Archives of Otolaryngology and Rhinology
The supraclavicular artery island flap in oral cavity reconstruction
Khoi A Nguyen1*, Nhat D Nguyen1, Tam C Tran1 and Khuong H LeM1
2Oncology Hospital, Ho Chi Minh City, Vietnam
Cite this as
Nguyen KA, Nguyen ND, Tran TC, Le KH (2020) The supraclavicular artery island flap in oral cavity reconstruction. Arch Otolaryngol Rhinol 6(3): 088-090. DOI: 10.17352/2455-1759.000130Objective: To evaluate the advantages and disadvantages of the SAI flap as an alternative for free flap in reconstruction of oral cavity defects.
Methods: We report a case series of 21 patients undergoing reconstructive operation from January 2018, through September 2019 after ablation of oral cavity malignant tumor.
Results: Mean flap dimensions were 5.6 cm wide and 24.2 cm long. Harvest time was 30 – 45 min. There are 6 patients with minor dehiscence and 2 patients requiring prolonged wound care. We have 2 patients with partial skin flap necrosis and one patient having complete loss of the flap.
Conclusion: The SAI flap provides a reliable choice for oncologic defects of the oral cavity. This flap is easy to raise. However, it is difficult to reconstruct the complex oral cavity defects with the SAI flap because of the limited length and limited rotation arc.
Introduction
The Supraclavicular Artery Island (SAI) flap is a regional fasciocutaneous flap which is raised from skin on the supraclavicular and shoulder area for reconstruction of head and neck defects. Mütter first reported the application of medial-based random shoulder flaps in 1842 [1]. In 1979, The supraclavicular artery flap was described by Lamberty as an axial flap [2]. Until the late 1990s, Pallua described a detailed anatomy of the blood supply to this flap [3]. In their study, the supraclavicular artery is a branch of the transverse cervical artery. The paired venae comitantes joint the transverse cervical vein or the external jugular vein. The origin of the flap artery is found in the triangle formed from the external jugular vein, the posterior border of the sternocleidomastoid muscle, and the clavicle. In 2009, Chiu applied the SAI flap to reconstruct the oncologic defects of the head and neck.
We have used the SAI flap for the head and neck defects after tumor ablation since 2012. The objectives of our study were to evaluate the advantages and disadvantages of the SAI flap in reconstruction of oral cavity defects.
Methods
We have a case series of 21 consecutive patients of squamous cell carinoma whose oral cavity were reconstructed by the SAI flap after tumor ablation. All reconstructive cases were performed from January 2018 through September 2019. We had 9 cases of T3 tumor and 12 cases of T4 tumor, and all of our patients with cervical lymph node metastases N1-2.
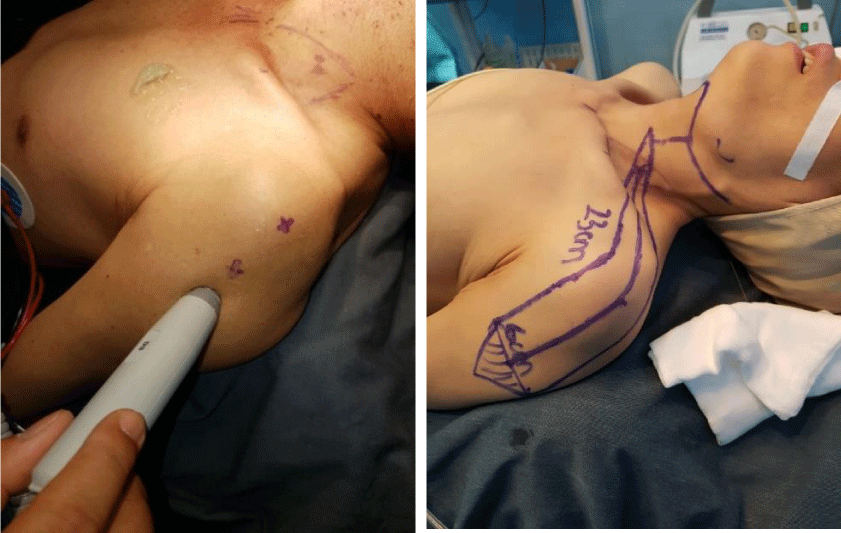
The Doppler probe is used to design the SAI flap based on the signals of the supraclavicular artery (Figure 1). This artery begins at a point 7 cm from the sternal notch and 2 cm from the clavicle posterior border. The vessels reach the acromion tip and run toward the elbow.
