Archives of Hematology Case Reports and Reviews
Recurrent thrombosis in a multiple myeloma patient with low risk for thrombosis despite being on thromboprophylaxis
Chow Siew Kian* and Fu Mei Sian
Cite this as
Kian CS, Sian FM (2019) Recurrent thrombosis in a multiple myeloma patient with low risk for thrombosis despite being on thromboprophylaxis. Arch Hematol Case Rep Rev 4(1): 003-005. DOI: 10.17352/ahcrr.000015It is a well-known fact that multiple myeloma (MM) patients have an increased risk for thromboembolic events involving both the venous and arterial territories. The etiologies can be multifactorial, for example, activation of procoagulant factors, acquired protein C resistance, MM-specified and treatment-related factors. The risk of venous thrombosis is high when patients receive treatment with thalidomide or lenalidomide in combination with dexamethasone or multi-agent chemotherapy. Arterial thromboses occur less compared to venous thrombotic events. Nonetheless, thromboprophylaxis is important in preventing both types of thromboses. In this case study, we reveal a patient whom thrombosis occurred concurrently in both arterial and venous despite being on aspirin prophylaxis.
Introduction
Multiple myeloma is a neoplastic proliferation of plasma cells producing monoclonal immunoglobulin lineages. These clonal plasma cells proliferate in the bone marrow and result in extensive skeletal destruction which leads to pathological fracture, renal failure, hypercalcemia, and anemia [1]. Treatment with immunomodulatory drugs (IMiDs) such as thalidomide and lenalidomide, bortezomib, as well as high-dose melphalan with stem cell transplantation improve patient overall survival. However, thrombotic events also increase with the introduction of IMiDs [2]. Thus, thrombosis prevention is crucial in high risk patients.
Case Report
Here we report a 52 year-oldgentleman with newly diagnosed kappa light chain restriction multiple myeloma in November 2017. He had completed 6 cycles of CTD regime (cyclophosphamide 400mg weekly for three weeks + dexamethasone 40mg weekly for 4 weeks and thalidomide 100mg ON). Bortezomib was not started as patient was unable to come to the hospital to receive weekly injections. At the same time, he was prepared for autologous haematopoietic cell transplantation. He responded well with the chemotherapy and was subsequently put on thalidomide-dexamethasone (TD) maintenance.
After being stable for 6 months, the patient presented to us with an acute abdomen. Serial investigations and CECT abdomen showed an ischemic ileum, and an ileal resection was carried out by the surgical team. He was then started on an antiplatelet, cardiprin 100mg daily, for thromboprophylaxis on top of a maintenance regime of thalidomide 100mg daily and dexamethasone 8mg per week. In the subsequent follow up, his full blood count revealed anaemia, leucopenia, a reverse globulin: albumin ratio and hypercalcemia. These results prompted us to proceed with a bone marrow aspiration and trephine biopsy. We then started him on VCD regime (subcutaneous velcade 2.4g weekly, cyclophosphamide 500mg weekly and dexamethasone40mg weekly).
Unfortunately, three weeks later, the patient’s results showed a relapse of his MM as evidenced by the presence of 47% abnormal plasma cell in his bone marrow and 21% plasma cell on immunophenotyping showing the phenotypes FSC mod-hi, SCC int, CD45 INT, CD 138+, CD38+ and CD19with kappa light-chain restriction. We decided to switch his regime to subcutaneous velcade 2.4g weekly, thalidomide 100mg ON and dexamethasone 40mg weekly (VTD regime).
