Archive of Urological Research
Repeated selective arterial embolization without surgical resection in the management of a giant sporadic renal angiomyolipoma in a female patient of childbearing age – A Case Report
Foo Chek Hao1, Pandiyan Pannirselvam1, Park Joon Jae2*, Ng Foo Cheong2 and Ng Keng Sin3
2Department of Urology, Changi General Hospital, Singapore
3Department of Radiology, Mount Alvernia Hospital and Changi General Hospital, Singapore
Cite this as
Foo CH, Pannirselvam P, Park JJ, Ng FC, Ng KS (2020) Repeated selective arterial embolization without surgical resection in the management of a giant sporadic renal angiomyolipoma in a female patient of childbearing age – A Case Report. Arch Urol Res 4(1): 076-079. DOI: 10.17352/aur.000024Introduction: Angiomyolipomas (AML) are the commonest benign renal tumors. Most are small and found incidentally, but some can reach sizes of >20cm (giant AMLs). Due to their risk of spontaneous hemorrhage, these giant AMLs are most commonly treated by surgical resection with or without preoperative Selective Arterial Embolization (SAE). To our knowledge, there have been no giant AML cases that were treated solely by SAE in the published English literature.
Methods: We present a case of sporadic giant renal AML in a 26-year-old female patient solely treated with SAE. The patient initially presented with a painless right-sided abdominal mass. A Computed Tomography (CT) of the abdomen and pelvis found multiple bilateral renal AMLs, the largest of which measured 25.3×19.6×9.4 cm arising from the right interpolar region. Subsequent screening tests show no features to suggest the presence of tuberous sclerosis.
Result: A total of four cycles of SAE was performed using Lipiodol (ethiodized oil), absolute alcohol and polyvinyl alcohol particles over a period of 48 months. The patient experienced post-embolization syndrome which resolved with supportive treatment. At 80 months follow up, the largest AML in the right kidney had decrease in size from 25.3 to 13.9 cm. The patient was counselled about the increased risk of spontaneous rupture during any future pregnancy and has so far declined surgical resection of her AMLs.
Conclusion: Multiple cycles of embolization have been shown to achieve a good response. SAE is a safe treatment modality and may be a viable nonsurgical option in the management of giant AMLs.
Abbreviations
AML: Angiomyolipoma; SAE: Selective Arterial Embolization; CT: Computed Tomography
Introduction
Renal angiomyolipomas (AML) are the commonest benign renal tumor. In the literature, an AML of >20 cm is commonly labelled as a giant AML (although some have a lower cut off value of >10 cm). Giant AMLs are clinically significant due to the potentially life-threatening complication of retroperitoneal hemorrhage and hence they merit early prophylactic intervention [1].
Elective Selective Arterial Embolization (SAE) is a minimally invasive treatment option observed to have outstanding technical success rates while preserving renal function and it is the treatment of choice for large or symptomatic AML. They also allow rapid hemodynamic stabilization in those patients presenting with acute spontaneous hemorrhage [2].
We present a clinical case of sporadic giant renal AML on a female patient of child bearing age measuring 25.3×19.6×9.4 cm presenting as a painless palpable abdominal mass. She responded well to four cycles of minimally invasive SAE and achieved size reduction after the third and fourth cycle to a current size of 13.6×10.3×9.3 cm.
