Archives of Hepatitis Research
Sarcoidosis-Lymphoma Syndrome presenting by severe Cholestatic Hepatitis
Omkolsoum M Alhaddad1, Maha M Elsabaawy1*, Omar A Shaarawy1, Nermine A Ehsan2, Doha Maher2, Khaled Gmeel1, Eman A Rewisha1 and Imam A Waked1
2Departments of Pathology, National Liver Institute, Menoufia University, Shebin El Kom 234511, Egypt
Cite this as
Alhaddad OM, Elsabaawy MM, Shaarawy OA, Ehsan NA, Maher D, et al. (2017) Sarcoidosis-Lymphoma Syndrome presenting by severe Cholestatic Hepatitis. Archives of Hepatitis Research 3(2): 023-026 DOI: 10.17352/ahr.000012Severe cholestatic hepatitis is an uncommon presentation of either sarcoidosis or Hodgkin lymphoma. Sarcoidosis lymphoma syndrome is a rare disorder with sarcoidosis heralding the onset of lymphoma. Here we report a case of coexisting sarcoidosis-Hodgkin’s lymphoma syndrome presenting with severe cholestatic hepatitis.
Introduction
Sarcoidosis is a multisystem disorder thought to be a result of exaggerated granulomatous reaction to an indeterminate antigen in genetically predisposed persons [1]. Tissue histopathology and comprehensive evaluation are prerequisites of definitive diagnosis [2].
Lungs and hilar lymph nodes are the most common sites responsible for the symptomatic disease [3]. Liver affection in sarcoidosis has been variably reported at rates of 11 to 80%, mostly in the form of elevated serum alkaline phosphatase and gamma glutamyl transpeptidase [4]. Clinically evident liver dysfunction occurs at lower rates, even in those with numerous hepatic granulomas [5]. In patients with sarcoidosis, cholestatic hepatitis is rarely seen [6].
Liver dysfunction in lymphoma is common mostly due to drug related hepatotoxicity or hepatic infiltration [7]. In a rare occasion, lymphoma presents by ductopenia related cholestasis as a paraneoplastic phenomenon [8].
An association between sarcoidosis and lymphoma labeled the sarcoidosis lymphoma syndrome) had been described in case reports since decades [9,10]. In the majority of these reports; sarcoidosis was followed by lymphoma, and exceptionally both coexisting together [11].
Case Presentation
37 years old gentleman presented with a three month history of high grade fever, mostly by night accompanied by profuse sweating with brief days of relieve on antipyretics and antibiotics. One month later, he had started to itch and noticed mild jaundice along with remarkable loss of appetite and weight.
The patient presented to National Liver Institute (NLI) hospital with fever, jaundice, hepatomegaly, and normal cardiopulmonary examination. Initial clinical and laboratory evaluation indicated presence of cholestatic hepatitis as shown in table 1. Ultrasound and magnetic resonance cholangiopancreatography (MRCP) excluded the presence of extrahepatic biliary obstruction as well as any hepatosplenic focal lesions or infiltration.
The patient was negative for hepatitis B surface antigen( HBS Ag), antibody to hepatitis B core IgM (anti-HBC IgM) , antibody to hepatitis B core IgG (anti-HBC IgG), hepatitis C antibody (HCV Ab), and polymerase chain reaction (PCR) for HCV-RNA, hepatitis A virus antibody (anti-HAV IgM), hepatitis E virus antibody (anti-HEV IgM), human immunodeficiency virus antibody (HIV Ab), Epstien Barr virus IgM antibody (EBV IgM), cytomegalovirus IgM antibody (CMV IgM), and herpes simplex IgM antibody (HSV IgM).
Autoantibodies were negative (anti- smooth-muscle antibody (ASMA), antinuclear antibody (ANA), perinuclear anti-neutrophil cytoplasmic antigen (P-ANCA), anti-liver kidney microsomal antibody (anti-LKM), and anti-mitochondrial antibody (AMA). Levels of Alphafetoprotien, carcinoembryonic antigen (CEA) and CA19.9 all were in the normal range. Repeated testing for salmonellosis and brucellosis were negative, and cultures of blood, urine and stool did not grow pathogenic organisms.