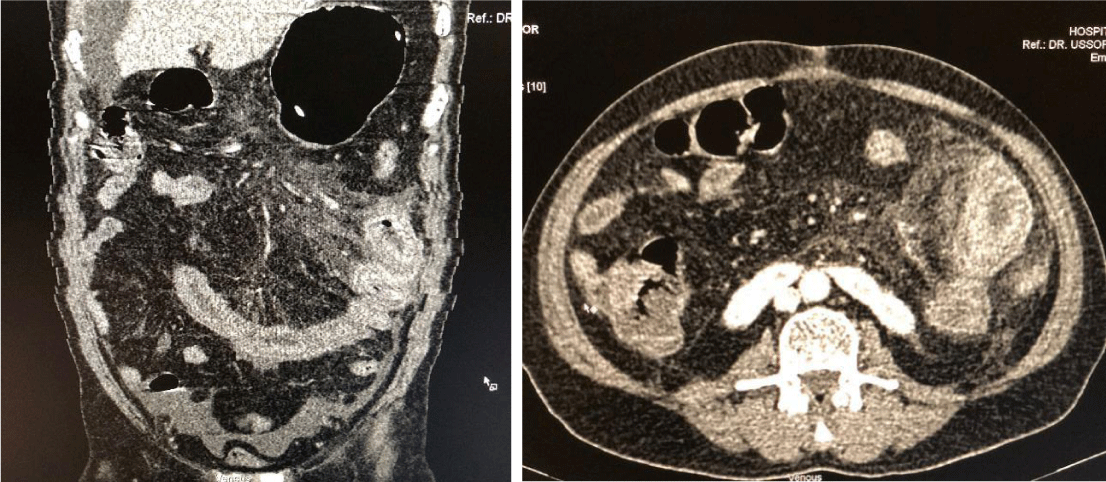
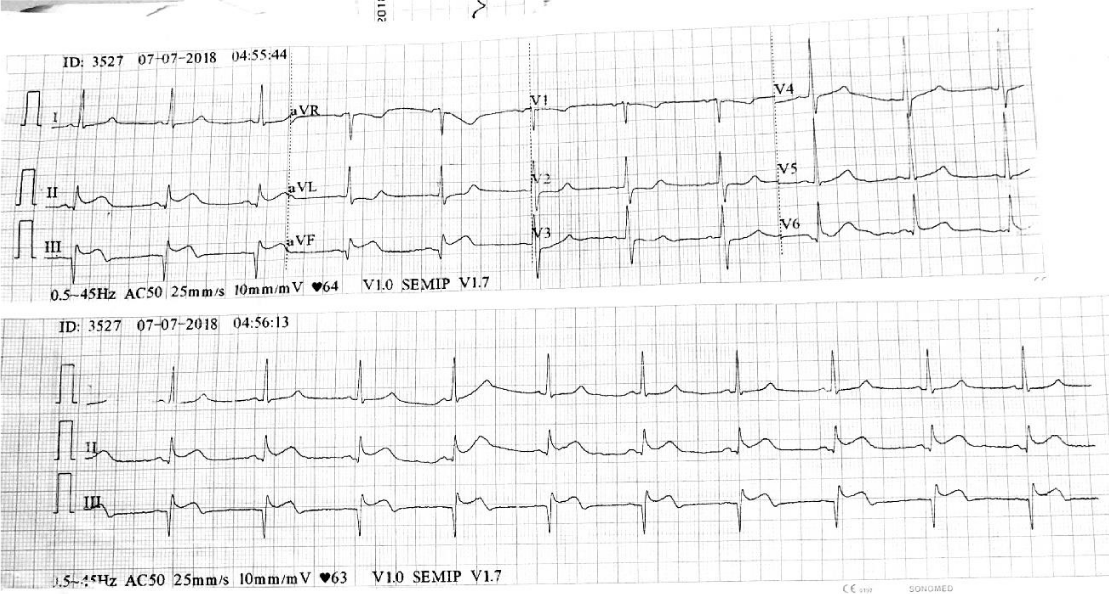
After 3 days of chemotherapy, the patient suddenly experienced abdominal pain and was admitted to a district hospital. CTA abdomen showed only circumferential long segment wall thickening of proximal small bowel and an engorged vasa recta, but no major vessels thrombosis. A diagnosis of acute ischemia bowel was made, and he was referred to the surgical team who commenced heparin infusion. Despite the heparin infusion, the patient started to complain of chest pain the next day, and ECG showed an infero-posterior STEMI. Due to the lack of percutaneous coronary intervention (PCI) facilities in district hospital, the patient was continued on the infusion heparin and started on dual antiplatelet. Traditional thrombolysis therapy was not commence due to recent surgery (ileal resection) done in past one month. He was discharged well and given an appointment with the cardiology department. We also referred him to a hematologist who rechallenged the patient with the CTD regime, and a thallium scan was arranged (Figures 1-3).
