Annals of Robotics and Automation
Robotic Modified Orr-Loygue Rectopexy for Internal and External Rectal Prolapse
Arifa Siddika* and Shahab Siddiqi
Cite this as
Siddika A, Siddiqi S (2017) Robotic Modified Orr-Loygue Rectopexy for Internal and External Rectal Prolapse. Ann Robot Automation 1(1): 001-003. DOI: 10.17352/ara.000001Laparoscopic ventral mesh rectopexy is the gold standard treatment for external rectal prolapse and an excellent treatment for symptomatic internal rectal prolapse. However, there is a recurrence rate for this procedure, part of which can be attributed to the untreated posterior rectal prolapse component. Here we describe a robotic Orr-Loygue rectopexy where an additional posterior mesh rectopexy is performed. This differs from other surgical descriptions in that the posterior mesh can be sutured to the rectal tube without risking rectal denervation, which would be a difficult proposition using a laparoscopic approach.
Introduction
Laparoscopic ventral mesh rectopexy (LVMR) is the treatment of choice for external rectal prolapse (ERP) and there is good evidence to support its use for symptomatic internal rectal prolapse (IRP) [1]. A significant number of patients who undergo LVMR for symptoms attributable to IRP either do not improve or have a recurrence, as do 4% of patients who have had LVMR for ERP [2]. A proportion of the recurrence is thought to be due to significant residual posterior and/or lateral prolapse [3]. Ventral rectal fixation addresses anterior prolapse directly, but only elevates remaining circumferential prolapse indirectly. A modification of the LVMR, known as modified Orr-Loygue rectopexy (MOLR), aims to treat posterior IRP and ERP by suture or mesh fixation of mesorectum to the sacral promontory. However, posterior rectopexy has a high rate of recurrence [4,5]. Fixation of mesh to mesorectum will only indirectly secure the underlying rectal wall [6,7]. Additionally, fixation of mesh to mesorectal fat is insecure. Fixation points between mesh and rectal muscle or the anterior longitudinal ligament have a failure pressure higher than the maximum human intra-abdominal pressure, but fixation of mesh to mesorectum will fail at a lower pressure [8]. A narrow posterior dissection is needed to avoid rectal denervation [9]. This limits the distal extent of dissection. Theoretically, dissecting to Waldeyer’s fascia will allow suture fixation of mesh to the muscular rectal tube. This inherently stronger fixation may reduce recurrence, especially for low take-off IRP and ERP. This narrow distal dissection is achievable more readily using a robotic platform rather than a laparoscopic approach.
Workup
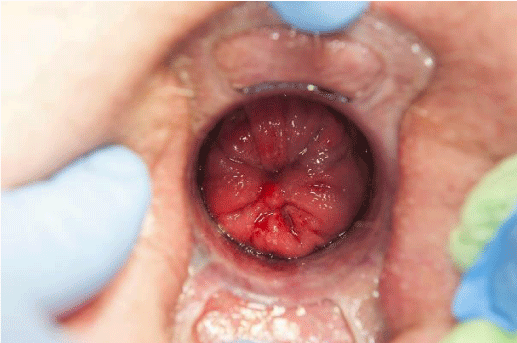
The preoperative workup consists of anorectal physiology studies, anal ultrasound, and defecating proctography. In equivocal cases, examination under anesthesia using a circular anal dilator is useful to assess the size, mural thickness, and location of take-off of the prolapse (Figure 1).
Operation
After general anesthesia with spinal infiltration, Intravenous antibiotic prophylaxis is administered and an indwelling urinary catheter is placed. A modified lithotomy position is used where the patient’s legs are placed in adjustable stirrups with sequential calf compression and the arms are wrapped and tucked alongside the body. A ‘Pink Pad’ (Pigazzi Patient Positioning System™, Xodus Medical and New Kensington, PA USA) is used to secure the body and a body warmer is applied.
