Archives of Otolaryngology and Rhinology
Effect of smoking on status of hearing: A cross-sectional study
Nandita Gautam1*, Shivalingesh KK2, Anushtha Kushwaha1, Varnika Singh3, Siddhant Singh4 and Shashank Kumar5
2Professor & Head, Department of Public Health Dentistry Institute of Dental Sciences, Bareilly, India
3Department of Conservative Dentistry & Endodontics, Institute of Dental Sciences, Bareilly, India
4Department of Periodontology, Institute of Dental Sciences, Bareilly, India
5Department of Pedodontics, Institute of Dental Sciences, Bareilly, India
Cite this as
Gautam N, Shivalingesh KK, Kushwaha A, Singh V, Singh S, et al. (2022) Effect of smoking on status of hearing: A cross-sectional study. Arch Otolaryngol Rhinol 8(3): 009-013. DOI: 10.17352/2455-1759.000146Copyright
© 2022 Gautam N, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Introduction: Smoking is a common tendency among all social classes around the globe, especially in the working population.
Objective: To assess the significant link between tobacco and cigarette smoking and its effect on hearing among smokers as there is limited study on this aspect of the Indian population particularly with a high-frequency hearing threshold.
Methodology: Cross-sectional study carried out on patients attending the OPD in ENT and Head & Neck Surgery Department of Rohilkhand Medical College & Hospital. The sample size came to be 90.
Results: In smokers, there were 72 (80%) males and 18 (20%) females while in the non-smoker group, there were 53 (58.8%) males and 37 (41.11%) females, and 39 (43.3%) subjects belonging to the rural population while 51 (56.7%) subjects belong to an urban population. out of 90 subjects, 43 (30.3%) had cochlear deafness followed by 40 (28.2%) who had normal hearing and 7 (4.9%) had retrocochlear deafness.
Conclusion: Tobacco has the power to reduce the ability to hear, mainly causing a sensorineural hearing loss at higher frequencies.
Introduction
Smoking is a common tendency among all social classes around the globe, especially in the working population. The World Health Organization has estimated that there are approximately 250 million people with hearing disabilities worldwide, making hearing loss the 15th greatest cause of the burden of disease as Disability Adjusted Life Years (DALYs) across sexes and age groups [1].
Apart from the systemic diseases caused by tobacco, it has been found that smoking affects the senses, which involves hearing. Current smokers are 1.69 times at a higher risk for hearing loss as compared to non-smokers. The auditory system is greatly affected by cigarette smoking apart from the onset of cancer, respiratory and cardiovascular diseases. The biomarker of exposure to tobacco in both active and passive smokers is cotinine, which is a major proximate metabolite of nicotine [1].
Smoking brings about ototoxic effects via substances like tar, toluene, styrene, xylene, lead, and carbon monoxide. So, tobacco is known to reduce the ability to hear, causing hearing loss at different frequencies through several mechanisms in the inner ear that can be categorized as direct or indirect. Reactive oxygen species (ROS) and free radicals are responsible for direct oxidative damage, leading to sensorineural hearing loss by destructing cellular components that especially affect higher frequencies. Nicotine causes indirect damage, which includes the vasospastic effect, leading to atherosclerosis of the auditory system. Thus, oxygen perfusion gets hampered by these conditions [2].
Nicotine causes vasospasm of cochlear vascular loops, production of carboxyhaemoglobin, increased blood viscosity, reduced oxygen transport, and difficulty in oxyhemoglobin dissociation leading to ischemia of the cochlea. Thus, damage to the hair cells of the organ of Corti takes place due to a reduction in the blood supply of cochlear vessels. Smoking has a synergistic effect on elevated diastolic blood pressure and Raynaud’s phenomenon.
It has been observed that cigarette smoking is responsible for elevated levels of platelet-activating factors, LDL and HDL, which may be related to smoking-induced atherosclerosis. Premature atherosclerosis may also be linked to elevated carbon monoxide concentrations inducing distant effects on the cochlear circulation. The tendency for blood to clot in the presence of atherosclerotic plaques may retard inner ear circulation. Thus cochlear circulation gets affected by all these factors.
