Annals of Pancreatic Disorders and Treatment
Pancreatic cysts: Not always Cystadenoma
Alba Manuel Vázquez*, Latorre Fragua R, de la Plaza R and Ramia JM
Cite this as
Vázquez AM, Latorre Fragua R, de la Plaza R, Ramia JM (2018) Pancreatic cysts: Not always Cystadenoma. Ann Pancreat Disord Treatm 2(1): 001-001. DOI: 10.17352/apdt.000004Case Report
Pancreatic neuroendocrine tumors (PNETs) account for 1-5% of all pancreatic neoplasms and are typically solid in nature. Only about 10% of are cystic [1-3]. One of the challenges in their management is establishing an accurate preoperative diagnosis.
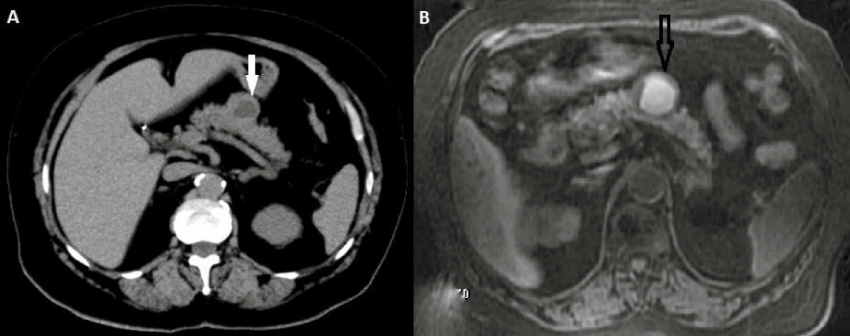
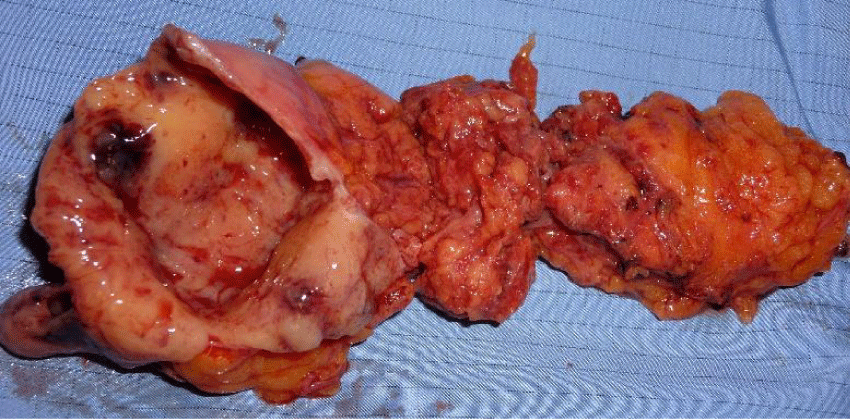
A 71-years-old female was incidentally discovered to have a 3.3-cm cystic lesion in pancreatic body on abdominal CT/MRI (Figure 1). Endoscopic Ultrasound (EUS) revealed a 4-cm cystic lesion in pancreatic body (Figure 2). A EUS guided biopsy was done and informed as cells with atypia. Due to a presumptive diagnosis of mucinous cystadenoma, laparoscopic distal pancreatectomy was performed (Figure 3). The patient was discharged with grade a pancreatic fistula, solved with conservative management (Clavien: I, CCI: 8.7). Histopathology study demonstrated a 4-cm cystic lesion confined to the pancreas, G1 neuroendocrine tumor (T2N0M0) (Ki-67: 5%). She did not receive any adjuvant treatment. No recurrence has been observed during seven years follow-up.
PNETs may have a biological behavior that can range from indolent benign lesions to malignant lesions capable of metastasis [1]. Cystic PNETs tend to be less aggressive compared with their solid counterpart, although they are larger lesions. They are associated with lower mitotic index, tumor necrosis, perineural and lymphovascular invasion and metastasis [1,3]. The patient survival is slightly higher than solid PNETs patients [3]. The pathophysiology of cystic PNETs remains uncertain, several theories exists: cystic degeneration, secondary to tumor necrosis, intra-cystic hemorrhage, or if they are a true different biological entity [2,3].
- Cloyd JM, Kopecky KE, Norton JA, Kunz PL, Fisher GA, et al. (2016) Neuroendocrine tumors of the pancreas: Degree of cystic component predicts prognosis. Surgery 160: 708-713. Link: https://goo.gl/RmN8kQ
- Caglià P, Cannizzaro MT, Tracia A, Amodeo L, Tracia L, et al. (2015) Cystic pancreatic neuroendocrine tumors: To date a diagnostic challenge. Int J Surg 1: S44-49. Link: https://goo.gl/p528Ya
- Koh YX, Chok AY, Zheng HL, Tan CS, Goh BK (2014) A systematic review and meta-analysis of the clinicopathologic characteristics of cystic versus solid pancreatic neuroendocrine neoplasms. Surgery 156: 83-96.e2. Link: https://goo.gl/Eq3g5z
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
