Archives of Hematology Case Reports and Reviews
Recurrent primary cutaneous anaplastic large cell lymphoma in young female patient from Ethiopia: A Case Report
Temesgen Assefa Ayele*, Abel Tenaw Tessema and Fisihatsion Tadesse
Cite this as
Ayele TA, Tessema AT, Tadesse F (2022) Recurrent primary cutaneous anaplastic large cell lymphoma in young female patient from Ethiopia: A Case Report. Arch Hematol Case Rep Rev 7(1): 019-022. DOI: 10.17352/ahcrr.000040Copyright License
© 2022 Ayele TA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Primary Cutaneous Anaplastic Large Cell Lymphoma (PC-ALCL) is a CD30+ lymphoproliferative disease of the skin characterized by single or focal nodules or plaques that ulcerate over time. Diagnosis of PC-ALCL relies heavily on clinicopathological correlations because of the potential morphological, clinical, and molecular overlap with other cutaneous CD30+ LPDs. Histopathologic features include diffuse nonepidermotropic infiltrates with an adherent layer of large undifferentiated CD30+ tumor cells.
The Exact incidence of PC-ALCL is not known partially because of the difficulty differentiating from the variety of CD30+ Lymphoproliferative disorders. Only a few cases are reported even from developed countries & reports from developing countries are lacking.
We present a possible case of primary cutaneous Anaplastic Large cell Lymphoma in a 20 years old Female patient who presented with a 2 months history of lateral neck swelling.
Introduction
Skin lymphoma usually presents as either primary cutaneous lymphoma without the involvement of other organs or systemic lymphoma with metastasis to the skin. Primary cutaneous lymphoma (PCL) is a heterogeneous group of B- and T-cell non-Hodgkin lymphomas present in the skin without evidence of skin disease at the time of diagnosis [1]. PCL is the second most common group of extranodal non-Hodgkin lymphoma, with an estimated annual incidence of 1 in 100,000 in Western countries [1], although reports from developing countries are limited. A report from Isfahan Province, Iran confirmed a total of 99 PCL cases over a 10-year period [2]. Primary T-cell lymphomas are a variety of cutaneous lymphomas of T-cell and NK-cell origin that primarily involve the skin without dermal involvement at initial presentation [1]. Primary cutaneous B-cell lymphoma (PCTCL) accounts for 4% of all NHLs and 75% - 80% of total PCLs, while primary cutaneous B-cell lymphomas account for about 20% - 25% of primary cutaneous lymphomas [3,4]. PCTCL has a 2:1 male predominance, and its incidence increases with age, with the mean age at diagnosis being 50 - 60 years [4]. Among PCTCLs, mycosis fungicide and primary cutaneous CD30+ lymphoproliferative disease-account for approximately 90% of PCTCLs [4]. According to 2016 WHO revision of the classification of lymphomas, CD30+ lymphoproliferative disease is the second most common type of PCTCL. These disorders are a wide range of Tell CD30+ disorders, ranging from more benign papillomatous lymphoma to primary non-cutaneous large cell lymphoma [5]. The exact incidence of PC-ALCL is not known in part because it is difficult to distinguish it from the CD30+ variant lymphoproliferative disorder. After all, only a few cases have been reported even in developed countries and there is a lack of reporting from developing countries [6]. We present a possible case of primary cutaneous Anaplastic Large cell Lymphoma in a 20 years old Female patient who presented with a 2 months history of lateral neck swelling.
Case presentation
A 20 years old female presented with Right Neck swelling of 2 months duration, the swelling was small initially which progressively increased in size after 2 weeks, and the swelling became ulcerated & started to drain whitish discharge. Two weeks prior to her presentation to the hospital she started to have difficulty swallowing, shortness of breath & dry cough. 5 years back she had similar swelling, for which Biopsy was taken which show High-Grade non-Hodgkin’s lymphoma, but the swelling subsided without any treatment within a period of 2 months; otherwise, she has no swelling on the left side of the neck, axilla, groin or abdomen.