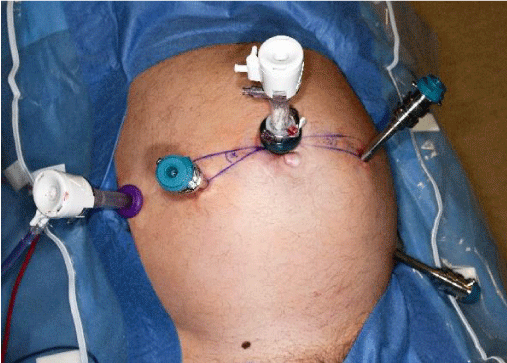
A 12mm trocar is inserted supra-umbilically and a laparoscopy performed. Additional ports are marked and placed after insufflation to 12mmHg. An 8mm trocar for robot arm-1 is inserted 8cm from the camera port 10 degrees caudal to the transverse umbilical line on the right (Figure 2). An assistant 5mm port is inserted lateral and 5cm cranial to the camera port, 5–8cm away from the arm-1trocar.The trocar for robot arm-2 is placed 8cm away from the camera port to the left, 10 degrees caudal to the transverse umbilical line. The trocar for robot arm-3 is inserted near the left anterior superior iliac spine 8–10cm away from the arm-2 trocar. The patient is then placed in a steep Trendelenburg position.
The da Vinci patient cart is docked near the left hip of the patient, aligning the patient cart and camera port in a straight line that crosses the anterior superior iliac spine. A zero-degree camera is used, along with scissors with monopolar diathermy, and a needle holder in arm-1, fenestrated bipolar diathermy forceps in arm-2, and a da Vinci Cadiere® forceps (428005) in arm-3.
The uterus (in women) or the recto-vesical pouch (in men) is elevated using a sling introduced through the skin above the pubis. The sigmoid colon is retracted and the epiploic fat is secured to the left flank using a Hem-o-lok® ligation system (5mm; Teleflex Medical, Wayne, PA, USA).
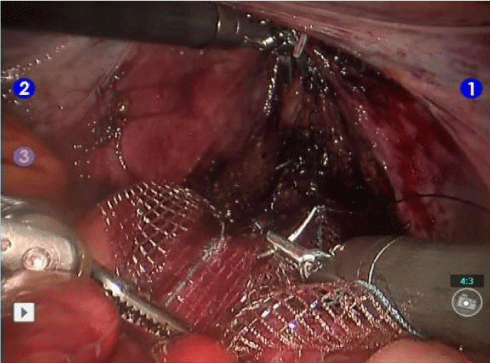
An incision is made over the right side of the sacral promontory, the transverse ligament over the sacral promontory is exposed, and the lateral rectal peritoneum is dissected to the pouch. A reverse J incision is made in the pouch and the rectovaginal plane identified. Dissection is continued to the pelvic floor. In men, dissection should be on the rectal side of Denonvilliers’ fascia to reduce the risk of nerve damage. Deep pouches should be excised. The width of the ventral dissection determines the width of the mesh (Dynamesh® PRS soft, PV350527; FEG Textilte chnik MbH, Aachen, Germany) to be used (2–3cm in men and 5cm in women). The length (16–18 cm) is the same in women and men (Figure 3). The anterior mesh is stitched to the sero-muscular rectum using 3-0 PDS II sutures (E91035; Ethicon Endo-Surgery Inc., Johnson & Johnson, Cincinnati, OH, USA) from the sphincters cranially in two parallel strips every 1.5cm and continued 2–3cm proximal to the peritoneal reflection to secure any high take-off prolapse. Additional pelvic floor fixation should be attempted. The mesh is not fixed to the sacral promontory at this stage. Examination under anesthesia of the anorectum is performed, and if the rectal prolapse has been reduced, the ventral mesh is fixed to the promontory. If elements of the prolapse remain, an MOLR is performed. The unsecured ventral mesh is used for traction.
A wide female pelvis and a gynecoid male pelvis allow for wider ventral dissection facilitating a wide ventral mesh to be sutured, easier access to the posterior distal rectal tube for further mesh fixation with less traction to the lateral rectal columns and nerves. It is in the narrow female pelvis and typical male pelvis, the stated advantages of a robotic platform over laparoscopy are striking. However, ventral dissection is limited before the lateral rectal columns are reached necessitating a narrow mesh. Reaching the posterior rectal muscle tube without undue traction on the lateral rectal columns is extremely challenging using laparoscopy, but achievable robotically.
