Archives of Nursing Practice and Care
Association of stress, anxiety and depression with the body mass index and the body image perception among medical students
Fateme Yavari1 and Esra Tajik2,3*
2Department of Community Nutrition, Faculty of Nutrition Sciences and Food Technology, Shahid Beheshti University of Medical Sciences, Tehran, Iran
3Psychiatry and Psychology Research Center, Tehran University of Medical Sciences, Tehran, Iran
Cite this as
Yavari F, Tajik E (2021) Association of stress, anxiety and depression with the body mass index and the body image perception among medical students. Arch Nurs Pract Care 7(1): 008-014. DOI: 10.17352/2581-4265.000054Introduction: Stress, anxiety, and depression are of high prevalence among all mental disorders. Their high prevalence among those students directly dealing with the public health, made us investigate the prevalence of these disorders and their related parameters such as the body mass index and body image perception among the medical students in Azad Medical University.
Materials and methods: This is a cross-sectional – analytical study conducted on 148 medical students (51 male and 97 female; average age 19.51±1.03 years) of the Azad Medical Sciences University of Tehran in their 1st to 7th semesters in a period between December and June 2017.. The students were given a questionnaire encompassing demographic information, 21-folded depression, anxiety, and stress index (DASS-21), and the questionnaire of the body image perception; and the participants’ height and weight data were also collected.
Results: 148 students filled in the questionnaires and 47%, 54% and 59.15% of them were diagnosed with depression, anxiety, and stress symptoms, respectively. These percentages were not significantly different between the basic medicals and physiopathology course groups. But the stress rate was lower among the physiopathology course group members (p=0.026). Furthermore, the BMI rate was normal in 61.5% of the students of the basic medicals courses and 71.9% of those of physiopathology courses. However, only 25.3% of the students perceived a correct image of their body, and this can provide grounds for the outbreak of depression among those students.
Conclusion: The present study revealed that the prevalence of depression, stress, and anxiety are high among medical students, and this makes them perceive an incorrect image of their body which should be studied. Therefore, regarding the results of this study, it is imperative to conduct more research on this group, so that the outcomes would be communicated with the relevant authorities and educational academies, in line with reducing the pressure on the students.
Abbreviations
BMI: Body Mass Index; EDA: Exploratory Data Analysis; CBS: Current Body Size; IBS: Ideal Body Size; DDBS: Degree of Dissatisfaction with the Body Size; DASS-21: The Depression, Anxiety and Stress 21 Scales; BM Students: Basic Medical Students; Pp students: Physiopathology students
Introduction
One of the most important issues studied by psychologists and health experts today is how to deal with the issues related to depression, stress, and anxiety [1]. According to the classification provided by the World Health Organization, more than half of the psychological disorders are associated with mental disorders such as stress, depression, and anxiety.
Depression is characterized by discomfort, loss of interest and anhedonia, feeling of guilt or low valor, sleep disturbance, appetite disturbance, feeling of fatigue, and poor concentration [2]. Depression can affect the job performance and social relations of the individuals [3]. This disorder involves many individuals in a manifest or latent way, to the extent where at final stages is accompanied by death and suicidal thoughts [4,5]. It is expected to rank first in disease burden in developed countries by 2030 [6].
Stress is associated with fatigue and stressful mood, which takes effect from internal and external factors. Scientists depict that the term stress cannot fit into just one definition, since it is a highly mental phenomenon. Stress may lead to physical and mental impairments and as observed in the studies, it can increase the risk of heart diseases and brain damages [7-11].
According to the World Health Organization’s announcement, it is estimated that in 2015, 4.4% and 3.6% of the world population suffers from depression syndromes, worriedness and anxiety symptoms respectively [2].
Depression can be observed in almost every age group (children, adolescents, young adults, adults, and elderly), every educational grade, and every social position. However, many studies have shown that mental diseases are more prevalent in females than in males [2]. Stress, anxiety, and depression are more common than other mental disorders among the students. Students are going through a certain age stage (from adolescence to adulthood). Entering society and becoming independent are also stressful [12,13]. Moreover, financial concerns among university students adversely affect their mental and physical health [14].