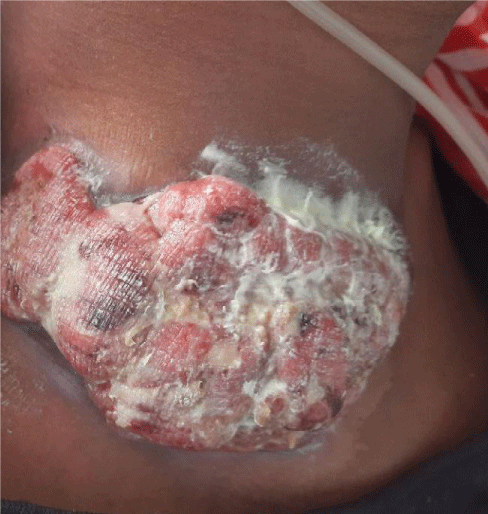
On Examination she was febrile with a Temperature record of 38.5Oc & have a 10 × 6 cm fungating mass over the right supraclavicular area with whitish discharge (Figure 1). At the presentation, an Imaging & Biopsy of the mass was done. Head & neck CT scan showed Lobulated Homogenously Enhancing Right lower cervical mass likely lymphoma.
Biopsy from the supraclavicular mass was performed & was revised by an experienced hematopathologist; it shows a hemorrhagic background with discohesive sheets of Intermediate to large cells showing atypical nuclei, some horseshoe-shaped with frequent multinucleated & abundant bluish vacuolated cytoplasm with heterogeneous lymphoid cells in the background with frequent Mitosis & the pathologic diagnosis of Anaplastic Large Cell Lymphoma was made. With the Working diagnosis of Anaplastic Large Cell Lymphoma, The patient was further worked up to exclude any systemic involvement of the Lymphoma & to differentiate whether the patient has Primary Cutaneous Anaplastic Large Cell Lymphoma or systemic Anaplastic Large Cell Lymphoma with secondary skin Involvement, for which CT scan of the Chest & Abdomen was done & it was found out to be Normal, so the Final working diagnosis of Primary Cutaneous Anaplastic Large Cell Lymphoma was made. Immunohistochemistry was planned but was not possible because the Immunohistochemistry service is not available in the country & the biopsy sample has to be transported abroad for Immunohistochemistry for which the patient has financial constraints.
Course in the hospital
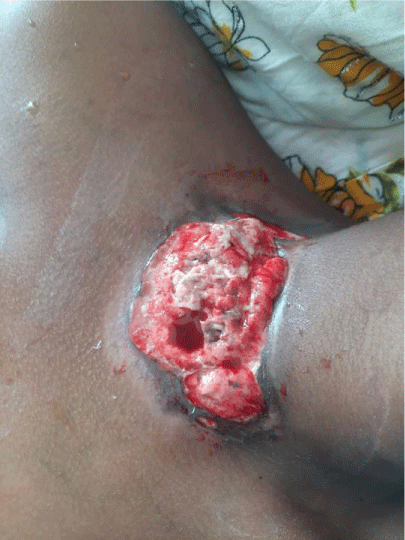
The patient was admitted with the working diagnosis of Primary Cutaneous Anaplastic Large Cell Lymphoma with super Infection; she was started on Dexamethasone 8mg IV TID to relieve the obstructive symptoms & was put on Ceftriaxone, & Metronidazole to treat the super Infection. After seven days of steroid & Antibiotics treatment, the patient was fever-free, whitish discharges cleared, the size of the mass significantly reduced (Figure 2 ) & the obstructive symptoms disappeared. After treatment of the bacterial superinfection, it was planned to treat her with Radiotherapy but was not possible because of technical difficulties then the patient was started on weekly Methotrexate 7.5 mg PO Bid with Folic acid 5 mg daily, and the patient was appointed for further follow-up.
Discussion
PC- ALCL is a rare type of indolent cutaneous lymphoma characterized by CD30+ atypical lymphocytes in the skin [7]. Its prevalence is unknown but it accounts for approximately 9% of cutaneous lymphomas. The male/female ratio is 3:2 [7]. PCALCL generally occurs in adults with a median age at diagnosis of 61 and occurs rarely in children and adolescents [8].