Health effects of smoking depend on the exposure history, including the duration of smoking, the number of cigarettes, the degree of inhalation and characteristics like tar and nicotine content. Certain factors are believed to aggravate SNHL such as raised blood pressure, deranged lipid metabolism, various systemic disorders, and ototoxic drugs [3].
The deleterious effect of smoking remains a major problem despite all the positive impacts on public health due to tobacco control policies. One of the major causes of the development of middle and inner ear pathologies is active smoke and passive smoke exposure.
Smoking may accelerate presbycusis, i.e., age-related hearing loss. According to World Health Organisation`s statistics, 5% of the whole world`s population has disabling hearing loss (defined as an average hearing threshold of 40 dBHL) and one-third of the over 65 years age group is affected by it [2].
The purpose of the present study is to assess the significant link between tobacco and cigarette smoking and its effect on hearing among smokers as there is limited study on this aspect of the Indian population, particularly with a high-frequency hearing threshold.
Methodology
The proposed study was carried out in the Department of Otorhinolaryngology and Head & Neck surgery, Rohilkhand Medical College and Hospital, Bareilly. All patients attending the OPD in ENT and Head & Neck Surgery Department of Rohilkhand Medical College & Hospital, Bareilly were enrolled for the study. The sample size was calculated by the formula 4pq/n2. As per the study by Kumar A, et al. (2013), the prevalence of hearing loss was 0.657 %. The sample size came to be 90. Ethical clearance was obtained from the Institutional Review Board (IRB) of Rohilkhand Medical College & Hospital, Bareilly.
All patients who had a history of smoking (Pack years Amir 2014), were willing to participate in this study, and the age group of 18-60 years was included in the study. Patients with a history of Diabetes mellitus, hypertension, known hearing loss, ear surgery, ototoxic drug use, and those with Familial deafness, and exposure to noise (occupational noise or non-occupational noise such as amplified music, etc.) were excluded. Also, All patients below the age of 18 years and above 60 years were excluded from the study.
Plan of study
- The medium of communication with the patient was in vernacular language. A written and informed consent from the patient was taken after explaining to them about the study, its procedure, and the aim and objectives.
- All the patients included in the study were thoroughly examined as per case record form and a detailed ENT examination with the appropriate investigation was done.
- The participants will be 90 smokers (i.e. who had smoked or were current smokers) and 90 non-smokers of age 18 - 60 years of either sex.
- The hearing tests were carried out in a sound-treated room in the OPD of the Otorhinolaryngology Dept. The hearing tests included a tuning fork test, pure tone audiometry, and a special test.
- The special test (Short Increment Sensitivity Index) was conducted in cases of sensori-neural hearing loss to differentiate between cochlear and retrocochlear pathology.
Results
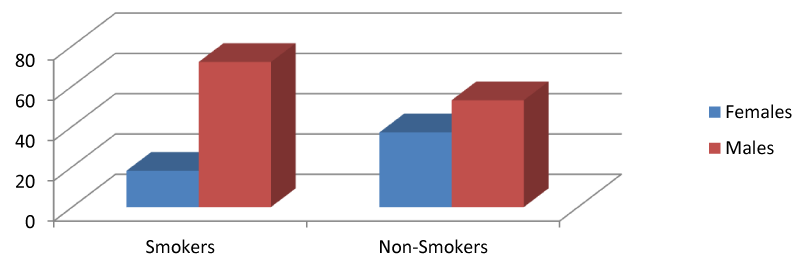
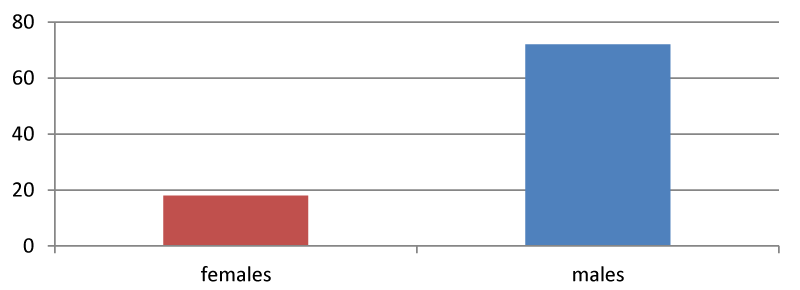
In our study, we included a total of 90 smokers and 90 non-smokers. In smokers, there were 72 (80%) males and 18 (20%) females while in the non-smoker group, there were 53 (58.8%) males and 37 (41.11%) females. Also Out of 90 subjects, there are 72 (80%) males and 18 (20%) females in this study as shown in Graphs 1,2.