The students often encounter numerous stressors such as the pressure from the university, educational academies, and the families expecting high ranks and marks, unclear future, remoteness from the family for their studies, difficulties of entering into the employment market, and financial constraints, which are all among the issues considered as mental concerns among the majority of the students [16,17]. Regarding the above-mentioned, it may be stated that medical students’ health condition is of special importance, as they are in charge of public health.
In a review carried out to determine the prevalence of stress among the students of four medical faculties in Tehran in 2007, it was reported as being 40.7% [18] which is much higher than that of the general public. Firth-Coze also claims that young doctors and medical students suffer extreme rates of stress and depression compared to the general public [19]. The prevalence of stress in medical universities of some countries are as follows, based on the undertaken studies: 30% medical students in Europe [20,21], 31.2% in the universities of Britain, 41.9% in Malaysia [15] and 61.4% in Thailand [22].
One of the factors that can cause a person to be isolated from society during adolescence and the onset of mental disorders is the standards imposed on the body appearance. During adolescence, people are very concerned about their appearance and overweight. Girls are looking for a lean body and boys are looking for a muscular and being taller. Distancing themselves from these standards imposed on communities can affect the prevalence of mental disorders [23]. Negative attitude towards body image perception can even affect dietary patterns and cause physical diseases especially it is more common in women [24].
A variety of studies have shown that the individuals’ perception of their body image is not proportionate to their BMI, but it is a subject of mental origin and other factors including the family, friends, culture, society, level of individual awareness, and male and female biological aspects are effective, which is the ground for mental problems such as depression, stress, and anxiety [25].
Due to the potential expectations they have about themselves and their families, their training in conformity with accepting the responsibility of the patients’ welfare, and because of their university courses and long hospital shifts, medical students are unable to spend reasonable time on recreational activities and therefore they are prone to suffer from anxiety and depression [26,27].
Hence, considering that this group of university students would become members of the medical staff and must be in good physical and mental health and conditions to deliver desirable services, we resolved to study on depression, anxiety, and stress prevalence and their association with the body mass and the body image perception among the medical students of basic medicals and physiopathology groups at the Azad Medical University of Tehran. This is to take a step forward in the promotion of the mental health of the medical students with the relevant authorities’ assistance.
Methods
This is a cross-sectional and descriptive-analytical study conducted between December and June 2017 on 153 students of Azad Medical Sciences University of Tehran. A minimum of 145 respondents was required for this study based on prevalence (29.1%) of anxiety among university students in Iran, a confidence level of 95% and a margin of error of 5% [28]. The participants were randomly selected from among the students of basic medicals and physiopathology disciplines, provided with questionnaires to collect the required data from them. After finalizing the data collection, five questionnaires were taken out of the samples, as they were not fully answered and failed to reach the statistical competence criteria. This made the final sample size become 148.
Data collection was carried out after obtaining the written consent of the students and giving them a detailed explanation of the study purposes. The means of data collection for this research included three stages of demographic information questionnaire, the questionnaire of depression, anxiety, and stress symptoms index (DASS-21), and the body image perception test.
It has been hypothesized that stress, anxiety, and depression have association with BMI and the body image perception among medical students.
The demographic information questionnaire encompassed information such as age, gender, course (physiopathology and basic medicals), height, and weight.
DASS-21 questionnaire was employed to study the students’ stress, anxiety, and depression status. This measure was prepared by Lovinband in 1995 and was tested on a large human sample [29]. It includes 21 questions in a way that each of the depression, anxiety, and stress factors are measures by 7 questions. This questionnaire is a tool with a 4-folded spectrum, options of which are denominated from 0 to 3. The value of 0 to 14 scores obtained by the means of this questionnaire is normal within the scope of stress and if it exceeds 15, that would be considered as abnormal stress. The DASS-21 test is validated for the Iranian population by Sahebi, et al. [30] and Moradi Panah [31].