Discussion
Multiple myeloma patients have a higher risk of developing thrombotic events compared to the general population, especially after the introduction of immunomodulatory drugs (IMiDs) such as thalidomide. According to a Swedish study, the risk for VTE was found to be higher by 7.5-fold at 1 year of follow-up and 4.1-fold at 10 years follow up [2]. On top of that, the risk for arterial thromboses (myocardial infarction, transient ischemic attack, and symptomatic peripheral artery disease) were also significantly increased compared with the control group [3]. Interestingly, arterial thromboses mostly occurred in patients with MM during and after the induction chemotherapy [4]. In a meta-analysis review by Li et al reported that there is increasing of cardiovascular events with the multiple myeloma [5].
Causes of venous thromboembolism (VTE) in MM patients are multifactorial. Besides the traditional risk factors such as immobilization due to bone pain or pathological fracture, obesity, surgery and central venous catheter (CVCs) insertion, patient-related risk factors include previous VTE and hematological disorders (such as factor V leiden, prothrombin G20210A mutation, protein C and S deficiency and antithrombin deficiency) also contribute to the risk of thrombosis. In addition, the combination of thalidomide with dexamethasone (12-26%)/anthracycline/melphalan and prednisolone (MPT)/ erythropoietin demonstrate substantial increases in the risk of thrombosis [6-9].
VTE can lead to catastrophic events such as pulmonary embolism whereas arterial thrombosis can lead to fatal myocardial infarctions and stroke. Kristinsson et al reported MM patients having a higher rate of any thrombosis compared to controlled group during a 10 years follow up study; the incidence of venous and arterial thromboses and the risk of death were at their highest during the first year after diagnosis and continued to be elevated at 5 and 10 years of follow up [3,10].
Hence it is crucial to start thrombotic prophylaxis to minimize mortality and morbidity rates. There are a few measures to reduce the risk of thrombosis. First, the use of bortezomib (velcade) in conjunction with thalidomide- and lenalidomide-containing regimens show promising reductions in thrombotic events through mechanisms that are still not fully understood [11]. Second, thromboprophylaxis started at the time of diagnosis and continued until thrombosis risk factors resolve, on the condition of absence of contraindications in selected patient (standard risk and high risk patients), help to reduce VTEs. MELLISE study showed no statistically difference of VTE between low, intermediate and high risk groups [12]. Choice of agents include aspirin, low molecular weight heparin (LMWH) and vitamin K antagonists (warfarin). The GIMEMA study aimed to evaluate the best choice of thromboprophylaxis in MM patients and results showed that there were no significant difference in the incidence of VTE between the three groups comprising of low-molecular weight heparin (LMWH), aspirin and warfarin, with a thrombotic incidence of 5%, 6% and 8%respectively [13]. However Larocca et al reported that the incidence of VTE in aspirin group was relatively higher compared to the LMWH group (2.27% VS 1.20%) as thromboprophylaxis in MM who received Lenalidomide plus dexamethasone [14].
However, we should remember that these steps do not completely eliminate the risk of thrombosis. Approximately 5–8% of MM patients still develop thrombosis despite being on prophylaxis [15]. This was evident in our patient who suffered from both an ischemic bowel and a myocardial infarction despite being initiated on aspirin after the first event of bowel ischemia. His first thrombotic encounter of ischemic bowel had put him into the standard risk of thrombosis, thus our patient was given aspirin 100mg and changed to bortezomib-combination chemotherapy. Nonetheless, a subsequent thrombosis still occurred.
When thrombotic events arise in MM patients, a proper clinical evaluation is important. It may actually signify a relapse of the primary disease, thus a detailed work up needs to be done. In this case, the patient was stable after a few cycles of chemotherapy. The sudden abdominal pain brought him to the hospital, revealing a bowel ischemia secondary to thrombosis. However, subsequent blood investigations, urine paraprotein and bone marrow aspiration proved the relapse of his MM. We have to be vigilant with MM patients who complain of abdominal pain, angina or hemiparesis since they have an inherent high risk to develop thromboses, necessitating a lower threshold for requesting urgent imaging such as CTA abdomen, CT brain and computed tomography of pulmonary artery (CTPA).Early detection of thrombosis can reduce morbidity and mortality rates.
Conclusion
Individuals with multiple myeloma have a higher risk of thrombosis especially when treated with IMiDs combination therapy. Thrombotic prophylaxis should be tailored to each individual, and constant vigilance is necessary to detect early evidence of relapsed MM so that suitable treatment modalities can be started.
