Archives of Pulmonology and Respiratory Care
High Flow Nasal Oxygen as a Treatment Option for Acute Respiratory Distress Syndrome in Coronavirus (COVID-19) Infection
Jlal Bathish1, Ayat Zabida1, Muhammad Kashkush1, Doron Mulla1, Yael Berman2, Lee Cohen1 and Aliza Zeidman1*
2Physiotherapy Department, Hasharon Hospital, Rabin Medical Center, Petach Tikva, Sackler Faculty of Medicine, Tel Aviv University, Israel
Cite this as
Bathish J, Zabida A, Kashkush M, Mulla D, Zeidman A, et al. (2020) High Flow Nasal Oxygen as a Treatment Option for Acute Respiratory Distress Syndrome in Coronavirus (COVID-19) Infection. Arch Pulmonol Respir Care 6(1): 023-025. DOI: 10.17352/aprc.000046The ongoing outbreak of COVID-19 that began in Wuhan, China, has constituted a Public Health Emergency of International Concern, with cases confirmed in multiple countries. The outbreak of COVID- 19 in Israel, in March 2020 caused major changes in the routine work in hospitals mainly internal medicine wards . Hasharon hospital, a small community hospital in Petah Tikva was converted to corona patients admissions only. In accordance with this new reality internal medicine B department prepared itself to provide treatments tailored to the clinical needs of the Covid 19 patients and the quarantine conditions of these patients hospitalization. We report a confirmed case of COVID-19 who was diagnosed with ARDS and refused intubation. He was treated with High Flow Nasal Oxygen (HFNO) combined with medication and physiotherapy with very good results. This case highlights the importance of non-Invasive ventilation treatment.
Introduction
The 2019–20 coronavirus pandemic [1], is an ongoing pandemic of coronavirus disease 2019 (COVID-19) with severe acute respiratory syndrome as the main cause for morbidity and mortality [2,3]. The World Health Organization declared the outbreak to be a Public Health Emergency of International Concern on 30 January 2020, and recognized it as a pandemic on 11 March 2020 [4]. There are suggested therapeutic protocols for different stages of the disease [5]. However the timing of intubation and use of high flow nasal oxygen support are still nonconclusive at this point [6,7].
Case
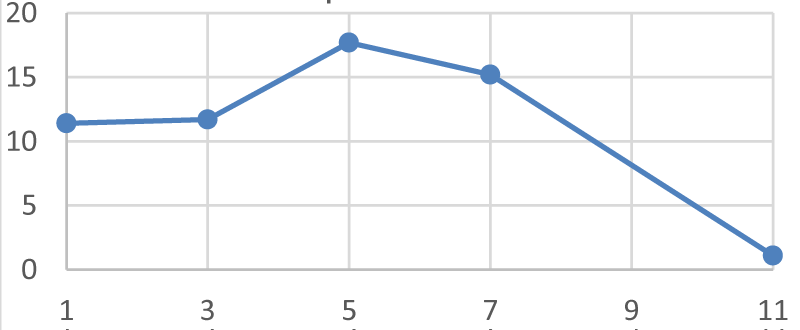
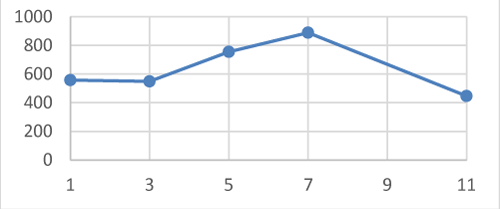
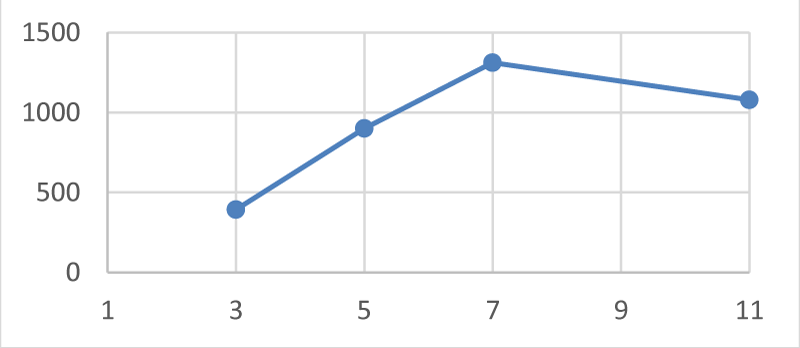
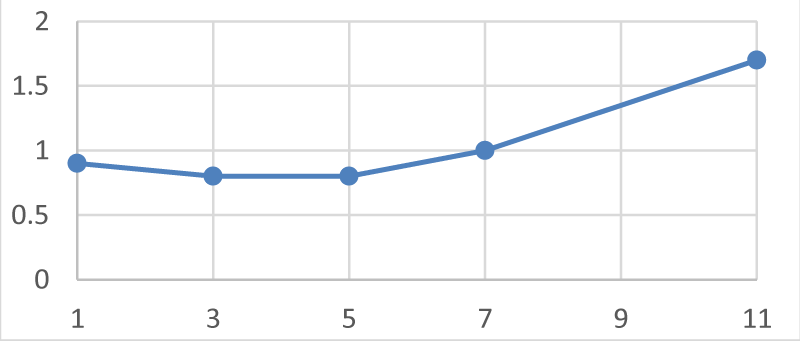
A confirmed case of COVID-19 patient, 56-year-old man, was admitted to the department of CORONA B in Hasharon hospital. The patient was complaining of fever up to 380 C, dry cough and dyspnea. He has a past medical history of obstructive sleep apnea (OSA) anxiety and heavy smoking. His current treatment at home includes using Continuous Positive Airway Pressure (CIPAP) mask and Venlafaxine 150mg (for anxiety) daily. He denies any other diseases including heart disease or heart failure. His symptoms of fever and sore throat began 5 days before admission and the patient was treated at home with oral antibiotics Zinnat 500 mg by his family physician with mild improvement and on the 6th day when his symptoms of sore throat, cough, and