The participants’ height and weight was measured and their body mass index (BMI) was classified as follows:
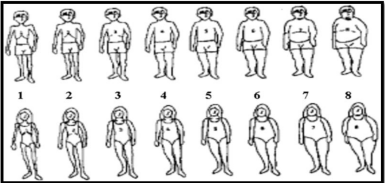
The questionnaire of body image perception includes 8 shapes that represent the general view of the body shape [32]. Its spectrum ranges from 1 to 8 (extremely thin to obese). The participants select among eight shapes the one that best corresponds to the current size of their body (CBS). This selected shape shows the contour they believe they are. Additionally, they select a shape that best corresponds to their Ideal Body Size (IBS). The degree of dissatisfaction with the body size (DDBS) is yielded through the formula of CBS minus IBS. The DDBS score indicates the degree of dissatisfaction of the body shape, therefore a positive score means that the individual wants to lose weight, and the negative score indicates their tendency for gaining weight.
Statistical analysis
The data were analyzed by the statistical software (SPSS ver. 23.0). The normality and homogeneity of the data were investigated through Exploratory Data Analysis (EDA). The descriptive figures such as frequency, percentage, and the average ± standard deviation for categorical and continuous variables were used. Moreover, the t-test and the chi-square test were used to compare the continuous variables and categorical variables respectively. The Pearson correlation coefficient was used to determine the relationship between the variables. The significance level was adjusted at p<0.05.
Results
The rate of response in this study was 96.7% and the data for 148 medial students (51 male and 97 female) were analyzed. Table 1 indicates the demographic information and the mental health conditions of the participants among male and female students of basic medicals and physiopathology disciplines. The age average of participants was 19.51±1.03 years and no significant difference existed among males (19.61±2.11 years) and females (19.44±1.05 years), and p = 0.415. The number of basic medicals course students (54.7 percent) was more than that of the physiopathology students (45.2 percent) and this difference was not significant in terms of gender (p>0.05) (Table 1).
Moreover, Table 1 shows that although there is no difference in terms of BMI categories between the two groups of students, 61.5% of the basic medicals students and 71.9% of the physiopathology students were in the normal BMI range, while 21.8% and 25% of them overweighed respectively. There was no obesity among the physiopathology students, but one of the students was at the border of obesity. According to the results, only 25.3% of the students perceived a normal image of their body, and 21.2% and 53.5% of them conceived themselves as obese or thin (Table 1).
Furthermore, Table 1 shows that there is no significant difference between the basic medicals and physiopathology students in terms of prevalence of depression and anxiety symptoms (p<0.05), although the difference of stress symptoms was significant between two groups (p=0.019) (Table 1).
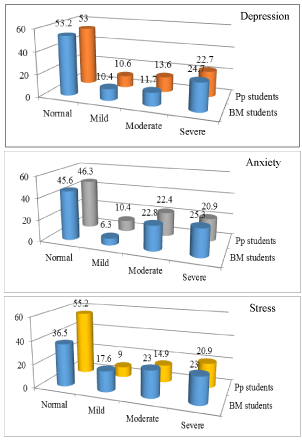
Figure 1 shows that more than half of the students (53.2 percent of the basic medicals students and 53 percent of physiopathology students) had no depression symptoms and this was less than half in case of anxiety (45.6 percent of the basic medicals students and 3.46 percent of physiopathology students). However, the normal level of stress symptoms among physiopathology students was higher than the basic medicals students (55.2 for 36.5 percent respectively) (0=0.026). There was no significant difference between the two groups of the students for other intensities of depression, anxiety, and stress (Figure 2).
Table 2 shows the significant and positive relationship between depression symptoms and anxiety (p<0.001, r=0.41), depression and stress symptoms (p<0.001, r=0.49), anxiety and stress symptoms (p<0.001, r=0.46), and the body image and BMI (p<0.001, r=0.30). Besides, there was a negative relationship between stress symptoms and education (p=0.013, r=-0.18) (Table 2).
Discussion
The present study carried out on 148 medical students of basic medicals (semesters 1 to 5) and physiopathology (semesters 6 and 7) courses showed that about 47%, 54%, and about 59.15% of the medical students had depression, anxiety, and stress symptoms respectively. Mental symptoms of depression, anxiety, and stress are reported among medical students from around the world. Fawzy et al. have also reported respectively 65%, 73%, and 59.9% of depression, anxiety, and stress levels among 700 medical students in Egypt [17]. In their systematic review carried out by means of a study in 2006 on depression, anxiety and other mental distress symptoms among American and Canadian medical students, and also by reviewing 40 articles published in this regard, Dyrbye et al. concluded that depression and anxiety have a high prevalence among medical students. This is generally more prevalent in comparison with the general public such that according to some articles, before entering into medical education, the said students were similar to the general public in terms of mental disorders prevalence [27]. This rate is depicted as being 15-25% among the general public [33].