Case presentation
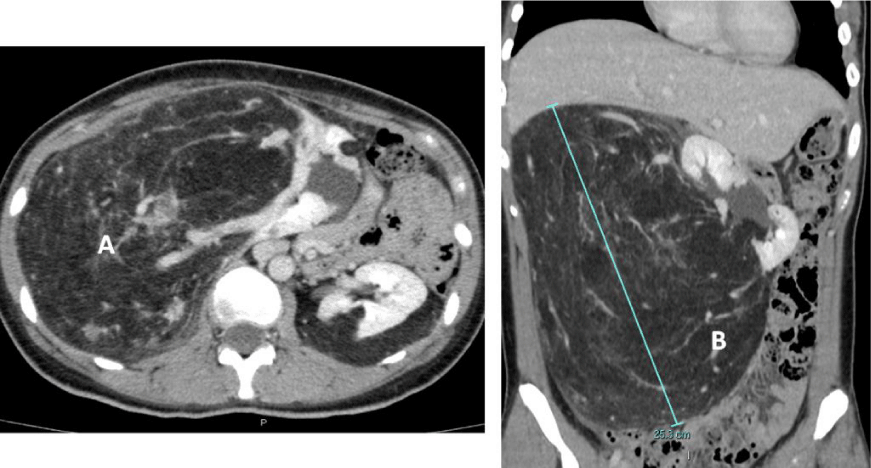
We present a 32-year-old east Asian female patient with a right-sided sporadic giant renal AML. Six years prior in April 2013, at 26 years of age, the patient was referred to the urologist for a palpable right-sided abdominal mass. She had no abdominal pain or hematuria. She had no significant past medical history. Her obstetric history was of gravida 0 and para 0 and she continuous to be so at the time of publication. A Computed Tomography (CT) of the abdomen and pelvis found multiple bilateral AMLs, with the largest one arising from the right kidney measuring 25.3×19.6×9.4 cm (Figure 1). A screening CT brain and CT chest did not show other features suggestive of tuberous sclerosis such as brain cortical tubers or lymphangioleiomyomatosis of the lungs.
Few weeks later, the patient underwent an elective Selective Arterial Embolization (SAE) of the right giant AML by the interventional radiologist. Vascular access was obtained via the right common femoral artery and a 6-French vascular sheath was inserted via a modified Seldinger technique. Flush aortogram was obtained before cannulation of right renal artery with a 5-French Cobra catheter (Cordis). A digital subtraction renal angiogram was obtained and branches supplying the right AML were super selected with a 2.7-French Progreat microcatheter (Terumo). A mixture of Lipiodol (Guerbet) and absolute alcohol was administered, followed by polyvinyl alcohol (PVA) particle (500 to 750 microns) embolization. The patient experienced right flank pain and fever consistent with post-embolization syndrome which resolved with supportive treatment alone.
Follow up CT abdomen and pelvis was performed one month later in May 2013 which showed reduced intra-tumoral vascular enhancement. The size of the giant AML remained unchanged. A second elective embolization was performed in a similar manner in June 2013. No post-embolization syndrome was encountered this time. Repeat CT abdomen and pelvis was performed and by January 2014, which showed a significant reduction in size, now measuring 17.3×13.9×11cm.
Subsequently, between May 2014 and May 2017, she underwent two further cycles of SAE to her giant right AML as well as two cycles to her smaller left AMLs. Renal angiogram at each SAE showed satisfactory decrease of intra-tumoral vasculature (Figure 2). Again, no post-operative complications or post-embolization syndrome was encountered. The latest CT abdomen / pelvis was performed April 2019, showed that the right giant AML had further decreased in size to 13.6×10.3×9.3 cm from 25.3×19.6×9.4cm. (Figure 3).
The patient, being of childbearing age, was warned about the increased risk of spontaneous bleeding during any future pregnancy. There is also a theoretical limited space for the expected expanding uterus that one should take into consideration. Therefore, the patient was offered bilateral open partial nephrectomies to excised the remnant AMLs. However, she declined surgery for multiple reasons. Among them, the possible risk of requiring a total nephrectomy should excessive bleeding is encountered intraoperatively.
At 80-months follow up the patient remained clinically well with no episodes of colic or hematuria and will continue to be followed up with routine CT scans.
Discussion
AMLs are the commonest benign renal tumors with a reported incidence of 0.4% and a higher predisposition in females [1]. Histology tends to show perivascular epithelioid cell tumors composed of adipose tissues, atypical blood vessels and smooth muscles. These atypical blood vessels are prone to aneurysmal formation and subsequent rupture. Renal AMLs may present sporadically or in association with tuberous sclerosis complex. These tumors tend to grow slowly, but some may enlarge up to 4 cm per year, especially during pregnancy or oral contraceptive therapy [3]. Giant AMLs are rare, with only 9 other sporadic cases reported in literature that are larger than 20 cm. To date, there is no universally agreed definition for giant AMLs, but a common cut off value is >20 cm [4] but others have put a lower value of >10 cm [5].
