Annals of Psychiatry and Treatment
A mixed-methods study protocol on the psychosocial health of stroke survivors and their informal carers (CARESS): experiences, needs and quality of life
Ana Moura1,2#, Filipa Teixeira1#, Conceição Nogueira3, Ana Henriques1, Cláudia de Freitas1,4,5 and Elisabete Alves6,7*
2Centre for Research and Intervention in Education (CIIE), Faculty of Psychology and Education Sciences, University of Porto, Porto, Portugal
3Center for Psychology at the University of Porto, Faculty of Psychology and Educational Sciences of the University of Porto, Porto, Portugal
4Department of Public Health and Forensic Sciences and Medical Education, Faculty of Medicine, University of Porto, Porto, Portugal
5Centre for Research and Studies in Sociology (CIES-IUL), University Institute of Lisbon (ISCTE-IUL), Lisbon, Portugal
6Nursing Department, University of Évora, Évora, Portugal
7Comprehensive Health Research Center (CHRC), University of Évora, 7000-801, Évora, Portugal
#These authors contributed equally to this work
Cite this as
Moura A, Teixeira F, Nogueira C, Henriques A, Freitas CD, et al. (2023) A mixed-methods study protocol on the psychosocial health of stroke survivors and their informal carers (CARESS): experiences, needs and quality of life. Ann Psychiatry Treatm 7(1): 010-017. DOI: 10.17352/apt.000048Copyright
© 2023 Moura A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Introduction: Surviving a stroke and caring for a survivor, impacts individuals’ psychological health and quality of life, which may impose substantial costs on healthcare and social systems. This study aims to understand and explore the psychological health, experiences, needs and quality of life of Portuguese stroke survivors and their informal carers.
Methods and analysis: This is a mixed-methods, observational study. The methodological strategy relies on 1) scoping review; 2) questionnaires to stroke survivors hospitalized between September 2018 and August 2019 in one of the 12 Stroke Units of the Northern Region Health Administration of Portugal and their informal carers, 18-24 months after the event (1775 survivors and 443 carers); and 3) semi-structured interviews to a subsample of stroke survivors (n = 49) and informal carers (n = 37); and 4) think tanks with stakeholders involved in the stroke rehabilitation process, namely stroke survivors, informal carers, researchers, and health and social professionals (n = 45). Descriptive and inferential statistics will be used to analyze the quantitative data, and content and interpretational analysis will be implemented to assess qualitative data.
Ethics and dissemination: The study protocol was approved by the Ethics Committees of all the hospitals involved. The expected dissemination actions are effective tools in designing strategies that aim to promote knowledge on a needs-driven, socioethical sensitive basis, which will contribute to the implementation of a model of coproduction of health in the context of post-stroke care.
Strengths and limitations of this study
- This mixed-methods project will fill methodological and theoretical gaps in the field of stroke survival and informal care.
- Based on a robust design, this study will understand and explore the medium and long-term psychological health, experiences, needs, and quality of life of a large sample of stroke survivors and informal carers.
- All the Stroke Units of the Northern Region Health Administration of Portugal (ARS-Norte) accepted to participate in the study, ensuring regional variability and representativeness of the sample.
- A selection bias is inherent to this project since the study design hampers the involvement of stroke survivors who are institutionalized, with formal carers, and with language and/or cognitive disorders.
Abbreviations
ARS-Norte: Northern Region Health Administration of Portugal
Introduction
Stroke is a major health burden worldwide and one of the leading causes of disability and mortality in industrialized countries [1-3]. In Portugal, stroke accounts for approximately 10% of the overall deaths, affecting mostly women (11.6% vs 8.9% among men) [4]. Although mortality due to stroke declined by 4% between 2008 and 2018 [5], these positive improvements have led to increased survival among stroke patients [2,3].
The significant burden of stroke extends across individuals, families, and health and social systems globally, with the majority of stroke survivors requiring the assistance of a carer who must adjust to the sudden and long-term stroke effects that require varying degrees of caregiving [6,7]. Research indicates that caring for a stroke survivor has a significant and negative impact on carers’ psychological health and quality of life [8-10], which may also impose substantial costs on healthcare and social systems. However, the majority of the studies, rarely developed with mixed-methods designs, have focused on the physical and emotional consequences of stroke, to the detriment of survivors’ and carers’ mental health and well-being [11,12], the burden in the early poststroke period [9,13-16], and on the provision of information regarding stroke survivor rehabilitation [17]. These studies have used knowledge transfer approaches mainly based on the perspectives of healthcare professionals [18,19]. Furthermore, the research carried out has not yet developed intervention strategies that are sensitive and address the needs of survivors and caregivers, especially due to the lack of methodological robustness and significant results [20,21].
