Archives of Renal Diseases and Management
Nutritional status of patients on chronic hospital hemodialysis vs home hemodialysis
Duranti Diletta1*, Ralli Chiara2 and Duranti Ennio3
2Dialysis Hospital of Nottola, Montepulciano (Siena), Italy
3Consultant Nephrologist, Arezzo, Italy
Cite this as
Duranti D, Ralli C, Duranti E (2020) Nutritional status of patients on chronic hospital hemodialysis vs home hemodialysis. Arch Renal Dis Manag 5(1): 001-004. DOI: 10.17352/2455-5495.000033Introduction
Although the majority of the End Stage Renal Disease patients are treated with conventional thrice weekly in-center hemodialysis, there has been recent growth in the adoption of home dialysis modalities, mainly peritoneal dialysis and in these last 10 years the resurgence of home hemodialysis in its daily or daily night version [1-3]. Latest observational studies have identified that home hemodialysis (HHD) is associated with improved patient survival compared with conventional in center hemodialysis (ICHD). At this regard, comparisons of HHD versus ICHD are considered limited by patient selection, because those who are able to receive HHD will have better health outcomes by virtue of their demographics, social supports, socioeconomic factors, and underlying health state as opposed to the dialysis modality itself [2-4]. Even if interesting, these comparisons do not allow one to determine whether the survival advantage is due to the dialysis modality or home location. Bearing in mind these assumptions, we wanted to select a group of pts in ICHD and compare them to a group with similar characteristics in HHD, in order to evaluate the respective Nutritional status, Food Intake and then alimentary habits, parameters that affect the survival of patients on chronic dialysis treatment.
Materials and methods
We compared two groups of patients on chronic dialysis treatment: a group switched from hospital hemodialysis treatment to HHD treatment and a group of patients, with similar characteristics, continuing ICHD treatment. Both groups consisted of 9 patients (5 males and 4 females), aged between 50 and 60 years, similar dialysis age and similar basic nephropathy (Table 1). Patients with severe heart failure, severe respiratory failure, solid and liquid neoplasms, chronic inflammatory diseases and psychiatric illness were excluded. For each patient we evaluated, at the beginning of the first session of the week, considered for our study ,the biochemical tests : Urea, Creatinine, Weekly KT/V, Albumin, Lynfocytes, Transferrin, Na, K, Ca, P, PTH, Uric Acid, CRP, Glucose, Total Cholesterol, Triglycerides, HDL, LDL, Bicarbonates. In addition, we considered the physiological parameters, related to general health and nutritional status: Height, Body dry weight, Body Mass Index (BMI), Arterial blood pressure, Protein Catabolic Rate (nPCR), Interdialytic weight gains after 24 e 48 hours. Among the bioimpedance parameters calculated, for each patient, with the BCM monitor of the Fresenius company, outside the dialysis session, we considered the Phase angle, the Body Cellular Mass (BCM) and the Body Cellular Mass Index (BCMI). Parameters that represent the most precise indices of nutritional status: A phase angle less than 5 °, a BCM less than 40% and 38% of body weight respectively in men and in women more then 50years old, a BCMI less than 8 Kg/m2 in men and 7 Kg/m2 in women represent a state of malnutrition [5-7]. In addition, everyone was given questionnaires related to self-assessment of appetite, ie Comprehensive Nutrition Assessment Questionnaire (CNAQ) which consists of 8 questions related to the sense of hunger, the sense of post-prandial fullness, the perception of the taste of food and flavors, the number of daily meals and the tone of mood; for each question a score from 1 to 5 is assigned, and a score <28 indicates a risk of weight loss of 5% in the following 6 months [8]. The degree of malnutrition/inflammation was obtained by the Malnutrition Inflammation Score (MIS), that is an index of protein-caloric malnutrition calculated according to ten parameters, for each of which a score from 0 to 3 is assigned: from the anamnesis and the physical examination Variations of the Dry Weight are obtained at the end of dialysis, Food Intake, Gastrointestinal Symptoms, Functional Capacity and Comorbidity in relation to dialysis age, Subcutaneous fat, Muscular Atrophy, BMI; in the laboratory, Serum Albumin and Iron-Total Binder Capacity (TIBC) are measured: the first score band (from 0 to 5) corresponds to a normal nutritional status, the second band (from 6 to 10) corresponds to Average Malnutrition, the third band of score (>10) at Moderate-Severe malnutrition [9]. On the basis of the food diary we reconstructed the patients’ diet and estimated the daily intake of the main nutrients, comparing the results obtained with the Recommended intake levels of energy and nutrients for the Italian population (Italian acronym LARN), recommended by the Italian Society of Human Nutrition (SINU) [10]. The statistical differences between the two groups were evaluated with the Student’s T for unpaired data and the Chi square test when deemed appropriate.
