Archive of Urological Research
The OEIS complex – clinical & radiological evaluation
HK Dutta1*, Dhaval D Dhingani2, RK Gogoi3 and Deb K Boruah4
2Post Graduate student, Department of Radiodiagnosis, Assam Medical College and Hospital, Dibrugarh, Assam, India
3Professor, Department of Radiodiagnosis, Assam Medical College and Hospital, Dibrugarh, Assam, India
4Associate Professor, Department of Radio-diagnosis, Assam Medical College and Hospital, Dibrugarh, Assam, India
Cite this as
Dutta HK, Dhingani DD, Gogoi RK, Boruah DK (2021) The OEIS complex – clinical & radiological evaluation. Arch Urol Res 5(2): 035-037. DOI: 10.17352/aur.000036Copyright
© 2021 Dutta HK, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.The OEIS complex comprises a constellation of complex and severe malformations of the abdominal wall, gastrointestinal and genitourinary tracts, and spinal cord. The malformation results from improper closure of the ventral abdominal wall due to failure of convergence of cephalo-caudal and lateral folding of the embryo during early gestation. The rarity of the condition suggests etiologic heterogeneity and the possible role of environmental and genetic factors. We present clinical and imaging findings of the OEIS complex in a neonate.
Introduction
OEIS complex includes a spectrum of complex and severe malformations involving multiple organ systems. The anomaly comprises omphalocele, cloacal exstrophy, imperforate anus, and spinal abnormalities. Cloacal exstrophy is the most severe form of the exstrophy-epispadias complex. The first description of the anomaly was published by Littre in 1709 and Carey et al first coined the term OEIS complex [1,2]. Reported incidence of OEIS varies from 1 in 2,00,000 to 4,00,000 pregnancies [3-5]. The rarity of the condition suggests etiologic heterogeneity and the possible role of environmental and genetic factors [6].
Case report
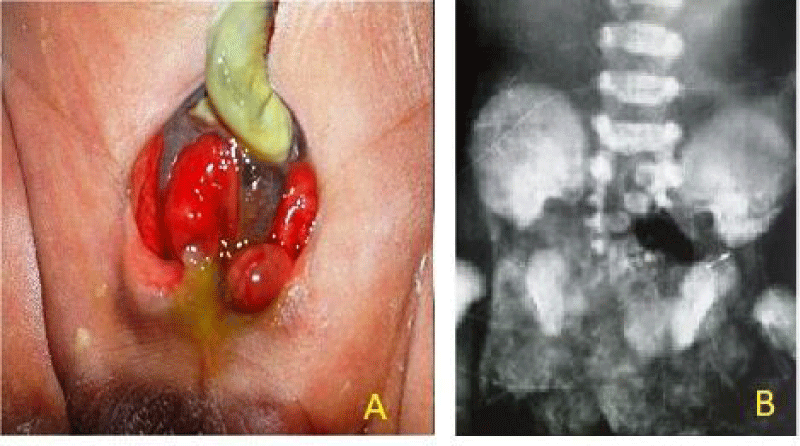
A 34 weeker, low birth weight baby born by normal vaginal delivery to a second gravida mother presented on day 2 with lower abdominal wall defect with exposed urinary bladder, through which bowel loops were protruding out and imperforate anus [Figure 1A]. A small exomphalos with a central cord was present just above the abdominal defect. The baby had a bifid penis and well developed scrotum with a descended and one undescended testis. An anal opening was absent and the patient was passing stool through the protruding bowel loop. There was a skin covered raised area with the consistency of fat noted in the midline over the lumbosacral region. The lower limbs below the knees showed minimal movement and without any reflexes. No abnormalities were noted in the upper abdomen, chest, upper limbs, and head. The baby was on breast feed.
Radiological findings
X-ray AP view of pelvis and lumbosacral spine revealed a wide pubic diastasis and defects involving a body of multiple sacral vertebrae (Figure 1B).
