Annals of Musculoskeletal Medicine
Functional outcomes and rehabilitation efficiency in patients with restricted weight-bearing
Meredith Ogilvie-Brown* and Tik Chan
Cite this as
Brown MO, Chan T (2019) Functional outcomes and rehabilitation efficiency in patients with restricted weight-bearing. Ann Musculoskelet Med 3(2): 006-010. DOI: 10.17352/amm.000016Orthopaedic injuries can require a period of restricted weight-bearing which can increase inpatient hospital admissions and place the patient at risk of the complications of immobility. This study aimed to identify the functional outcomes and rehabilitation efficiency for patients admitted to rehabilitation with restricted weight bearing.
Method: Patients admitted to Brighton Rehabilitation Unit between 1 January 2015 to 31 December 2016 with weight-bearing restrictions for either upper or lower limbs were included in the study. Analysis of data for LOS, duration of restriction, complications and Functional Independent Measure scores were used to compare to all the admissions to the unit during 2015.
Results: There was a significant difference between LOS of patients with restricted weight bearing (52.57 days) compared to the general rehabilitation population (37.3 days) (p=0.0002). The average FIM change of NWB group (24.6) was comparable to average FIM of the general rehabilitation population. Only 23% were discharged home with weight bearing restrictions and the rest required NWB to be upgraded before discharge. Thirty-one admissions (28%) were complicated by urinary tract infection.
Conclusion: Restricted weight bearing increases rehabilitation LOS and patients are unlikely to discharge home with these restrictions in place. The admissions were complicated by a high incidence of urinary tract infection. Once allowed to weight bear, most of these patients were able to discharge home and were functionally better on discharge when compared to the general rehabilitation patients.
Orthopaedic injuries and procedures can require a period of restricted weight-bearing to allow healing to occur before returning to normal activity. This can lead to lengthy hospital admissions and socioeconomic problems if the patient is unable to safely manage at home [1].
Extended hospital admissions are detrimental to both the patient and the economy. Long hospital stays increase costs for the health service and reduced bed turnover impairs access to services. Patients may find their health adversely affected by the immobility of restricted-weight bearing, with complications such as deconditioning, sarcopenia, deep venous thrombosis (DVT), constipation, pressure injury and urinary tract infection (UTI) [2]. Non-weight-bearing status itself is a risk factor for the development of venous thromboembolism [3]. Both upper and lower limb non-weight-bearing can impact on a person’s ability to mobilise if they require their upper limb to assist in rising from a chair or weight-bearing with a mobility aid.
Patients may be allowed to “partial”- or “touch- weight-bear” however this does not necessarily enable the patient to be discharged from hospital earlier than “non-weight-bearing status”. Many studies have shown that patients and healthy volunteers are unable to successfully keep to the restriction [4-6]. This prevents hospital discharge if the patient is not able to mobilise according to the orthopaedic instructions.
Rehabilitation during the period of immobilization after ankle fracture, for example, has not previously been shown to be beneficial [7]. A review of the literature failed to find data regarding length of stay for patients who have restricted weight-bearing. This study aims to identify the functional outcomes and rehabilitation efficiency for patients admitted to a rehabilitation unit with restricted weight-bearing, by examining length of stay, discharge destination, Functional Independence Measure (FIM) change and efficiency. It was hypothesised that patients who are required to comply with a period of restricted weight-bearing would have an increased rehabilitation length of stay and reduced rehabilitation efficiency when compared to the general rehabilitation unit population.
Method
The study was undertaken at Brighton Rehabilitation Unit, a 50 bed, Level 4 subacute rehabilitation facility in Queensland, Australia. The unit provides a multidisciplinary rehabilitation service with rehabilitation physicians, a geriatrician, nursing and allied health staff. It admits the majority of patients from the Metro North Health Service district who are unable to be discharged directly from the acute ward due to restricted weight-bearing. Ethics approval was granted by The Prince Charles Hospital Human Research Ethics Committee.
The investigators conducted a manual review of all referrals to Brighton Rehabilitation Unit from 1 January 2015 to 31 December 2016. Patients were included for upper limb fractures if they were required to be non-weight-bearing or have motion restricted by a device e.g. sling. Lower limb fractures were included if the patient was required to be “non-weight-bearing”, “touch-weight-bearing” or “partial-weight-bearing”.
Patients were excluded if they had not completed their rehabilitation by 31 December 2016, if they died during the rehabilitation admission, discharged against the advice of the medical team prior to completing their rehabilitation or if they were transferred to another hospital for acute surgical or medical management and subsequently discharged by the acute facility.
