Archives of Pulmonology and Respiratory Care
A foreign body aspiration presenting as left sided empyema and its removal by novel method
Ram Niwas*, Gopal Chawla, Nishant Kumar Chauhan and Naveen Dutt
Cite this as
Ram Niwas, Chawla G, Chauhan NK, Dutt N (2019) A foreign body aspiration presenting as left sided empyema and its removal by novel method. Arch Pulmonol Respir Care 5(1): 012-014. DOI: 10.17352/aprc.000036Introduction
Foreign body(FB) aspiration is seen commonly in children and can present acutely in form collapse stridor or respiratory arrest, though in adults FB aspiration is less common as compared to children. Here young male presented with dyspnoea which started after FB aspiration and resulted in formation of empyema increasing the respiratory distress.
Case Report
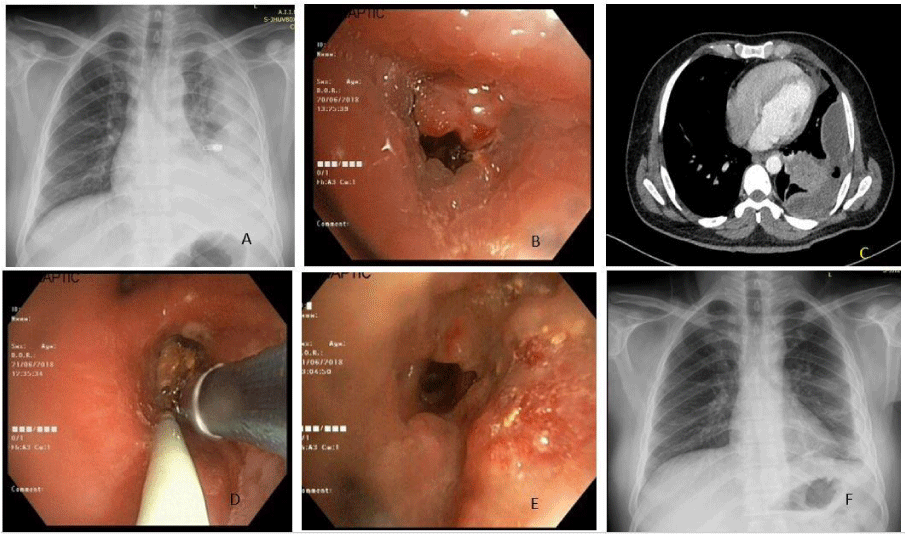
A 36 year old non-smoker who was occasional betel nut chewer, gold smith by occupation, having background history of Type 1 Diabetes Mellitus for past 6 years and was on anti-depressants for mood disorders for past 4 years, presented to emergency with worsening breathlessness and fever for past 4 days and chest pain for 3 days, he was having chest x ray which was done 3 days back showing blunting of left costophrenic angle. Patient was admitted and fresh tests were ordered along with chest x ray. On detailed history he told that 6 days back while eating betel nut he started coughing and felt he may have aspirated. Chest x ray showed increase in effusion along with some opacities extending up to middle zone. USG chest was done which showed organized effusion, which could not be aspirated even with 18 G needle , so USG guided pigtail (16 fr) was inserted and thick brown pus was drained , which was sent for microbiological analysis. Contrast enhanced computerized tomography of chest showed presence of loculated collection in left pleural space with gas locules and pleural enhancement with collapse-consolidation of underlying left lower lobe parenchyma (predominantly posterior basal segment). Multiple homogenously enhancing lymph nodes were noted in pre/paratracheal, subcarinal and aortopulmonary window regions. Side by side fiberoptic bronchoscopy was planned. During FOB fleshy endobronchial growth was seen in lower lobe post segment, which bleed to touch, mucus was seen coming from side of growth. BAL was taken and sent for microbiological analysis. Patient was planned for repeat FOB for endobronchial biopsy next day after informed consent. Globular fleshy mass was cauterised partially to take biopsy, but to surprise brown unidentified material was seen below that mass after electro cautery (Figure 1).
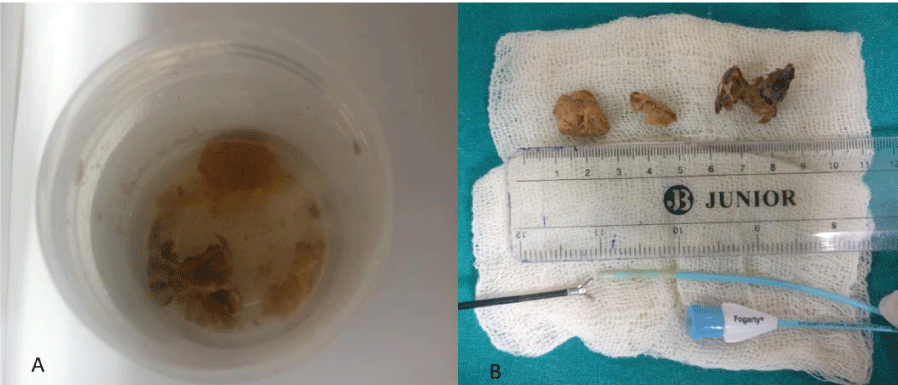
Histopathologic examination of biopsy showed fibro-collagenous tissue infiltrated with acute on chronic inflammatory infiltrate and numerous proliferating blood vessels with adjacent areas of fibrosis. Bacterial colonies noted along with separate focus showing organic foreign body probably betel nut. It was removed in novel way after 3 days by introducing Fogarty (Figure 2). It was inflated and pulled along with endobronchial biopsy forceps while maintaining traction over the fogarty. Post removal of foreign body patient improved clinically and radiologically.