Recognizing that survivors’ and informal carers’ support needs change across the care continuum [22], there is a need to develop studies that analyze the medium- and long-term impact of stroke on survivors’ and carers’ psychological health, namely depressive and anxiety symptoms. Clarifying the specific timing of survivors’ and carers’ experiences and needs permits the development of timely sensitive education and support interventions [22]. Additionally, understanding the implications of gender inequalities on survivors’ and carers’ experiences and psychosocial health, can establish effective ways to screen for groups at risk, and design and implement support interventions that address survivors’ and carers’ needs. Finally, to better explore the impact of the caregiving role on carers’ psychosocial health and defining effective supportive strategies is central to exploring the coping strategies enacted by carers to deal with this event. These research needs are particularly relevant in Portugal, where non-communicable diseases and informal care are gaining more prominence, while research, guidelines, and recommendations regarding the needs and psychosocial health of stroke survivors and carers are still lacking.
Therefore, considering the gaps identified in the literature and the Portuguese context, the mixed-methods project was designed to deeply understand the psychological health, experiences, needs, and quality of life of Portuguese stroke survivors and their informal carers, in the medium and long-term. The specific objectives are:
- To assess the psychological profile, namely, depressive and anxiety symptoms of stroke survivors and their informal carers as well as their burden and quality of life, according to socioeconomic characteristics, the care trajectory and the survivor’s health status.
- To explore the gender-specific needs of information, support, and assistance among stroke survivors and their informal carers according to socioeconomic characteristics, the time of caregiving, and the stroke survivor’s health status.
- To identify the facilitators and barriers related to health and social services availability and access, taking into account the perspectives of stroke survivors and their informal carers.
- To explore stroke survivors’ and informal carers’ perceptions of social support and quality of life by integrating quantitative and qualitative data.
- To develop knowledge and devise strategies aimed at enhancing integrated people-centered care regarding informal carers’ support and well-being, with special attention given to the challenges and needs experienced by carers of stroke survivors at medical and social levels and the strategies used to overcome them.
Methods and analysis
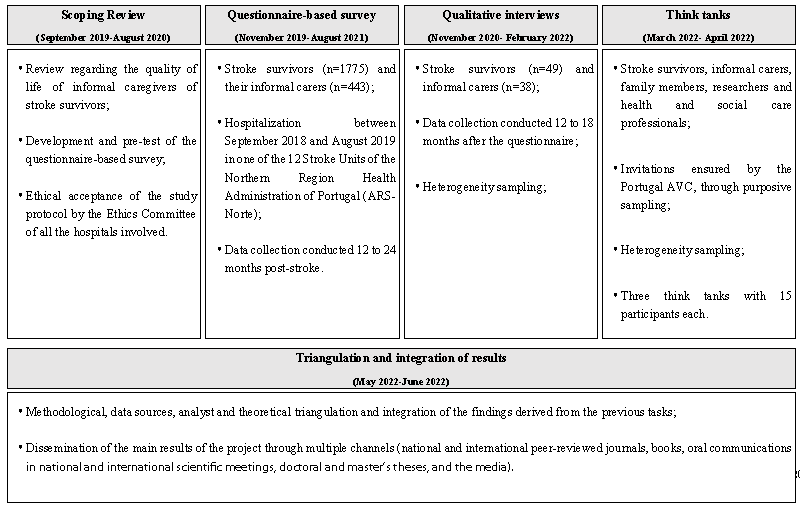
This mixed-methods, observational study will be a five-stage project conducted over 42 months (Figure 1). The study will achieve its objectives through multiple tasks, resulting in different activities and using different methods:
Scoping review
A scoping review was performed to assess the available evidence regarding the quality of life (QoL) of informal caregivers of stroke survivors, by identifying the instruments used to assess QoL and its associated characteristics, between September 2019 and August 2020. Following the Preferred Reporting Items for Systematic reviews and Meta-Analysis extension for Scoping Reviews (PRISMA-ScR) guidelines [23], the electronic databases PubMed, ISI WoK, PsycINFO, and Scielo were searched for empirical, peer-reviewed, original, and full-length studies on the characteristics influencing the QoL of informal caregivers of stroke survivors. The following search expression was used: (((adaptation) OR (transition) OR (management) OR (rehabilitation) OR (education) OR (learning) OR (training)) AND ((stroke) OR (brain vascular accident) OR (cerebrovascular accident) OR (post-stroke) OR (post-stroke) OR (poststroke) OR (transitional care) OR (discharge planning) OR (care-coordination) OR (continuity of care) OR (long-term care) OR (follow-up after discharge)) AND ((survivor*)) AND ((caregiver*) OR (informal caregiver*) OR (carer*) OR (primary caregiver*) OR (caregiving) OR (family caregiver*) OR (spouse caregiver*))). Eligibility and data extraction were conducted by two independent researchers. The main quantitative findings were synthesized, and qualitative data were explored by thematic content analysis.