Results
The two populations were similar and homogeneous in terms of sex distribution and the age of the components, as well as the dialysis age (Table 2). The group in ICHD included 5 pts in Bicarbonate dialysis, 2 pts in Acetate Free Biofiltration (AFB), 1 pt in Hemodiafiltration with endogenous Reinfusion (HFR) and 1 pt in online Hemodiafiltration (HDF), for which we stress that 45% of the patients were treated with high methods efficiency. On the contrary, the HHD group was treated with the NXstage method (Fresenius Medical Care), that is a low efficiency standard method [1] enhanced with an increase in the number of weekly dialysis sessions (at least 4-5 weekly). We emphasize that the weekly KT/V was higher, although not significantly, in the HHD group than in the ICHD group. In our opinion, this datum acquires a moderate importance , considering that the vascular access used, in the ICHD group, was the native arteriovenous Fistula in 8 pts and in only 1 pt a permanent central venous catheter; while in HHD group 3 pts used permanent CVCs, 5 pts native arteriovenous fistulas and 1 pt prosthetic graft .Therefore, presenting the latter group greater technical difficulties in the management of blood flows that allowed a lower purification efficiency for each dialysis session thus increasing weekly efficiency with a greater number of weekly dialysis sessions. As regards Body dry weight, Body Mass Index (BMI), Arterial blood pressure, did not show significant differences between the two populations. On the contrary the difference in the interdialitic weight increase (∆ WEIGHT) was significant in the long intervals and even more in the short intervals, infact the interdialytic increase values concerning ICHD patients compared to HHD patients was almost double both after 24 and 48 hours. The laboratory parameters showed no significant differences between the two groups, except for a higher concentration of albumin, a lower value of Ca, Uric Acid and an increase in Bicarbonates in the group of patients on HHD. BIA showed better mean values of Phase angle ( 5,4°± 1,1° vs 4,7°± 1,3° ) , BCM (34,1%±11,05% vs 27,3% ±11,3 % ), BCMI (8,1±2,6 Kg/m2 vs 7,1±2,8 Kg/m2) in HHD pts with respect to ICHD pts. The average nPCR values (>1 g/kg/day) were practically overlapping between the two populations, a value that the guidelines associate with a lower risk of morbidity. As regards appetite evaluation (Figure 1) a significant difference (p< 0,009) emerges in favour of HHD patients who all have a score > 28, while among ICHD patients two pts had a score < 28. So HHD treatment seems to favor more appetite conservation and therefore the prevention of weight loss in patients. As regards malnutrition and MIS questionnaire, significant differences (p< 0,001) have emerged between the two populations (Figure 2): Even if no patient was at risk of severe malnutrition, 4 of the ICHD patients showed scores indicative of average malnutrition, while all HHD patients showed a normal nutritional status. On the basis of the food diary we reconstructed the patients’ diet and estimated the daily intake of the main nutrients: The total caloric intake was 19 Kcal / Kg weight in ICHD vs a better intake of 26 Kcal/Kg weight in HHD even if below the recommended values (30-35 Kcal/Kg weight, LARN recommendations). In both populations, even the total protein intake resulted below the recommended values of 1-1.2 g prot/Kg weight by LARN reccomendations, even if better in HHD: 0.7 g prot/Kg weight in ICHD vs 0.9 g prot/Kg weight in HHD. P intake was very close to the maximum LARN recommended values of 800 mg/day: 733 mg for ICHD vs 801 mg for HHD. The overall percentage of proteins was in line with the LARN values of 15% (15% for ICHD vs 14% for HHD). The percentages of the other macronutrients were comparable in the two populations: Glucides 49% for ICHD vs 51% for HHD (51% LARN reccomendations) and lipids 37% in both populations (slightly higher with respect to 25-30% of LARN reccomendations) (Table 3).
