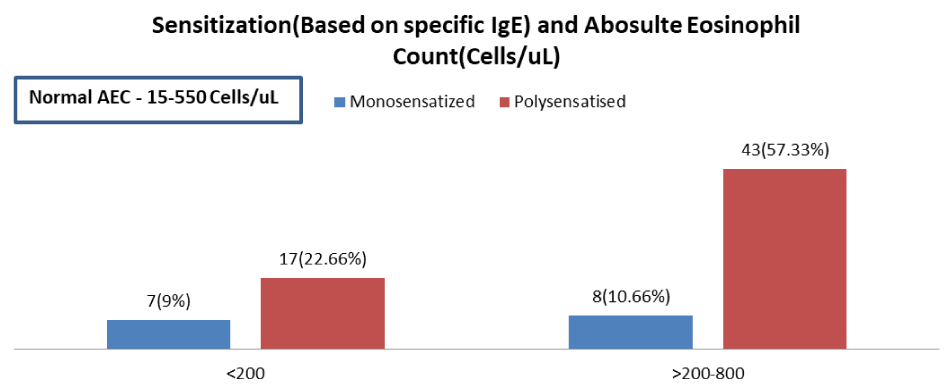
Increased Absolute Eosinophil count >200 cells /ul was found in 57.33% (Figure 11) among poly-sensitized subjects, which supports the prominent role of Eosinophils & maintenance of ILC2 (Innate Lymphocyte Cell Type-2) and Th2 mediated cytokines (IL-5 & IL-13).
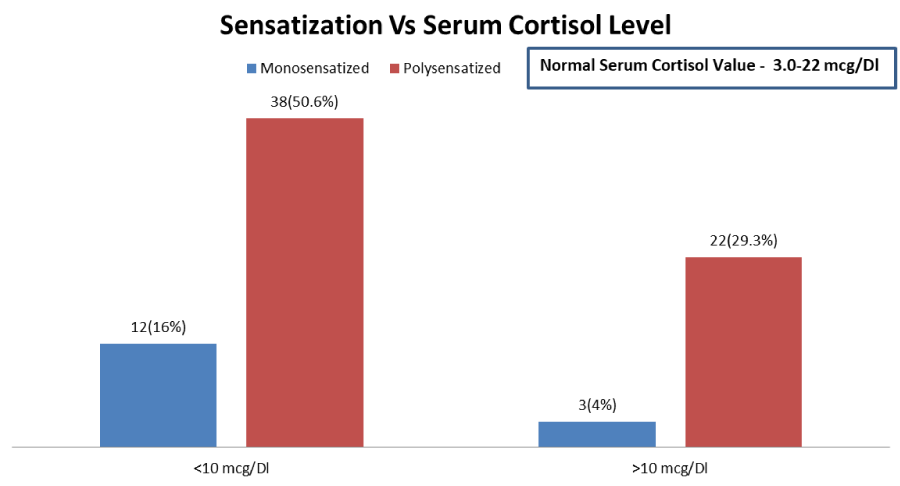
Low level of S. Cortisol < 10 mcg/dL (N=22, 29.3%) (Figure 10) was found. Which may be due to the complex interaction of neuro endocrine & immune system or due to exogenous irregular intake of oral corticosteroids [21]. To the best of our knowledge there is no published data attributable to find the significance of lower cortisol level in polysensitized respiratory allergic patients.
Conclusion
Our study has several strengths and limitations that are worth acknowledging. One strength is that our study was based upon data collected from a nationally representative population with a wide range of age. This allowed us to directly compare sensitization rates in subjects of different ages suffering from respiratory allergies (allergic rhinitis bronchial asthma). Secondly, sensitization of subjects was confirmed by a standardized measurement of allergen-specific IgE and skin prick test (cutoff for sensitization considered as SPT > 4mm wheal Size & specific IgE >1 Ku/ml). Thirdly, we limited our subjects to those with a history of physician diagnosed respiratory allergic diseases and with active symptoms, and excluded patients with possible non allergic diseases.
