Archives of Pulmonology and Respiratory Care
Normal left pulmonary inferior lobe in abnormal systemic circulation arterial supply
Weiqiang Yan1, Zhidong Yuan1, Musen Ye1,2, Sijia Zuo1,2 and Guanxun Cheng1*
2Shenzhen University Health Science Centre, Shenzhen 518061, P. R.China
Guanxun Cheng, Department of Radiology, Peking University Shenzhen Hospital, Shenzhen, 518061, P. R. China, Tel:+(086)-13925200816, E-mail: 18903015678@189.cn
Cite this as
Yan W, Yuan Z, Ye M, Zuo S, Cheng G (2022) Normal left pulmonary inferior lobe in abnormal systemic circulation arterial supply. Arch Pulmonol Respir Care 8(1): 020-022. DOI: 10.17352/aprc.000079Copyright License
© 2022 Yan W, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Normal left pulmonary inferior lobe in abnormal systemic circulation arterial supply without sequestration is a rare malformation of congenital lung vascular. Multi-Detector Computed Tomography (MDCT) and it’s Three-Dimensional (3D) reconstruction can display clearly the signs of the abnormal systemic circulation arterial supply to the lung lobe and the imaging changes of the left pulmonary inferior lobe associated with this disorder, it can provide detailed information for the clinician to make the treatment planning.
Introduction
The Abnormal Systemic Circulation Artery (ASCA) supply to the left pulmonary inferior lobe is a rare congenital pulmonary anomaly vascular, which is characterized by an aberrant artery branch originating from the descending aorta that supplies the basal segment of the left pulmonary inferior lobe [1-3]. The average age was about 32 years old when this disorder is discovered, most of the patients with this disorder may consult with a cough, and approximately 40% of cases may accompany bloody sputum [4]. Herein, we introduce a young man who confirmed the ASCA supply to the left pulmonary inferior lobe by multi-detector computed tomography (MDCT) and show its imaging manifestations.
Case presentation
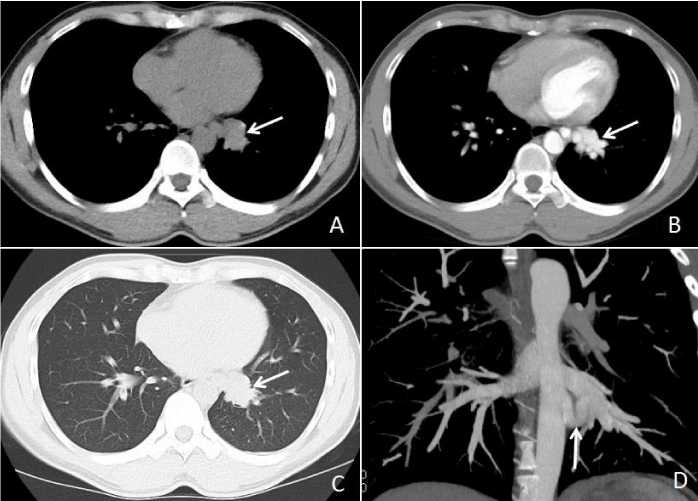
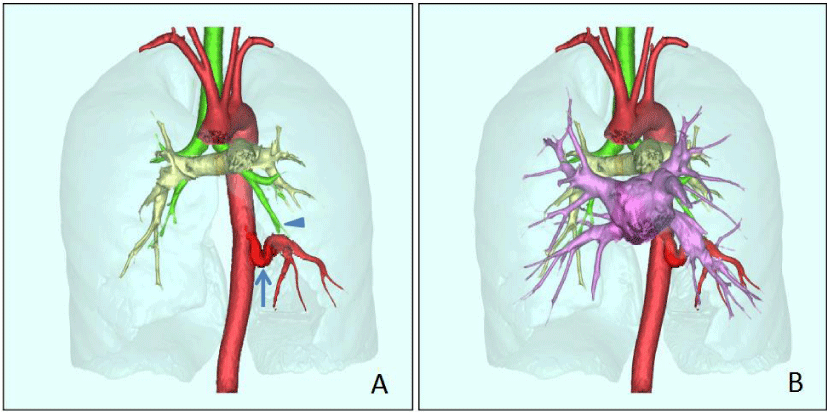
A 28-year-old male patient presented with an episode of cough with little phlegm for more than one month, he denied any history of chest trauma and previous lung diseases, and the laboratory tests were all normal. The chest DR suspected a small nodule in the heart overlapping area of the left lower lung field. Non-enhanced MDCT showed a paramediastinal soft tissue density nodule in the left lower lung (Figure 1A), the contrast-enhanced MDCT demonstrated the “nodule” was clustered vascular (Figure 1B), the axial lung window image revealed transparency of the left lower lung was normal and the opacity paramediastinal nodule in the left lower lung shown simultaneously (Figure 1C), the coronal reconstructed image demonstrated the ASCA supplying the basal segment of left pulmonary inferior lobe (Figure 1D); MDCT three-dimensional (3D) reconstructed imaging depicted the ASCA and normal left lower lobe bronchus (Figure 2A), the merged imaging showed the relationship of ASCA, left lower lobe bronchus, as well as pulmonary artery and vein (Figure 2B). Based on our hospital policy, the Institutional Review Board of the Ethics Committee of Peking University Shenzhen Hospital approved this retrospective report and waived the requirement for informed consent.