Discussion
Current clinical practice guidelines recommend that the dose of dialysis for hemodialysis schedules other than thrice weekly be measured by determination of the weekly standard Kt/V defined as the weekly urea generation rate factored by the average predialysis serum urea concentration during a week normalized to the total volume of distribution of urea [12-15]. Current clinical practice guidelines for hemodialysis adequacy suggest a target Kt/V of 2.3, with a minimum delivered dose of 2.1 [14,15]. On the basis of these indications the two groups of patients received an excellent weekly dialysis dose, with better values for HHD than for the ICHD. In this regard, our work confirms the data of previous works, namely that the purification treatment in home dialysis is better than the three-weekly hospital treatment [16-20]. In our case also independently of the availability of more efficient vascular accesses (5 pts of HHD group were treated with a CVC access with respect to only 1 pt in ICHD group). Other data such as better control of albumin, better control of calcium, phosphorus, uric acid and bicarbonates are indicative that home treatment allows, as already reported in previous works, a better control of uremic syndrome with implications also positive on nutritional status. To confirm these data are also the questionnaires related to appetite and inflammation/malnutrition. The sum of all cells of the inner organs and muscles, that are actively involved in the metabolic processes is called BCM. Given that all of the body’s metabolic function is performed within the cells of the BCM, the BCM is the main specification for the analysis of a patient’s nutritional state. It is also used as the standard specification for establishing the calorific requirement of the body and for the assessment of energy consumption.So our study confirms other various studies, that frequent hemodialysis or HHD preserve nutritional status and prevent or attenuate the anticipated decline in BCM [5-7] and has been associated with improved appetite, increased protein and caloric intake, and incremental increases in muscle mass, and serum albumin [5-7] . This data are confirmed in the light of the results of the HEMO trial whose study included two groups of subjects on dialysis: The first group of subjects dialyzed 3x per week at standard and the second group at high per session Kt/V, with low and high flux dialyzers [11,12]. All of them showed a progressive decline in serum albumin, nPCR, and body weight [11] unaffected by dialysis dose or flux. In other words this study seems to demonstrate that the dialysis efficiency of techniques and membranes seems to be less effective than the number of weekly dialysis sessions even if performed for less long times and with significantly lower blood and dialysate flows. In addition and to confirm the HEMO study data , the higher BMI values of the ICHD patients associated with greater interdialitic weight gains, both at 24 and 48 hours, compared to HHD patients, seem to demonstrate a greater expansion of volumes and therefore a greater water retention.The food diary shows a lower daily caloric and protein load compared to the LARN recommendations in both groups of patients, although slightly better in HHD pts. Therefore, it is our opinion that these data are indicative of incorrect eating habits that affect the tendency to malnutrition and therefore require, in both groups and therefore in all patients, on chronic hemodialysis treatment, a continuous food counseling. In conclusion, our work seems to confirm a better metabolic control in subjects treated with home hemodialysis, compared to patients in hospital hemodialysis. In addition, the home hemodialysis patients seem to have a better nutritional status even if insufficient compared to normal subjects. Therefore, it is our opinion that the periodic presence of a nutritionist is necessary in dialysis centers, to contribute and help correct patients’ dietary errors.
- Ralli C, Duranti E (2017) The History of Home Hemodialysis and its Possible Revival. Enliven: Nephrology and Renal Studies 4: 1-6. Link: https://bit.ly/2wAXI4V
- United States Renal Data System (2016) USRDS Annual Data Report: Epidemiology of Kidney Disease in the United States, Bethesda, MD, National Institutes of Health, National Institute of Diabetes and Digestive and Kidney Diseases.