Based on the current study and the data analysis following conclusions can be drawn
a. Skin prick test and Specific IgE concordance (cutoff for sensitization considered as SPT > 4mm wheal Size & specific IgE >1 kU/ml) were found to be immunologically significant. Both tests are equally acceptable with higher sensitivity levels 100% and higher percentage of Positive Predictive Values (PPV) 74.6 %. There was high agreement between both the tests in cases of mites, pollen & cockroach and low levels of agreement in case of fungi & food allergens. Poly sensitization based on specific IgE and SPT (figure 4) had maximum cases of dust mite (n=67, 89.33%), fungi (n=21, 28%), pollen (n=56, 74.6%), Cockroach (n=57, 76%).
b. Poly-sensitization has strong association with high levels of total IgE>250 IU/ml (n=44, 58.6%) (Figure 9), AEC level cut off >200 cell/uL (n=43; 57.33%) (Figure 11) and also low level of S. cortisol 10pg/ml (n=38; 50.6%) (Figure 10) suggestive of ongoing inflammation and remodeling with HPA Suppression.
c. When these biomarkers (Total IgE, S. cortisol, AEC) were taken for differentiating Mono allergen-sensitized from Poly allergen-sensitized, low PPV %(95%CI) were observed: 38.2 (21.9-54.6), 28.2 (14.1-42.3), 28.6 (14.9-42.2) for Total IgE, S. cortisol, and AEC respectively and percentage for correctly differentiating Mono allergen-sensitized from Poly allergen-sensitized were found to be 17.3, 14.7 and 16.0 for these biomarkers respectively.
We would like to thank Mr. Kamal Upadhyay for collating the data for the study and Mr. Sushant Tyagi for supporting in data management and analysis for the study.
- Prashad R, Kumar R (2013) Allergy Situation in India: What is Being Done? Indian J Chest Dis Allied Sci 55: 7-8. Link: https://bit.ly/2VUSHR0
- Anonymou (1998) Worldwide variation in prevalence of symptoms of asthma, allergic rhinoconjunctivitis and atopic eczema: ISAAC. Lancet 351: 1225-1232. Link: https://bit.ly/3iKZ1U2
- Yanagida N, Sato S, Takahashi K, Nagakura KI, Ogura K, et al. (2018) Skin prick test is more useful than specific IgE for diagnosis of buckwheat allergy: A retrospective cross-sectional study. Allergol Int 67: 67-71. Link: https://bit.ly/3yS9Qcr
- Nevis IF, Binkley K, Kabali C (2016) Diagnostic accuracy of skin-prick testing for allergic rhinitis: a systematic review and meta-analysis. Allergy Asthma Clin Immunol 12: 20. Link: https://bit.ly/3sjh8nb
- Choi IS, Koh YI, Koh JS, Lee MG (2005) Sensitivity of the skin prick test and the specificity of the serum specific IgE test for airway responsiveness to house dust mites in asthma. J Asthma 42: 197-202. Link: https://bit.ly/3k3MquK
- Erwin EA, Rönmark E, Wickens K, Perzanowski MS, Barry D, et al. (2007) Contribution of dust mite and cat specific IgE to total IgE: relevance to asthma prevalence. J Allergy Clin Immunol 119: 359-365. Link: https://bit.ly/3CNPQKt
- Martinez TB, Garcia-Ara C, Diaz-Pena JM, Munoz FM, Sanchez GG, et al. (2001) Validity of specific IgE antibodies in children with egg allergy. Clin Exp Allergy 31: 1464-1469. Link: https://bit.ly/2VXcy1E
