Archive of Urological Research
GIANT vesical stone on an intra-uterine dispositive prolapse in vagina complicated with a vesical fistula: Case report and review of literature
Avakoudjo Josue Dejinnin Georges1, Agounkpe Michel Michael1, Byabene Kaduku Gloire À Dieu2,3*, Yunga Foma Jean De Dieu4, Natchagande Gilles1, Loko David1, Hodonou Fred Detondji Martin1, Muhindo Valimungighe Moise2, Yevi Ines Dodji Magloire1, Sossa Jean1 and Mukwege Mukengere Denis5
2Department of General Surgery, Université Evangélique en Afrique, Panzi Hospital, Bukavu, D.R. Congo
3Department of General and Digestive Surgery, CNHU/Hubert Koutoukou Maga, Cotonou, Bénin
4Department of Gynecology, Institut Supérieur des Techniques Médicales, Uvira, D.R.Congo
5Gynecology department of Université Evangélique en Afrique, Panzi Hospital, D.R. Congo
Cite this as
Dejinnin Georges AJ, Michael AM, Gloire À Dieu BK, Jean De Dieu YF, Gilles N, et al. (2021) GIANT vesical stone on an intra-uterine dispositive prolapse in vagina complicated with a vesical fistula: Case report and review of literature. Arch Urol Res 5(2): 028-032. DOI: 10.17352/aur.000034Intrauterine device is the commonest method of reversible contraception worldwide. It’s trans vesical migration or misplacement is a very rare complication with a high ratio of calculi formation. We present a case of a 39-year old patient with a large vesical stone prolapse in vagina lumen measuring 15.36 cm × 8.87 cm weighing 450 grams on a intra uterine copper contraceptive dispositive complicated with a large vesical fistula. The a lithotomy was performed via the low approach. The management of the fistula was done 3 months later.
Giant bladder stone on an intra uterine contraceptive device is a very rare clinical entity. monitoring of intrauterine contraceptive devices is necessary.
Introduction
Intrauterine Contraceptive Device (IUCD) is the commonest method of reversible contraception worldwide. It is used by approximately 14% of women due to its efficacy, safety, and low cost. [1] IUCD is not free from complications; in fact, complication such as IUCD migration is one the gynecologist’s challenges [2]. IUCD migration is commonly into the abdominal cavity; however, migration into the adnexa, iliac vein, and broad ligament has been reported. Intravesical migration is a rare complication of IUCD [3].
However, trans vesical migration or misplacement of an IUD is a very rare complication with a high ratio of calculi formation [4,5].
Giant vesical stone (more than 100 g) is a very rare clinical entity [6].
We present a giant stone formed on a migrated IUD in the bladder prolapse in the vagina lumen complicated by a large vesico-vaginal fistula in a 39-year-old multiparous.
Case presentation
A woman 39-year-old patient 3 gravida, with a history of last delivery by caesarean surgery 20 years of for big baby. No menstruation since 15 years. A intra uterine dispositive for contraception after 20 years presented to consultation in a humanitarian mission with pelvic pain, feeling of pelvic mass, heaviness urinary leakage. This symptoms appears progressively since approximatively six months after caesarean procedure. The patient reported the feeling of a solid mass in her vagina 5 years after the caesarean which gradually take the volume.
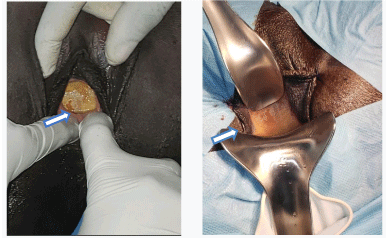
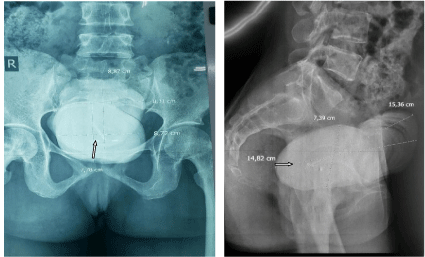
On physical examination we noticed urine listener, there were an oval pelvic mobile mass palped a mass that measures 15cm from the pubic bone. There was urine leakage with perineal itch. At the speculum examination they were a stone brownish in color, 4 cm from the vulva prolapse vaginal, with hard consistency. There was urinary loss at it’s mobilization. The cervix was not seen because of the vaginal’s obstruction (Figures 1,2). A standard X-ray made it possible to note a 15.36cm x 8.87cm macrolithiasis (Figures 3,4). The diagnosis of a large trigono-retrotrigonal vesicovaginal fistula and bladder microlithiasis was made.