During the development of the scoping review, existing questionnaires related to the psychosocial health and needs of stroke survivors and their informal carers were collected, and our own questionnaire was developed and pre-tested. The pre-test of the questionnaire was conducted with 20 stroke survivors and their informal carers who were able to understand the items easily, requiring an average of 30 minutes each to fill out the questionnaire.
During this period, ethical evaluation and data protection authorization was obtained from the Ethics Committees and the respective Data Protection Offices of the 12 hospitals included in the study.
Questionnaire-based survey
Between November 2019 and August 2021, all stroke survivors hospitalized between September 2018 and August 2019 in one of the 12 Stroke Units of the Northern Region Health Administration of Portugal (ARS-Norte) and their informal carers (unpaid individuals who care for people who need help taking care of themselves) are invited to participate in the study. Only stroke survivors and their respective carers, if any, with available telephone contact and who agreed to be contacted by the research team were considered eligible to participate in the study. Stroke survivors who were institutionalized, with formal carers or living in foster families, who do not understand or speak Portuguese, or who have language and/or cognitive disorders (e.g., dysphasia, dementia, memory loss, deafness/hearing loss) and inmates were excluded.
Participants were first approached by the stroke medical team asking for their permission to be contacted by the research team. After acceptance, participants were invited to participate in the study, and a meeting is scheduled according to the participants’ availability and convenience to conduct the data collection. In accordance with the health status of the stroke survivor, three options are foreseen for data collection: 1) if the survivor does not have an informal carer (autonomous stroke survivors), the questionnaire was carried out by telephone on a day and time scheduled accordingly with the convenience of the participant; 2) if the survivor has an informal carer, both were invited to respond, preferably face-to-face, to a questionnaire each at a place and date scheduled according to the convenience of the two participants; 3) if the survivor has an informal carer but is unable to answer the questionnaire, the carer was asked to answer some questions related to the survivor as well as the carer role, preferably face-to-face, according to the participant’s preference.
Of the 2170 eligible stroke survivors invited, 1775 agreed to participate by completing a questionnaire (participation rate of 81.8%). Thus, a total of 1332 survivors without an informal carer and 443 pairs of survivors and carers (886 subjects) were enrolled. The main reasons for participation refusal were lack of time, lack of interest in the study, and psychological unavailability. Slight more than half of the stroke survivors (54.8%) were men and their mean (SD) age was 68.6 (13.9) years. A high proportion (65.1%) were married or lived with a partner and 66.5% reported less than 5 years of formal education. Approximately 35% of the stroke survivors had a household income lower than 1000€, while almost 45% did not know or preferred not to answer the question. This was the first stroke for more than 78.4% of the participants, with less than 15% reporting the absence of any impairments due to stroke. Concerning the informal carers, almost 90% were women (87.4%) and their mean (SD) age was 57.5 (12.6) years. More than three-quarters of the carers were married or lived with a partner (80.1%), and 42.6% had four or fewer years of education. Nearly 55% described a household income lower than 1000€/month and 48.1% considered living in an urban area.
Regarding the questionnaire, specific questions were produced, and previously validated instruments were selected according to the purposes of the study and based on recent literature to gather information about stroke survivors and their carers. The questionnaire directed to autonomous stroke survivors assesses data regarding sociodemographic characteristics, lifestyle changes, return to work, stroke impact [24], functional independence and disability [25,26], community integration [27,28], and stroke survivors’ quality of life [29]. The informal carers’ questionnaire explores the following dimensions: sociodemographic characteristics, lifestyle changes, health knowledge, and information sources, access to health and social services, psychological profile (depression and anxiety symptoms) [30], burden [31], social support [32], and quality of life [33] (Table 1). Clinical records were collected, namely, date and type of stroke, duration of hospitalization, and destination after discharge. This information is intended to obtain accurate data that allow reliable characterization of stroke episodes. Questionnaires were administered by researchers trained specifically for this task.