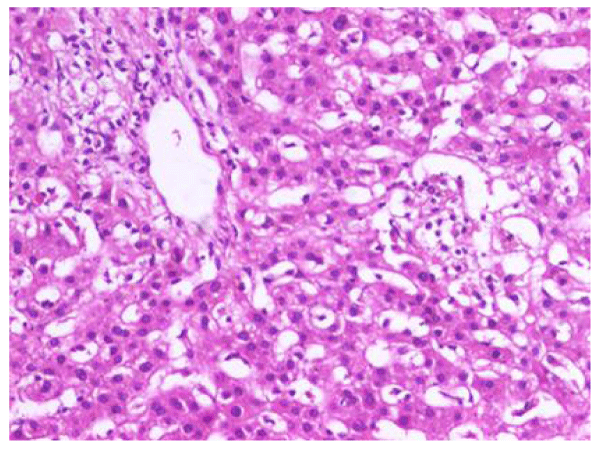
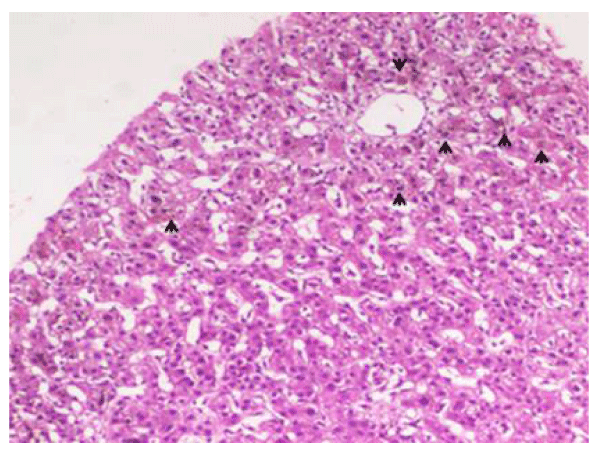
By the second week of admission, follow up laboratory data showed persistence of high cholestatic parameters and further rise in serum ferritin (Table 1). CT scanning showed homogenous non-enhancing enlarged right lower deep cervical and paratracheal lymph nodes (size around 1 cm with no calcification or degeneration, bright hepatomegaly with normal pancreatobiliary system and gall bladder. Histopathological examination of a liver biopsy specimen showed a preserved lobular architecture with expanded portal tracts by periportal fibrosis with mononuclear infiltration, with evident destruction of bile ducts. Parenchyma showed cholestasis with cholestatic rosettes. Portal and parenchymal epithelioid non caseating granulomas were also seen (Figures 1,2). These features strongly suggested the diagnosis of sarcoidosis; which was supported by elevated serum angiotensin converting enzyme (ACE). Prednisolone 60 mg daily was initiated.
By the third week, there was moderate clinical and marked biochemical improvement, including decrease levels of ACE and some sonographic evidence of attenuation of cervical adenopathy.
By the fourth week, fever recurred, right sided deep cervical lymph nodes and the spleen became palpable, and biochemical tests of cholestatic increased. Positron emission tomography (PET)-CT scan showed metabolically active mediastinal, cervical, splenic hilum, left gastric, portahepatis, celiac, portocaval, mesenteric, paraaortic, left internal and external iliac lymph nodes, along with splenic, hepatic, and bone marrow lesions, a picture highly suggestive of lymphoma (Figure 3).
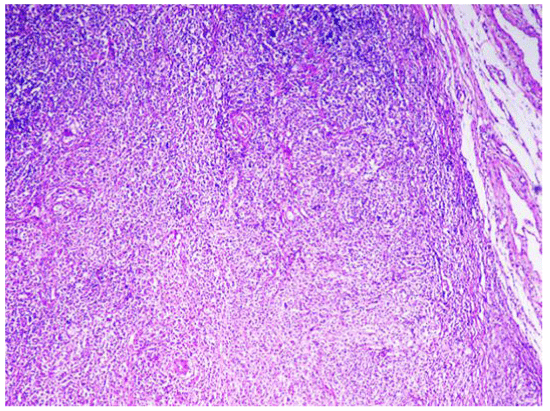
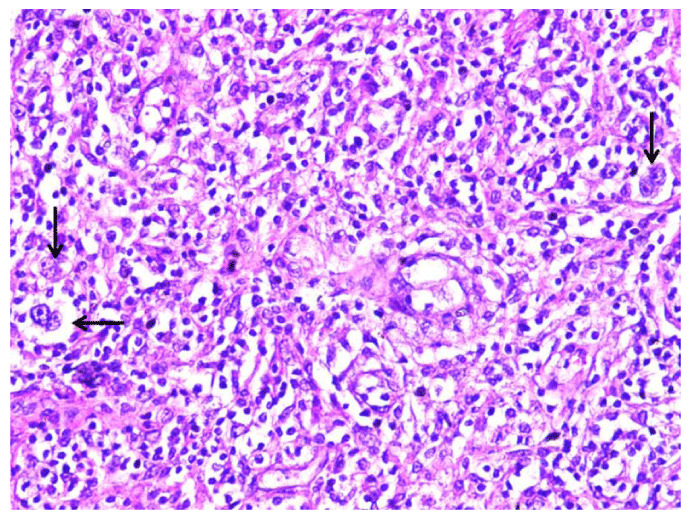
A right cervical lymph node was surgically removed. Lymph nodal effacement with the characteristic Reed Sternberg cells was seen, and Hodgkin lymphoma, nodular sclerosis type diagnosed (Figures 4,5) He was referred to oncology to receive specific treatment.