Although most non-giant AMLs are asymptomatic and discovered incidentally, all cases of giant AML identified by Alshehri were symptomatic at the time of diagnosis [4]. Symptoms included dull abdominal pain, flank mass, abdominal bloating and nausea or vomiting. It is well known that that AMLs >4 cm have a higher incidence of spontaneous bleeding leading to retroperitoneal, renal subcapsular or perineal space hemorrhage [5,6]. Risk factors for bleeding include tumor size, grade of angiogenic component of tumor and association with tuberous sclerosis [7]. As more than 25% of AMLs carry estrogen and progesterone receptors they are thought to grow during pregnancy or with oral contraceptive use. There are now numerous case reports of spontaneous bleeding of AML during pregnancy. None of which met the criteria of a giant AML with a cut off value of >20cm [8].
Renal ultrasound is a safe diagnostic modality to identify AMLs as well-circumscribed hyperechogenic masses with posterior acoustic shadowing. Contrast enhanced CT is an accurate diagnostic modality to detect the presence of fat attenuation and differentiate from renal cell carcinoma, though diagnosis may be challenging in 5% of AMLs with minimal fat content [9]. Interventions are offered in patients with tumor diameters >4 cm or those who are symptomatic. Options include tumor enucleation, partial or total nephrectomy, or minimally invasive therapies such as selective arterial embolization, radiofrequency ablation or cryoablation [10]. Surgery is currently advocated for hilar tumors, those with uncertain diagnosis or have vascular anatomy which might cause technical failure during embolization [11]. Embolization with alcohol/Lipiodol mixtures or particles such as polyvinyl alcohol (PVA) or spheres is preferred as they allow complete occlusion of the feeding arteries [10].
At present, the only medical therapy for AMLs is the use of the mammalian target of rapamycin (mTOR) inhibitor called Everolimus. However, its use has only been reported in patients with tuberous sclerosis associated AMLs [12].
There have been case reports of giant AML treated with SAE pre-operatively to reduce operative blood loss.
Singla, et al. reported a case of giant renal AML measuring 26×22 cm that was treated with preoperative embolization followed by partial nephrectomy [13]. To our knowledge, our case is the first known reported of giant renal AML to be managed with SAE alone.
Multiple studies have quantified the success and complication rates of SAE, albeit only in smaller AMLs. In a systematic review of 524 AMLs, Murray, et al. observed a technical success rate of 93% for SAR, with mean tumor size reduction from 8.8 to 3.4 cm (38%) at 39 months [14]. Repeat embolization or surgery was required in 21% of patients, usually due to tumor growth or revascularization. Post-embolization syndrome was the commonest complication with an incidence of 35.9%. No procedural mortality was reported.
Hocquelet, et al. found a mean volumetric reduction of 72% at median follow-up time of 28 months in 39 AMLs [15]. Tumor size reduction has been found to be greatest early after embolization before gradually plateauing and has been better in tumors with larger angiomyomatous components or lower fat components [16,17].
We, the authors, feels that with increasing worldwide use of CT scans the discoveries of such giant AMLs may become more common. Discoveries in younger, asymptomatic female patients (like in our case) will add further challenge to an already complex clinical scenario. Due to their rarity, the optimal management of giant AMLs has not been established. As interventional radiology expertise continuous to grow, we currently do not know what is the role of SAE as a sole treatment modality in the management of giant sporadic AMLs and will require further long-term data based on randomized studies.
Conclusion
We report a case of sporadic giant renal AML on a female patient of child bearing age that underwent four SAE sessions with good response. The patient declined further surgical resection and remains well after 80 months follow up. Repeat SAE is a safe treatment modality and may be a viable non-surgical option in the management of giant AMLs.