Many of the different challenges the universities and colleges create to promote the educational status of the students, and the belief that the students’ performance would go better by heavy competition lead to heavy pressures on and negative outcomes by the students [34]. Surbhi Sidana states in a study, that educational performance is related to the level of depression, and those students obtaining better marks are more exposed to mental pressures and depression [35].
In their study in 15 US universities on 8488 students in 2012, Eisenberg et al. reported that 22% of the students show depression symptoms in the acute phase [36].
In different studies conducted in Iran, the rate of depression prevalence was reported as follows: Eslami, et al. [37] and Kelyani, et al. [38] have reported this percentage as being 53.1%. The medical education system of some countries such as Iran, India, etc. bear several unique and different properties compared to other countries, such that the procedure of the students’ qualification is dependent on their marks and ranks obtained in special examinations, while in the Western countries this qualification is considered based on the personal statements and interests, interviews and extracurricular history, in addition to other factors such as voluntary services or participation in research programs [39]. This can be a reason for the higher prevalence of stress, anxiety, and depression among the Iranian and Indian students.
Just like the results obtained from some other studies, no significant difference was observed in mental disorders prevalence among females and males in the present study [40,41], while this rate is found to be higher among women in some of the studies [2,25,42,43].
Recent studies also reveal the prevalence of depression along different stages of medical education [43]. We have also found results showing 46.8% prevalence during the first two years and 47% in the third year. In a study carried out in Mecca, the depression and stress prevalence among the third-year medical students was reported to be more than those of the second year [43]. However, the depression prevalence was not significantly different among the second and third-year students in our study, while the stress prevalence among the second-year students was higher than those in their third year. This can be due to the basic medicals course exams and the pressure exerted as a result of the intensity of the courses during the first two years of medical education in Iran. Moreover, the first-year medical students are under more pressure due to shifting from high school to the university, passing a difficult entrance exam, emotional issues as a result of remoteness from the families, and their tendency for independence. Dyrbye et al. believe that the depression prevalence rate reduces in some of the years of medical educations courses due to the medical students’ age, variety of courses in the medical education, and also depression measurement methods [32]. Some other studies also remind this fact [44,45].
The depression rate among the medical students may also be consequent to substance abuse, suicidal thoughts [45,46], weakness in their professional performance [32,47], and dissatisfaction about their body image [48].
Some articles have raised the relationship between body image dissatisfaction and depression [48]. One noticeable point here is that like we have also found in this study, body image perception has a relationship with the individuals’ BMI. Those individuals who become sensitive about their body image, get a negative impression about themselves which is a stressor situation for which a significant relationship was observed in this study so that the greater BMI the individuals had, the fatter they perceived their body image. This may also lead to an outbreak of depression symptoms [49].
Fatness, excess weight, and being underweight are known to be the factors related to the body image perception among adolescents. That is, unhealthy weight control behaviors and low-quality nutritional diet is observed among those adolescents with an abnormal perception about their body image which is also harmful to their mental health [50]. The adolescents’ nutrition condition in the present study showed that 58.1% of the participants were within the normal limits of BMI, but only 38.2% of them had a correct perception of their body images. An incorrect perception about body image may lead to poor eating habits and bears consequences for the individual’s health. On the other hand, several studies have shown that exercise and physical movement may increase awareness about the body and satisfaction with the body image [51-53].
There are some strengths and limitations for the current study. The strong points are newness of the survey to combine psychological factors and nutritional factors among medical students in Tehran, and also results on body image perception among medical students which is not any available data in Iran. However, the lack of the study is the limited time and limited budget to do the larger size of sampling and generalization to the other medical faculties in Tehran. Further researches can provide some data on a bigger sample size and other university students rather than medical students to identify some more significant associations. There are more basic factors to affect students and threat their mental health.
