Archives of Otolaryngology and Rhinology
Dilated jugular venous arch mimicking a medial neck mass – A case report
Tran Van Buu1*, Grégoire Braux2, Benoît Pacquelet2, Emmanuel Babin1,3 and Justin Dugué1
2Department of Radiology, University Hospital, Caen 14000, France
3Unité 1086, INSERM-University of Caen-Basse Normandie, 14032 Caen, France
Cite this as
Buu TV, Braux G, Pacquelet B, Babin E, Dugué J (2021) Dilated jugular venous arch mimicking a medial neck mass – A case report. Arch Otolaryngol Rhinol 7(2): 016-018. DOI: 10.17352/2455-1759.000140The Anterior Jugular Venous System (AJVS) comprises a pair of anterior jugular veins and jugular venous arch, which plays an important role in the interconnection between superficial and deep veins. Anatomical variation of the AJVS predisposes one to dangerous complications during procedures involving head and neck region. Furthermore, these aberrant anatomies may manifest in various clinical forms which may be a challenge to diagnose. In the present study, we report a case of a enlarged jugular venous arch inducing a tumor-mimicking lesion in suprasternal notch. The knowledge about these anatomical variations can assist the physicians in interpreting neck masses and preventing iatrogenic injury.
Abbreviations
JVA: Jugular Venous Arch, AJVS: Anterior Jugular Venous System, AJV: Anterior Jugular Vein, CTA: Computed Tomography Angiography, SCM: Sternocleidomastoid Muscle.
Introduction
The Jugular Venous Arch (JVA) forms an integral part of the Anterior Jugular Venous System (AJVS) providing a collateral pathway communicating both innominate veins. Anatomical variation of the JVA is uncommon and may be a source of unintended complications during diagnostic and surgical procedures involving the head and neck regions [1,2]. These anomalies may be present early but not evident until a later age. They can be detected either during cadaveric dissection [3,4], central venous cannulation [2] or when they have grown large enough to cause symptoms. In this presentation, a male presenting a enlarged JVA which was imitating a neck mass was reported and the importance of anatomical anomaly was emphasized.
Case presentation
A 48-yr-old man presented at the ENT clinic with a midline neck mass just above the manubrium sternum that had been present for years (Figure 1). The man had no history of trauma or cardiovascular diseases. He was healthy, had neither associated symptoms nor documented medical co-morbidities.
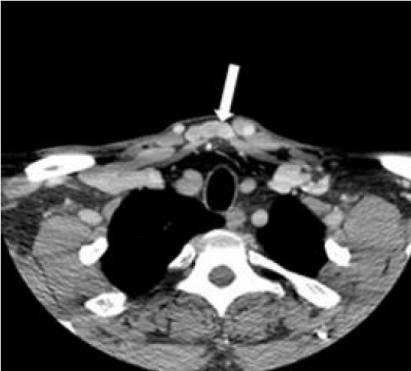
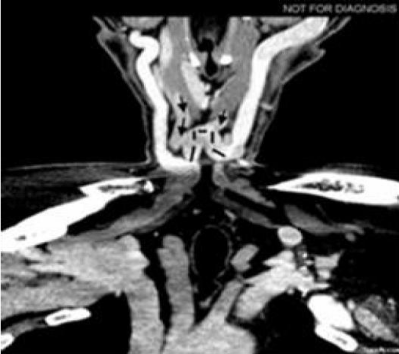
Clinical examination revealed a soft, compressible, painless mass on suprasternal space. The overlying skin was intact, and no lymphadenopathy was palpable. ENT and oral examination were normal. Clinical assessment clearly suggested a benign venous mass. A computed tomography angiography (CTA) of the head and neck was requested to expedite the diagnosis. The axial CTA of the root neck in the venous phase showed a median cervical swelling corresponding to a vein communicating between the two anterior jugular veins (Figure 2). The reconstruction in the coronal plane confimed an enlarged JVA (Figure 3).
Discussion
The venous drainage system of the head and neck region comprises superficial and deep veins. Deep veins drain into the internal jugular vein and the subclavian vein. Superficial veins ultimately open into the external and anterior jugular veins.