USG of Lumbo-sacral region showed:
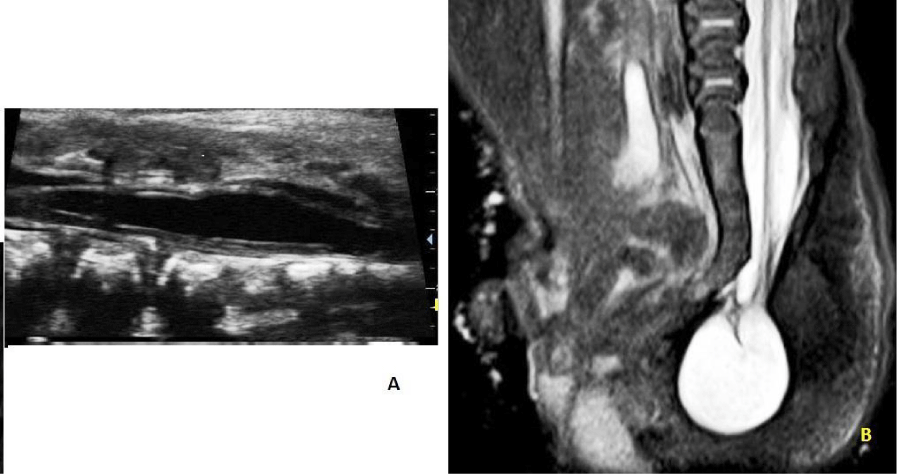
- Hypoechoic cystic lesion containing echogenic nerve roots within and tethered cord in sacro-coccygeal region with intact overlying skin and subcutaneous tissue (Figure 2A).
- Proximal syrinx formation in the region of the lower lumbar and sacral spinal canal was also noted.
MRI of Lumbo-sacral spine confirmed the above findings suggesting a closed spinal dysraphism -- terminal myelocystocele with tethered cord at sacro-coccygeal junction and syrinx formation (Figure 2B).
Discussion
Although the first description of a case of OEIS complex was reported in 1709, it was only in 1978 that Carey et al first used the term OEIS complex [1,2]. The anomaly is thought to be due to a defect in early blastogenesis or of mesodermal migration during the primitive streak period [7,8]. These defects lead to improper closure of ventral abdominal wall due to failure of convergence of four ecto-mesodermal folds (a cranial, a caudal, and two lateral) of an embryo with associated defects in the development of cloaca and urorectal septum during 4th gestational week. The cloacal membrane is composed of ectodermal and endodermal layers and it covers the region from the umbilicus to the tail portion of the embryo at the 4-mm stage. In subsequent stages, the primitive streak mesoderm invades the membrane to form the lower abdominal wall. Lack of mesoderm in the infra-umbilical abdominal wall results in omphalocele. During the 8- to the 16-mm stage, the urorectal septum meets the cloacal membrane and divides the cloacal chamber into an anterior urogenital and posterior alimentary systems. Cloacal exstrophy results when the membrane ruptures before the formation of the urogenital septum. The coexistence of cloacal exstrophy and spinal dysraphism may be explained by a single insult in the embryonic tail in early pregnancy [6]. Caudal dysgenesis interferes with somite formation resulting in defective vertebrae [9].
Because of its rarity and sporadic occurrences, some environmental and genetic factors may be responsible for its causation [6]. One study reported maternal exposure to diphenyl hydantoin and valproic acid and cigarette smoking as possible risk factors [2,6,9]. Higher incidence of OEIS in monozygotic twins than in dizygotic twins suggesting a possible genetic contribution to the occurrence of these defects was reported [10].
The OEIS complex involves multiple body systems. The classical presentation consists of omphalocele superiorly with an open plate mucosa inferiorly consisting of two posterior walls of hemibladder on either side with a central strip of ithe ntestinal mucosa [11]. Similar findings were noted in our case with the passage of meconium and stool from the protruding bowel loop in the upper part of the central bowel strip. Ambiguous genitalia is common with bilateral cryptochidism in males. In the present case, one testis was found in the hemiscrotum, but the other remained high in the inguinal canal. Renal anomalies such as agenesis, rudimentary kidney, ectopic kidney pelviureteric junction obstruction etc have been reported [12]. The congenital vertebral malformations associated with cloacal exstrophy vary from congenital scoliosis, kyphosis, abnormal lumbosacral segmentation, sacral agenesis, interpedicular lumbar widening to hemivertebra, spina bifida occulta, and myelomeningocele [13,14]. In the present case, there was terminal myelocystocele with tethered cord and syrinx formation. The baby had a partial neurological deficit in both lower limbs below the level of the knee. Talipes in association with OEIS complex is related to a tethered cord. Central nervous system anomalies are not commonly encountered in OEIS complex.
OEIS complex is difficult to diagnose prenatally and all the abnormalities in the fetus may not be clear until a thorough postnatal evaluation [15]. The major criteria for the prenatal diagnosis include non visualization of fetal bladder, infraumbilical anterior abdominal wall defect, omphalocele and myelomeningocele [15,16]. The minor criteria include lower extremity abnormalities (talipes), renal anomalies, ascites, widened pubic arches, narrow thorax, kypho-scoliosis, hydrocephalus and single umbilical artery. Presence of omphalocele and spinal defects on prenatal ultrasonography strongly suggest OEIS complex.