Conclusion
We have demonstrated cross-sectional relationship between BMI and body image perception with the symptoms of some mental disorders. Junior students were at risk for stress symptoms. The high prevalence of stress and depression among medical students compared to the general population can be related to academic stress and low self-awareness. On the other hand, since according to the current study body image perception as a psychological factor in most participants was abnormal, self-awareness and self-confidence courses should be requirement. Despite the limitations, this study may prepare some bases for researchers to develop studies on the association between stress and depression with more probable factors.
Ethics approval and consent to participate
The project got ethic approval from the ethical committee of faculty of medical sciences, Azad Medical University of Tehran. Furthermore, after a short explanation at the beginning of the data collection, written consent forms were delivered and collected from participants.
- Shao R, He P, Ling B, Tan L, Xu L, et al. (2020) Prevalence of depression and anxiety and correlations between depression, anxiety, family functioning, social support and coping styles among Chinese medical students . BMC Psychol 8: 38. Link: http://bit.ly/3uMe4AN
- WHO (2017) Depression and Other Common Mental Disorders Global Health Estimates, booklet, Geneva, Switzerland. Link: http://bit.ly/3kCCjwL
- Public Health Agency of Canada (2012) Mood disorders. In: The human face of mental health and mental illness in Canada. 2006. Ottawa (ON): The Agency 57-70. Link: https://bit.ly/3bXCXB2
- Makhubela M (2021) Suicide and depression in university students: a possible epidemic. South African Journal of Psychology. Link: http://bit.ly/3qaTw1i
- Errazuriz A, Crisostomo N (2021) Prevalence of depression in Latin America and the Caribbean: protocol for a systematic review and meta-analysis. JBI Evid Synth 19: 201–207. Link: http://bit.ly/2Ok7y3j
- Mathers CD, Loncar D (2006) Projections of global mortality and burden of disease from 2002 to 2030. PLoS Med 3: e442. Link: http://bit.ly/2NU8eg0
- Sahebi A, Asghari MJ, Salari RS (2005) Validity of depression, anxiety and stress scale (DASS21) for an Iranian population. Iranian Psychologist Journal 4: 299-312. Link: http://bit.ly/3uI8ijA
- Rahimi Ahmadabadi S, Hejazi A, Attaran H, Rahimi A, Kohestani L, et al. (2016) Comparison of stress, anxiety, depression & sexual role in subjects involved gender dysphoria with normal subjects. IJFM 22: 67-75. Link: http://bit.ly/3qcIAAa
- Albert MA, Durazo EM, Slopen N, Zaslavsky AM, Buring JE, et al. (2017) Cumulative psychological stress and cardiovascular disease risk in middle aged and older women: Rationale, design, and baseline characteristics. Am Heart J 192: 1-12. Link: http://bit.ly/3bcmRo2
- Sapolsky RM (2014) Why zebras don't get ulcers: The acclaimed guide to stress, stress-related diseases, and coping-now revised and updated. Holt paperbacks 37: 71.
- Jones F, Bright J, Clow A (2001) Stress: myth, theory, and research, Pearson Education 1-4. Link: http://bit.ly/3e0fFgx
- Ghafari M, Sharifirad GR, Zanjani S, Hassanzadeh A (2012) Stress, anxiety and depression levels among elderly referrals to Tehran Elderly Club. Iranian Journal of Ageing 7: 53-59. Link: http://bit.ly/3qbRf6f
- Buchanan JL (2012) Prevention of depression in the college student Population: a review of the literature. Arch Psychiatric Nurs 26: 21-42. Link: http://bit.ly/3sOyZl3
- Jessop DC, Reid M, Solomon L (2020) Financial concern predicts deteriorations in mental and physical health among university students. Psychol Heal 35: 196-209. Link: http://bit.ly/3q6HJB3
- Sherina MS, Rampal L, Kaneson N (2004) Psychological stress among undergraduate medical students. Med J Malaysia 59: 207-211. Link: http://bit.ly/3uX7CqX
