Archive of Urological Research
Para-stomal variceal bleed, 9 years post-radical cystectomy: An Unusual emergency at a usually missed location
Suvraraj Das1, Gaurav Aggarwal2* and Sujoy Gupta3
2MS, DNB, Consultant, Department of Uro-Oncology, Tata Medical Center, Newtown, Kolkata, West Bengal, India
3MS, FRCS, Sr. Consultant, Uro-Oncology, Tata Medical Center, Newtown, Kolkata, West Bengal, India
Cite this as
Das S, Aggarwal G, Gupta S (2020) Para-stomal variceal bleed, 9 years post-radical cystectomy: An Unusual emergency at a usually missed location. Arch Urol Res 4(1): 090-092. DOI: 10.17352/aur.000027Parastomal or stomal varices are infrequently encountered with majority occurring secondary to portal hypertension. They can be a source of considerable morbidity, mandating hospitalization, blood transfusions, angiographic or surgical intervention and may even be fatal.
We describe a rare instance of parastomal variceal bleeding in a patient who had undergone a radical cystectomy and ileal conduit-urinary diversion in 2011 for a high-grade muscle-invasive transitional cell carcinoma of the urinary bladder, which was managed via simple suture-ligation. Though reported as a temporary measure, he remained stable till date.
The point to note is that this approach is beneficial, especially in an emergent scenario- to avoid missing this unusual occurrence, at a usually missed site.
Introduction
Parastomal or stomal varices are rarely encountered with only a handful of cases having been reported in the literature to date, and a majority of those occurring secondary to subsequently developed portal hypertension. They can be a source of considerable morbidity, mandating hospitalization, multiple blood transfusions, angiographic or surgical intervention and may even be fatal if left untreated.
We describe a rare instance of parastomal variceal bleeding in our patient who had undergone a radical cystectomy and ileal conduit-urinary diversion, in 2011 for a high-grade muscle-invasive transitional cell carcinoma of the urinary bladder. He was on regular surveillance protocol and recurrence free till date.
The point we would like to highlight to our oncological community is the extreme difficulty in diagnosis as well as the dilemma in the management of this rarely occurring disease entity, as well as an easy temporarising measure.
Case report
A 64 year old gentleman presented to the emergency department with intermittent, but profuse bleeding in his stoma bag, since the past 1 month. In between stomal urine was completely clear.
He had undergone a radical cystectomy and ileal conduit-urinary diversion, in 2011 for a high-grade muscle-invasive transitional cell carcinoma of the urinary bladder (Final histology pT2N0Mx). He was on our regular surveillance protocol and recurrence-free to date. There was no associated fever, abdominal pain, altered bowel habits or any history of chronic liver disease or vascular abnormalities such as varicose veins.
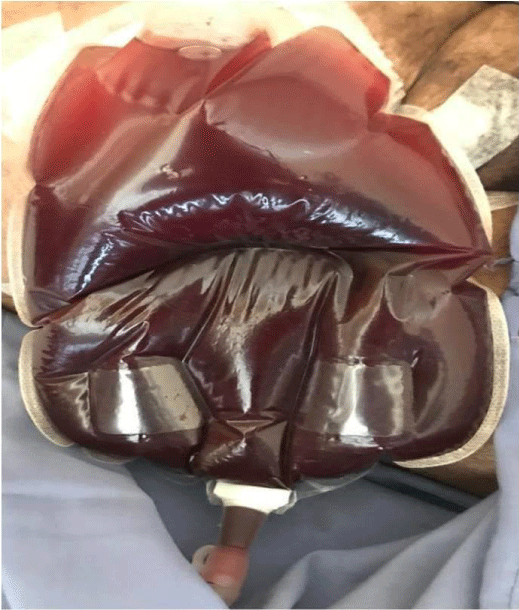
At presentation, he was haemodynamically stable with a non-tender abdomen. His stoma bag had gross haematuria (Figure 1). Biochemical workup confirmed haemoglobin of 5.1gm/dl, total leukocyte count 12000/cumm and platelets 1.41 lakhs/cumm. Liver function tests, coagulation profile, and all other blood investigations were within normal limits. He was managed with transfusion of 4 units of packed RBC (Red Blood Cells). The post transfusion haemoglobin improved to 9.8gm/dl.