- Rivara MB, Mehrotra R (2014) The changing landscape of home dialysis in the United States. Curr Opin Nephrol Hypertens 23: 586-591. Link: https://bit.ly/2Jr7ARA
- Centers for Medicare & Medicaid Services (CMS) (2015) HHS: Medicare program; end-stage renal disease prospective payment system, and quality incentive program. Final rule. Fed Regist 80: 68968-69077. Link: https://bit.ly/2WS2BkL
- Mandolfo S, Farina M, Imbasciati E (1995) Bioelectrical impedance and hemodialysis. Int J Artif Organs 18: 700-704. Link: https://bit.ly/2wLL1Ej
- Kyle UG, Bosaeus I, De Lorenzo AD, Deurenberg P, Elia M, et al. (2004) Bioelectrical impedance analysis—part I: review of principles and methods. Clin Nutr 23: 1226-1243. Link: https://bit.ly/2wMdmKK
- Foster R, Lukaski HC (1996) Whole-body impedance-what does it measure? Am J Clin Nutr 64: 388S-396S. Link: https://bit.ly/2wKAauc
- Barrett JS, Gibson PR (2010) Development and Validation of a Comprehensive Semi-Quantitative Food Frequency Questionnaire that Includes FODMAP Intake and Glycemic Index. J Am Diet Assoc 110: 1469-1476. Link: https://bit.ly/2xArQ06
- Ho LC, Wang HH, Peng YS, Chiang CK, Huang JW, et al. (2008) Clinical Utility of Malnutrition-Inflammation Score in Maintenance Hemodialysis Patients: Focus on Identifying the Best Cut-Off Point. Am J Nephrol 28: 840-846. Link: https://bit.ly/2xBBX5a
- SINU (2014) Società Italiana di Nutrizione Umana. LARN, Livelli di Assunzione Raccomandati di Energia e Nutrienti per la Popolazione Italiana, IV Revisione . Milano, SICS Ed. Link: https://bit.ly/3dG2Wgc
- Eknoyan G, Beck GJ, Cheung AK, Daugirdas JT, Greene T, et al. (2002) Hemodialysis (HEMO) Study Group: Effect of dialysis dose and membrane flux in maintenance hemodialysis. N Engl J Med 347: 2010-2019. Link: https://bit.ly/3dyxXmp
- Rocco MV, Dwyer JT, Larive B (2004) The effect of dialysis dose and membrane flux on nutritional parameters in hemodialysis patients: results of the HEMO Study. Kidney Int 65: 2321-233. Link: https://bit.ly/2UvAV3D
- Miller JE, Kovesdy CP, Nissenson AR, Mehrotra R, Streja E, et al. (2010) Association of hemodialysis treatment time and dose with mortality and the role of race and sex. Am J Kidney Dis 55: 100-112. Link: https://bit.ly/2wKAtVS
- Daugirdas JT, Depner TA, Inrig J, Mehrotra R, Rocco MV, et al. (2015) National Kidney Foundation: KDOQI clinical practice guideline for hemodialysis adequacy: 2015Update. AmJ KidneyDis 66: 884-930. Link: https://bit.ly/39rSIwN
- Rivara MB, Ravel V, Streja EV, Obi Y , Soohoo M, et al. (2018) Weekly Standard Kt/Vurea and Clinical Outcomes in Home and In-Center Hemodialysis. Clin J Am Soc Nephrol 13: 445-455. Link: https://bit.ly/33TP4ut
- Rocco MV, Daugirdas JT, Greene T (2015) Long-term Effects of Frequent Nocturnal Hemodialysis on Mortality: The Frequent Hemodialysis Network (FHN) Nocturnal Trial. Am J Kidney Dis 66: 459-468. Link: https://bit.ly/2UJlSCk
- Hall YN, Larive B, Painter P (2012) Effects of six versus three times per week hemodialysis on physical performance, health, and functioning: Frequent Hemodialysis Network (FHN) randomized trials. Clin J Am Soc Nephrol 7: 782-794. Link: https://bit.ly/3dHbiEj
- Galland R, Traeger J, Arkouche W (2001) Short daily hemodialysis and nutritional status. A9m J Kidney Dis 37: S95-S98. Link: https://bit.ly/2UsZUEL
- Galland R, Traeger J, Arkouche W (2001) Short daily hemodialysis rapidly improves nutritional status in hemodialysis patients. Kidney Int 60: 1555-1560. Link: https://bit.ly/2Jr8e1s
- Spanner E, Suri R, Heidenheim AP, Lindsay RM (2003) The impact of quotidian hemodialysis on nutrition. Am J Kidney Dis 42: 30-35. Link: https://bit.ly/2JraW73

Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

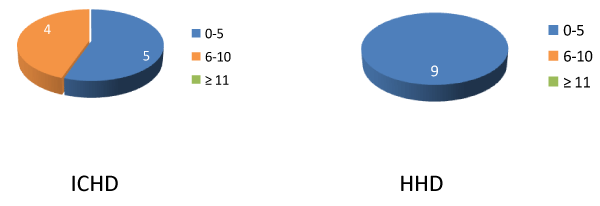
 Save to Mendeley
Save to Mendeley