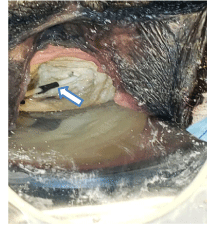
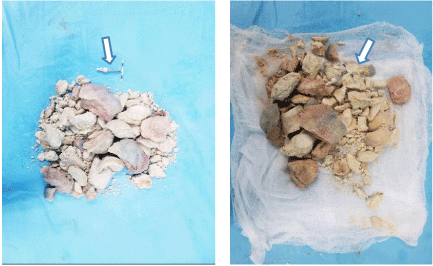
On spinal anesthesia, in a gynecological position a vaginal exploration reveals a bulky bladder lithiasis of brownish color of hard, friable consistency, protruding into the vagina with urinary discharge into the vagina. Partial lithotripsy was performed using the lithoclast, a chisel and a hammer. Gradual extraction of lithiasis fragments weighing 245g. It was found an intrauterine device incarcerated in the lithiasis(Figures 5-7). Copious bladder and vaginal lavage was done. An examination under valve after placement of a urethro-vaginal probe allows to find induration of the vaginal walls, postoperative vaginal dermabrasions and the presence of a trigono-retrotrigonal vesicovaginal fistula of about 08cm with irregular contours. The postoperative follow-up was marked by a drying up of urine leaks and dry bedding on D 7 postoperatively. The monitoring of the patient was done. A revisional surgery 3 months later through a vaginal route was performed. The postoperative fistula treatment outcomes was simple.
Discussion
Intrauterine Contraceptive Device (IUCD) has been widely used since 1965[7,8].
It is the most popular method of reversible contraception in developing countries due to its efficiency and low cost [1,9].
There has been concomitant large number of reported complications [11], the spectrum of which varies greatly from slight discomfort at time of insertion to death [12]. Perforation of the uterus by an IUCD with migration into the bladder is very uncommon.
Intramyometrial migration begins with the incarceration of a branch of the IUCD in the myometrium the next step is inflammatory phenomena as well as uterine contractions that will make the IUCD to continue its migration [13,14].
IUCD migration into the bladder can be asymptomatic or present with clinical conditions like haematuria, UTI or hydronephrosis. The presence of bladder stone formation is unusual in women and should raise suspicion of IUCD perforation. The IUCD acts as a nidus for stone formation in the bladder [15].
Risk factors of IUCD perforation include insertion of the IUCD by inexperienced physicians, incorrect positioning of the IUCD, uterine abnormalities, multiparity, and recent abortion or pregnancy [16].
Migration of an IUCD into the bladder is a low frequency complication.
IUCD migration into the structures adjacent to uterus is a rare complication with an estimated incidence of 1/1000 insertions [2]. The literature mainly mentions some case reports and case series [3,17-19]. Goyal, et al. in India, in a study of 240 copper-bearing IUCDs inserted during a 12-month period, had reported only 2 cases of migration, including intravesical migration [19].
The mechanism of uterine perforation by IUCD may be primarily at the time of insertion [20].
It is closely related to the time and technique of insertion, the type of IUCD, the skill of the physician, and the anatomy of the cervix and uterus [12].
Currently, there are about 200 cases of uterine perforation reported (in a literature review in 1999, a total of 165 cases were collected by Kassab and Audra [21]) in the literature. In about 90 of the cases, the IUCD migration to bladder was seen with or without stone formation. The true incidence of perforation might be most likely higher because of the frequently asymptomatic nature of perforation [11].
Kassab, et al. reported 165 cases of IUCD migration. In this study, the IUCD was located at the following sites: omentum, 45; rectosigmoid, 44; peritoneum, 41; bladder, 23; appendix, 8; small bowel, 2; adnexa, 1; and iliac vein, 1.2 IUCD migration to the peritoneal cavity might cause adhesions, volvulus, fistula, and bowel perforation.
Otherwise, urogenital fistula such as vesico uterine fistula may be the main presenting feature [22].
Bladder stones as complication of IUCD migration into the bladder have also been reported causing obstructive (emptying phase) lower urinary tract symptoms, such as straining on micturition and acute retention of urine [23].
Stones can form as a result of complete migration of the IUCD. Ozcelik B, et al. reported approximately 70 cases of IUCD migration to the bladder have been reported in the scientific literature, and about half of them resulted in stone formation, with established stone sizes varying from 1 cm to 8 cm [5,24].
Stone formation is due to calcium precipitation on the device that plays the role of a matrix [25].