Discussion
Foreign body aspiration is seen all over the world. It usually presents in a variety of ways, ranging from being asymptomatic or trivial symptoms to life threatening respiratory and death. Foreign body aspiration in adults is usually seen in advanced age, poor dentition, underlying neurological disorder, alcohol use and use of sedatives. In the absence of predisposing factors, children are reported to be at a higher risk than adults. In children material which are aspirated are objects like part of toys, screws and other household items. Aspiration of organic material such as nuts, peas, fruit seeds, pieces of vegetables, betel nut and bones have been described in adults [1-4].
In young patient occult foreign body presenting as empyema is a reported in patients where occult long standing foreign body such as bone or rear cap of ball point pen which resulted in development of empyema over several months to 30 years [5-7].
Aspirated FB at times cause unresolved pneumonia or even rarely result empyema in adult patient like the one described above. Bronchoscopy becomes the investigation of choice in majority of such patients. A high degree of suspicion coupled with radiology is necessary to avoid the delay in procedure thus decrease in the rate of complications. Unresolved pneumonia, localised bronchiectasis, collapse or localised hyperlucency/air trapping are helpful clinical hints in radiology that point towards foreign body [8].
Our patient had initial chest x ray which showed heterogeneous opacity in left lower lobe and next radiology was suggestive of massive pleural effusion which later turned out to be empyema. This is quite unusual as there is no report which shows acute aspiration of betel nut results in empyema. It may be because our patient was having diabetes which has been shown independent risk factor in diabetes [9].
It is a known fact that long standing FB aspiration may cause bronchiectasis, necrotising pneumonia or pleural effusion [10]. Empyema following aspiration of a FB is rare scenario which has never been reported in literature in adults. One study which was done over a period of 15 year revealed among 1038 patients of bronchiectasis only eight were found to be due to a long retained FB [9]. It has been proven again and again that removal of FB is sufficient to revert the lung changes to normal, and usually it does not warrant any surgical intervention but at times need lobectomy or even pneumectomy [10].
In the present case, the acute aspiration of FB occurred in the left lower lobe bronchus as compared to common observation of lodgement in right main bronchus, but few previous studies had shown that FB aspiration into the left main bronchus was also not that uncommon. Dong et al showed that out of 200 patients with FB, 80 (40%) had in left endobronchial tree [11].
Removal of foreign body is especially tricky because during removal they can break dislodge further in bronchial tree. Various modalities have been used like rigid bronchoscopy, dormia basket, cryoextraction etc. Here we used fogarty and flexible holding forceps, inflated fogarty placed distally prevented dislodgement and also helped in providing traction along with holding forceps [12].
To conclude FB aspiration should be considered as one of the important differential of chronic intractable cough or unresolved pneumonia. An old unrecognised FB aspiration can present with recurrent pneumonia and secondary empyema. Especially in patients with immunosuppression it can present early and should be considered by giving due importance to history and course of illness.
- al Majed SA, Ashour M, al-Moberireek AF, al-Hajjaj MS, Alzeer AH, et al. (1997) Overlooked inhaled foreign bodies: late sequelae and the likelihood of recovery. Resp Med 91: 293-296. Link: http://bit.ly/2KsKOd4
- Irwin RS, Ashba JK, Braman SS, Lee HY, Corrao WM (1997) Food asphyxiation in hospitalized patients. JAMA 237: 2744-2745. Link: http://bit.ly/2MddBVb
- Rahulan V, Patel M, Sy E, Menon L (2003) Foreign body aspiration in elderly: an occult cause of chronic pulmonary symptoms and persistent infiltrates. Clin Geriatr 11: 41-43.
- Baharloo F, Veyckemans F, Francis C, Biettlot MP, Rodenstein DO (1999) Tracheobronchial foreign bodies: presentation and management in children and adults. Chest 115: 1357-1362. Link: http://bit.ly/2Kroelb
- Kevin Schembri, Viktor Serafimov, Stephen Montefort, Alexander Manche (2003) Empyema thoracis caused by a foreign body inhaled 30 years previously. 2: 581-583. Link: http://bit.ly/2KKxsrN
- Asadi Gharabaghi M, Asadi Gharabaghi M, Firoozbakhsh S (2012) Empyema caused by foreign body aspiration Case Reports 2012: bcr2012007760. Link: http://bit.ly/2OQ9PDt
- Mehta A, Gupta A, Ks A, Venkitakrishnan R (2015) Endobronchial Foreign Body (FB): A Rare Cause of Empyema. J Clin Diagn Res 9: OJ02-OJ03. Link: http://bit.ly/2Z06cia
- Zissin R, Shapiro-Feinberg M, Rozenman J, Apter S, Smorjik J (2001) et al. CT findings of the chest in adults with aspirated foreign bodies. Eur Radiol 11: 606-611. Link: http://bit.ly/2Z1rRSS
- Lai SW, Lin CL, Liao KF (2017) Population-based cohort study investigating the correlation of diabetes mellitus with pleural empyema in adults in Taiwan. Medicine (Baltimore) 96: e7763. Link: http://bit.ly/2MdIU2j
- Kane GC, Sloane PJ, McComb B, Chinn B, Gottlied JE (1994) 'Missed' inhaled foreign body in the adult. Respir Med 88: 551-554. Link: http://bit.ly/2ZVRCFx
- Dong YC, Zhou GW, Bai C, Huang HD, Sun QY, et al. (2012) Removal of tracheobronchial foreign bodies in adults using a flexible bronchoscope: experience with 200 cases in China. Intern Med 51: 2515-2519. Link: http://bit.ly/2YS81xB
- Lim SH, Lee DK, Lee JY (2011) Bronchial foreign body removal under general anesthesia with a modified port, a fogarty balloon catheter and a grasping forceps. Korean J Anesthesiol 61: 177-179. Link: http://bit.ly/2Z05flV
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