For the patients meeting the inclusion criteria, data was collected for: age, gender, comorbidities, home situation, date of acute admission or surgery, date of rehabilitation admission, date weight bearing was upgraded to “weight-bear as tolerated” or “full weight-bear”, rehabilitation discharge date, and FIM scores at admission and discharge from rehabilitation. For analysis, patients were divided into “Upper Limb”, “Lower Limb” and “Multitrauma” groups, with patients having one affected limb being allocated to the upper or lower limb groups and patients with two or more affected limbs being allocated to the multitrauma group.
Analysis was conducted using the Student t test to determine the significances comparing the included patients to the total admissions for the whole unit and between the groups.
Results
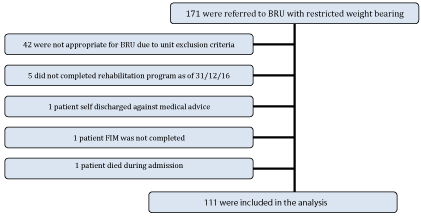
One hundred and seventy-one patients were referred to Brighton Rehabilitation Unit with a weight-bearing restriction (82 in 2015 and 88 in 2016) figure 1. All patients referred where community-dwellers prior to admission. Forty-two patients were not admitted and 5 patients were excluded because they had not completed their rehabilitation as of 31 December 2016. One patient died during the rehabilitation admission, 1 patient self-discharged against medical advice and the discharge FIM was missing for 1 patient. The total number of patients admitted to the rehabilitation unit for any condition in 2015 was 401.
One hundred and eleven patients were included in the analysis. Their average age was 71.77 years, 76 (69%) were female and 54 (49%) were living alone prior to admission table 1. The 111 patients included accounted for 4,082 days of restricted weight-bearing over the 2 years. The total length of stay for these 111 patients was 5,836 days table 2. On average, patients spent 36.77 days (5.1 weeks) with restricted weight-bearing during the rehabilitation admission and were discharged 15.80 days (2.3 weeks) after their weight-bearing status was upgraded. The average length of stay was 52.57 (+/-42) days. There was a significant difference between LOS of the all the patients admitted to Brighton when compared to the patients with restricted weight-bearing (p= 0.0002) table 3.
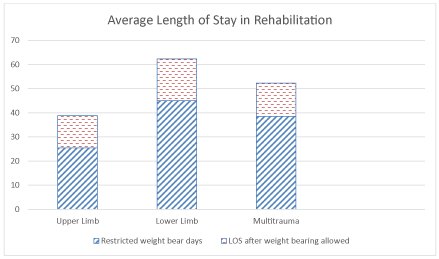
The upper limb group had the shortest average length of stay with 38.85 (+/-23) days compared with 62.39 (+/-66) days for the lower limb group and 52.28 (+/-18) days for the multitrauma group (see table 2). Once allowed to weight bear, the lower limb group required longer to achieve adequate function for discharge (average 17.32 days) than the other groups. This was significant when compared to the upper limb group (p= 0.0169) table 4 but not with the multi trauma group (p= 0.259). The difference in LOS between the upper limb group (38.83 days) and multitrauma group (52.28 days) was not significant (p=0.546) (Figure 2).
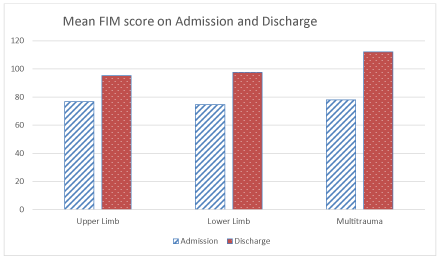
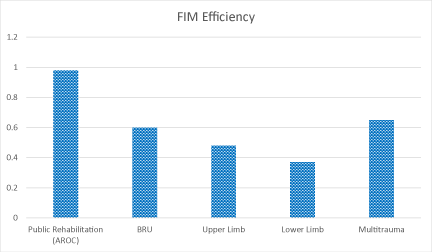
The average admission FIM for all RWB patients was 75.77 with an average FIM change of 24.60. The average FIM efficiency was 0.44. The differences of FIM efficiency between the groups did not reach significance (upper limb vs multi trauma p= 0.283; lower limb vs multi trauma p= 0.229 and upper limb vs lower limb p= 0.921). There was a significant difference when FIM efficiency of the RWB group was compared to all the BRU admissions (p=0.0001). The FIM change for upper limb (18.55) vs multi trauma (34.12) was significant (p=0.001) whereas comparing FIM change of lower limb (22.83) vs upper limb was not significant (p=0.43) (Figures 3,4).
Thirty-one patients (28%) had their rehabilitation admissions complicated by UTI – 4 in upper limb, 20 in lower limb and 7 in the multi-trauma group. Other complications documented in the discharge summaries included cellulitis, pulmonary embolus, falls, wound infections, ileus, pressure area, norovirus infections.