Mean follow-up was 6.3 (range, 3-24) months. Surgical information collected included defect location and size, flap size, levels of neck dissection, and duration to harvest the flap. In addition, complications and survival rate of the flap were recorded (Table 1).
Results
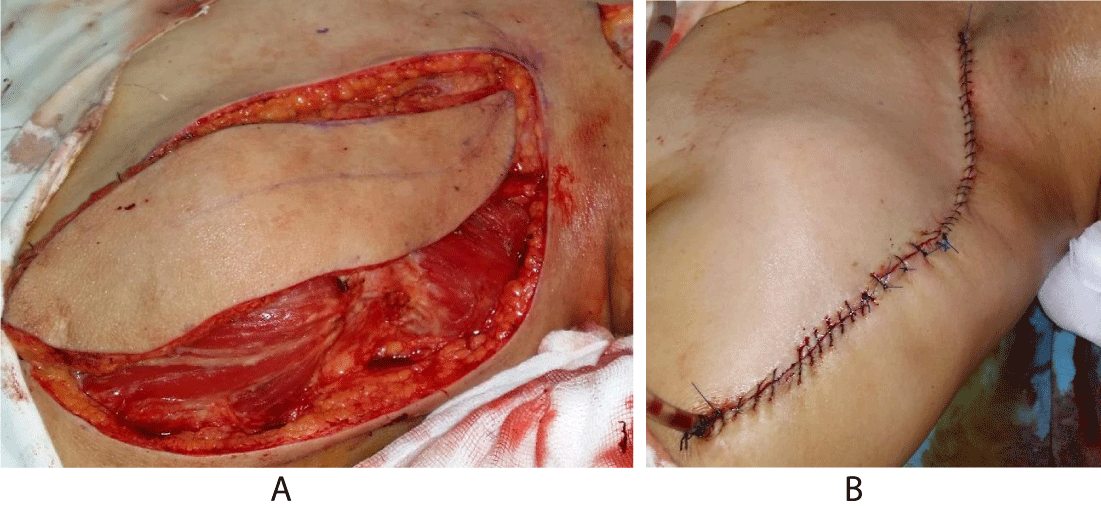
The mean length of the SAI flap was 24.6 cm (range, 23 - 27) (Figure 2), we de-epithelialized the proximal portion of the flap to fit the defect, medium skin paddle size was 51.2 cm2 (range, 48 - 54). Harvest duration was 38.9 minutes (range, 30 - 45).
We had 6 patients (28%) with minor donor-site dehiscence, whereas larger dehiscence occurred in 2 patients (19%). The donor-site wound of these two patients requires prolonged wound care. We have no case in which severe
limitations of arm movement was reported. We had 2 patients (19%) with partial skin flap necrosis, and one case (4.7%) with complete loss of the skin paddle. With total skin flap necrosis, in the case of total glossectomy, we have performed a second reconstructive procedure using pectoralis major flap.
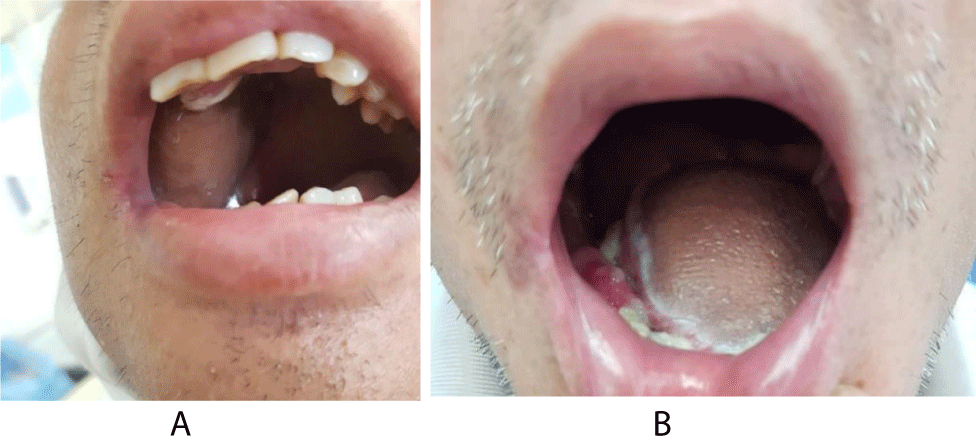
Four patients of ours (16%) acquire the complication of salivary fistula, all of the fistulas recovered spontaneously. All of our patients have accepted rehabilitation of speech and swallowing capacity (Figure 3).
