Archives of Pulmonology and Respiratory Care
Design a simulating lung in 36h or less
Jean Sébastien Buvat1, Laurent Faivre2, Pierre Romet3, Ludovic Vitu4, Julio Badie5, Fernando Daniel Berdaguer Ferrari5 and Sylvain Malfroy5*
2Nurse technical coordinator, Nord Franche Comté Hospital, Intensive Care Unit, 100 route de Moval, 90400 Trevenans, France
3CIAD UMR 7533,UNIV. Bourgogne Franche-Comté, UTBM, F-90010 Belfort, France
4ICB UMR 6303, CNRS, Univ. Bourgogne Franche-Comté, UTBM, F-90010 Belfort, France
5MD, Nord Franche Comté Hospital, Intensive Care Unit, 100 route de Moval, 90400 Trevenans, France
Cite this as
Buvat JS, Faivre L, Romet P, Vitu L, Badie J, et al. (2022) Design a simulating lung in 36h or less. Arch Pulmonol Respir Care 8(1): 012-015. DOI: 10.17352/aprc.000077Copyright License
© 2022 Buvat JS, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Background: During the COVID health crisis, intensive care units were quickly overwhelmed and had to call for help. The only solution was to call for this help among nurses, nursing auxiliaries, and physicians that were normally not working in the ICU units (consultations, operating room, medical units). These people needed mechanical ventilation courses before beginning their job in the ICU unit.
Simulation appeared to be the best solution because of its safety and educational effectiveness.
Approach: We developed an artificial lung during the 36 hours innovation marathon Crunch Maker Camp 2021. It included three main settings which were lung compliance, airways resistances, and diaphragmatic inspiratory trigger. These parameters seemed to be essential for us in order to simulate the mechanical ventilation characteristics of a COVID lung. The simulator was entirely made of physical components.
Evaluation: The team composed of engineers and intensive care medical instructors developed the first proof of concept of the artificial lung. The different controllable modules were able to adjust compliance, and resistance on the respirator, and an inspiratory trigger was efficient. They reflected correctly a normal or a COVID lung, simulating a patient on a ventilator.
The simulator was presented to the jury and after deliberation, the teams’ work was rewarded with the first innovation prize.
Reflection: We designed a controlled simulation for COVID respiratory issues; the artificial lung was rewarded during this innovation marathon Crunch Maker Camp 2021. This allowed us to improve the simulator and we plan to start using this tool during training sessions soon. We will then measure Pedagogic impact, focusing on long-term memorization.
Background
During the COVID crisis, patients affected by acute respiratory distress syndrome (ARDS) quickly overwhelmed intensive care units (ICU). In order to take care of these patients, specific preparedness is required [1] and temporary units were opened when necessary.
Even when beds and respirators were available, there was objectively a lack of qualified staff to care for these patients, so medical personnel from many other specialties arrived to support resuscitation teams. There was an urgent need to train these healthcare workers and simulators seemed to be the most suitable tool [2,3], but they were not always available especially those able to replicate mechanical ventilation. Dixon’s team tried the same experience in the field of trauma [3]. This article highlights the great value of simulation whatever the application is. Like them, we used new technology like 3D printing to develop our prototype.
Indeed, understanding the main concepts of mechanical ventilation such as compliance, resistance, inspiratory and expiratory triggers, asynchronies, and driving pressure is not easy but is really essential in order to apply safe protective lung strategies [4].
Patients’ lungs experiencing ARDS have some particularity like reduced lung compliance [5,6] or excessive bronchial secretions. The risk of barotrauma is high with complications like lung fibrosis or pneumothorax, which can lead to chronic respiratory insufficiency [7].
Physiopathology of COVID ARDS is often described in clinical trials but only a few teams studied the effectiveness of educational programs for reinforcement staff during the COVID crisis.
We imagined that a lung simulator that could visually reproduce a normal or a COVID lung would be a great educational tool for training unqualified staff. In fact, thanks to simulation tools, students can link theoretical concepts to practical skills and work as a team to resolve problems [8,9].
Currently, there are only a few lung simulation tools on the market (Table 1). Most of them only include a computer program distributed by respirator manufacturers. Hence, fields of application and educational interest are restrained. Our aim was to create a nonvirtual pedagogical lung so that learners can understand visually lung mechanics in the ARDS for example.
In order to solve this problem, a small team from the Hospital Nord Franche Comté’s intensive care unit asked the FabLab’s engineers of the Université de Technologie de Belfort Montbéliard to help in designing such a simulator.
Innovation marathon Crunch Maker Camp 2021 organized by the French engineering school Université de Technologie de Belfort Montbéliard took place in Belfort from June 4th until June 6th, the workshop focused on developing technical solutions for today’s medical problems. During the thirty-six hours event, we developed the first proof of concept artificial lung for mechanical ventilation training.
The aim of this article is to describe how we developed this inexpensive functional prototype able to simulate a ventilated lung.