- Brenneisen Mayer F, Souza Santos I, Silveira PS, Itaqui Lopes MH, de Souza AR, et al. (2016) Factors associated to depression and anxiety in medical students: a multicenter study. BMC Med Educ 16: 282. Link: http://bit.ly/3bWcXG7
- Fawzy M, Hamed SA (2017) Prevalence of psychological stress, depression and anxiety among medical students in Egypt. Psychiatry Res 255: 186-194. Link: http://bit.ly/3bXEHdy
- Shariati M, Yunesian M, Vash JH (2007) Mental health of medical students, a cross-sectional study in Tehran. Psychol Rep 100: 346-354. Link: http://bit.ly/308esvi
- Firth-cozens J (1989) Stress in medical undergreduated and house officers. Br J Hosp Med 41: 161-164. Link: http://bit.ly/2OcPXdM
- Moutinho IL, Maddalena NC, Roland RK, Lucchetti AL, Tibiriçá SH, et al. (2017) Depression, stress and anxiety in medical students: a crosssectional comparison between students from different semesters. Rev Assoc Med Bras 63: 21-28. Link: http://bit.ly/3uNeuXC
- Haldorsen H, Bak NH, Dissing A, Petersson B (2014) Stress and symptoms of depression among medical students at the University of Copenhagen. Scand J Public Health 42: 89-95. Link: http://bit.ly/3sK4axP
- Rehmani N, Khan QA, Fatima SS (2018) Stress, anxiety and depression in students of a private medical school in Karachi, Pakistan. Pak J Med Sci 34: 696-701. Link: http://bit.ly/2Pl9hGc
- Soares Filho LC, Batista RFL, Cardoso VC, Simões VMF, Santos AM, et al. (2021) Body image dissatisfaction and symptoms of depression disorder in adolescents. Braz J Med Biol Res 54: e10397. Link: http://bit.ly/305cL1V
- Tayfur SN, Evrensel A (2020) Investigation of the relationships between eating attitudes, body image and depression among Turkish university students. Riv Psichiatr 55: 90-97. Link: http://bit.ly/3b7VdbI
- Aline R, Sabine R, Tina L, Monika E (2016) Is body weight dissatisfaction a predictor of depression independent of body mass index, sex and age? Results of a cross-sectional study. BMC Public Health 16: 863. Link: http://bit.ly/3b94DDG
- Sood R (2008) Medical education in India. Med Teach 30: 585-591. Link: http://bit.ly/3rfLFB8
- Dyrbye LN, Thomas MR, Shanafelt TD (2006) Systematic review of depression, anxiety and other indicators of psychological distress among US and Canadian medical students. Acad Med 81: 354-373. Link: http://bit.ly/2OlXZRO
- Jamali H, Ghalenoei M, Aval MY, Taban E, Kolahdouzi M, et al. (2017) Prevalence of anxiety among environmental and occupational health students in Qazvin University of Medical Sciences Iran, in 2015. JOHE 6: 128-135. Link: https://bit.ly/3kDlWzO
- Lovibond SH, Lovibond PF (1996) The Dass: Manual for the Depression, Anxiety Stress Scales. Sydney, Australia: Psychology Foundation of Australia.
- Sahebi A, Asghari MJ, Salari RS (2005) Validation of Depression Anxiety and Stress Scale (DASS-21) for an Iranian Population. Jouranl Developemental Psychology 4: 299-312. Link: http://bit.ly/303H0WO
- Moradipanah F (2015) Effect of light music on depression, Anxiety and stress (DASS-21) for Iranian population [master degree]. Iran Tarbiat Modarres University of Tehran.
- Childress AC, Jarrell MP, Brewerton TD (1993) The Kids’ Eating Disorders Survey (KEDS): Internal Consistency, Test-Retest Validity and Reliability. Eating Disorders 1: 123-133. Link: https://bit.ly/3kFfEzH
- Kaplan HI, Sadock BJ (1998) Synopsis of psychiatry, book, London.
- Naidoo S, Van Wyk J, Higgins-Opitz SB, Moodley K (2014) An evaluation of stress in medical students at a South African university. South African Family Practice 56: 258-262. Link: https://bit.ly/3e2XJlf
- Sidana S, Kishore J, Ghosh V, Gulati D, Jiloha R, et al. (2012) Prevalence of depression in students of a medical college in New Delhi: A cross-sectional study. Australas Med J 5: 247–250. Link: http://bit.ly/2MFe0S7
- Eisenberg D, Chung H (2012) Depression treatment among college students in the United States. General hospital psychiatry 34: 213-220.