Overall prognosis of babies born with OEIS complex depends on severity of the anomalies and presence of infection. With surgical intervention and improved medical therapy, the survival of these patients has been greatly improved. Infants who are medically stable may be considered for surgical reconstruction with closure of omphalocele, separation of ileocecal connection from the exstrophied bladder plate, and reapproximation of an end colostomy with preservation of all bowels [14]. Approximation of the pubis usually with osteotomy is beneficial in reconstruction of the pelvic ring and bladder closure [16]. Bowel and urinary incontinence may persist even after good reconstruction because of neurological abnormalities. Spinal cord untethering may be required years after closure of the spinal defect [14,17]. Early evaluation with magnetic resonance imaging will allow rapid treatment and prevention of further loss of function. Male patients may have infertility or subfertility issues and erectile dysfunction.
Conclusion
Babies born with OEIS complex require the care of a multidisciplinary team of neonatologists, pediatric surgeons, and pediatric urologists. These patients need multiple surgeries, with many potential complications. There is no definite etiological factor responsible for this anomaly. Prenatal diagnosis is possible based on specific ultrasonologic criterias.
- Spencer R (1965) Exstrophia splanchnica (exstrophy of the cloaca). Pediatr Surg 57: 751-766. Link: https://bit.ly/3E5GfyP
- Carey JC, Greenbaum B, Hall BD (1978) The OEIS complex (omphalocele, exstrophy, imperforate anus, spinal defects). Birth Defects Orig Art Ser 14: 253-263. Link: https://bit.ly/3p2Iwog
- Hurwitz RS, Manzoni GAM, Ransley PG, Stephens FD (1987) Cloacal exstrophy: a case report of 34 cases. J Urol 138: 1060-1064. Link: https://bit.ly/3xxZrTu
- Kallen K, Castilla EE, Robert E, Mastroiacovo P, Kallen B (2000) OEIS complex—a population study. Am J Med Genet 92: 62-68. Link: https://bit.ly/3o2oACM
- Carey JC (2001) Exstrophy of the cloaca and the OEIS complex: one and the same. (Letter) Am J Med Genet 99: 270. Link: https://bit.ly/3ldR22A
- Keppler-Noreuil KM (2001) OEIS complex (omphalocele-exstrophy-imperforate anus-spinal defects): a review of 14 cases. Am J Med Genet 99: 271-279. Link: https://bit.ly/3xyIJmP
- Opitz JM (1993) Blastogenesis and the primary field in human development. BDOAS 29: 3-37. Link: https://bit.ly/3cZVSvO
- Pauli RM (1994) Lower mesodermal defects: a common cause of fetal and early neonatal death. Am J Med Genet 50: 154-172. Link: https://bit.ly/3lhrxh1
- Cohen AR (1991) The mermaid malformation: cloacal exstrophy and occult spinal dysraphism. Neurosurgery 28: 834-843. Link: https://bit.ly/3FXPAcu
- Lee DH, Cottrell JR, Sanders RC, Meyers CM, Wulfsberg EA, et al. (1999) OEIS complex (omphalocele-exstrophy imperforate anus-spinal defects) in monozygotic twins. Am J Med Genet 84: 29-33. Link: https://bit.ly/3FSZ4pu
- Bhosale Y, Rajagopal L, Nandanwar YS (2007) Omphalocele, Exstrophy of cloaca,Imperforate anus and spinal defects(OEIS Complex): A case report and review of literature. J Ana Soc 56: 41-43. Link: https://bit.ly/3FVDNvl
- Mathew R, Jeffs R, Reiner W, Docimo S, Gearhart J (1998) Cloacal exstrophy—improving the quality of life: the Johns Hopkins experience. J Urol 160: 2452–2456. Link: https://bit.ly/31756DR
- Loder RT, Dayioglu MM (1990) Association of congenital vertebral malformations with bladder and cloacal exstrophy. J Pediatric Orthop 10: 389-393. Link: https://bit.ly/3xyDgwu
- Schober JM, Carmichael PA, Hines M, Ransley PG (2002) The ultimate challenge of cloacal exstrophy. J Urol 167: 300-304. Link: https://bit.ly/31dJUMN
- Gosden C, Brock DJH (1981) Prenatal diagnosis of exstrophy of the cloaca. Am J Med Genet 8: 95-109. Link: https://bit.ly/3p6zqac
- Vasudevan PC, Cohen MC, Whitby EH, Anumba DOC, Quarrell OW (2006) The OEIS complex: Two case reports that illustrate the spectrum of abnormalities and a review of the literature. J Prenat Diagn 26: 267–272. Link: https://bit.ly/3d1cWBA
- Ben-Chaim J, Peppas DS, Sponsellar PD, Jeffs RD, Gearhart JP (1995) Applications of osteotomy in cloacal exstrophy patient. J Urol 154: 865-867. Link: https://bit.ly/3E5jafR
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
