Archive of Gerontology and Geriatrics Research
Impact of a COVID-19 outbreak in a long-term care facility in Barcelona, Spain: The role of a COVID-19 prevention and control program
Gabriel Vallecillo1-3*, Marta Anguera1, Noemi Martin1,3, Cristina González3, Consol Serra5, Juan Pablo Horcajada2,3 and Víctor Pérez1,2
2Hospital del Mar Medical Research Institute (IMIM), Barcelona, Spain
3Infection Control Program, Hospital del Mar, Parc de Salut Mar Consortium, Barcelona, Spain
4Occupational Health Department, Hospital del Mar, Parc de Salut Mar Consortium, Barcelona, Spain
Cite this as
Vallecillo G, Anguera M, Martin N, González C, Serra C, et al. (2020) Impact of a COVID-19 outbreak in a long-term care facility in Barcelona, Spain: The role of a COVID-19 prevention and control program. Arch Gerontol Geriatr Res 5(1): 043-047. DOI: 10.17352/aggr.000026Background: COVID-19 outbreaks in long-term care facilities are a significant impact on infection rates and mortality rates of the residents. The study aimed to describe the effectiveness of a COVID-19 prevention and control (CPC) program in a long-term care facility.
Methods: A CPC program, including social isolation, active symptoms screening for all residents and staff, SARS-CoV-2 testing for symptomatic individuals, droplet and contact isolation measures for asymptomatic residents, confinement of the unit and clinical care in a separate unit for patients, was implemented in a long-term care facility with two geriatrics and two psychiatric units, with aa total of 300 beds. The attack rate was calculated as the number of COVID-19 confirmed cases divided by the total number of exposed individuals and case fatality rate as the deceased COVID-19 cases divided by the total number of COVID-19 cases.
Results: Two geriatric (unit-1 and 2) and one psychiatric (unit-4) units were affected by the outbreak. Attack rates were 26/47(55.3%) for unit-1, 15/29(51.7%) for unit-1and 11/46(23.9%) for unit-4. Case fatality rates were 3/25(12.0%) for unit-1 and 2/16 (12.5%) for unit-2 and no patient from the unit-4 died. Among healthcare professionals, total attack rate was 30/124(24.2%) with no differences between units. Viral pneumonia was present in 13(25%) residents and all healthcare professionals had mild COVID-19.
Conclusions: Timely institution of a CPC program with close monitoring of all exposed individuals are essential to decrease the negative outcomes of COVID-19 outbreaks in long-term care facilities. Droplet and contact isolation for all residents is a useful alternative to wide-facility SARS-CoV-2 testing.
Introduction
The COVID-19 pandemic (coronavirus disease 2019) is a devastating disease that has affected more than a hundred countries causing a serious impact on the health, economy and society [1]. COVID-19 mortality is higher in people aged 60 years or over and with underlying medical conditions, such as cardiovascular disease, chronic respiratory disease, diabetes and cancer [2-5]. During the ongoing COVID-19 pandemic, long-term care facilities and other congregate living settings have been identified as high-risk settings for severe outbreaks and poor outcomes [6-11]. These facilities are particularly susceptible as many of their residents are older, frail, with disabilities and multiple and severe chronic comorbidities or immunocompromised status [12]. Moreover, clinical and social characteristics of long-term care facilities provide an ideal environment for acquisition and spread of COVID-19, resulting in large outbreaks [6-11]. Gathering of a large number of residents who share multiple resident rooms, group activities and clinical care, together with a high number of health care professionals and visitors, are factors that promote the coronavirus spreading in the facility [13,14]. Moreover, control measures are difficult to enforce for residents with dementia and behavior disturbances [13,14]. In addition, most facilities are poorly prepared to implement infection control policies owing to shortage of protective equipment and relatively low level of staff training [13-15].
Anyway, the rapid evolution and mortality of COVID-19 outbreaks in long-term care facilities highlight the critical need of implementing a strong COVID-19 prevention and control (CPC) program to protect both residents and Healthcare Professionals (HCP) [16-18]. However, characteristics and functioning of CPC programs vary depending on the resources of each facility [6-11], so studies are necessaries to evaluate the effectiveness of CPC programs to reduce the morbidity and mortality of outbreaks in long-term care facilities.
Therefore, the objective of this study was to describe the effectiveness of a COVID-19 prevention and control action program, including social isolation, active symptoms screening for all residents and staff, SARS-CoV-2 testing for symptomatic individuals, droplet and contact isolation measures for asymptomatic residents, confinement of the unit and clinical care in a separate unit for patients in a long-term care facility during the first wave of COVID-19 epidemic in Spain [19].
Material and methods
Setting
The study was conducted at the Emili Mira Healthcare Center, a public acute and long-term care center for medical and psychosocial rehabilitation in Barcelona, (Spain) dependent on a large tertiary teaching hospital. The center had 2 main buildings for clinical care: The Central Building and the Levante Building. The Central Building offered acute psychiatric care in 4 units with a total of 100 beds. The Levante Building was the long-term care facility and had 4 units with 50 bed each one. Units 3 and 4 were for psychiatric care, and units 1 and 2 for geriatric care. The psychiatric units offered long-term mental health care for people with severe mental disorders and geriatric units offered care for patients >65 years who were recovering from an illness or surgery and needed the assistance of a caregiver for activities of daily living, such as eating, bathing, and taking oral medications at the correct time, in addition to ongoing medical care.