Statistical analysis will be performed using STATA 15.1 (College Station, TX, 2009). Data will be described as counts and proportions for categorical variables and means and standard deviations for normally distributed continuous variables. According to the specific objectives established, different analytic approaches will be considered. Means will be compared with the student’s t or Mann-Whitney tests as appropriate. For categorical variables, differences in frequencies and proportions will be assessed using the X2 test or Fisher’s exact test. The associations between the socioeconomic characteristics, the care trajectory, and the survivor’s health status with the psychological profile (depressive and anxiety symptoms, burden, and quality of life) of both stroke survivors and their informal carers will be estimated by crude and adjusted by odds ratios (OR) and respective 95% CI using logistic regression.
Qualitative interviews
At the time of questionnaire filling, participants were asked for written authorization and consent to provide telephone contact for later scheduling of semi-structured interviews. Thus, a sub-sample of the stroke survivors and informal carers that participated in the quantitative study were contacted, approximately 12 to 18 months later (November 2020 to February 2022). These interviews enable researchers to pursue deeper insight into the views and experiences of stroke survivors and their informal carers regarding integrated people-centered care and the development of a model of co-organization of care.
Interviews were held by telephone and at participants’ homes and were digitally recorded after informed consent. In order to obtain a maximum variation of views and experiences and heterogeneity sampling participants’ recruitment ceased when data saturation was reached (when no new, significant data emerged from the interviews) [34].
Among the participants invited to participate in the semi-structured interviews. Stroke survivors who were at that time institutionalized (n = 4) or died (n = 3) and previous informal carers who were no longer informal carers (n = 2) were excluded. Thus, 57 stroke survivors and 48 informal carers were invited to attend the interview. Among those, 8 survivors and 10 carers refused to be interviewed by lack of time (n = 3 and n = 5, respectively), psychological unavailability (n = 2 and n = 4, respectively), and lack of interest in the study (n = 3 and n = 1, respectively). The final sample included 49 stroke survivors (25 females and 24 males) and 37 informal carers (24 females and 13 males). Interviews with stroke survivors and carers were conducted telephonically (n = 46 and n = 20, respectively) and face-to-face at participants’ homes (n = 3 and n = 18, respectively). Informal carers were spouses (n = 20), offspring (n = 12), sons-in-law/daughters-in-law (n = 3), grandchildren (n = 1), and siblings (n = 1). Interview duration with stroke survivors ranged from 6 to 61 min (mean: 17 minutes) and between 15 and 98 minutes (mean: 44 minutes) among informal carers.
The interview guide was developed based on an extensive review of the literature and on the main results of the quantitative data. The interview guide covered six main issues: 1) adaptation after stroke; 2) challenges and needs experienced by stroke survivors and informal carers, as well as strategies used to overcome them; 3) social support and availability of health and services; 4) policies surrounding stroke survival and informal care and their rights; 5) impact of COVID-19 pandemic; and 6) work reintegration.
Interviewing and analysis will be carried out by two hired researchers to guarantee consistent training and quality assurance.
Future tasks will be the verbatim transcription of the audio-digital files, which will be validated for accuracy and precision, and respective qualitative analysis. A qualitative content analysis and a hermeneutic analysis will be carried out, to allow a more consistent, rigorous, and deeper analysis and discussion. Qualitative content analysis is a method for systematically describing meanings of qualitative data through coding and categorization and has features description and interpretation of material [35]. Hermeneutic analysis is the process of interpreting and understanding a text in a “circular movement” involving subjective and objective approaches [35]. The use of both approaches permits the systematization, coding, categorization, interpretation, understanding of meanings and reflection of the interviews. Content analysis will be performed using NVivo 12 (QSR International, USA, 2018). Hermeneutic analysis of transcripts, using constant comparison and category-building procedures, will be conducted by two independent researchers to identify major themes. Then, data will be classified by dimensions within each theme. Disagreements in abstractions will be discussed with a third researcher and resolved by consensus. Finally, the most elucidative expressions of the meanings, views, and experiences emerging from the narratives will be selected.
Think tanks
Between March and April 2022, a qualitative study was undertaken by deploying think tanks with stakeholders involved in the stroke rehabilitation process. Think tanks are a form of group interview particularly suitable to inquire and elicit debate on previously defined topics among heterogeneous stakeholder groups [36].