-
1. Hallek M, Bergsagel PL, Anderson KC (1998) Multiple myeloma: increasing evidence for a multistep transformation process. Blood 91: 3-21. Link: https://tinyurl.com/y45nr59o
2. Kristinsson SY, Fears TR, Gridley G, Turesson I, Mellqvist UH, et al. (2008) Deep vein thrombosis after monoclonal gammopathy of undetermined significance and multiple myeloma. Blood 112: 3582-3586. Link: https://tinyurl.com/yxh6ooce
3. Kristinsson SY, Pfeiffer RM, Björkholm M, Goldin LR, Schulman S, et al. (2010) Arterial and venous thrombosis in monoclonal gammopathy of undetermined significance and multiple myeloma: a population-based study. Blood 115: 4991-4998. Link: https://tinyurl.com/y63dhmbp
4. Libourel EJ, Sonneveld P, van der Holt B, de Maat MP, Leebeek FW (2010) High incidence of arterial thrombosis in young patients treated for multiple myeloma: results of a prospective cohort study. Blood 116: 22-26. Link: https://tinyurl.com/y4k75z74
5. Li W, Garcia D, Cornell RF, Gailani D, Laubach J, et al. (2017) Cardiovascular and Thrombotic Complications of Novel Multiple Myeloma Therapies. JAMA Oncol 3: 980-988. Link: https://tinyurl.com/y6k2gghk
6. Rajkumar SV, Jacobus S, Callander N, Fonseca R, Vesole D, et al. (2007) Phase III trial of lenalidomide plus high-dose dexamethasone versus lenalidomide plus low-dose dexamethasone in newly diagnosed multiple myeloma (E4A03): A trial coordinated by the Eastern Cooperative Oncology Group. Clin Oncol 25. Link: https://tinyurl.com/y225yy4z
7. Carrier M, Le Gal G, Tay J, Wu C, Lee Ay (2011) Rates of venous thromboembolism in multiple myeloma patients undergoing immunomodulatory therapy with thalidomide or lenalidomide: a systematic review and meta-analysis. Journal of Thrombosis and Haemostasis 9: 653-663. Link: https://tinyurl.com/y69qdm5g
8. Robert knight RJD, Jerome B (2006) Lenalidomide and Venous Thrombosis in Multiple Myeloma. New England Journal of Medicine 354: 2079-2080. Link: https://tinyurl.com/y43yklyf
9. Chalayer E, Chapelle C, Leleu X, Elalamy I, Laporte S, et al. (2016) Does the choice of thrombotic prophylactic drug depend on the known risk factors of patients with multiple myeloma in clinical practice? Thromb Res; 143: 101-102. Link: https://tinyurl.com/y4n3t2v5
10. Kristinsson SY, Pfeiffer RM, Björkholm M, Schulman S, Landgren O (2012) Thrombosis is associated with inferior survival in multiple myeloma. Haematologica 97: 1603-1607. Link: https://tinyurl.com/yxutq2km
11. Zangari M, Fink L, Zhan F, Tricot G (2011) Low venous thromboembolic risk with bortezomib in multiple myeloma and potential protective effect with thalidomide/lenalidomide-based therapy: review of data from phase 3 trials and studies of novel combination regimens. Clinical lymphoma, myeloma & leukemia 11: 228-236. Link: https://tinyurl.com/y2s2n6w4
12. Leebeek FWG (2016) Update of thrombosis in multiple myeloma. Thromb Res 140 Suppl 1: S76-S80. Link: https://tinyurl.com/y6o6el9h
13. Palumbo A, Cavo M, Bringhen S, Cavalli M, Patriarca F, et al. (2009) A Phase III Study of Enoxaparin vs Aspirin vs Low-Dose Warfarin as Thromboprophylaxis for Newly Diagnosed Myeloma Patients Treated with Thalidomide Based-Regimens. Blood 114: 492. Link: https://tinyurl.com/y2fohlsm
14. Larocca A, Cavallo F, Bringhen S, Di Raimondo F, Falanga A, et al. (2012) Aspirin or enoxaparin thromboprophylaxis for patients with newly diagnosed multiple myeloma treated with lenalidomide. Blood 119: 933-999. Link: https://tinyurl.com/yxbdhvl4
15. Cesarman-Maus G, Braggio E, Fonseca R (2012) Thrombosis in multiple myeloma (MM). Hematology (Amsterdam, Netherlands) 17: S177-S180. Link: https://tinyurl.com/y6ednk6f
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