chest distress accompanied with progressive dyspnea he was tested by oropharyngeal swab test of SARS-CoV-2, qualitative real-time reverse-transcriptase–polymerase-chain-reaction (RT-PCR) assay and was found positive for COVID-19 and was admitted to our department. On admission, his physical examination revealed subclinical fever 37.80 C and no apparent dyspnea. Oxygen saturation on room air was 95% and the patient denies any difficulty breathing. Arterial blood gas analysis indicated PO2/FIO2 =238. Blood routine tests reveal C- reactive protein (CRP) - 11.5 (normal range 0-1). Hb- 13.6 g/Dl, WBC- 9370/micl, absolute lymphocytes-1000/micl (10.6%), Liver and renal function tests, myocardial enzymes, electrolyte were all in normal range. Chest X Ray shows mild bilateral Ground glass consolidation without a pleural effusion. And the patient was diagnosed with Mild ARDS (Berlin severity classification of ARDS) [7]. The patient was treated as moderate degree Corona patient including 3 days regimen of Azithromycin 500 mg/d, 5 days of Hydroxychloroquine 400 mg/d and oxygen by nasal cannula. Two days later the patient`s condition deteriorated, he became dyspneic and oxygen saturation dropped to 87-91% on room air. His blood tests deteriorated including CRP- 18 , absolute lymphocyte count 800/micl (8%), ferritin- 890 ng/mil ( normal range 13-150 ng/ml) and elevated DIDimer 1310 ng/ml ( normal range 0-500 ng/ml) (Figures 1-4).
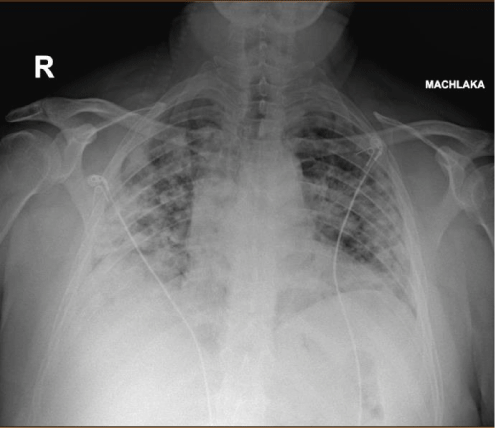
Chest X Ray showed bilateral interstitial ground glass finding diagnosed as severe ARDS (Figure 5).
At this point we consulted intensive care unit expert and the decision was to intubate the patient and start mechanical ventilation support. However, the patient became agitated and refused intubation and since the patient was alert and conscious, we decided to try High Flow Nasal Oxygen along with physiotherapy treatment and assurance of the patient. The whole process was performed via video cameras from outside the ward and a small team of staff near the patient. Since the patient was a former heavy smoker he was treated with Intravenous hydrocortisone 150 mg/once. Oxygen saturation improved immediately and the patient was able to maintain saturation of 95-96% by HFNO support. In the next few days the patient condition continued to improve, his respiratory symptoms improved, and he maintained normal body temperature. Four days later the patient was able to keep saturation with nasal oxygen tube and physiotherapy guidance via telemedicine. Blood test shows improvement of lymphopenia: absolute lymphocyte count was 1700 micl (24%) on day 8, and went back to normal (2700 micl -31%) on day 12. DIDimer and CRP dropped to normal rang on day 11 and ferritin level was 470 ng/ml. Negative PCR test for COVID- 19 was found in 2 consecutive tests and the patient was declared as non-active COVID 19 and was discharged home with oxygen and physiotherapy support. Two weeks later the patient reports of much better improvement, he only uses nasal oxygen at night and he is gradually going back to his normal activities.