Heterogeneity sampling was used first to assure maximum variation of experiences and perspectives based on gender and type of connection to stroke (stroke survivors, informal carers, family members, researchers, and health and social care professionals). Participants’ invitations were ensured by the Portuguese Association of Stroke Survivors, Family Members, and Friends - Portugal AVC, which was responsible for the participants’ selection through purposive sampling. Subsequently, participants were randomly assigned to a think tank. A total of fifteen participants were included per think tank and data saturation was reached with three think tanks [37].
The think tanks focused on the challenges and needs experienced by informal carers of stroke survivors and on the strategies that can be used to overcome them. The discussion was led by a post-doc researcher, who was the moderator, together with a Ph.D. researcher, who summarized the main discussion topics at the end of each think tank. The discussion was elicited based on a brief presentation reporting the findings of the questionnaires and the interviews. Participants were given the opportunity to comment on think tank summaries and to make final observations.
After verbatim transcription and validation, rigor and precision data will be analyzed with NVivo 12 (QSR International, USA, 2018) by employing inductive and deductive approaches to interpretational analysis.
Triangulation and integration of results
Since this project relies in different research methodologies, sources, and theoretical perspectives, which will result in different but complementary results, the development of triangulation and integration strategies will be an added value. These approaches will permit not only the guarantee of rigor and quality of research but also the validity of conclusions and will be implemented between May and June 2022.
Thus, four types of triangulation will be used, namely, methodological triangulation, data sources triangulation, analyst triangulation, and theoretical triangulation. Scientific mixed-methods and multi-methods articles will be useful tools to integrate the results. Through the analysis (quantitative and qualitative), reflection, and discussion of the distinct results, an interaction and “conversation” between findings will be made.
Patient and public involvement
Drawing on robust methodological and theoretical approaches, this project actively involved survivors and carers, as well as lay and professional stakeholders, across different stages of the study design. They were specifically invited to participate in the questionnaire and interview designs and will be included in the dissemination of the results through participation in public meetings and science promotion events. This project has also previously been discussed with health professionals from the Portuguese Association of Stroke Survivors, Family Members, and Friends - Portugal AVC. It is expected that the engagement of participants towards responsible and innovative research will promote results that are sensitive to different realities and, therefore, enhance empirically grounded recommendations and integrated people-centered care.
This project was consciously designed to further improve the quality, efficiency, and cost-effectiveness of health and social services, as well as to generate and disseminate knowledge on a needs-driven, socio-ethical sensitive basis, which will contribute to the implementation of a model of co-production of health.
Ethics and dissemination
The study protocol was approved by the Ethics Committees and the respective Data Protection Offices of all 12 Stroke Units of the Northern Region Health Administration of Portugal. Data collection in each Stroke Unit was only initiated after obtaining ethical approval from its respective Ethics Committee. In accordance with the General Data Protection Regulation, a set of procedures will be taken into account to comply with the requirements of the European Regulation regarding scientific research and the protection of personal data.
Informed consent will be obtained from all participants at the three moments of data collection, after clarification of any arising doubts. The researchers will provide clear, transparent, and detailed information (orally and written on an information sheet) about the following: research objectives, name, and institution of researchers, voluntary nature of participation, expected duration of the questionnaire/interview/think tank, reasons for audio recording, procedures taken to protect personal data, participants’ entitlement to obtain additional information and clarification on any aspect related to the study and the option to be informed about the results of the study, guarantee of the possibility to withdraw from the study at any time without consequences, and data retention period. Informed consent to access and analyze personal and clinical data will also be requested.
Confidentiality, anonymity, and data protection will be guaranteed. A unique code will be assigned to each questionnaire, interview, and transcript of the content of the think tanks. To protect their personal data, participants will not be asked for their full birth date, ethnicity/race, address/residence, religion, or other “sensitive” data. Additionally, the following actions will be taken: data collection will be carried out in private places; a specific database will be created and intended only for research purposes to which only the research team will have access; the data recorded in audio will be transcribed and stored in secure computer files, and any data likely to identify the participants will be deleted/replaced; all materials, in physical and digital format, will be stored in locked file cabinets and/or on a computer with restricted access and with a password; after transcribing the interviews and think tanks, the audio files will be destroyed within three months; at the end of data collection, the telephone contact requested initially will be dissociated from the participant’s code, contributing to greater data anonymization; and all databases properly stored and password protected will be preserved until all relevant data are published in scientific journals or up to a maximum period of five years after the last publication for data review purposes. All researchers will be closely supervised by the research leader, and they will be asked to sign a confidentiality agreement ensuring their commitment to confidentiality, privacy, and respect for participants’ rights.
