Archives of Otolaryngology and Rhinology
Complete endoscopic removal of Maxillary Odontogenic Keratocyst: A case report
Shashikant Anil Pol1*, Surinder K Singhal2, Nitin Gupta3, Shalima PS4 and Himanshu C Bayad5
2Associate Professror and Head, Department of ENT, GMCH Chandigarh, UT, India
3Associate Professor, Department of ENT, GMCH Chandigarh, UT, India
4Junior Resident, Department of ENT, GMCH Chandigarh, UT, India
5Senior Resident, Department of ENT, GMCH Chandigarh, UT, India
Cite this as
Pol SA, Singhal SK, Gupta N, Shalima PS, Bayad HC (2020) Complete endoscopic removal of Maxillary Odontogenic Keratocyst: A case report. Arch Otolaryngol Rhinol 6(2): 049-051. DOI: 10.17352/2455-1759.000121Objective: To present a rare case of endoscopic removal of maxillary Odontogenic Keratocyst in a paediatric patient.
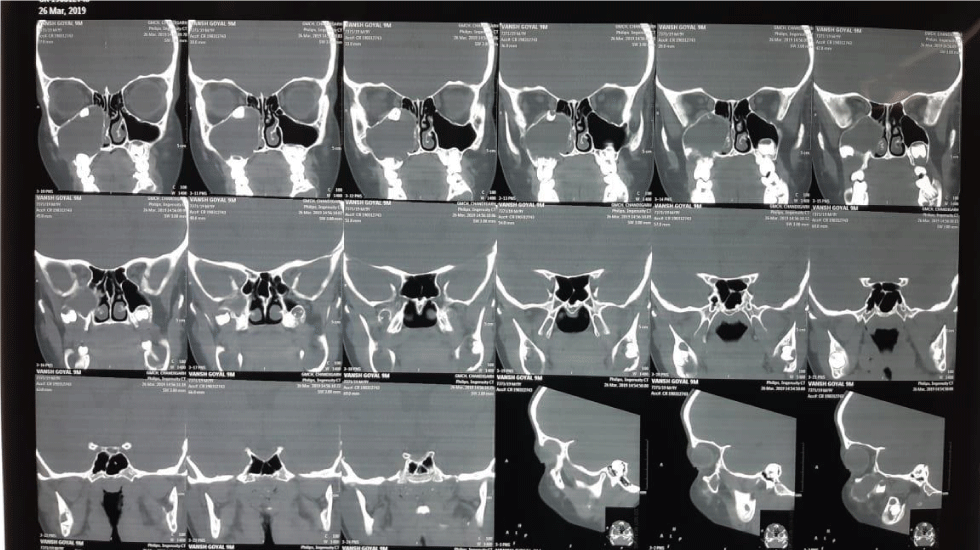
Case report: We are presenting the case of a 9 year old male, with chief complaint of swelling on right side of face for 5 months. It was not associated with decrease in vision or diplopia. On examination there was a single swelling of size 4×3 cm on right side of cheek, with smooth surface and firm consistency. Non Contrast Computed Tomography of nose and paranasal sinus showed expansile fluid density lesion completely filling right maxillary sinus with impacted tooth in superior part along the roof of maxillary sinus. Cyst wall with impacted tooth was removed completely by endoscopic approach without any need for Caldwell approach. Final histopathological report was odontogenic keratocyst. Patient is on regular follow up and is asymptomatic till date without any recurrence.
Conclusion: Odontogenic keratocyst should be considered as one of the differential diagnoses in any cystic swelling involving maxilla and mandible. CT scan is the main diagnostic modality to see the exact location and extent and also helps in planning the surgical approach. Endoscopic approach provide excellent surgical outcome with preservation of normal anatomy. Long term surveillance is required to look for any recurrence.
Introduction
Odontogenic Keratocyst (OKC) is a developmental, non-inflammatory cyst. It arises from cell rests of dental lamina according to latest WHO classification [1]. It was first described in 1956 by Philipsen [2]. Though a benign lesion, OKC is locally destructive with high recurrence rate of about 25 to 62.5% [1]. It is more commonly seen in mandible as compared to maxilla [3]. It is predominant in 2nd to 3rd decade with slight male preponderance. Though complete endoscopic removal is advantageous over open approach, it is rarely used for maxillary odontogenic keratocyst. Here we are presenting a case of a 9-year-old male patient with odontogenic keratocyst of maxilla, which was successfully excised by endoscopic approach.