One hundred and one patients (91%) were discharged to the community (93 to their own home and 8 to a different home with friends or relatives). Seven patients (6%) were discharged to Residential Care Facilities and 2 to a slow-stream inpatient rehabilitation program for ongoing therapy prior to eventual discharge home. Twenty-five patients (23%) were discharged while non-weight bearing: 2 in the multi trauma group (8%), 8 in the upper limb group (40%) and 15 in the lower limb group (23%) which included 10 of the lower limb who were discharged prior to orthopaedic review and 5 who were upgraded from non-weight-bearing to partial-weight-bearing.
Discussion
The patients in the current study required significantly longer periods of inpatient rehabilitation when compared to the general rehabilitation population. Hospitalisation contributes the majority of the costs that are associated with injuries such as hip fractures [8]. Therefore, it is in the financial interests of the health service to reduce length of stay. A previous study found that, when compared to weight bearing recommendations from the literature, full weight bearing was only prescribed in 51% of cases [9]. There is significant variation amongst orthopaedic surgeons with respect to selecting the period of non-weight-bearing after ankle fracture, for example [10]. This suggests that more patients could be allowed to weight bear earlier and thus reduce hospitalization costs. There is growing evidence that early weight-bearing can lead to faster rehabilitation and early return to work and daily activities [11-14].
The Rest Easy Study [15], found that early mobilisation and the general health of the patient were the most predictive of a short hospital LOS. The presence of two or more comorbidities and female gender have previously been shown to be risk factors for the loss of autonomy following an ankle fracture [16]. Eight-six percent of our included patients had 2 or more comorbidities and 68% were female. All patients in the upper limb group had 2 or more comorbidities. This could have represented overall frailty in the group and may be the reason that the patients with upper limb restricted weight bearing were not able to be discharged home immediately after the acute admission [17]. The upper limb group had significantly more comorbidities than the other groups, but this group also had a shorter length of stay, so in this study, it was unlikely that the number of comorbidities influenced the results.
The mean FIM efficiency for the whole group was lower than the mean FIM efficiency for patients with orthopaedic fractures in public rehabilitation units (0.44 vs 0.98) [18]. In addition, the FIM efficiency for the restricted-weight-bearing patients was less than the FIM efficiency for the whole rehabilitation unit (0.44 vs 0.6). However, the FIM efficiency was significantly higher in the multitrauma group compared to the upper limb and lower limb groups and was comparable to that of the general Brighton patient population. It could therefore be appropriate to consider patients with multitrauma for rehabilitation despite reduced weight-bearing status. Patients with single limb fractures and multiple comorbidities have poorer rehabilitation potential according to our results. Unfortunately, the lower limb group was larger than the upper limb group which affected the results reaching significance for length of stay.
Depressive symptoms have previously been associated with frailty [19]. Seventeen (15%) of the included patients had a diagnosis of depression. This number may have been more if this was tested prospectively rather than relying on patient records for diagnosis and subsequently, may have been a confounder to the length of stay and FIM efficiency scores [20].
When reviewing the referrals, it was found that the referrers did not necessarily state that the upper limb fracture was non-weight bearing and this had to be inferred due to the use of an immobilisation device. Upper limb fractures were included in this study because the authors had observed that patients were not able to be discharged if they are unable to use their arm for activities of daily living or mobilise safely using an assistive mobility device e.g. four-wheeled walker. The current study confirmed this observation, as 60% of patients with upper limb restrictions were not able to be discharged while those restrictions were in place.
The results of this study have not previously been reported. A literature search of Medline, PubMed and CINAHL failed to identify previous studies that have investigated the effect of weight bearing status on rehabilitation length of stay. The current study is limited by its small cohort and single centre, retrospective design as this limited the content and accuracy of the data.
Conclusion
Restricted weight bearing increases rehabilitation LOS and patients are unlikely to discharge home with these restrictions in place. The resulting rehabilitation admissions were longer than the general rehabilitation population and complicated by a high number of urinary tract infections. Although the functional gains made during the rehabilitation stay are comparable to the general rehabilitation population, the LOS of cohorts with restricted weight bearing is significantly longer, with the lower limb group requiring much longer LOS than the upper limb group. Once allowed to weight bear, most of these patients were able to discharge home and were functionally better on discharge when compared to the general rehabilitation patients. More funding should therefore be allocated to patients with restricted weight bearing, in particular, those with lower limb fractures. Further research is needed to enable rehabilitation physicians to prospectively identify those patients who would benefit from a rehabilitation program whilst restricted with respect to weight bearing status.