Procedure
Some medical personnel of the Hospital Nord Franche Comté, Trevenans, France, participated in the Crunch Maker Camp event. Our team was composed of 3 medical professionals and 6 engineers. This challenge started with a medical formation about the mechanical ventilation and the outlining of specifications. Three main requirements were established: adaptable lung compliance, variable tracheal resistance, and the need for an inspiratory trigger. These three specifications were to be adjusted through computer software.
We started with a short medical presentation about normal lung function and the main abnormalities encountered in COVID patients. This first stage allowed the team to understand the main issues in the management of mechanical ventilation. The concepts of lung compliance, tracheal resistance, and inspiratory trigger appeared to be essential.
Then a large brainstorming began in order to imagine matching technical solutions and how those concepts could interact depending on respirator feedback. In addition, the team had to find a way for the medical instructor to control the simulator depending on the selected scenario.
This time of idea generation lead to the creation of a complex and connected system composed of different mechatronics modules that had to reproduce the physiological constraints of compliance, resistance, and inspiratory trigger.
Concerning compliance and resistance, a mechanical compression applied with electromechanical motors on a volume turned out to be able to generate the disorders observed in ARDS lungs.
Reproducing the inspiratory trigger turned out to be the most difficult part of the challenge. We had to generate a small depression inside the breathing circuit as does the patients’ diaphragm. We developed an adjustable mechanical depression system controlled by several motors. This module has been tested and validated by medical professionals after the completion of processing.
Different teams were formed to develop these specific aspects during the 36-hour challenge. Each model was developed by computer-aided design. Then the elements were 3D printed, laser cut in wood or Plexiglas and then assembled.
The last remaining hours were consecrated to final tests and preparation of the oral presentation for the public and jury members.
Results
The three medical professionals on our team conducted the final tests on the model. When the pulmonary trainer is connected to a ventilator, it allows ventilation in all modes thanks to the trigger, resistance, and pulmonary compliance modules. We checked the main measured parameters during modifications of resistance and compliance on the respirator. The aspect of ventilation pressure and volume curves seemed to be realistic when compared to a normal or a COVID lung.
At the end of the challenge, the ten competing teams presented their work. Next to our project, some teams transformed bikes into wheeling chairs while others improved the functioning of 3D-printed hand prostheses.
The presented prototype was fully functional and a demonstration of the different functions showed the pedagogical interest of this tool. The visual aspect of the ventilated balloon compressed by the webbing and the acute sound of the respirator’s turbines clearly simulated a severely affected lung increasing driving pressure.
Likewise, the compression of the plastic tube during modification of resistance quickly triggered the alarm of over-peak pressure simulating laryngospasm or obstruction of the laryngeal tube.
We were also able to show interest in a good setting of the inspiratory trigger thanks to the electronic gusset.
The jury was composed of members of different engineering schools, local hospitals, and patient associations. After deliberation, the jury decided to reward our work with the first prize of innovation emphasizing the good visual qualities of the simulator which was able to show to non-specialists the main disorders of a lung affected by COVID’s ARDS.
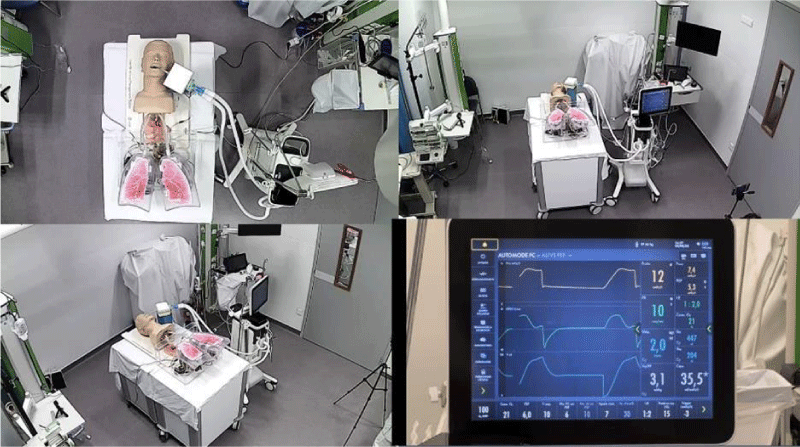
In the last version of the simulator (Picture 1), the pulmonary compliance module consists of two test balloons with elastic specificities mimicking a pulmonary alveolus. In the situation where lung compliance decreases, balloons are constrained by straps driven by stepper motors.
In this first version developed during a hackathon, we have not developed a method to evaluate the efficiency of gas exchanges.
This will probably be an additional innovation in the aftermath of product development.
Discussion
Through this challenge, many lessons were learned and further developments for this type of project were discovered.
The concept of mechanical ventilation is complex but relating to physics principles, we were able to explain the main parameters clinically relevant to a non-medical team of engineers. Developing a palpable and visible simulator probably allows non-specialists to understand the physio-pathology of COVIDs ARDS. This is a promising result for developing practical training for reinforcement task forces in intensive care units. Using different tools in addition to theoretical presentations should help students understand and memorize the critical parts of the training.