- Kalani N, Akbar RE, Kooti W, Abadi NA, marzoni HZ (2015) The study of depression prevalence among the students of Jahrom University of medical science in 2013. Zanko J Med Sci 15: 58-66. Link: http://bit.ly/3e4iJIg
- Najafi Kayani M, Pourjam E, Jamshidi N, Karimi S, Najafi kalyani V (2013) Survey of stress, anxiety, depression and self-concept of students of Fasa University of medical sciences 2010. J Fasa Univ Med Sci 3: 235-340. Link: http://bit.ly/3q5tzAg
- Jayakrishnan T, Honhar M, Jolly GP, Abraham JTJ (2012) Medical education in India: time to make some change. Natl Med J India 23: 164-167. Link: http://bit.ly/3baghOH
- Akbari M, Nejat AH, Dastorani SM, Rouhani A (2011) Evaluation of Stress Level and Related Factors among Students of Mashhad Dental School (Iran) in Academic Year of 2008-2009. J Mash Dent Sch 35: 165-176. Link: http://bit.ly/2NUYq5z
- Khan MS, Mahmood S, Badshah A, Ali SU, Jamal Y (2006) Prevalence of depression, anxiety and their associated factors among medical students in Karachi, Pakistan. J Pack Med Assoc 56: 583-586. Link: http://bit.ly/3bQioX6
- Lqbal S, Gupta S, Venkatarao E (2015) Stress, anxiety & depression among medical undergraduate students & their socio-demographic correlates. Indian J Med Res 141: 354-357. Link: http://bit.ly/3sH3J7m
- Aboalshamat Kh, Hou XY, Strodl E (2015) Psychological well-being status among medical and dental students in Makkah, Saudi Arabia: a cross-sectional study. Med Teach 37: 75-81. Link: http://bit.ly/2NXw0HZ
- Jadoon NA, Yaqoob R, Shehzad MA, Zeshan SC (2010) Anxiety and depression among medical students: a cross-sectional study. J Pak Med Assoc 60: 699-702. Link: http://bit.ly/3e38ZhJ
- Puthran R, Zhang MW, Tam WW, Ho RC (2016) Prevalence of depression amongst medical students: a meta-analysis. Med Educ 50: 456-468. Link: http://bit.ly/3e9PgwV
- Moir F, Yielder J, Sanson J, Chen Y (2018) Depression in medical students: current insights. Adv Med Educ Pract 9: 323-333. Link: http://bit.ly/3q5utwE
- Dyrbye LN, Thomas MN, Shanafelt TD (2005) Medical student distress: causes, consequences, and proposed solutions. Mayo Clin Proc 80: 1613-1622. Link: http://bit.ly/385KcFJ
- Neumark-Sztainer D, Hannan PJ, Eisenberg ME (2006) Body Dissatisfaction Prospectively Predicts Depressive Mood and Low Self-Esteem in Adolescent Girls and Boys. J Clin Child Adolesc Psychol 35: 539-549. Link: http://bit.ly/2Ohd9rg
- Gaskin JL, et al. (2013) Perception or reality of body weight: Which matters to the depressive symptoms. J Affect Disord 150: 350-355. Link: http://bit.ly/3bSI1Xq
- Duong HT, Roberts RE (2014) Perceived weight in youths and risk of overweight or obesity six years later. J Psychosom Res 76: 23-27. Link: http://bit.ly/3q6MnPv
- Kantanista A, Osiński W, Borowiec J, Tomczak M, Król-Zielińska M, et al. (2015) Body image, BMI, and physical activity in girls and boys aged 14–16 years. Body Image 15: 40-43. Link: http://bit.ly/3815wMv
- Dan SP, Mohd Nasir MT, Zalilah MS (2011) Determination of Factors Associated with Physical Activity Levels among Adolescents Attending School in Kuantan, Malaysia. Mal J Nutr 17: 175-187. Link: http://bit.ly/3rgARCE
- Fox KR (1999) The influence of physical activity on mental well-being. Public Health Nutr 2: 411-418. Link: http://bit.ly/3bRqcYC

Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.
 Save to Mendeley
Save to Mendeley