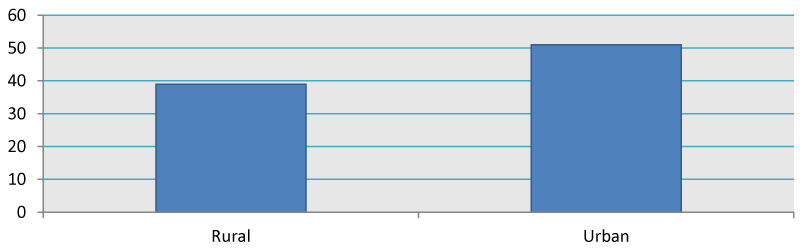
Graph 3 depicts that, 39 (43.3%) subjects belong to the rural population while 51 (56.7%) subjects belong to an urban population. In our study, there are subjects of various age groups, 33 (36.6%) subjects belong to 20-30 years of age, 22 (24.4%) belong to 31 - 40 years of age, 19 (21.1%) subjects belong to 41-50 years of age and 16 (17.7%) subjects belong to 51-60 years of age as shown in Graph 4.
In our study, out of 90 subjects, 21(23.3%) had complained of decreased mouth opening, 22 (24.4%) had foreign body sensation throat and 47 (52.2%) had an oral lesion and also found that 40 (44.4%) has sensorineural hearing loss, followed by 37 (41.1%) has normal hearing, followed by 9 (10%) had Mixed hearing loss and 4 (4.4%) had conductive hearing loss as shown in Tables 1,2.
In this study, out of 90 controls, we included 53 (58.9%) males and 37 (41.1%) females (Table 3). We also found that out of 45 Bidi smokers, 31 (68.8%) were males and 14 (31.11%) were females, whereas out of 45 cigarette smokers, 41 (91.11%) were males and 4 (8.88%) were females (Table 4).
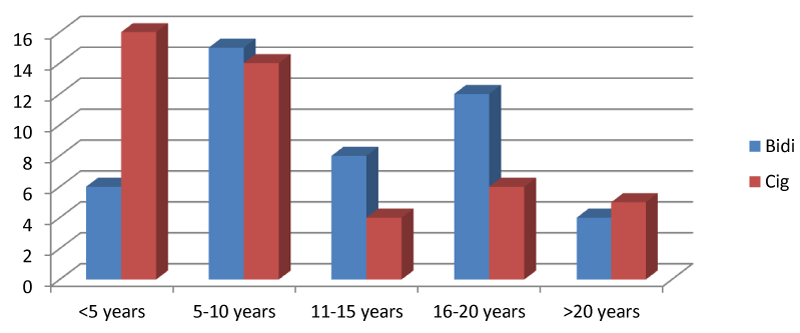
In this study we found that out of 90 smokers, 6 (6.67%) bidi smokers and 16 (17.77%) cigarette smokers smoked for a duration <5 years, 15 (16.67%) bidi smokers and 14 (15.55%) cigarette smokers smoked for the duration of 5 - 10 years, 8 (8.88%) bidi smokers and 4 (4.44%) cigarette smokers smoked for the duration of 11 - 15 years, 12 (13.33%) bidi smokers and 6 (6.67%) cigarette smokers smoked for the duration for 16 - 20 years and 4 (4.44%) bidi smokers and 5 (5.55%) cigarette smokers smoked for >20 years of duration as shown in Graph 5.