In either a localized or multifocal distribution, PC-ALCL typically manifests as large, solitary, or multiple slow-growing erythematous skin plaques, nodules, or tumors. In 10% of cases, it extends beyond the skin to the lymph nodes and presents as a painless swelling, particularly in the neck, armpit, or groin. These lesions may become ulcerated and/or itchy. It may also encompass extranodal locations, though unusual. Loss of appetite, weight loss, and night sweats are common general symptoms that are typically present in instances with extracutaneous involvement [9,10].
Histologically dense dermal infiltrate that typically does not involve the epidermis can be seen. The infiltrate is made up of continuous sheets of large CD30+ tumor cells that share similarities with systemic ALCL in terms of their morphology with the typical finding of big cells with abundant, pale, eosinophilic cytoplasm and round or pleomorphic horseshoe-shaped nuclei with prominent nucleoli.
In the periphery of the tumor cells, reactive lymphocytes, histiocytes, eosinophils, and neutrophils are frequently found, and in ulcerating lesions, epidermal hyperplasia may be noticeable [11]. Immunohistochemistry is required for a conclusive diagnosis, and at least 75% of tumor cells express CD30 in addition to the majority of cases expressing CD4 and varying loss of CD2, CD3 and CD5. Cutaneous Lymphocyte Antigen (CLA) is present in the majority of instances, although, unlike systemic ALCL, they do not express Epithelial Membrane Antigen (EMA) and Anaplastic Lymphoma Kinase (ALK) [12].
Lymphomatoid papulosis (LyP), systemic ALCL, altered mycosis fungoides, and reactive lymphoid hyperplasias are among the differential diagnoses [1]. PCALCL and LyP appear to be related morphologically and immunohistochemically. Consequently, it is crucial to correlate pathology findings to clinical history [12].
As opposed to PCALC, LyP is a recurrent, self-healing disorder marked by self-limiting papulonodular skin eruptions [13].
Depending on the size of the lesion, several treatments are used for PC-ALCL. If the lesion is isolated or restricted to a single location, excision and/or radiation therapy are used. Chemotherapy with methotrexate, systemic retinoid, and anti-CD30 monoclonal antibody brenituximab vedotin can be utilized if lesions are spread in numerous areas of the body [14].
With a 90% five-year survival rate, the prognosis is generally favorable. Spontaneous regression is seen in 25% of instances. In 30% of instances, relapses develop in the absence of extracutaneous spread [7].
Although confirmatory immunohistochemistry was not performed to definitively confirm the diagnosis, our case is a potential instance of recurrent anaplastic large cell lymphoma in a young female patient with a typical histopathological description of cutaneous anaplastic large cell lymphoma. Since she has a similar clinical presentation which subsided by itself & with biopsy description of high-grade lymphoma, it is evidence of recurrent disease.
In conclusion, a diagnosis of Primary Cutaneous Anaplastic Large Cell Lymphoma needs to be considered, regardless of the age in patients who presented with recurrent soft tissue mass with typical histopathologic findings of cutaneous Anaplastic Large cell Lymphoma & if possible the biopsy tissue should be subjected to histopathologic evaluation and immunohistochemistry for definitive diagnosis.
Disclosure
- Verbal Informed consent was obtained from the patient.
- The patient is fully volunteered for the reporting of the case and to continue the care.
Author information
Dr. Temesgen Assefa Ayele, Internist, Assistant Professor of Internal Medicine, Hematology Fellow, Hematology Unit, Department of Internal Medicine, College of Medicine & Health Sciences, Adissababa University.
Dr.Abel Tenaw Tessema, Internal Medicine Resident, Department of Internal Medicine, College of Medicine & Health Sciences, Adissababa University.
Dr. Fisihatsion Tadesse, Internist, Assistant Professor of Internal Medicine, Consultant Hematologist, Hematology Unit, Department of Internal Medicine, College of Medicine & Health Sciences, Adissababa University.
- Bolognia JL, Schaffer JV, Cerroni L. Editors. Dermatology. 4th ed revised. New York: Elsevier. 2018; 2:2127-2147.
- Naeini FF, Abtahi-Naeini B, Pourazizi M, Sadeghiyan H, Najafian J. Primary cutaneous lymphomas: A clinical and histological study of 99 cases in Isfahan, Iran. J Res Med Sci. 2015 Sep;20(9):827-31. doi: 10.4103/1735-1995.170595. PMID: 26759567; PMCID: PMC4696365.