Though bladder stones are often found in women with urinary stasis due to outlet obstruction (pelvic organ prolapse, urethral stricture) and detrusal instability resulting in significant post-void residual urine, it is also found in healthy women [26]. Alkaline urine caused by urea splitting organisms (Proteus, Klebsiella, Serratia, and Enterobacter) is responsible for struvite stones (ammonium magnesium phosphate) [27]. Foreign bodies such as retained non-absorbable sutures, synthetic slings, or mesh used for treatment of stress incontinence or pelvic organ prolapse, and migrated intrauterine copper-T within the bladder have lithogenic potentiality. Kidney stone if dropped in bladder may remain as foreign body and attains larger size due to deposition of phosphates around it [27,28].
Therefore, the encrustation nature of the stone could be a logical justification for the easy fragmentation of such stones.
We suggest that in our case the uterine performation had occurred at the time of insertion or shortly afterwards. The deposit of calcium and the stasis would have led to the gradual increase in the volume of the stone. As the stone took on volume, it would have resulted in compression of the bladder and consequently a large vesicovaginal fistula on the eschar and after the stone would be the basis of its prolapse in the vagina and the signs of mass that the patient had to present.
The stone measured 15.36cm x 8.87cm. We did not find in the literature such a large bladder stone nor a prolapsed stone in the vaginal lumen resulting from the migration of an IUCD.
Most of perforations are diagnosed at the time of insertion (86%) and indicated by pain, bleeding or a lost thread, however some perforations remain undiagnosed for several years [28].
Pelvic ultrasound is considered the first modality of choice. However, CT is the best modality to evaluate intraabdominal complications of IUCD perforation [29].
For our patient the bladder stone was revealed by the vesicovaginal fistula. The final lesion diagnosis was made after the stone was removed, which revealed local fibrosis and soft tissue induration with large vesicovaginal fistula. A urethral vesical catheter was placed and the balloon was been palpated in the crater of the fistula.
The treatment options for IUCD bladder migration include a conservative treatment or removal via a cystoscopic extraction, a laparoscopic surgery or an open surgery [30].
Laparoscopic surgery is preferred due to its minimal invasive approach and lower morbidity. But sometimes an open surgery is necessary in cases with the formation of big bladder stones, with partial penetration of the bladder wall or in the presence of adhesions to the bladder wall. Shin, et al. described a case of a migrated IUCD with embedment into the muscular layer of the bladder. The IUCD was removed through an excision of the bladder wall around the device to prevent formation of VVF [31].
Yahsi, et al. reported a case of an embedded IUCD into the posterior bladder wall [32].
Their initial surgical removal with cystoscopic forceps was unsuccessful, because the IUCD was stuck to the bladder wall. However, in a second laparoscopic surgery the complete removal of the IUCD was achieved [33].
It can also be removed by suprapubic cystotomy such as was used in other reports .Open surgery was generally used for the removal of the big stones around IUCD. However, open surgery has definitive morbidity over the patient[34].
For our patient, we decided to make the fragmentation of the stone by vaginal route since it was visible intra vaginally on speculum examination and palpated 4 cm from the vulva and because of the dimensions of the stone for less disrepair and to be able to cure the fistula later.
For our patient the cystoscope would not have passed given the obstruction by the stone. An ablation of the stone in trans abdominal would have resulted in more lesions of the soft parts with a great risk of infection. The trans vaginal approach made it possible not to have other loco-regional lesions apart from the anterior ones.
Conclusion
Giant bladder stone itself is a very rare clinical entity. IUCD is usually a safe contraceptive method. However, IUCD perforation is a rare but serious complication, which may present with bladder migration and secondary stone formation that can take volume and become giant afterward. Migrated IUCDs should be completely exposed and removed to avoid secondary fracturing. We reported the first giant bladder stone prolapsed in vagina caused by a migration of a IUCD complicated with vesical large fistula for our known. The ablation of the stone can be made by endoscopy or laparotomy approach but also a trans vaginal approach if the stone is giant and prolapse in vagina with a vesico vaginal fistula.
Authors’ contributions
This work was carried out in collaboration between all authors.
- Khanna A, Pandey B, Vashishta K, Kalia K, Pradeepkumar B (2015) A Study of Today’s A.I. through Chatbots and Rediscovery of Machine Intelligence. International Journal Service, Science and Technology 8: 277-284. Link: https://bit.ly/3pJB1Cu
- Shawar BA, Atwell E (2007) “Chatbots: are they really useful?”. LDV Forum 22. Link: https://bit.ly/3viAfxo
- Turing AM (1950) “Computing Machinery and Intelligence”. Mind 433-460. Link: https://bit.ly/3xiBUoq
- Khanna A (2015) “Pandorabots Chatbot Hosting Platform. SARANG Bot”.
- Alice AI (2015) “Foundation. Free A.L.I.C.E. AIML Set”.
- Whitby B (2009) Author, “Artificial Intelligence”, The Rosen Publishing Group.
