Archives of Nursing Practice and Care
Reaching Out: Supporting Families and Carers Bereaved During COVID-19
Barbara von Barsewisch*, Su Yin Yap and Bernie Byrne
Cite this as
Barsewisch BV, Yap SY, Byrne B (2020) Reaching Out: Supporting Families and Carers Bereaved During COVID-19. Arch Nurs Pract Care 6(1): 049-050. DOI: 10.17352/2581-4265.000049Background
The past few months of responding to COVID-19 were undoubtedly a challenging time. The North Middlesex University Hospital in North London experienced an early peak of deaths from Covid-19. With no visiting allowed to keeo the footfall through the hospital as low as possible, patients and their families were unable to share the final days or hours and were unable to say goodbye. In response, Su Yin Yap, the Lead for clinical health psychology and Bernie Byrne, the interim Macmillan lead nurse for cancer, set up a project of reaching out and supporting families and carers bereaved during this time.
At the beginning of the global pandemic of COVID-19, there was a peak of deaths from the middle of March to the middle of April 2020 at the North Middlesex University Hospital . Approximately 40% of the usual annual deaths occurred within a 5 week period.
In line with national guidance, rules on hospital visiting were changed significantly in order to protect people from the spread of the virus. All visiting was stopped and, as a result, many patients died without family present, leaving families and loved ones without the opportunity to say goodbye.
Due to the nature of the virus, patients with COVID-19 often deteriorated rapidly and died within a short timeframe. Restrictions around social distancing and travel meant that bereaved families may not have had the same access to their usual support network and religious rituals around death and burial. These factors increase the risk of a traumatic bereavement. In light of the challenges presented during COVID-19, it was recognised that there was a need to respond rapidly to the unique and unprecedented challenges faced by relatives of the deceased.
Aims
The aim of the project was to design a pathway of support for Next of Kin (NOK) of adults who died in North Middlesex University Hospital (NMUH) during the pandemic.
The support included written resources, telephone support and clinical follow up when required. A further aim was to gather feedback from bereaved NOK’s to improve future practice.
Methods
A Process Map was designed outlining the pathway for the Bereavement Phone Support.
A proforma for calls was designed using Agile principles, with flexibility, scalability and adaptability a key to the formulation.
A Bereavement Support Information Booklet ‘Supporting People Through Bereavement and Grief’ was written and produced specifically with the NMUH patient cohort in mind. A skilled workforce was mobilized to provide telephone support to the bereaved. Previous advanced communication skills’ training was a prerequisite for being able to join the team.
There were weekly peer supervision meetings established via MicrosoftTeams for debriefing. These sessions were also an opportunity to decide on amendments to the original proforma in order to both guide the calls and to help gather information such as specific themes and needs which were voiced.
The project aligned with a hospital initiative of sending a bereavement card and knitted heart from the community to all bereaved NOK. As well as offering each family an interdenominational candle lighting ceremony. When necessary a clinical follow-up team responded to NOK queries that were medical and /or specialist in nature.
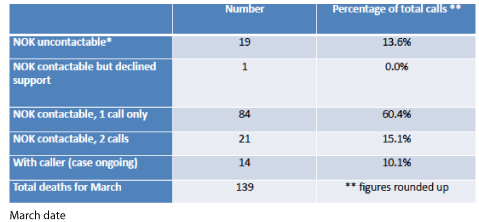
Results for a march audit (see below)
Results show that telephone support was established in the majority of cases.
Reaching out to families was appreciated, and feedback from calls indicated that the majority of Next of Kin were grateful to receive telephone support from the hospital.
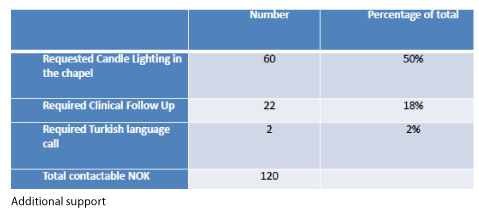
The candle lighting ceremony was appreciated by bereaved families, with half opting for this service. Furthermore the team could respond to identifying the needs of the BAME (Black, Asian and minority ethnic) community: The Bereavement Support team was able to provide calls in English and Spanish. Turkish language was identified as an area of need and thus a Turkish speaking staff member with the requisite skills and knowledge was approached and recruited to the team.
After approximately 300 supportive calls were made by August 2020, the project was temporarily halted. A business case has been submitted for a new fixed term contract position to take over the project and lead on the calls. As the pandemic is far from over, theneed for this project to continue remains a vital contribution to the holistic care offered by the hospital.
Reflection
As a haematology clinical nurse specialist I decided to join the small bereavement support team. For each of us, the bereavement support work was done on top of our own busy jobs. I often made time at the end of the day as I did not know how long a conversation might take. Working with a proforma to support and structure the phone calls, much assistance from a dedicated administrative team supporting this work and weekly peer supervision, I asked for my first ‘allocation’. It was and remained tense dialling a number without knowing the family and which way the conversation would unfold. In my own clinical work I deal with bad news, death and grief regularly, but I know my patients, their families, often their neighbours or even the cat’s name. It is easier to be there and listen when the family is familiar with me and know all the work and indeed hope for a patient’s good outcome that has gone into a patient’s treatment and care.
It was both a hard and rewarding commitment to be part of the support team. Many phone calls were raw with the next of kin’s heartache. Their recurrent theme was the pain of not being with the loved one at the time of death, not being able to hold their hand or tell them that they are loved. Many relatives asked who was with their relative at the time of their passing, and whether a nurse held their hand. There has been praise for some doctors and nurses who facilitated phone calls during critical times when generally relatives found communication insufficient. However, there was always the on-going challenge of how best to help people deal with the ‘unknown’ that arises when someone cannot be physically present in the hospital to witness the changes in their loved one and observe the care and interventions given to the patient. People react to this in many different ways, often accompanied by other reactions to loss such as anger and depression.
Equally I had good conversations, when relatives shared extraordinary life stories, or complicated dynamics that somehow seemed to unravel at this stage to form a different understanding to that which went before. There have been anecdotes and insights that made us smile, and invariably there was respect for every life lost to Covid-19. But whether a phone call was emotionally harder or easier for me to make to was beside the point. The overriding feeling was that it was a privilege to be part of the project at this critical time - to let relatives know that we acknowledge their loss and that we are sorry that we could do no more.
Conclusion
The Bereavement Support Project offered families of our deceased patients a much needed connection with the hospital. One of the key pieces of feedback received from families is how difficult they found not having any communication with the hospital following the admission of their loved one and their subsequent death. The learning from this project is being fed back into the relevant teams and departments across the hospital. The project is an excellent example of cross-departmental and multi-professional working. All of the Bereavement Support eam were also fulfilling their own roles as well as contributing to the service. As such, it constitutes excellent value for money for the Hospital.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.
 Save to Mendeley
Save to Mendeley