After the primary haematuria, his urine cleared off completely and during his first 3 days of hospitalization there was no further bleeding episode. However, on the 4th day there was a recurrence of gross haematuria with a drop in haemoglobin to 7.8gm/dl.
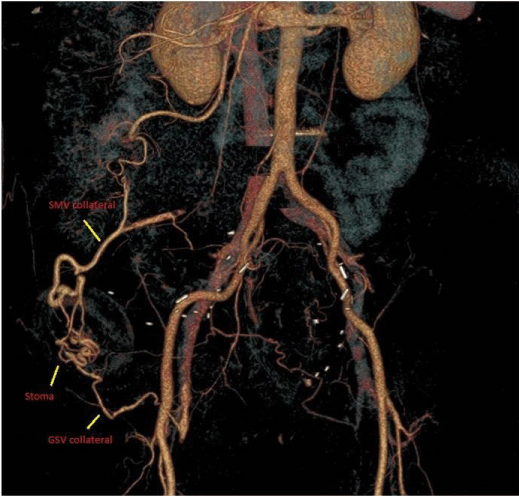
A CT[Computed Tomography] angiogram was done in order to identify the source of bleeding and rule out any upper renal tract lesion. The angiogram showed dilated tortuous stomal venous collaterals- one of which was draining into the SMV[Superior Mesenteric Vein](along the superior margin of the stoma) and the other draining into the right great saphenous vein(along the inferior margin of the stoma) (Figure 2). There were no features of portal hypertension or portal or splenic vein thrombosis.
No interventional radiological intervention was possible due to the risk of stomal necrosis in addition to difficulty in extremely precise super-selective embolization.
A conduitoscopy to rule out any local pathology or visible varices (per-stomal flexible cystoscopy) revealed a normal healthy ileal mucosa, no obvious bleeding point/varices identified.
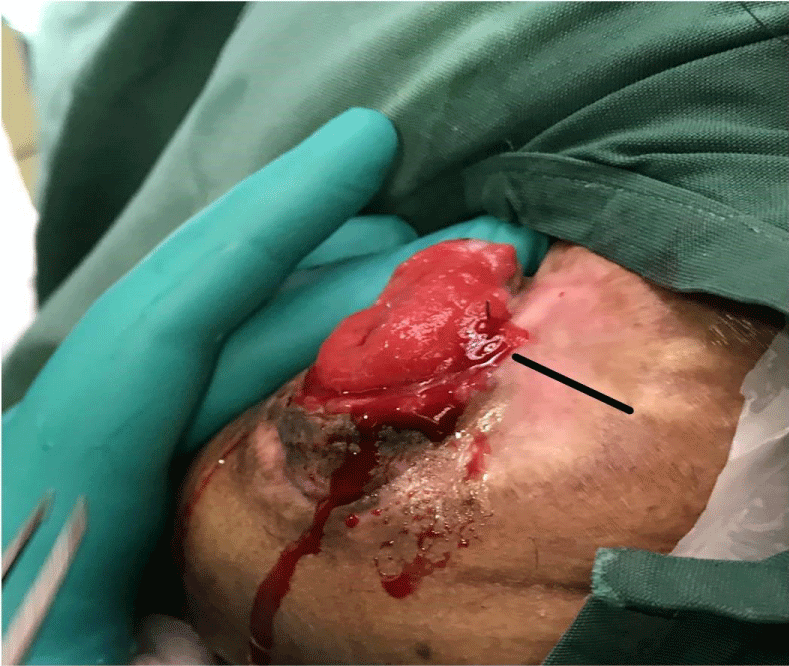
On careful examination, we were able to identify a parastomal bleeding varix, on the surface, at 3 o’clock position (which corroborated with the CT angiographic images) (Figure 3). The bleeding vessel was underrun with interrupted vicryl 3-0 sutures. An additional suture was taken at the 6 O’clock position in accordance with the CT-position of the second varix from the GSV [Great Saphenous Vein].
He was observed for48 hours post-intervention and then discharged in a stable condition with no further episode of bleeding. Patient has remained asymptomatic at 3 months follow up with a healthy stoma.