- Srinivasan CM, Moran CG (2001) Internal fixation of ankle fractures in the very elderly. Injury 32: 559-563. Link: http://bit.ly/2LODCJp
- Allen C, Glasziou P, Del Mar C (1999) Bedrest: a potentially harmful treatment needing more careful evaluation. Lancet 354: 1229-1233. Link: http://bit.ly/2LhZ2zo
- Horner D (2001) Towards evidence-based emergency medicine: best BETs from the Manchester Royal Infirmary. Evidence exists to guide thromboembolic prophylaxis in ambulatory patients with temporary lower limb immobilisation. Emerg Med J 28: 718-720. Link: http://bit.ly/2LPXlbW
- Vasarhelyi A, Baumert T, Fritsch C, Hopfenmuller W, Gradl G, et al. (2006) Partial weight bearing after surgery for fractures of the lower extremity - is it achievable? Gait Posture 23: 99-105. Link: http://bit.ly/2NRmXaL
- Ebert JR, Ackland TR, Lloyd DG, Wood DJ (2008) Accuracy of partial weight bearing after autologous chondrocyte implantation. Arch Phys Med Rehabil 89: 1528-1534. Link: http://bit.ly/2XIyca4
- Mason LW, Dodds A (2010) A prospective study comparing attempted weight bearing in fiberglass below-knee casts and prefabricated pneumatic braces. Foot Ankle Spec 3: 64-66. Link: http://bit.ly/2Lf55Vr
- Lin CW, Donkers NA, Refshauge KM, Beckenkamp PR, Khera K, et al. (2012) Rehabilitation for ankle fractures in adults. Cochrane Database Syst Rev 11: CD005595. Link: http://bit.ly/2LQAWLo
- Ebert JR, Ackland TR, Lloyd DG, Wood DJ (2008) Accuracy of partial weight bearing after autologous chondrocyte implantation. Arch Phys Med Rehabil 89: 1528-1534. Link: http://bit.ly/2XIyca4
- Mammel JA, Haugen JL, Buckley RE (2008) Weight bearing orders after hip fracture surgery: a quality assurance project. Orthop Nurs 12: 151-158. Link: http://bit.ly/2JRjFiP
- Swart E, Bezhani H, Greisberg J, Vosseller JT (2015) How long should patients be kept non-weight bearing after ankle fracture fixation? A survey of OTA and AOFAS members. Injury. 46: 1127-1130. Link: http://bit.ly/2YQ0pbv
- Black JDJ, Bhavikatti M, Al-Hadithy N, Hakmi A, Kitson J (2013) Early weight-bearing in operatively fixed ankle fractures: A systematic review. Foot 23: 78-85. Link: http://bit.ly/2G7i7jq
- Smeeing DPJ, Houwert RM, Briet JP, Kelder JC, Segers MJM, et al. (2015) Weight-bearing and mobilization in the postoperative care of ankle fractures: a systematic review and meta-analysis of randomized controlled trials and cohort studies. PLoS One 10: e0118320. Link: http://bit.ly/2YNFhT7
- Tan EW, Sirisreetreerux N, Paez AG, Parks BG, Schon LC, et al. (2016) Early weightbearing after operatively treated ankle fractures. Foot Ankle Int 37: 652-658. Link: http://bit.ly/2YP8ey7
- Dehghan N, McKee MD, Jenkinson RJ, Schemitsch EH, Stas V, et al. (2016) Early weightbearing and range of motion vs non-weightbearing and immobilization after open reduction and internal fixation of unstable ankle fractures. J Orthop Trauma 30: 341-352. Link: http://bit.ly/2XHYt8m
- Borqquist L, Lindelow G, Thorngre KG (1991) Costs of hip fracture. Rehabilitation of 180 patients in primary health care. Act Orthop Scand 62: 39-48. Link: http://bit.ly/2XYVMPg
- Gauthé R, Desseauz A, Rony L, Tarissi N, Dujardin F (2016) Ankle fractures in the elderly: Treatment and results in 477 patients. Orthop Traumatol Surg Res 102: S241-244. Link: http://bit.ly/2JDxIIt
- Winograd CH, Gerety MB, Chung M, Goldstein MK, Dominguez F, et al. (1991) Screening for frailty: criteria and predictors of outcomes. J Am Geriatr Soc 39: 778-784. Link: http://bit.ly/2Y2d8Lc
- Australasian Rehabilitation Outcomes Centre (2017) AROC FIM Splat Report. University of Woolloongong. Link: http://bit.ly/2XGaC93
- Fugate Woods N, LaCroix AZ, Gray SL, Aragaki A, Cochrane BB, et al. (2005) Frailty: Emergence and Consequences in Women Aged 65 and Older in the Women's Health Initiative Observational Study. J Am Geriatr Soc 53: 1321–1330. Link: http://bit.ly/2XHxJos
- Hershkovitz A, Kalandariov Z, Hermush V, Weiss R, Brill (2007) Factors Affecting Short-Term Rehabilitation Outcomes of Disabled Elderly Patients With Proximal Hip Fracture. Arch Phys Med Rehabil 88: 916–921. Link: http://bit.ly/2XXX5Ot
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