The dissemination of the results of this study will be carried out through national and international peer-reviewed journals (especially those with higher impact factors), books, oral communications in national and international scientific meetings, doctoral and master’s theses, and national seminars, namely those related to caregiving, stroke survival, and public health. It will be chosen means of dissemination of various areas of knowledge (e.g., public health, health education, sociology), in order to improve the interdisciplinary sharing and discussion of results, increasing their scientific and social impact. The results dissemination will be targeted to practitioners, policymakers, and postgraduate students to debate the implications of stroke survivors’ and informal carers’ health and quality of life. Moreover, dissemination of the results among stroke survivors and informal carers will be accomplished through the organization of one science shop and by spreading the main results in the media.
Funding
This study is co-funded by national funding from the Foundation for Science and Technology – FCT (Portuguese Ministry of Science, Technology and Higher Education), the Regional Development Fund (ERDF), European Social Fund (ESF), Portugal 2020 and European Structural and Investment Funds, through the Regional Operational Programme Norte (Norte 2020), under the project POCI-01-0145-FEDER-031898; by the Operational Programme Competitiveness and Internationalization (COMPETE 2020), Portugal 2020, European Regional Development Fund, under the Unidade de Investigação em Epidemiologia - Instituto de Saúde Pública da Universidade do Porto (EPIUnit) (POCI-01-045-FEDER-016867; Ref. FCT UID/DTP/04750/2019); by the CIIE’s multi-annual FCT funding (UIDB/00167/2020 and UIDP/00167/2020); by the Ph.D. grand 2020.07312.BD (to AM); by the post-doc grant SFRH/BDP/103562/2014 (to EA), co-funded by the FCT and the POPH/FSE; by an individual contract grant DL57/2016/CP1336/CT0001 (to CDF); and by a Scientific Employment Stimulus contract CEECIND/01793/2017 (to AH).
Authors’ contributions
AM and FT contributed to the study conception and design and drafted the manuscript. CN, AH, and CDF contributed to the study conception and design and provided critical revisions. EA is the principal investigator, conceived the study, acquired funding for this project, and coordinated the manuscript. All authors read, reviewed, and approved the final manuscript.
Data statement section
Data will be available upon request.
- Katan M, Luft A. Global Burden of Stroke. Semin Neurol. 2018 Apr;38(2):208-211. doi: 10.1055/s-0038-1649503. Epub 2018 May 23. PMID: 29791947.
- GBD 2016 Neurology Collaborators. Global, regional, and national burden of neurological disorders, 1990-2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet Neurol. 2019 May;18(5):459-480. doi: 10.1016/S1474-4422(18)30499-X. Epub 2019 Mar 14. PMID: 30879893; PMCID: PMC6459001.
- Gorelick PB. The global burden of stroke: persistent and disabling. Lancet Neurol. 2019 May;18(5):417-418. doi: 10.1016/S1474-4422(19)30030-4. Epub 2019 Mar 11. PMID: 30871943.
- National Institute of Statistics. [Demographic statistics 2019]. Lisboa, 2019. https://www.ine.pt/xportal/xmain?xpid=INE&xpgid=ine_publicacoes&PUBLICACOESpub_boui=71882686&PUBLICACOESmodo=2.
- National Institute of Statistics. [Causes of death 2018]. Lisboa, 2019 https://www.ine.pt/xportal/xmain?xpid=INE&xpgid=ine_destaques&DESTAQUESdest_boui=399595079&DESTAQUESmodo=2.
- Long NX, Pinyopasakul W, Pongthavornkamol K, Panitrat R. Factors predicting the health status of caregivers of stroke survivors: A cross-sectional study. Nurs Health Sci. 2019 Jun;21(2):262-268. doi: 10.1111/nhs.12591. Epub 2019 Jan 7. PMID: 30618202.
- Zhang J, Lee DT. Meaning in stroke family caregiving: A literature review. Geriatr Nurs. 2017 Jan-Feb;38(1):48-56. doi: 10.1016/j.gerinurse.2016.07.005. Epub 2016 Sep 23. PMID: 27671537.
- Okoye EC, Okoro SC, Akosile CO, Onwuakagba IU, Ihegihu EY, Ihegihu CC. Informal caregivers' well-being and care recipients' quality of life and community reintegration - findings from a stroke survivor sample. Scand J Caring Sci. 2019 Sep;33(3):641-650. doi: 10.1111/scs.12657. Epub 2019 Feb 7. PMID: 30734330.