A narrow posterior window created between the hypogastric nerves and the dissection is continued in the presacral plane to the muscular rectal tube. A 2×15cm Dynamesh patch is sutured to the rectal tube and proximally to the mesorectum. The posterior and anterior mesh is then secured to the sacral promontory using an Ethibond® suture (E6193S; Ethicon). The peritoneum is closed transversely with 2-0 coated Vicryl™ (E9902S; Ethicon). The retractions are then released and the ports closed. A vaginal pack is inserted and removed the following day. Ibuprofen, paracetamol and laxatives are prescribed for 6 weeks and codeine may be used as required.
The advantages of robotic surgery include stereotactic vision, a stable camera platform, improved access to the narrow pelvis, and less pelvic nerve damage [10].
Further, fixation of mesh to rectal muscle rather than to mesorectum may reduce the recurrence rate found with LVMR, whether performed for IRP or ERP. Outcome data for the first 32 cases performed by the authors are included in Table 1. The patients were followed up at 3 months, 6 months and 1 year and discharged unless there was ongoing problem.
Conclusion
A robotic MOLR is safe and feasible for patients with symptomatic IRP or ERP. Given that the long-term recurrence rate after LVMR for ERP is already low, we would only recommend robotic MOLR for ERP if there are additional symptoms of obstructive defecation syndrome. However, the long-term outcomes using this modified procedure are presently unknown.
- Samaranayake CB, Luo C, Plank AW, Merrie AE, Plank LD, et al. (2010) Systematic review on ventral rectopexy for rectal prolapse and intussusception. Colorectal Dis 12: 504-512. Link: https://goo.gl/u7SxjR
- Sahoo MR, Thimmegowda AK, Gowda MS (2014) A single centre comparative study of laparoscopic mesh rectopexy versus suture rectopexy. J Minim Access Surg 10: 18-22. Link: https://goo.gl/hVeAiQ
- Senapati A, Gray RG, Middleton LJ, Harding J, Hills RK, et al. (2013) PROSPER: a randomised comparison of surgical treatments for rectal prolapse. Colorectal Dis 15: 858–868. Link: https://goo.gl/xnPj2z
- Sayfan J, Pinho M, Alexander‐Williams J, Keighley MR (1990) Sutured posterior abdominal rectopexy with sigmoidectomy compared with Marlex rectopexy for rectal prolapse. Br J Surg 77: 143-145. Link: https://goo.gl/0QO1Cz
- Yoshioka K, Heyen F, Keighley MR (1989) Functional results after posterior abdominal rectopexy for rectal prolapse. Dis Colon Rectum 32: 835-838. Link: https://goo.gl/hD5QQI
- Liyanage CA, Rathnayake G, Deen KI (2009) A new technique for suture rectopexy without resection for rectal prolapse. Tech Coloproctol. 13: 27-31. Link: https://goo.gl/A5d8hI
- Kessler H, Jerby BL, Milsom JW (1999) Successful treatment of rectal prolapse by laparoscopic suture rectopexy. Surg Endosc 13: 858-861. Link: https://goo.gl/p0r41D
- Cobb WS, Burns JM, Kercher KW, Matthews BD, Norton HJ, et al. (2005) Normal intraabdominal pressure in healthy adults. J Surg Res 129: 231-235. Link: https://goo.gl/OKKRKt
- Luca F, Valvo M, Ghezzi TL, Zuccaro M, Cenciarelli S, et al. (2013) Impact of robotic surgery on sexual and urinary functions after fully robotic nerve-sparing total mesorectal excision for rectal cancer. Ann Surg 257:672-678. Link: https://goo.gl/OVr8NL
- Kim JY, Kim NK, Lee KY, Hur H, Min BS, et al. (2012) A comparative study of voiding and sexual function after total mesorectal excision with autonomic nerve preservation for rectal cancer: laparoscopic versus robotic surgery. Ann Surg Oncol 19: 2485-2493. Link: https://goo.gl/VvQhzx
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