Nurses, physicians, physiotherapist and social workers were the HCP involved in the clinical care of patients. Each unit had its own medical staff but some nurses and physicians were shared between units and buildings depending on clinical programs. There were resting areas for each specific unit and a shared locker room located in the Central Building for all HCP.
Interventions
From the beginning of the national state of alarm (declared on the 14th March, 2020), a structured CPC program was implemented in the facility to prevent and control COVID-19 among residents. The CPC program was designed by the clinical staff and was approved by the medical direction of the facility. The CPC program was coordinated by a physician specialized in infectious diseases and included preventive measures for residents, HCP and facility according to the international guidelines [16-18].
Residents
All residents were screened for symptoms every day and axillary temperature every 8 hours. A determination of coronavirus SARS-Cov-2 real time reverse-transcription-polymerase chain reaction (cobas® SARS-CoV-2 Test Roche laboratories) in nasopharyngeal samples was done for any suspected case of COVID-19. Residents who tested positive for SARS-CoV-2 were transferred to a specific acute care unit inside the facility. Before the outbreak New resident admissions were admitted and were placed in quarantine during the first 14 days. New resident’s admissions were cancelled during the outbreak.
HCP
HCP were checked themselves for fever and symptoms of COVID-19 at the beginning and during the work shift. Symptomatic HCP were tested for coronavirus SARS-CoV-2 and positive cases were isolated at home until recovering and having a negative test, HCP were educated on correctly performing hand hygiene and the use of personal protective equipment according to local guidelines.
Facility
All groups’ activities, including communal dining were cancelled and older people were locked in their room with droplet and contact isolation measures. Family and caregiver visits were restricted but residents could establish video call once a day through an electronic device supervised by assistant nurses. Resident clothes and linens were changed every day for all residents, as well as medical clothes for HCP. The number of cleaning times of the rooms and staff office was doubled and droplet and contact isolation measures were established for all individuals. A specific acute care unit for residents with confirmed COVID-19 was created in the facility, which was placed on a different floor and worked with own medical staff. All measures were finished in each unit 14 days after the last COVID-19 diagnoses in residents or HCP.
Definitions
The COVID-19 primary case was defined as the first case diagnosed among residents or HCP. COVID-19 confirmed cases were defined as symptomatic resident or HCP who had tested positive in the SARS-CoV-2 RT-PCR. Total number of residents exposed included all the patients who were residing in each unit at the time of the primary case diagnosed and those who were discharged in the previous two days to the primary case diagnosed. Total number of staff exposed included all HCP who were working in each unit at the at the time of the primary case diagnosed and those who were working in the previous two days to the primary case diagnosed. The duration f the outbreak included the period between the diagnosis of the primary case and the last case diagnosed.
The main variables of the study were the attack and case fatality rates of the residents and the HCP. The secondary variables of the study were the description of the clinical characteristics of patients and HCP with COVID-19.
The attack rate was calculated as the number of confirmed cases divided by the total number of exposed individuals, and case fatality rate as the deceased confirmed cases divided by the total number of confirmed.
Statistics
Descriptive statistics was expressed as mean and standard deviation, whereas quantitative variables with nonparametric distribution were expressed as median and interquartile range. Absolute frequencies and percentages were expressed for the qualitative variables. One-way ANOVA and Kruskal-Wallis test were used to compare quantitative variables. Analyses were made using SPSS software, version 17.0.0 (Chicago, Illinois).
Ethics
The study followed the ORION statement guidelines for transparent reporting of outbreak reports and intervention studies of nosocomial infection [20] and complied with the ethical statements in the Declaration of Helsinky (64th General Assembly, Fortaleza, Brazil, October 2013).
Results
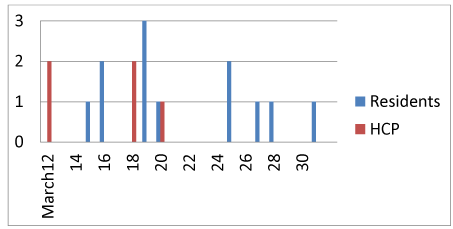
The outbreak affected the two geriatric (unit-1 and 2) and one the psychiatric(unit-4) units of the long-term care facility (Levante Building). There were 122 residents (47 unit-1, 29 unit-2, 46 unit-3), and 124 HCP (61 unit-1, 23 unit-2, 14 shared between unit-1 and unit-2 and 26 in unit-4) exposed during the outbreak. The primary case was diagnosed on March 12 in a regular HCP of the unit-4 and the last confirmed case on April 24 in a resident of the unit-1. In total there were 82 confirmed COVID-19 cases: 52 in residents and 30 in HCP. Duration of the outbreak was 20 days for the unit-4 (March 12 to March 31), 23 for the unit-2 (March 17 to April 7) and 30 for the unit-1(March 23 to April 22). The epidemiological curve for each unit is shown in the Figure 1.