This tool should be included in formation focused on the concept of protective lung ventilation. This concept is today’s standard of care in the field of mechanical ventilation. Its aim is to prevent Ventilator Induced Lung Injury. The main mechanisms of these injuries are Volo and baro traumatisms due to high tidal volumes or high trans-pulmonary pressure. Other mechanisms include repetitive opening and closing of alveoli, pulmonary edema, and disruption of the surfactant layer. The other side effects of mechanical ventilation when improperly adjusted are diaphragm injury due to dysssynchrony, as well as excessive or insufficient assistance.
To resume this concept, the main characteristics of protective lung ventilation are:
- Any ventilation strategy that aims to minimize or prevent VILI
- ARDSnet Low VT, Plateau < 30 & PEEP/FiO2 table
- Open Lung Ventilation (Recruitment, HFO, APRV, Optimal PEEP)
- Prone Ventilation
- Adjunctive Therapies: Pulmonary vasodilators, ECLS, gene therapy, pharmacological, etc…..
Our simulator fits well in such critical training by its ability to reflect the driving pressure and the plateau pressure. It helps recognize a modification of compliance reflected by a linear increase of plateau and peak pressure whereas resistance modifications only modify peak pressure. Applications of low or high tidal volume with distention of the balloon are easily shown.
Our prototype could be improved in numerous ways:
- The development of a two balloons model would allow explaining the impact of therapies such as positive airway pressure on different kinds of topographic lung affections (mono vs. global lung low compliance)
- Adding visual representations of the lung to show inadequate ventilation and sound effects reflecting auscultation
- Configuration of scenarios describing main pathologies (bronchospasm, pneumothorax, ARDS, atelectasis, obstruction of the laryngeal tube, …).
We plan to develop a second prototype with these characteristics in a few months. We will then start using this tool during training sessions. On this occasion, the pedagogic impact of this simulation lung will be measured including long-term memorization.
- Goh KJ, Wong J, Tien JC, Ng SY, Duu Wen S, Phua GC, Leong CK. Preparing your intensive care unit for the COVID-19 pandemic: practical considerations and strategies. Crit Care. 2020 May 11;24(1):215. doi: 10.1186/s13054-020-02916-4. PMID: 32393325; PMCID: PMC7213774.
- Yuriditsky E, Horowitz JM, Nair S, Kaufman BS. Simulation-based uptraining improves provider comfort in the management of critically ill patients with COVID-19. J Crit Care. 2021 Feb;61:14-17. doi: 10.1016/j.jcrc.2020.09.035. Epub 2020 Oct 3. PMID: 33049487; PMCID: PMC7834289.
- Dixon W, Miller N, Toal GG, Sebok-Syer SS, Gisondi MA. Development of a 3D printed simulator for closed reduction of distal radius fractures. Perspect Med Educ. 2021 Jun;10(3):192-195. doi: 10.1007/s40037-020-00609-w. PMID: 32989709; PMCID: PMC8187689.
- Ziehr DR, Alladina J, Petri CR, Maley JH, Moskowitz A, Medoff BD, Hibbert KA, Thompson BT, Hardin CC. Respiratory Pathophysiology of Mechanically Ventilated Patients with COVID-19: A Cohort Study. Am J Respir Crit Care Med. 2020 Jun 15;201(12):1560-1564. doi: 10.1164/rccm.202004-1163LE. PMID: 32348678; PMCID: PMC7301734.
- Wilson JG, Calfee CS. ARDS Subphenotypes: Understanding a Heterogeneous Syndrome. Crit Care. 2020 Mar 24;24(1):102. doi: 10.1186/s13054-020-2778-x. PMID: 32204722; PMCID: PMC7092435.
- ARDS Definition Task Force, Ranieri VM, Rubenfeld GD, Thompson BT, Ferguson ND, Caldwell E, Fan E, Camporota L, Slutsky AS. Acute respiratory distress syndrome: the Berlin Definition. JAMA. 2012 Jun 20;307(23):2526-33. doi: 10.1001/jama.2012.5669. PMID: 22797452.
- Gosangi B, Rubinowitz AN, Irugu D, Gange C, Bader A, Cortopassi I. COVID-19 ARDS: a review of imaging features and overview of mechanical ventilation and its complications. Emerg Radiol. 2022 Feb;29(1):23-34. doi: 10.1007/s10140-021-01976-5. Epub 2021 Oct 26. Erratum in: Emerg Radiol. 2021 Nov 6;: PMID: 34698956; PMCID: PMC8545770.
- Li L, Lin M, Wang X, Bao P, Li Y. Preparing and responding to 2019 novel coronavirus with simulation and technology-enhanced learning for healthcare professionals: challenges and opportunities in China. BMJ Simul Technol Enhanc Learn. 2020 Jul;6(4):196-198. doi: 10.1136/bmjstel-2020-000609. Epub 2020 Mar 11. PMID: 32832099; PMCID: PMC7410111.
- Pasteka R, Forjan M, Sauermann S, Drauschke A. Electro-mechanical Lung Simulator Using Polymer and Organic Human Lung Equivalents for Realistic Breathing Simulation. Sci Rep. 2019 Dec 24;9(1):19778. doi: 10.1038/s41598-019-56176-6. PMID: 31874980; PMCID: PMC6930199.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.





 Save to Mendeley
Save to Mendeley