Discussion
Among the choices of head and neck reconstruction, microvascular free flap is the standard of operation, the radial forearm flap and anterolateral thigh flap are considered the workhorse flaps. Free-tissue transfer is very reliable and versatile but requires technical expertise and longer surgery duration.
Our initial experience with the SAI flap has revealed this flap to be available for reconstructing a variety of oral cavity defects.
Niels Kokot, et al. have found the SAI flap to be safe, versatile, easy to harvest, and reliable for the head and neck defects [4]. Jay W. Granzow et al have supposed this flap to be thin, pliable fasciocutaneous regional flap [4].
According to the research of Niels Kokot on 45 patients, there are 8 cases (18%) of partial skin flap necrosis and 2 cases (4%) of total flap necrosis [3]. Our research has 9.5% partial flap necrosis and 4.8% total necrosis. Our SAI flap sizes are similar to those of the other authors [5].
The SAI flap has a long pedicle, so this flap can reach most of the oral cavity defects [6-8]. However, in some cases of complex three-dimensional defects, the SAI flap showed some shortcomings because of the rotational nature of the flap. If we try to stretch the flap to cover the defect, the tension combined with the rotation at the flap pedicle may compromise the distal skin paddle.
Conclusion
The SAI flap is reliable and versatile in reconstruction of oncologic defects of oral cavity and may be an alternative for free-tissue transfer in selected patients. However, the SAI flap has some disavantages because of its length and its rotational arc, so this flap is limited for some complex oral cavity defects.
- Mütter TD (1842) Case of deformity from burns relievedby operation. Am J Med Sci 4: 66.
- Lamberty BG (1979) The supra-clavicular axialpatterned flap. Br J Plast Surg 32: 207-212. Link: https://bit.ly/2EbcDqj
- Kokot N, Mazhar K, Reder LS (2013) The Supraclavicular Artery Island Flapin Head and Neck Reconstruction. JAMA Otolaryngol Head Neck Surg 139: 1247-1255. Link: https://bit.ly/3j29GH8
- Granzow JW, Suliman A, Roostaeian J, Perry A, Boyd JB (2009) The Supraclavicular Artery Island Flap (SCAIF) for Head and Neck Reconstruction: Surgical Technique and Refinements. Otolaryngol - Head Neck Surg 148: 933-940. Link: https://bit.ly/32kHhFx
- Chiu ES, Liu PH, Friedlander PL (2009) Supraclavicularartery island flap for head and neck oncologicreconstruction: indications, complications and
outcomes. Plast Reconstr Surg 124: 115-123. Link: https://bit.ly/3j96DNv - Alves HR, Ishida LC, Ishida LH, Besteiro JM, Gemperli R, et al. (2012) A clinical experience of the supraclavicular flap used toreconstruct head and neck defects in late stagecancer patients. J Plast Reconstr Aesthet Surg 65: 1350-1356. Link: https://bit.ly/3lcTQeH
- Lee SH, Cho HM, Kim JK, Nam W (2018) The supraclavicular artery island flap: a
salvage option for head and neck reconstruction. Maxillofac Plast Reconstr Surg 40: 25. Link: https://bit.ly/3lbTjK3 - Wong S, Brennan M, Nishikaw S, Lim JH (2019) Supraclavicular Artery Island Flap in Head and Neck Reconstruction: A Case Series and Literature Review. Perm J23. Link: https://bit.ly/3gnNky4
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