As shown in Table 5, according to the above-mentioned classification, out of 45 bidi smokers, 12 (13.33%) had mild, 22 (24.44%) had moderate, 9 (10%) had moderately severe and 2 (2.22%) had severe degree of hearing loss whereas out of 45 cigarette smokers, 25 (27.77%) had mild, 11 (12.22%) had moderate, 8 (8.88%) had moderately severe and 1 (1.11%) had severe hearing loss.
Also, based on the Short increment sensitivity index, out of 90 subjects, 43 (30.3%) had cochlear deafness followed by 40 (28.2%) who had normal hearing and 7 (4.9%) had retrocochlear deafness as shown in Tables 6-8.
Discussion
In our study, we included a total of 90 smokers and 90 non-smokers. In smokers, there were 72 (80%) males and 18 (20%) females while in the non-smoker group, there were 53 (58.8%) males and 37 (41.11%) females in a study conducted by Chang J, et al. [4], among 12,935 participants analyzed, 3,374 (26.08%) were current smokers, 2,792 (21.58%) were passive smokers and 6,769 (52.33%) were non-smokers. Out of 90 subjects, there are 72 (80%) males and 18 (20%) females in the present study. whereas in a study conducted by Abraham B. et al. [5], among the non-exposed the percentage of hearing loss increased with increasing quantity smoked, although the individual differences were small and not statistically significant. Among exposed men, similar trends were noted except in the 30 to 39-year age groups. In our study, 39 (43.3%) subjects belong to the rural population while 51 (56.7%) subjects belong to the urban population whereas in research carried out by Gaur K, et al. [6], Eight hundred and sixty-seven (49.8%) tobacco users and 1438 (59.8%) non-users were residents of the urban area and 872 (50.2%) tobacco users and 966 (40.2%) non-users were the residents of semi-urban and rural areas.
In our study, there are subjects of various age groups, 33 (36.6%) subjects belong to 20 - 30 years of age, 22 (24.4%) belong to 31-40 years of age, 19 (21.1%) subjects belong to 41-50 years of age and 16 (17.7%) subjects belong to 51-60 years of age whereas In a study conducted by Chang J, et al. [4], 1,683 (13.01%) were aged between 19 and 29, 2,570 (19.87%) were in their 30s, 2,401 (18.56%) were in their 40s, 2,550 (19.91%) were in their 50s, 2,041 (15.78%) were in their 60s, 1,445 (11.17%) were in their 70s and 245 (1.89%) were over 80 years old.
In our study, out of 90 subjects, 21(23.3%) had complained of decreased mouth opening, 22 (24.4%) had foreign body sensation throat and 47 (52.2%) had oral lesions while in research carried out by Gaur K, et al. [6], among 11,454 study subjects the middle ear diseases chronic suppurative otitis media (CSOM), acute otitis media (AOM), secretory otitis media (SOM) and otosclerosis were found to be the most common with 659 (15.9%), 136 (3.2%), 88 (2.1%) and 41 (0.9%) patients respectively when adjusted for age.
Distribution of data based on PTA among smokers
In our study we found that 40 (44.4%) has sensorineural hearing loss, followed by 37 (41.1%) has normal hearing, followed by 9 (10%) had Mixed hearing loss and 4 (4.4%) had conductive hearing loss whereas Chang J, et al. [4], reported that PTA threshold measured after exposure to tobacco is around 20 - 25 dBHL, indicating that passive smoking is related to mild or minimal sensorineural hearing loss. There are few available studies conducted in adults, but these report that passive exposure to tobacco is more likely to result in hearing loss. Also Adair-Bischoff, et al. [7], reported low odds of middle ear diseases (overall odds 1.13, CI 0.97 - 1.31) as compared to sensorineural hearing loss (overall odds 1.40, CI 1.07 - 1.85) due to confounding effects of different type of tobacco usage in the study. Also in research carried out by Mehrparvar HA, et al. [8], the mean exposure to noise in all subjects was 92.1 ± 2.4 dBA (Leq8h). The highest level of noise was found in spray drying (94.9 dBA), and the lowest noise level was observed in loading (84.9 dBA).