- Pucciarelli G, Ausili D, Galbussera AA, Rebora P, Savini S, Simeone S, Alvaro R, Vellone E. Quality of life, anxiety, depression and burden among stroke caregivers: A longitudinal, observational multicentre study. J Adv Nurs. 2018 Apr 27. doi: 10.1111/jan.13695. Epub ahead of print. PMID: 29700840.
- Sennfält S, Ullberg T. Informal caregivers in stroke: Life impact, support, and psychological well-being-A Swedish Stroke Register (Riksstroke) study. Int J Stroke. 2020 Feb;15(2):197-205. doi: 10.1177/1747493019858776. Epub 2019 Jun 25. PMID: 31237832.
- El Masry Y, Mullan B, Hackett M. Psychosocial experiences and needs of Australian caregivers of people with stroke: prognosis messages, caregiver resilience, and relationships. Top Stroke Rehabil. 2013 Jul-Aug;20(4):356-68. doi: 10.1310/tsr2004-356. PMID: 23893835.
- Lou S, Carstensen K, Jørgensen CR, Nielsen CP. Stroke patients' and informal carers' experiences with life after stroke: an overview of qualitative systematic reviews. Disabil Rehabil. 2017 Feb;39(3):301-313. doi: 10.3109/09638288.2016.1140836. Epub 2016 Feb 17. PMID: 26882958.
- Rigby H, Gubitz G, Phillips S. A systematic review of caregiver burden following stroke. Int J Stroke. 2009 Aug;4(4):285-92. doi: 10.1111/j.1747-4949.2009.00289.x. PMID: 19689757.
- Saban KL, Sherwood PR, DeVon HA, Hynes DM. Measures of psychological stress and physical health in family caregivers of stroke survivors: a literature review. J Neurosci Nurs. 2010 Jun;42(3):128-38. doi: 10.1097/jnn.0b013e3181d4a3ee. PMID: 20550072.
- McCurley JL, Funes CJ, Zale EL, Lin A, Jacobo M, Jacobs JM, Salgueiro D, Tehan T, Rosand J, Vranceanu AM. Preventing Chronic Emotional Distress in Stroke Survivors and Their Informal Caregivers. Neurocrit Care. 2019 Jun;30(3):581-589. doi: 10.1007/s12028-018-0641-6. PMID: 30421266; PMCID: PMC6958510.
- Tsai YH, Lou MF, Feng TH, Chu TL, Chen YJ, Liu HE. Mediating effects of burden on quality of life for caregivers of first-time stroke patients discharged from the hospital within one year. BMC Neurol. 2018 Apr 25;18(1):50. doi: 10.1186/s12883-018-1057-9. PMID: 29699521; PMCID: PMC5921300.
- Hafsteinsdóttir TB, Vergunst M, Lindeman E, Schuurmans M. Educational needs of patients with a stroke and their caregivers: a systematic review of the literature. Patient Educ Couns. 2011 Oct;85(1):14-25. doi: 10.1016/j.pec.2010.07.046. Epub 2010 Sep 23. PMID: 20869189.
- Singh M, Hynie M, Rivera T, Macisaac L, Gladman A, Cheng A. An evaluation study of the implementation of stroke best practice guidelines using a Knowledge Transfer Team approach. Can J Neurosci Nurs. 2015;37(1):24-33. PMID: 26152100.
- Denham AMJ, Wynne O, Baker AL, Spratt NJ, Turner A, Magin P, Janssen H, English C, Loh M, Bonevski B. "This is our life now. Our new normal": A qualitative study of the unmet needs of carers of stroke survivors. PLoS One. 2019 May 8;14(5):e0216682. doi: 10.1371/journal.pone.0216682. PMID: 31067286; PMCID: PMC6505885.
- Legg LA, Quinn TJ, Mahmood F, Weir CJ, Tierney J, Stott DJ, Smith LN, Langhorne P. Non-pharmacological interventions for caregivers of stroke survivors. Cochrane Database Syst Rev. 2011 Oct 5;(10):CD008179. doi: 10.1002/14651858.CD008179.pub2. PMID: 21975778.
- Crocker TF, Brown L, Lam N, Wray F, Knapp P, Forster A. Information provision for stroke survivors and their carers. Cochrane Database Syst Rev. 2021 Nov 23;11(11):CD001919. doi: 10.1002/14651858.CD001919.pub4. PMID: 34813082; PMCID: PMC8610078.