Discussion
Although the ASCA supply to the left pulmonary inferior lobe can be considered as a type of pulmonary sequestration according to Pryce’s classification, unlike the typical sequestration, the left lower lobe bronchus and the transparency of the left pulmonary inferior lobe maintain normal in this disorder, there is no sequestration of the pulmonary parenchyma and the left pulmonary inferior lobe basal segment artery is absent in cases of ASCA. As the pathological basis of this disorder describe above, whether ASCA supply to the left pulmonary inferior lobe is different from pulmonary sequestration and its appropriate name is still disputed [2,3].
Unlike lung sequestration with common symptoms of recurrent pneumonia accompanied by cough and expectoration, the main symptom of ASCA supply to the left pulmonary inferior lobe is hemoptysis, this is because most of the ASCA originate from the descending aorta, which increased the pressure both in the pulmonary capillaries and pulmonary veins, then excessive pressure causing vessel rupture to lead to intra-alveolar hemorrhage [4] and admitted with cough and blood in the phlegm [5-7]. When the pressure of pulmonary capillaries and pulmonary veins is within the safe range, the patient can remain with no bloody phlegm just like the case in this article.
Both digital subtraction angiography (DSA) and MDCT angiography allow us to accurately evaluate the ASCA, as the non-invasive, flexible, and 3D reconstruction images of MDCT angiography, it is widely used in routine to detect vascular diseases. As for ASCA, the contrast-enhanced MDCT can depict the ASCA and evaluate the intrapulmonary state at the same time [5-8], by axial imaging, we can find this disorder as opacity paramediastinal nodular or clustered vascular imaging in pre- or post-contrast enhancement respectively. Maximal Intensity Projection (MIP), Multiplanar Reconstruction (MPR) and Volume Rendering (VR) are common methods of 3D reconstruction for MDCT angiography, with a combination of MPR and MIP can display the details of ASCA, descending aorta and left inferior pulmonary vein, with VR reconstruction, the relationship between the ASCA, the descending aorta, pulmonary vein and left lower lobe bronchus can be revealed clearly, the merged VR images combination of the color marker can provide more vivid and intuitive images for ASCA supply to left pulmonary inferior lobe.
Interventional embolization and surgical treatment are the two main treatment methods for ASCA supply to the left pulmonary inferior lobe as described in previous literature, the surgical treatment has progressed from lobectomy by thoracotomy to thoracoscopic lobectomy, anatomical segment resection [9-15]. No matter what method, accurate preoperative assessment of ASCA and its relationship between the descending aorta and pulmonary vessels is the key step to successful treatment.
Considering these advantages of MDCT, we recommend it as the prior method for evaluating the ASCA supply to the left pulmonary inferior lobe. Using 3D reconstruction and colorful markers, the vessels, bronchi, and lung segments can be merged into a colorful 3D image [8], it can provide detailed and clear anatomical structure images for the clinician to understand the vascular malformation of ASCA and make an appropriate treatment plan.
Conclusion
The condition of ASCA supply to the left pulmonary inferior lobe is rare, MDCT three-dimensional reconstruction is the important method for the diagnosis of this disorder, with the merged images of MDCT three-dimensional reconstruction, the ASCA, bronchus and lung segments can be revealed perfectly, relevant imaging information can help clinicians to make reasonable treatment plans for ASCA supply to left pulmonary inferior lobe.
This work was funded by the Shenzhen Science and Technology Program(JCYJ20220531093604009); Peking University Health Science Center Medical Education Research Funding Project (2019YB17); Project of Teaching Base of Department of Education of Guangdong Province(2019JD105); Education and Teaching Project of Peking University Shenzhen Hospital(JX202005).
- Le TB, Huyen TNHH, Ngo DHA, Le MT, Nguyen VP, Nguyen TT, Le TK. Isolated arterial pulmonary malinosculation without sequestration in an adult: A case report and literature review. Respir Med Case Rep. 2021 Sep 10;34:101514. doi: 10.1016/j.rmcr.2021.101514. PMID: 34540582; PMCID: PMC8441071.
- Giannotta M, Leone MB, Greco L, Baldazzi M, Zompatori M. Intralobar pulmonary sequestration with bronchial atresia and a systemic artery feeding a normal contralateral lung. BJR Case Rep. 2015 Nov 12;2(1):20150176. doi: 10.1259/bjrcr.20150176. PMID: 30364365; PMCID: PMC6195924.