Protein, ESR: erythrocyte sedimentation rate, LDH: lactate dehydrogenase, ACE: angiotensin converting enzyme
Discussion
Sarcoidosis typically presents as non-caseating epithelioid granuloma. The finding of sarcoid granulomas in the liver is frequent; however, severe hepatic affection is rare [5].
In contrast to sarcoidosis, cholestasis is frequent in lymphoma and could carry poor prognosis [7]. Lymphoma associated cholestasis is mainly due to bile duct compression by a nodal mass or extensive hepatic infiltration [12]. Stauffer’s syndrome, a rare phenomenon, is cholestasis in absence of metastases in patients with renal cell carcinoma and some other cancers [8]. A variant of Stauffer’s syndrome; icteric hepatic dysfunction, had been described in Hodgkin’s lymphoma mostly due to ductopenia as the underlying pathology [13,14]. Lymphoma related cholestasis in absence of ductopenia is rarely reported and has shown better prognosis [15,16].
The occurrence of lymphoma in the context of sarcoidosis, the so called sarcodiososis lymphoma syndrome, has been observed since decades. An early study reported an 11-fold increase in lymphoma cases among patients with sarcoidosis [9]. When sarcoidosis precedes lymphoma as in the most, or coexisting as in fewer cases, a delay in diagnosing lymphoma can be troublesome [17].
Being a rare manifestation of sarcoidosis, the presence of cholestatic hepatitis in this case raised the possibility of other etiologies, and viral, toxic, and autoimmune disorders were excluded. Presence of non-caseating granulomas in liver tissue and elevated ACE, along with initially clear pulmonary imaging were the reason for early diagnosing the case as isolated hepatic sarcoidosis. Early clinical improvement on steroids with drop of serum levels of ACE and inflammatory markers supported the diagnosis.
However, in this case; the regression of initial improvement together with the rapidly appearing cervical adenopathy and enlarged spleen questioned the diagnosis of simple sarcoidosis.
In most commentaries of sarcoidosis-lymphoma syndrome (SLS), sarcoidosis was of mild severity, with favorable clinical responses in treated cases [18].
The presence of non-caseating granulomas in lymph nodes draining solid tumors has been mentioned in the literature, labeled sarcoid reaction. However absence of clinical and biological features of sarcoidosis remains the mainstay of differentiation between sarcoid reaction and true sarcoidosis [19]. In this patient, histopathological examination of cervical lymph nodes revealed presence of Hodgkin’s lymphoma of nodular sclerosis variety.
Sharquie et al., considered sarcoidosis and lymphoma as a continuum of one disease entity, considering it either sarcoidosis evolving to lymphoma or lymphoma presented by sarcoidosis [20].
Presenting by severe cholestatic hepatitis, this case presented a new spectrum of sarcoidosis lymphoma state. Liver biopsy in this case showed evidence of bile duct destruction but it didn’t satisfy the definition of vanishing bile duct syndrome; requiring loss of interlobular bile ducts in more than 50% of portal tracts [21].
Conclusively, for the acknowledged sequential linkage between lymphoma and sarcoidosis, the likelihood of yet evolving disease should be considered in every single case of sarcoidosis or lymphoma.