In this study, we found that out of 90 smokers, 6 (6.67%) bidi smokers and 16 (17.77%) cigarette smokers smoked for a duration <5 years on the contrary in research carried out by Gaur K, et al. [6] among 11,454 study subjects 1739 (42.0%) were smokers or used tobacco and Gopinath, et al. [9], reported that prevalence of hearing loss at baseline in this population was 33.0%, with the majority (81.0%) consuming some type of alcoholic drink per day. Similarly in research carried out by Mehrparvar HA, et al. [8]. Subjects in the smokers group smoked 6.7 ± 2.4 pack-years (range: 1–35 pack-years).
In this study, out of 45 bidi smokers, 12 (13.33%) had mild, 22 (24.44%) had moderate, 9 (10%) had moderately severe and 2 (2.22%) had severe degree of hearing loss whereas out of 45 cigarette smokers, 25 (27.77%) had mild, 11 (12.22%) had moderate, 8 (8.88%) had moderately severe and 1 (1.11%) had severe hearing loss whereas in research carried out by Gaur K, et al. [6], betel-quid, pan-masala, alcohol use and other addictions which all can independently influence the middle and internal ear diseases.
Distribution of data based on the duration of smoking and degree of hearing loss among the study subjects
In research carried out by Mehrparvar HA, et al. [8], the highest threshold in conventional and high-frequency audiometry was observed at 6 kHz and 16 kHz, respectively which was relatively higher than the present study. Several other studies showed a definitive correlation between SNHL and tobacco addiction. In a population‑based study done by Cruickshanks, et al. [10], it was shown that smokers are at 1.7 times more risk of developing SNHL than nonsmokers. Several other studies such as Itoh, et al. [11], and Rosenhall, et al. [12], have shown that smoking is a major risk factor for SNHL. It is clearly shown that smoking causes high‑frequency SNHL by Cunningham, et al. [13], studies. An India‑based study done by Kumar, et al. [14], showed a similar finding that there is a direct association between smoking and SNHL.
Conclusion
It seems quite clear from the report above that the harmful effects of cigarette smoking greatly affect the auditory apparatus, as well as promote the onset of cancer, cardiovascular disease, and respiratory disease. Therefore, tobacco has the power to reduce the ability to hear, mainly causing sensorineural hearing loss at higher frequencies.
- World Health Organization. Millions of people in the world have hearing loss that can be treated or prevented. http://www.who.int/pbd/deafness/ news/Millionslivewithhearingloss.pdf.
- Hu H, Sasaki N, Ogasawara T, Nagahama S, Akter S, Kuwahara K, Kochi T, Eguchi M, Kashino I, Murakami T, Shimizu M, Uehara A, Yamamoto M, Nakagawa T, Honda T, Yamamoto S, Hori A, Nishiura C, Okazaki H, Imai T, Nishihara A, Miyamoto T, Tomita K, Kabe I, Mizoue T, Kunugita N, Dohi S; Japan Epidemiology Collaboration on Occupational Health Study Group. Smoking, Smoking Cessation, and the Risk of Hearing Loss: Japan Epidemiology Collaboration on Occupational Health Study. Nicotine Tob Res. 2019 Mar 30;21(4):481-488. doi: 10.1093/ntr/nty026. PMID: 29547985.
- Sumit AF, Das A, Sharmin Z, Ahsan N, Ohgami N, Kato M, Akhand AA. Cigarette smoking causes hearing impairment among Bangladeshi population. PLoS One. 2015 Mar 17;10(3):e0118960. doi: 10.1371/journal.pone.0118960. PMID: 25781179; PMCID: PMC4363488.
- Chang J, Ryou N, Jun HJ, Hwang SY, Song JJ, Chae SW. Effect of Cigarette Smoking and Passive Smoking on Hearing Impairment: Data from a Population-Based Study. PLoS One. 2016 Jan 12;11(1):e0146608. doi: 10.1371/journal.pone.0146608. PMID: 26756932; PMCID: PMC4710530.