- Sharma S, Kathuria PC, Gupta CK, Nordling K, Ghosh B, et al. (2006) Total serum immunoglobulin E Level in a case- control study in asthmatic/allergic patients , their family members, and healthy subjects from india. Clin Exp Allergy 36: 1019-1027. Link: https://bit.ly/3AIRQSq
- Tehranchinia Z, Rahimi H, Lotfi S (2017) Basal serum cortisol and adrenocorticotropic hormone levels in patients with atopic dermatitis. Dermatol Pract Concept 7: 25-29. Link: https://bit.ly/3siNbUn
- Ramirez GA, Yacoub MR, Ripa M, Mannina D, Cariddi A, et al. (2018) Eosinophils from Physiology to Disease: A Comprehensive Review. Biomed Res Int 2018: 9095275. Link: https://bit.ly/2W0rqgj
- Taylor KJ, Luksza AR (1987) Peripheral blood eosinophil counts and bronchial responsiveness. Thorax 42: 452-456. Link: https://bit.ly/3iNkQlO
- Humbert M, Menz G, Ying S, Corrigan CJ, Robinson DS, et al. (1999) The immunopathology of extrinsic (atopy) and intrinsic (non-atopic) asthma: more similarities than difference. Immunol Today 20: 528-533. Link: https://bit.ly/3iQoOKI
- Kuntz KM, Kitch BT, Fuhlbrigge AL, Paltiel AD, Weiss ST (2002) A novel approach to defining the relationship between lung function and symptom status in asthma. J Clin Epidemiol 55: 11-18. Link: https://bit.ly/2W1ksra
- Kerkhof M, Dubois AE, Postma DS, Schouten JP, de Mon-chy JG (2003) Role and interpretation of total serum IgE measurements in the diagnosis of allergic airway disease in adults. Allergy 58: 905-911. Link: https://bit.ly/3AISkbc
- Klinke M, Cline MG, Halonen M, Burrows B (1990) Problems in defining normal limits for serum IgE. J Allergy Clin Immunol 80: 440-444. Link: https://bit.ly/3sm6coT
- Annesi I, Oryszozyn MP, Frette C, Neukirch F, Orvoen-Frija E, et al. (1992) Total circulating IgE and FEV1 in adult men; an epidemiologic longitudinal study. Chest 101: 642-648. Link: https://bit.ly/3xPuj0i
- Chauvea A, Dalphin ML, Kaulek V, Roduit C, Pugin A, et al. (2016) Disagreement between skin prick tests and specific IgE in early childhood. Int Arch Allergy Immunol 170: 69-74. Link: https://bit.ly/3m6eQa3
- Pastorello EA, Incorvaia C, Ortolani C, Bonini S, Canonica GW, et al. (1995) Studies on the relationship between the level of specific IgE antibodies and the clinical expression of allergy. I. Definition of levels distinguishing patients with symptomatic from patients with as-symptomatic allergy to common aeroallergens. J Allergy Clin Immunol 96: 580-587. Link: https://bit.ly/3iQpe3K
- Patil SP, Niphadkar PV, Bapat MM (2001) Chickpea a major food allergen in the Indian subcontinent and its clinical and im-munochemical correlation. Ann Allergy Asthma Immunol 87: 140-145. Link: https://bit.ly/3CTEAfs
- Sampson HA, Ho DG (1997) Relationship between food specific IgE concentrations and the risk of positive food challenges in children and adolescents. J Allergy Clin Immunol 100: 444-451. Link: https://bit.ly/3mbTCYp
- Thomas AE, Schuyler AJ, Erwin EA, Commins SP, Woodfolk JA (2016) Platts-Mills; Aetal IgE in the diagnosis and treatment of allergic disease. J Allergy Clin Immunol 137: 1662-1670. Link: https://bit.ly/3yLUp5A
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.
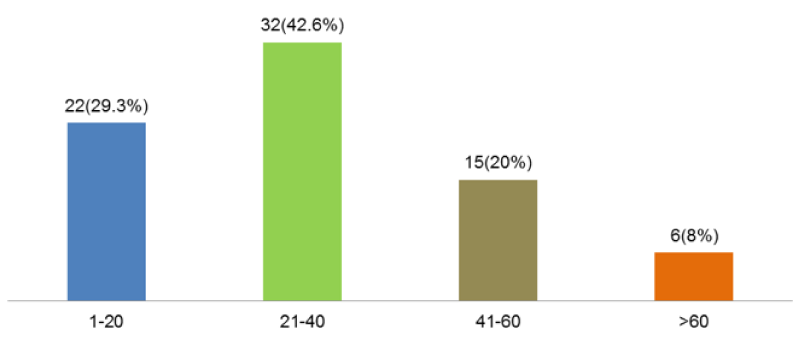



 Save to Mendeley
Save to Mendeley