- Willemze R, Jaffe ES, Burg G, Cerroni L, Berti E, Swerdlow SH, Ralfkiaer E, Chimenti S, Diaz-Perez JL, Duncan LM, Grange F, Harris NL, Kempf W, Kerl H, Kurrer M, Knobler R, Pimpinelli N, Sander C, Santucci M, Sterry W, Vermeer MH, Wechsler J, Whittaker S, Meijer CJ. WHO-EORTC classification for cutaneous lymphomas. Blood. 2005 May 15;105(10):3768-85. doi: 10.1182/blood-2004-09-3502. Epub 2005 Feb 3. PMID: 15692063.
- Sidiropoulos KG, Martinez-Escala ME, Yelamos O, Guitart J, Sidiropoulos M. Primary cutaneous T-cell lymphomas: a review. J Clin Pathol. 2015 Dec;68(12):1003-10. doi: 10.1136/jclinpath-2015-203133. PMID: 26602417.
- Swerdlow SH, Campo E, Pileri SA, Harris NL, Stein H, Siebert R, Advani R, Ghielmini M, Salles GA, Zelenetz AD, Jaffe ES. The 2016 revision of the World Health Organization classification of lymphoid neoplasms. Blood. 2016 May 19;127(20):2375-90. doi: 10.1182/blood-2016-01-643569. Epub 2016 Mar 15. PMID: 26980727; PMCID: PMC4874220.
- Moodley N, Nombona P, Mosam A. Primary Cutaneous Anaplastic Large-Cell Lymphoma. Dermatopathology (Basel). 2019 Jun 26;6(2):163-169. doi: 10.1159/000500259. PMID: 31700858; PMCID: PMC6827451.
- Booken N, Goerdt S, Klemke CD. Clinical spectrum of primary cutaneous CD30-positive anaplastic large cell lymphoma: an analysis of the Mannheim Cutaneous Lymphoma Registry. J Dtsch Dermatol Ges. 2012 May;10(5):331-9. doi: 10.1111/j.1610-0387.2011.07794.x. PMID: 22525148.
- Bekkenk MW, Geelen FA, van Voorst Vader PC, Heule F, Geerts ML, van Vloten WA, Meijer CJ, Willemze R. Primary and secondary cutaneous CD30(+) lymphoproliferative disorders: a report from the Dutch Cutaneous Lymphoma Group on the long-term follow-up data of 219 patients and guidelines for diagnosis and treatment. Blood. 2000 Jun 15;95(12):3653-61. PMID: 10845893.
- Bolognia JL, Schaffer JV, Cerroni L, editors. Dermatology. 4th ed, revised. New York: Elsevier. 2018; 2: 2127-2147
- Oliveira LS, Nobrega MP, Monteiro MG, Almeida WL. Primary cutaneous anaplastic large-cell lymphoma--case report. An Bras Dermatol. 2013 Nov-Dec;88(6 Suppl 1):132-5. doi: 10.1590/abd1806-4841.20131731. PMID: 24346900; PMCID: PMC3875977.
- Brown RA, Fernandez-Pol S, Kim J. Primary cutaneous anaplastic large cell lymphoma. J Cutan Pathol. 2017 Jun;44(6):570-577. doi: 10.1111/cup.12937. Epub 2017 Apr 25. PMID: 28342276.
- Swerdlow SH, Campo E, Harris NL. World Health Organization Classification of Tumours of Haematopoietic and Lymphoid Tissues, IARC Press, Lyon. 2008.
- Dawn G, Morrison A, Morton R, Bilsland D, Jackson R. Co-existent primary cutaneous anaplastic large cell lymphoma and lymphomatoid papulosis. Clin Exp Dermatol. 2003 Nov;28(6):620-4. doi: 10.1046/j.1365-2230.2003.01406.x. PMID: 14616830.
- Booken N, Goerdt S, Klemke CD. Clinical spectrum of primary cutaneous CD30-positive anaplastic large cell lymphoma: an analysis of the Mannheim Cutaneous Lymphoma Registry. J Dtsch Dermatol Ges. 2012 May;10(5):331-9. doi: 10.1111/j.1610-0387.2011.07794.x. PMID: 22525148.

Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