- Siegelaub AB, Friedman GD, Adour K, Seltzer CC. Hearing loss in adults: relation to age, sex, exposure to loud noise, and cigarette smoking. Arch Environ Health. 1974 Aug;29(2):107-9. doi: 10.1080/00039896.1974.10666542. PMID: 4835178.
- Gaur K, Kasliwal N, Gupta R. Association of smoking or tobacco use with ear diseases among men: a retrospective study. Tob Induc Dis. 2012 Apr 3;10(1):4. doi: 10.1186/1617-9625-10-4. PMID: 22471960; PMCID: PMC3366886.
- Adair-Bischoff CE, Sauve RS. Environmental tobacco smoke and middle ear disease in preschool-age children. Arch Pediatr Adolesc Med. 1998 Feb;152(2):127-33. doi: 10.1001/archpedi.152.2.127. PMID: 9491037.
- Mehrparvar AH, Mirmohammadi SJ, Hashemi SH, Davari MH, Mostaghaci M, Mollasadeghi A, Zare Z. Concurrent effect of noise exposure and smoking on extended high-frequency pure-tone thresholds. Int J Audiol. 2015 May;54(5):301-7. doi: 10.3109/14992027.2014.978906. Epub 2014 Dec 3. PMID: 25470622.
- Gopinath B, Flood VM, McMahon CM, Burlutsky G, Smith W, Mitchell P. The effects of smoking and alcohol consumption on age-related hearing loss: the Blue Mountains Hearing Study. Ear Hear. 2010 Apr;31(2):277-82. doi: 10.1097/AUD.0b013e3181c8e902. PMID: 20054277.
- Cruickshanks KJ, Klein R, Klein BE, Wiley TL, Nondahl DM, Tweed TS. Cigarette smoking and hearing loss: the epidemiology of hearing loss study. JAMA. 1998 Jun 3;279(21):1715-9. doi: 10.1001/jama.279.21.1715. PMID: 9624024.
- Itoh A, Nakashima T, Arao H, Wakai K, Tamakoshi A, Kawamura T, Ohno Y. Smoking and drinking habits as risk factors for hearing loss in the elderly: epidemiological study of subjects undergoing routine health checks in Aichi, Japan. Public Health. 2001 May;115(3):192-6. doi: 10.1038/sj.ph.1900765. PMID: 11429714.
- Rosenhall U, Sixt E, Sundh V, Svanborg A. Correlations between presbyacusis and extrinsic noxious factors. Audiology. 1993 Jul-Aug;32(4):234-43. doi: 10.3109/00206099309072939. PMID: 8343080.
- Cunningham LL, Tucci DL. Hearing Loss in Adults. N Engl J Med. 2017 Dec 21;377(25):2465-2473. doi: 10.1056/NEJMra1616601. PMID: 29262274; PMCID: PMC6457651.
- Kumar A, Gulati R, Singhal S, Hasan A, Khan A. The effect of smoking on the hearing status-a hospital based study. J Clin Diagn Res. 2013 Feb;7(2):210-4. doi: 10.7860/JCDR/2013/4968.2730. Epub 2013 Feb 1. PMID: 23542766; PMCID: PMC3592276.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.
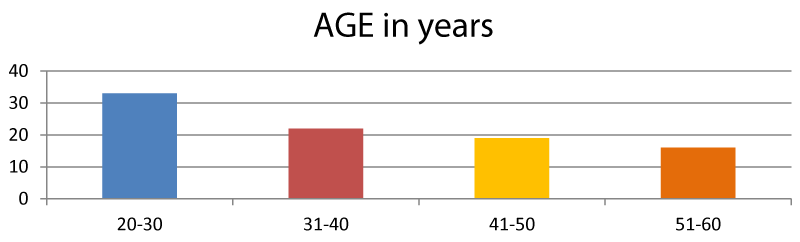

 Save to Mendeley
Save to Mendeley