- Weizenbaum J (1966) ELIZA—a computer program for the study of natural language communication between man and machine. Commun ACM 9: 36-45. Link: https://bit.ly/3ggAy7H
- Brandtzaeg PB, Følstad A (2017) Why people use chatbots. In: Kompatsiaris, I., et al. (eds.) Internet Science, 377–392.
- Colby KM, Weber S, Hilf FD (1971) Artificial paranoia. Artif Intell 2: 1–25. Link: https://stanford.io/35eNUek
- Wallace RS (2009) The anatomy of A.L.I.C.E. In: Epstein, R., Roberts, G., Beber, G. (eds.) Parsing the Turing Test: Philosophical and Methodological Issues in the Quest for the Thinking Computer. 181–210.
- Marietto M, Marietto B, Varago de Aguiar R, de Oliveira Barbosa G, Botelho WT, et al. (2013) Artificial intelligence markup language: a brief tutorial. Int J Comput Sci Eng Surv 4 Link: https://bit.ly/3cAX74Y
- Molnár G, Zoltán S (2018) The role of chatbots in formal education. 2018 IEEE 16th International Symposium on Intelligent Systems and Informatics (SISY). Link: https://bit.ly/3vhQevG
- Personal Digital Assistant - Cortana Home Assistant – Microsoft. Link: https://bit.ly/2RLDxf0
- What exactly is Alexa? Where does she come from? And how does she work? . Link: https://bit.ly/3veypO3
- Google Assistant, your own personal Google. Link: https://bit.ly/3iBjsDd
- IBM Watson. Link: https://ibm.co/3pODOKW
- Scopus - Document search. Link: https://bit.ly/3iCqFTl
- Colace F, De Santo M, Lombardi M, Pascale F, Pietrosanto A, et al. (2018) Chatbot for e-learning: a case of study. Int J Mech Eng Robot Res 7: 528–533. Link: https://bit.ly/2TlzHKa
- Ranoliya BR, Raghuwanshi N, Singh S (2017) Chatbot for university related FAQs. In: 2017 International Conference on Advances in Computing, Communications and Informatics (ICACCI). Udupi 1525–1530. Link: https://bit.ly/3zoRDUv
- da Costa PCF (2018) Conversing with personal digital assistants: on gender and artificial intelligence. J Sci Technol Arts 10: 59-72. Link: https://bit.ly/3gepurF
- Xu A, Liu Z, Guo Y, Sinha V, Akkiraju R (2017) A new chatbot for customer service on social media. In: Proceedings of the 2017 CHI Conference on Human Factors in Computing Systems. 3506-3510. Link: https://bit.ly/2SsUOtQ
- Følstad A, Nordheim CB, Bjørkli CA (2018) What makes users trust a chatbot for customer service? An exploratory interview study. In: Bodrunova, S.S. (ed.) INSCI 2018. LNCS, 11193: 194–208. Link: https://bit.ly/3cBCBkD
- Go E, Sundar SS (2019) Humanizing chatbots: the effects of visual, identity and conversational cues on humanness perceptions. Comput Hum Behav 97: 304-316. Link: https://bit.ly/35r0uaN
- Sannon S, Stoll B, DiFranzo D, Jung M, Bazarova NN, et al. (2018) How personification and interactivity influence stress-related disclosures to conversational agents. In: Companion of the 2018 ACM Conference on Computer Supported Cooperative Work and Social Computing 285–288. Link: https://bit.ly/3viBxbI
- Fernandes A (2017) NLP, NLU, NLG and how Chatbots work. Link: https://bit.ly/3vc3B0p
- Dale R (2016) The return of the chatbots. Nat Lang Eng 22: 811–817. Link: https://bit.ly/3gcJUl0
- Ramesh K, Ravishankaran S, Joshi A, Chandrasekaran K (2017) A survey of design techniques for conversational agents. In: Kaushik, S., Gupta, D., Kharb, L., Chahal, D. (eds.) ICICCT 2017. CCIS. 750: 336-350. Link: https://bit.ly/3znATNC
- Akma N, Hafiz M, Zainal A, Fairuz M, Adnan Z (2018) Review of chatbots design techniques. Int J Comput Appl 181: 7-10. Link: https://bit.ly/3zjrkPz
- Thomas N (2016) An e-business chatbot using AIML and LSA. Link: https://bit.ly/3guc7T7
- Artificial Intelligence Scripting Language - RiveScript.com. Link: https://www.rivescript.com/
- Jung S (2019) Semantic vector learning for natural language understanding. Comput Speech Lang 56: 130-145. Link: https://bit.ly/3xgDmrf
- Canonico M, Russis LD (2018) A comparison and critique of natural language understanding tools. Link: https://bit.ly/3vhwQPt
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