Consent
An informed consent for publication was taken from the patient
- Gezer NS, Başara I, Altay C, Rocher L, Karabulut N, et al. (2015) Abdominal sarcoidosis: cross-sectional imaging findings. Diagn Interv Radiol 21: 111–117. Link: https://goo.gl/blyKKt
- Judson MA, Boan AD, Lackland DT (2012) The clinical course of sarcoidosis: presentation, diagnosis, and treatment in a large white and black cohort in the United States. Sarcoidosis Vasc Diffuse Lung Dis 29: 119-27. Link: https://goo.gl/mfTvV3
- Baughman R, Teirstein A, Judson M, Rossman MD, Yeager H, et al. (2001) Clinical characteristics of patients in a case control study of sarcoidosis. Am J Respir Crit Care Med 164: 1885–1889. Link: https://goo.gl/b6JKsE
- Tadros, Forouhar, Wucorresponding (2013) Hepatic Sarcoidosis. J Clin Transl Hepatol 1: 87–93. Link: https://goo.gl/Y6Ib5j
- Ayyala US, Padilla ML (2006) Diagnosis and treatment of hepatic sarcoidosis. Curr Treat Options Gastroenterol 9: 475-483.Link: https://goo.gl/YaQ8Ww
- Bass NM, Burroughs AK, Scheuer PJ, GERAINT DJ, SHEILA S, et al. (1982) Chronic intrahepatic cholestasis due to sarcoidosis. Gut 23: 417–421. Link: https://goo.gl/eKLXn0
- McDermott RS, Maher MM, Dunleavy K (2002) unusual presentations of lymphoma: Case 2. Non-Hodgkin’s lymphoma presenting as liver disease. J Clin Oncol 20: 1943-1946. Link: https://goo.gl/P2XZQ0
- Morla D, Alazemi S, Lichtstein D (2006) Stauffer's Syndrome Variant with Cholestatic Jaundice A Case Report. J Gen Intern Med 21: C11–C13. Link: https://goo.gl/ssKKiL
- Brincker H, Wilbek E (1974) The incidence of malignant tumours in patients with respiratory sarcoidosis. Br J Cancer 29: 247-252. Link: https://goo.gl/W7Qk2o
- Brincker H (986) The sarcoidosis-lymphoma syndrome. Br J Cancer 54: 467-473. Link: https://goo.gl/sFspB3
- Kis A, Eszes N, Tamasi T, Gyorgy L, Attila C, et al. (2013) Sarcoidosis lymphoma syndrome – the value of PET-CT in the diagnosis. World Journal of Surgical Oncology 11: 235. Link: https://goo.gl/2b6gwv
- Odemiş B, Parlak E, Başar O, Yüksel, Sahin B, et al. (2007) Biliary tract obstruction secondary to malignant lymphoma: experience at a referral center. Dig Dis Sci 52: 2323-32. Link: https://goo.gl/YhlKpV
- Tomadoni A, García C, Márquez M, Ayala JC, Prado F, et al. (2010) Stauffer's syndrome with jaundice, a paraneoplastic manifestation of renal cell carcinoma: a case report. Arch Esp Urol 63: 154-6.Link: https://goo.gl/iUXdrl
- Farouj N, Cadranel J, Mofredj A, Vincent J, Maria L, et al. (2011) Ductopenia related liver sarcoidosis. World J Hepatol 27: 170–174 . Link: https://goo.gl/yu4XVZ
- Behnava B, Alavian S (2010) A Woman with Recent Jaundice and Pruritus. Hepat Mon 10: 48–52.14.Link: https://goo.gl/ylTV6P
- Atalay A, Boyuk B, Ates M, Muhammet A, Aslan C, et al. (2015) Idiopathic Intrahepatic Cholestasis as an Unusual Presentation of Hodgkin's Disease. Case Rep Hematol 987860. Link: https://goo.gl/mzS5L9
- Papanikolaou IC, Sharma OP (2010) the relationship between sarcoidosis and lymphoma. European Respiratory Journal 36: 1207-1219. Link: https://goo.gl/HdCEME
- London J, Grados A., Fermé C, Charmillon A, Maurier F, et al. (2014) Sarcoidosis Occurring After Lymphoma: Report of 14 Patients and Review of the Literature Medicine. Medicine (Baltimore) 93: e121. Link: https://goo.gl/ZgsJ4Cn
- Baldeep-Wirk B (2010) Sarcoid Reactions after Chemotherapy for Hodgkin’s Lymphoma. Clin Med Insights Case Rep 3: 21–25.Link: https://goo.gl/AFZNII
- Sharquie KH, Al-Hayani R, Abdulwahhab W (2015) Sarcoidosis-Lymphoma Syndrome: A Spectrum of One Disease. Journal of Cosmetics, Dermatological Sciences and Applications 5: 181-188.Link: https://goo.gl/mCN3XD
- Nader K, Mok S, Kalra A, Harb A, Schwarting R, et al. (2013) Vanishing bile duct syndrome as a manifestation of Hodgkin's lymphoma: a case report and review of the literature. Tumori 99: e164-168. Link: https://goo.gl/qIFpCt
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