- Cameron JI, Gignac MA. "Timing It Right": a conceptual framework for addressing the support needs of family caregivers to stroke survivors from the hospital to the home. Patient Educ Couns. 2008 Mar;70(3):305-14. doi: 10.1016/j.pec.2007.10.020. Epub 2007 Dec 21. PMID: 18155388.
- Tricco AC, Lillie E, Zarin W, O'Brien KK, Colquhoun H, Levac D, Moher D, Peters MDJ, Horsley T, Weeks L, Hempel S, Akl EA, Chang C, McGowan J, Stewart L, Hartling L, Aldcroft A, Wilson MG, Garritty C, Lewin S, Godfrey CM, Macdonald MT, Langlois EV, Soares-Weiser K, Moriarty J, Clifford T, Tunçalp Ö, Straus SE. PRISMA Extension for Scoping Reviews (PRISMA-ScR): Checklist and Explanation. Ann Intern Med. 2018 Oct 2;169(7):467-473. doi: 10.7326/M18-0850. Epub 2018 Sep 4. PMID: 30178033.
- Philp I, Brainin M, Walker MF, Ward AB, Gillard P, Shields AL, Norrving B; Global Stroke Community Advisory Panel. Development of a poststroke checklist to standardize follow-up care for stroke survivors. J Stroke Cerebrovasc Dis. 2013 Oct;22(7):e173-80. doi: 10.1016/j.jstrokecerebrovasdis.2012.10.016. Epub 2012 Dec 21. PMID: 23265778.
- Farrell B, Godwin J, Richards S, Warlow C. The United Kingdom transient ischaemic attack (UK-TIA) aspirin trial: final results. J Neurol Neurosurg Psychiatry. 1991 Dec;54(12):1044-54. doi: 10.1136/jnnp.54.12.1044. PMID: 1783914; PMCID: PMC1014676.
- Araújo F, Pais-Ribeiro J, Oliveira A, Pinto C. Validation of the Barthel Index in a sample of non-institutionalized elderly. Rev Port Saúde Pública. 2007; 25(2):59-66.
- Fraga-Maia HM, Werneck G, Dourado I, Fernandes Rde C, Brito LL. Translation, adaptation and validation of "Community Integration Questionnaire". Cien Saude Colet. 2015 May;20(5):1341-52. English, Portuguese. doi: 10.1590/1413-81232015205.08312014. PMID: 26017937.
- Willer B, Ottenbacher K, Coad M. Community Integration Questionaire: a comparative examination. Am J Phys Med Rehabil. 1994; 73:103–11.
- Malheiro A, Nicola A, Pereira C. Contribution to the adaptation and validation of the Quality of Life Assessment Scale for Patients after Stroke. EssFisiOnline. 2005; 5(2):12-24.
- Pais-Ribeiro J, Silva I, Ferreira T, Martins A, Meneses R, Baltar M. Validation study of a Portuguese version of the Hospital Anxiety and Depression Scale. Psychol Health Med. 2007 Mar;12(2):225-35; quiz 235-7. English, Portuguese. doi: 10.1080/13548500500524088. PMID: 17365902.
- Sequeira C. Adaptation and validation of the Zarit Caregiver Burden Scale. Referência. 2010; 2(12):9-16.
- Carvalho S, Pinto-Gouveia J, Pimentel P, Maia D, Mota-Pereira J. Psychometric characteristics of the Portuguese version of the Multidimensional Scale of Perceived Social Support (MSPSS). Psychologica . 2011; 54:309–58.
- Joseph S, Becker S, Elwick H, Silburn R. Adult carers quality of life questionnaire (AC-QoL): Development of an evidence-based tool. Ment Heal Rev J. 2012; 17(2):57-69.
- Guest G, Bunce A, Johnson L. How many interviews are enough? An experiment with data saturation and variability. Field Methods. 2006; 18(1):59–82.
- Vieira KAL, de Quiroz GM. Hermeneutic Content Analysis: a method of textual analysis. IJBMM. 2017; 2(8):8-15.
- Viseu S, Carvalho LM. Think tanks, policy networks and education governance: The rising of new intra-national spaces of policy in Portugal. Educ Policy Anal Arch. 2018; 26(108):1-26.
- de Freitas C, Dos Reis V, Silva S, Videira PA, Morava E, Jaeken J. Public and patient involvement in needs assessment and social innovation: a people-centred approach to care and research for congenital disorders of glycosylation. BMC Health Serv Res. 2017 Sep 26;17(1):682. doi: 10.1186/s12913-017-2625-1. PMID: 28950866; PMCID: PMC5615629.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