- Gonca C, Hamzayev E, Atasoy C, Enon S. Anomalous systemic arterial supply to normal basal segments of the left lung without sequestration. Eur J Cardiothorac Surg. 2015 Mar;47(3):578. doi: 10.1093/ejcts/ezu209. Epub 2014 May 22. PMID: 24855194.
- Higuchi M, Chida M, Muto A, Fukuhara M, Suzuki H, Gotoh M. Anomalous systemic arterial supply to the basal segments of the lung. Fukushima J Med Sci. 2013;59(2):93-6. doi: 10.5387/fms.59.93. PMID: 24500385.
- Ko SF, Ng SH, Lee TY, Wan YL, Lee CM, Hsieh MJ, Chen MC. Anomalous systemic arterialization to normal basal segments of the left lower lobe: helical CT and CTA findings. J Comput Assist Tomogr. 2000 Nov-Dec;24(6):971-6. doi: 10.1097/00004728-200011000-00026. PMID: 11105720.
- Kim TS, Lee KS, Im JG, Goo JM, Park JS, Kim JH. Systemic arterial supply to the normal basal segments of the left lower lobe: radiographic and CT findings in 11 patients. J Thorac Imaging. 2002 Jan;17(1):34-9. doi: 10.1097/00005382-200201000-00004. PMID: 11828210.
- Ashizawa K, Ishida Y, Matsunaga N, Otsuji H, Sakamoto I, Hayashi K. Anomalous systemic arterial supply to normal basal segments of left lower lobe: characteristic imaging findings. J Comput Assist Tomogr. 2001 Sep-Oct;25(5):764-9. doi: 10.1097/00004728-200109000-00016. PMID: 11584238.
- Hu B, Lan Y, Li Q, Yang X, Tian B, Qing H, Zhou P, Wang T, Yang X. Merged image reconstruction for anomalous systemic arterial supply to a normal lung. J Med Radiat Sci. 2020 Jun;67(2):151-154. doi: 10.1002/jmrs.383. Epub 2020 Mar 2. PMID: 32118356; PMCID: PMC7276187.
- Machida Y, Motono N, Matsui T, Usuda K, Uramoto H. Successful endovascular coil embolization in an elder and asymptomatic case of anomalous systemic arterial supply to the normal basal segment. Int J Surg Case Rep. 2017;34:103-105. doi: 10.1016/j.ijscr.2017.03.030. Epub 2017 Mar 22. PMID: 28376417; PMCID: PMC5379902.
- Jiang S, Yu D, Jie B. Transarterial Embolization of Anomalous Systemic Arterial Supply to Normal Basal Segments of the Lung. Cardiovasc Intervent Radiol. 2016 Sep;39(9):1256-65. doi: 10.1007/s00270-016-1361-y. Epub 2016 May 5. PMID: 27150806.
- Sugihara F, Murata S, Uchiyama F, Watari J, Tanaka E, Muraishi N, Satoh E, Kumita S. Transcatheter arterial embolization of anomalous systemic arterial supply to the basal segment of the lung. Acta Radiol Short Rep. 2013 Nov 26;2(7):2047981613511363. doi: 10.1177/2047981613511363. PMID: 24349714; PMCID: PMC3863966.
- Machida Y, Motono N, Matsui T, Usuda K, Uramoto H. Successful endovascular coil embolization in an elder and asymptomatic case of anomalous systemic arterial supply to the normal basal segment. Int J Surg Case Rep. 2017;34:103-105. doi: 10.1016/j.ijscr.2017.03.030. Epub 2017 Mar 22. PMID: 28376417; PMCID: PMC5379902.
- Kawaguchi T, Tojo T, Yasukawa M, Watanabe T, Kawai N, Taniguchi S. Surgical intervention without lung resection for Pryce type I sequestration. Asian Cardiovasc Thorac Ann. 2015 Sep;23(7):872-4. doi: 10.1177/0218492315574389. Epub 2015 Feb 20. PMID: 25700707.
- Ebihara M, Fujimori S, Suzuki S, Yotsumoto T, Kikunaga S, Ohtsuka R, Matsuyama S. Anomalous systemic arterial supply to the left basal lung with a calcified abnormal vessel: a case report. Surg Case Rep. 2022 Jun 22;8(1):121. doi: 10.1186/s40792-022-01469-8. PMID: 35729289; PMCID: PMC9213598.
- Utsumi T, Hino H, Kuwauchi S, Zempo N, Ishida K, Maru N, Matsui H, Taniguchi Y, Saito T, Tsuta K, Murakawa T. Anomalous systemic arterial supply to the basal segment of the lung with giant aberrant artery: a case report. Surg Case Rep. 2020 Nov 12;6(1):285. doi: 10.1186/s40792-020-01063-w. PMID: 33179205; PMCID: PMC7658289.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