- Fittschen A, Wendlik I, Oeztuerk S, Kratzer W, Akinli AS, et al. (2014) Prevalence of sporadic renal angiomyolipoma: a retrospective analysis of 61,389 in- and out-patients. Abdom Imaging 2014; 39: 1009-1013. Link: https://bit.ly/3kz76d2
- Faddegon S, So A (2011) Treatment of angiomyolipoma at a tertiary care centre: the decision between surgery and angioembolization. Can Urol Assoc J 5: E138- E141. Link: https://bit.ly/35EGIIq
- Seyam RM, Bissada NK, Kattan SA, Mokhtar AA, Aslam M, et al. (2008) Changing trends in presentation, diagnosis and management of renal angiomyolipoma: comparison of sporadic and tuberous sclerosis complex-associated forms. Urology 72: 1077-1082. Link: https://bit.ly/2HJD6g6
- Alshehri M, Hakami B, Aljameel N, Alayyaf M, Raheem AA (2020) Sporadic giant renal angiomyolipoma: A case report and literature review of clinical presentation, diagnosis, and treatment options. Urol Ann 12: 167-171. Link: https://bit.ly/3eaLIZe
- Chen P, Jin L, Yang Y, Chen Z, Ni L, et al. (2017) Giant renal angiomyolipoma: A case report. Mol Clin Oncol 7: 298-300. Link: https://bit.ly/37L6HjV
- Albersheim-Carter J, Klein M, Murugan P, Weight CJ (2016) Partial Nephrectomy for a Massive Sporadic Renal Angiomyolipoma: Case Report and Review of the Literature. Case Rep Urol 2016: 3420741. Link: https://bit.ly/2TvL7HY
- Ramon J, Rimon U, Garniek A, Golan G, Bensaid P, et al. (2009) Renal angiomyolipoma: long-term results following selective arterial embolization. Eur Urol 55: 1155-1161. Link: https://bit.ly/3jAfgAv
- Çetin C, Büyükkurt S, Demir C, Evrüke C (2015) Renal angiomyolipoma during pregnancy: Case report and literature review. Turk J Obstet Gynecol 12:118-121. Link: https://bit.ly/2HJzhrj
- Simmons JL, Hussain SA, Riley P, Wallace DM (2003) Management of renal angiomyolipoma in patients with tuberous sclerosis complex. Oncol Rep 10: 237-241. Link: https://bit.ly/3e10odn
- Kiefer RM, Stavropoulos SW (2017) The Role of Interventional Radiology Techniques in the Management of Renal Angiomyolipomas. Curr Urol Rep 18: 36. Link: https://bit.ly/3e6JWZ8
- Razik A, Das CJ, Sharma S (2019) Angiomyolipoma of the Kidneys: Current Perspectives and Challenges in Diagnostic Imaging and Image-Guided Therapy. Curr Probl Diagn Radiol 48: 251-261. Link: https://bit.ly/3ozbYBe
- Bissler JJ, Kingswood JC, Radzikowska E, Zonnenberg BA, Belousova E, et al. (2017) Everolimus long-term use in patients with tuberous sclerosis complex: Four-year update of the EXIST-2 study. PLoS One 12: e0180939. Link: https://bit.ly/3jB03yU
- Singla A, Chaitanya Arudra SK, Bharti N (2009) Giant sporadic renal angiomyolipoma treated with nephron-sparing surgery. Urology 74 :294-295. Link: https://bit.ly/3oxKHiq
- Murray TE, Doyle F, Lee M (2015) Transarterial Embolization of Angiomyolipoma: A Systematic Review. J Urol 194: 635-639. Link: https://bit.ly/3kvJJRs
- Hocquelet A, Cornelis F, Le Bras Y, Meyer M, Tricaud E, et al. (2014) Long-term results of preventive embolization of renal angiomyolipomas: evaluation of predictive factors of volume decrease. Eur Radiol 24: 1785-1793. Link: https://bit.ly/3kGK3gw
- Lee SY, Hsu HH, Chen YC, Huang CC, Wong YC, et al. (2009) Embolization of renal angiomyolipomas: short-term and long-term outcomes, complications, and tumor shrinkage. Cardiovasc Intervent Radiol 32: 1171-1178. Link: https://bit.ly/31RVJWi
- Patatas K, Robinson GJ, Ettles DF, Lakshminarayan R (2013) Patterns of renal angiomyolipoma regression post embolisation on medium- to long-term follow-up. Br J Radiol 86: 20120633. Link: https://bit.ly/3ovEXpr
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.



 Save to Mendeley
Save to Mendeley