Discussion
High flow nasal oxygen (HFNO) is a non-invasive respiratory support modality that delivers high flow (liters per minute) medical oxygen to a patient through an interface (nasal cannula) intended to create a wash-out of the upper airway. The applied gas is heated to best match human body temperature (37°C) and humidified targeting ideal body saturation vapor pressure [7,8]. Oxygenation is achieved by providing an increased FiO2 in the air flow to the patient. The constant flush of the upper airway creates a reservoir that reduces room-air entrainment to such an amount that it becomes a true fraction of inspired oxygen as set by the device [8].
Among patients with acute hypoxemic respiratory failure, HFNO was proven to avoid intubation compared to conventional oxygen device [9]. However, there is major concern that HFNO may increase bio-aerosol dispersion in the environment due to the high gas flow used. The increased dispersion might favor transmission of infectious agents, such as COVID-19, carried in aerosol droplets generated by the infected patient. There appears to be uncertainty and a trend to avoid HFNC among COVID-19 patients in the western world [9], thus increasing early intubation rates potentially causing associated harms related to sedation and prolonged intensive care unit stay. Furthermore, intubation procedures are associated with high risk for viral exposure of medical staff. Also, early intubation increases the demand for ventilators, contributing to the critical shortage reported worldwide. Avoiding or delaying invasive mechanical ventilation could substantially reduce immediate demand for ventilators.
Broad use of HFNO was observed in a study by Yang and colleagues from Wuhan, China where 33 out of 52 ICU patients were treated with HFNO with good results [11].
We described a patient who deteriorated to severe ARDS and we had to decide quickly on the method of respiratory support. Since he was alert and conscious and did not agree to intubation we decided to support him with HFNO combined with physiotherapy and one dose of corticosteroids with good clinical and laboratory results.
Conclusion
HFNO treatment provided to the right patient can improve respiratory treatment and avoid intubation even in ARDS. Further clinical studies are needed to truly evaluate aerosol dispersion and aerosol dynamics during physiological exhalation and cough in COVID 19
- Huang C, Wang Y, X li, Ren L, zhao J, et a. (2020) Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet 395:497-506. Link: https://bit.ly/2xTWmCO
- Yang X, Yu Y, Xu J, Shu H, Xia J, et al. (2020) Clinical course and outcome of critically ill patients with SARS-COV-2 pneumonia in Wuhan China: a single centered retrospective, observational study. Lancet Resp Med 8: 475-481. Link: https://bit.ly/2y8ysnk
- World Health Organization (2020) Clinical management of severe acute respiratory infection (SARI) when COVID-19 disease is suspected. Interim guidance. Link: https://bit.ly/2Z77abN
- Force ADT, Rainieri VM, Rubenfeld GD, Thompson BT, Ferguson ND, et al. (2012) Acute respiratory distress syndrome: The Berlin definition. JAMA 307: 2526-2533. Link: https://bit.ly/2WVaPa4
- McCreary EK, Pogue JM (2020) COVID-19 Treatment: A Review of Early and Emerging Options. Open Forum Infectious Diseases. 7: ofaa105. Link: https://bit.ly/2X2n7NQ
- Cascella M, Rajnik M, Cuomo A, Dulebohn S, Di Napoli R (2020) Features evaluation and treatment of Coronavirus (COVID-19). Ncbi Bookshelf. A service of the National library of medicine, National Institutes of Health. Link: https://bit.ly/2WYXe1t
- Frizzola M, Miller TL, Rodriguez ME, Zhu Y, Rojas J, et al. (2011) High-Flow Nasal Cannula: Impact on Oxygenation and Ventilation in an Acute Lung Model". Pediatr Pulmonol 46: 67-74. Link: https://bit.ly/363IJNT
- Dysart K, Miller TL, Wolfson MR, Shaffer TH (2009) Research in high flow therapy: Mechanisms of action. Respir Med 103: 1400-1405. Link: https://bit.ly/2WR1wb2
- Murthy S, Gomersall CD, Fowler RA (2020) Care for critically ill patients with COVID-19. JAMA 323:1499-1500.
- Rochwerg B, Granton D, Wang DX, Helviz Y, Einav S, et al. (2019) High flow nasal cannula compared with conventional oxygen therapy for acute hypoxemic respiratory failure: a systematic review and meta-analysis.Intensive Care Med 45:563-572. Link: https://bit.ly/3dQGMHB
- He G, Han Y, Fang Q, Zou J, Shen J, et al. (2020) Clinical experience of high-flow nasal cannula oxygen therapy in severe corona virus disease 2019 (covid-19) patients. Zhejing Da Xue Xue Bao Yi Xue Ban 25:49. Link: https://bit.ly/2y4h6rH
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