Discussion
Parastomal bleeding varices are infrequently encountered. Their rarity makes them almost “surgically notifiable”. Peri or parastomal variceal bleeding accounts for up to 5% of all variceal bleeds, as per available literature [1]. Most of the available data about parastomal variceal bleeding is obtained from case reports or short series of cases [1].
Any surgical intervention involving the apposition of abdominal structures (drained by the systemic veins) to the bowel (drained by the portal tributaries) might result in the formation of collateral vessels at an unusual site [1]. Various aetiologies have been postulated for their occurrence, with an ill-fitting stoma apparatus [2] and underlying portal hypertension, which is the most common [3,4]. In our case, there was no underlying portal hypertension, and the patient was well versed with the stoma appliance, having been using the same for the past 9 years.
Bleeding stomal varices, by themselves, carry increased morbidity due to recurrent episodic bleeding, chronic anaemia requiring transfusions, and hospitalization. Treatment options reported in the literature include conservative treatments such as local wound care, pressure dressing, suture ligation, cautery, and injection sclerotherapy with variable outcomes [4].
Speir, et al. [5] in their analysis of 74 studies (n=234 patients) with bleeding stomal varices, concluded that conservative measures are temporary ways to stop bleeding in these patients, especially with a background of portal hypertension and a vast majority would eventually require a definitive approach such as trans-jugular intravascular trans-hepatic shunts, surgical shunts, or liver transplantation [5].
Ahmed Helmy, et al. [1] have also recommended conservative therapies like endoscopic therapy, interventional therapy and surgical shunt, or liver transplantation as the possible management options. Sclerotherapy or band ligation of the stomal varices, run the risk of potential necrosis and massive haemorrhage following sloughing of the occluded varices [1]. Thus there is no single recommended standard therapy for parastomal variceal bleeding.
In our patient, there was no clinico-radiological evidence of underlying cirrhosis or portal hypertension. We do not recommend our approach as a definitive one, but this can definitely be a practical option to tackle parastomal bleeding with no underlying liver disease or portal hypertension, especially in an emergent scenario.
Conclusion
Bleeding parastomal varices are a rare entity, with significant morbidity. Though they occur most commonly on a background of portal hypertension, they can be seen even in its absence. Recurrence of the disease in the upper tracts or uretero-ileal anastomosis, must be excluded.
Our case highlights this brief, as well as simple suture-ligation, as a method to immediately stop this bleeding from having catastrophic outcomes. Though reported as a temporary measure, our patient has remained stable to date.
We would like to highlight this scenario to our oncological fraternity, to keep this approach in mind, especially in an emergent scenario- to avoid missing this unusual occurrence, at a usually missed site.
As is rightly said, “what the mind knows is what the eyes see”.
- Helmy A, Al Kahtani K, Al Fadda M (2008) Updates in the pathogenesis, diagnosis and management of ectopic varices. Hepatol Int 2: 322-334. Link: https://bit.ly/3mWNRdR
- Gowda S, Sethi P, Motapothula U (2020) Peristomal variceal hemorrhage at the ileal conduit site due to extrahepatic portosystemic shunt. Indian J Urol 36: 130-132. Link: https://bit.ly/3mW8yGz
- Khan F, Vessal S, Gordon-Williams R (2011) Bleeding from peristomal varices: A complication of portal hypertension. BMJ Case Rep 2011: Bcr0820114598. Link: https://bit.ly/3rulPJY
- Kang E, Yoon S, Kim S, Cho JH, Kang JM, et al. (2009) Bleeding from an Ileal Conduit Stomal Varix: Diagnosis with Three-Dimmensional Volume Rendered Images by the use of Multidetector-Row CT (MDCT) and Management with a Transjugular Intrahepatic Portosystemic Shunt. Journal of the Korean Society of Radiology 60: 227. Link: https://bit.ly/3mVQ5dl
- Spier BJ, Fayyad AA, Lucey MR, Johnson EA, Wojtowycz M, et al. (2008) Bleeding stomal varices: case series and systematic review of the literature. Clin Gastroenterol Hepatol 6: 346-352. Link: https://bit.ly/3mX2DkK
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