Case report
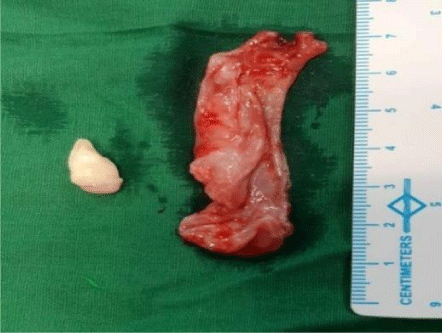
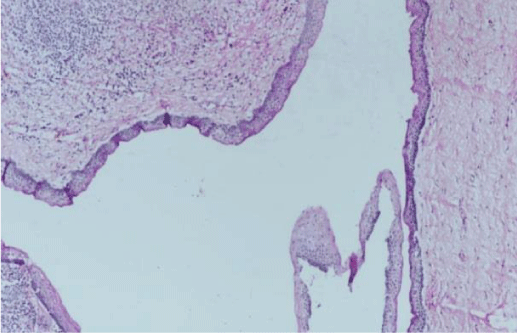
A 9 year old male presented to ENT OPD with chief complaint of swelling on right side of cheek for 5 months. On examination of face, there was a single swelling of 4x3cm on right side of cheek lateral to nose. It was extending superiorly just inferior to medial canthus, inferiorly till upper part of right alar cartilage, medially from lateral margin of nasal bone with obliteration of nasofacial groove and laterally just lateral to infraorbital foramen area (Figure 1). On palpation, it was found to be firm in consistency with smooth surface. All margins were regular. Overlying skin was pinchable and sensations were normal. Right alar margin was displaced inferiorly with bulge on right lateral wall of vestibule. Anterior rhinoscopy examination showed a bulge, on right lateral wall of nose almost, obscuring right nasal cavity. Non Contrast Computed Tomography scan of nose and paranasal sinus revealed multilocular expansile fluid density lesion with dependent hyperdense contents completely filling right maxillary sinus with tooth impacted in superior part along the roof of maxillary sinus (Figure 2). The differential diagnoses considered were dentigerous cysts, ameloblastoma, simple bone cyst, odontogenic myxoma. After taking informed and written consent from patient’s relatives in their own language, child was taken up for endoscopic excision under general anaesthesia (Figure 3). After thorough nasal decongestion, uncinectomy and wide middle meatal antrostomy was done to expose the cyst wall. Cyst was punctured to suction out whitish discharge. The whole cyst with tooth in the medial part of roof of maxillary sinus was removed in toto, taking adequate precaution to avoid damage to orbital floor (Figure 4). Cyst was just abutting the orbital floor and was attached to enamel/crown of right molar tooth. Anterior nasal packing was done. Post operative period was uneventful and vision was normal. Patient was discharged satisfactorily after pack removal on post operative day two. Histopathological evaluation showed cysts lined by stratified squamous epithelium showing palisaded hyperchromatic basal layer. Luminal surface shows corrugated parakeratotic epithelial cells along with keratinaceous debris suggestive of right maxillary odontogenic keratocyst (Figure 5). Patient is on regular follow up for 4 months and is doing fine without any recurrence or cosmetic deformity (Figure 6).
Discussion
Odontogenic keratocycst is one of the common jaw tumors and constitute about 4-10 percent of all odontogenic cysts. It has a bimodal age distribution with first peak in 2nd and 3rd decade and second peak in 5th decade or older [4]. It is more common in mandible as compared to maxilla [3]. Also, maxillary cysts are usually unilocular. But in our case, it was a multilocular maxillary cyst, that too in a 9 year old child. Carcinoma transformation is about 0.01-0.02 % [5]. Around 40% are associated with impacted teeth [6]. It may be seen as an incidental finding on radiographic evaluation [7]. Cysts are filled with keratinous debris. Odontogenic keratocyst are surgically removed by marsupialisation, enucleation and chemical curettage with carnoys solution. Cyst can be removed by open as well as endoscopic approach. We opted for an endoscopic approach because it offers minimal reductive change. It is advantageous for complete removal without the risk of damage to the ossification centers of maxilla and without any facial scar and subsequent cosmetic deformity. Patient should be followed up once a year for the first 5 years post-operation and once every 2 years thereafter, in view of the high recurrence rate of the disease. To the best of our knowledge, only two cases of complete endoscopic excision of maxillary odontogenic keratocyst has been described in the literature [8].
Conclusion
Odontogenic keratocyst should be considered as a differential diagnosis in cases of cystic swelling over jaw. Though it is more common in mandible, it is also seen in maxilla. CT scan is the main diagnostic modality to see the exact location and extent that helps in planning the surgical approach. Surgical excision is the only treatment of choice. Of late, endoscopic approach has become popular by virtue of its ability for complete removal without damaging the ossification centers of maxilla.
Consent for Publication
As we are working in a government institute it is our protocol to take consent from patient regarding both for the procedure and for publication purpose.
Authorship contribution
Shashikant Pol has made the manuscript, Surinder K Singhal was operating surgeon, Nitin Gupta has reviewed the manuscript, Shalima P.S. has collected the data for manuscript, Madhur Kalia has made the raw manuscript.
- Meara JG, Shah SS, Li KK, Cunnigham M (1998) The odontogenickeratocyst: a 20-year clinicopathologic review. Laryngoscope 108: 280-283. Link: https://bit.ly/35YfbBp
- Philipsen HP (1956) Om keratocyster (kolesteatom) I kaeberbe. Tandlaegebladet 60: 963-980.
- Fries G, Board FR, Woodburn RL, Service IR (2003) Dentistry 134: 877-883.
- Shear M (2007) Cysts of the oral and maxillofacial Regions. 4th edition. Blackwell Munksgaard 6-58.
- Jalali E, Ferneini EM, Rengasamy K, Tadinada A (2017) Squamous cell carcinoma arising within a maxillary odontogenic keratocyst: A rare occurrence. Imaging Sci Dent 47: 135-140. Link: https://bit.ly/2zt162I
- Newaskar V, Verma M, Rajmohan S, Dashore D (2016) KCOT occurring in bilateral maxillary sinus in non-syndromic patient. J Clin Diagn Res 10: ZD16-ZD18. Link: https://bit.ly/3crgH1g
- Marzella ML, Poon CY, Peck R (2000) Odontogenickeratocyst of the maxilla presenting as periodontal abscess. Singapore Dent J 23: 45-48. Link: https://bit.ly/2YTcmQE
- Marino MJ, Luong A, Yao WC, Citardi MJ (2018) Management of Odontogenic Cysts by Endonasal Endoscopic Techniques: A Systematic Review and Case Series. Am J Rhinol Allergy 32: 40-45. Link: https://bit.ly/2LnXRwh
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.




 Save to Mendeley
Save to Mendeley