The Anterior Jugular Vein (AJV) typically emerges near the hyoid from the confluence of superficial submandibular veins. The AJV descends between the anterior midline and the anterior border of the Sternocleidomastoid Muscle (SCM). Near the root of the neck, it turns laterally, passes beneath the SCM, and drains into the termination of the external jugular vein or into the subclavian vein. Just above the sternum, each AJV gives off a branch towards its contralateral counterpart to form the JVA in the suprasternal space [5].
The two AJV communicate with the ipsilateral deep vein system and are interconnected through JVA, which provides an important collateral venous network across the midline of the upper anterior part of the thorax. In case of an obstruction of an innominate vein, blood travels through the JVA to the opposite side. Ergo, enlargement and tortuosity of collateral vessels (e.g., JVA) may be signs of associated venous occlusion [2,6].
Only a small fraction of variations involving JVA have been reported in the literature to the best of our knowledge. A case was reported where the JVA was abnormally large, doubled, and highly placed at the lower part of isthmus of the thyroid gland [4]. Another variation manifested as one AJV running in the midline of the neck, which is termed the median cervical vein [7]. Another reported case showed the left AJV crossing the midline to join with right AJV to form a common trunk. Besides, a small innominate vein arising from left AJV communicates with a small portion of commun trunk to form the JVA [3].
In the current case, the arch is abnormally large and lies just above the manubrium sternum, in the suprasternal space. This anomalous JVA may confuse the clinicians while interpreting the midline neck mass. However, the venous-phase CTA helped to confirm the diagnosis of this dilated JVA. Furthermore, we can infer from the patient’s clinical symptom that this is an anatomical anomaly of the JVA, which is subtly different from asymptomatic antomical variation thereof.
The case reported and its ensuing discussions advocated that JVA can show a high degree of anatomical variations. This kind of variation can cause considerable bleeding in thyroid surgeries and percutaneous tracheostomy. It can also be the source of malposition of the venous catheter, misinterpretation of the examination of cardiovascular system and complications in central venous catheterizations [1-3].
As a result and in order to avoid unforeseen and potential dangerous injuries, a good understanding of these variant anatomies is important for clinicians, radiologists, anesthesiologists and surgeons, and all practitioners performing diagnostic and surgical procedures in the head and neck area. Moreover, use of the venous-phase CTA prior to these procedures may be helpful.
Conclusion
Dilated JVA can manifest itself as midline neck mass and be a source of complications. Physicians should keep in mind these anatomical variations while interpreting neck masses and performing procedures involving this region to prevent unintended complications.
Compliance with ethical standards
Ethical standards: We state that the present report complies with the current laws of the country in which it was performed.
- McCormick B, Manara AR (2005) Mortality from percutaneous dilatational tracheostomy: A report of three cases. Anaesthesia 60: 490-495. Link: https://bit.ly/2RN8sHY
- Schummer W, Schummer C, Bredle D, Frober R (2004) The anterior jugular venous system: variability and clinical impact. Anesth Analg 99: 1625-1629. Link: https://bit.ly/2RIm5YL
- Premavathy D, Seppan P (2015) Anatomical variation in the anterior jugular veins and its clinical implications – A case report. Journal of the Anatomical Society of India 64: 40-43. Link: https://bit.ly/3zd6WQh
- Nayak BS (2006) Surgically important variations of the jugular vein. Clin Anat 19: 544-546. Link: https://bit.ly/3gojb3H
- Moore KL, Dalley AF, Agur AMR (2014) Clinically oriented anatomy (7th ed.). Lippincott Williams & Wilkins, Philadelphia. Link: https://bit.ly/3gpKb2R
- Chasen MH, Charnsangavej C (1998) Venous chest anatomy: clinical implications. Eur J Radiol 27: 2-14. Link: https://bit.ly/3pJ18d1
- Dalip D, Iwanaga J, Loukas M, Oskouian RJ, Tubbs RS (2018) Review of the Variations of the Superficial Veins of the Neck. Cureus 10: e2826. Link: https://bit.ly/3zl9hZu
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