Clinical characteristics and attack and case fatality rates of residents with COVID-19 are showed in Table 1. Residents from the geriatric units were older, had lower functional index and higher comorbidity, COVID-19 pneumonia, attack and case fatality rates compared to the residents from the psychiatric unit.
Among HCP, the median age was 38 (IQR: 26-51) years and 24/30 (77.4%) were women. All cases were mild COVID-19 and none HCP died. The total attack rate was 30/124(24.2%) with no differences between units: 14/75 (18.6%) for unit-1, 12/37 (32.4%) for unit-2 and 5/26(19.2%) for unit-4 (p 0.23).
Discussion
The results of this study describing the effectiveness of a CPC program focused on symptom-based screening, showed similar results than programs based on facility-wide SARS-CoV-2 testing in terms of incidence [10]. Facility-wide testing is essential to detect asymptomatic patients who can keep active the outbreak in the facility [21,22]. However, the virus spread has already occurred at the time the first case is identified in the facilities and some patients can test negative because the disease is under the incubation period [9] and thus, implementing isolation measures by contact and drops for all residents at this time is a suitable preventive measure to control the outbreak. The results of this study supports this option for CPC programs of facilities which have limited access to laboratory for asymptomatic patients.
Moreover, this study showed nearly twice of infections among residents of geriatric units compared to the psychiatric unit. This fact is important, as residents from the geriatric units had high needs of nursing care secondary to their functional disability, according to the Barthel index, that predisposed them to an intense contact with HCP during the daily routine care [23], which is a risk factor for infection [24,25]. Thus, HCP should be aware of the risk of nursing care and adhere strictly to CPC practices to prevent the spread of infection.
Another point of interest of this study was that the primary case of each unit was diagnosed in one HCP, and later in residents and others HCP, as it was seen in the epidemic curve. This fact highlights the importance of checking symptoms of HCP and policies to avoid that symptomatic HCP continued working in the facility [26-28]. By contrast, staff rotation between care units could not be avoided in this study, which could spread COVID-19 to others units, particularly if they were asymptomatic [29-30]. Otherwise, the high attack rate among HCP observed in this study, in spite of availability of the personal protective equipment, suggests some deficiencies in the compliance and adherence to preventive measures. During outbreaks, there are considerable disruptions in the clinical care routine, such as leave staff absenteeism, fear to the infection, low experience using personal protective equipment, increased workload and relaxing preventive measures over time and at work breaks, which can affect the compliance and adherence to preventive measures [31,32]. Anyway, regular auditing and feedback from observation of staff workflow could be a useful option to maintain optimal HCP adherence to preventive measures during outbreaks [33].
It is also necessary to note the low mortality among patients with COVID-19 in this study, who had several factors for high risk mortality [2-4] as older age, comorbidities and functional dependency. Probably early diagnosis and treatment in a specific unit with a comprehensive clinical care [34], could contribute to this result.
This study has some limitations and advantages. Lack of a facility-wide SARS-CoV-2 testing initiated before identification of a COVID-19 case is essential to prevent outbreaks and to detect asymptomatic patients who can spread the virus during outbreak [10]. However, the CPC program, including droplet and contact isolation to prevent that hypothetical asymptomatic patients spread the virus, proved to be effectiveness for controlling the outbreak in a more difficult and complex center, with two facilities, high number of residents and HCP and common spaces for HCP [11].
Given that antiviral drugs have failed to prevent COVID-19 after exposure, specially hydroycloroquine [35,36], future line of research should be focused on health policies that generalize the incorporation of CPC programs, including facility-wide SARS-CoV-2 testing. Additionally, incorporation of SARS-CoV-2 antigen tests for the screening of asymptomatic residents and HCP should be evaluated [37].
Conclusions
In conclusion, COVID-19 outbreaks in long-term care facilities cause serious adverse outcomes among residents and affect a high number of HCP. The extent to which COVID-19 outbreaks in these facilities can be prevented and reduced their clinical impact depend on the application of
Community-facility contact restrictions, increased testing of residents and staff, and heightened infection control including more access to personal protective equipment for staff. In facilities where wide testing SARS-CoV-2 is restricted for asymptomatic residents, droplet and contact isolation measures for all residents is a useful alternative.
As the COVID-19 crisis continues, long-term care facilities are in critical need of these resources to protect their vulnerable populations.
1. HighlightsA COVID-19 prevention and control program is necessary to reduce the negative clinical impact of COVID-19 outbreak, especially in older adults with comorbidities and disabilities.
2. Including a droplet and contact isolation for all residents in the program is a useful alternative to wide-facility SARS-CoV-2 testing.
Authors’ declaration
Conflicts of interest to declare by author due to financial and personal relationships that could potentially bias this work: none.
- Sharma S, Singh G (2020) Prevalence and Global Impact of 2019-nCoV Zoonotic Viruses on China and World: Consequences of Chaotic and Stressed Environment. International Journal of Computer Applications and information technology 12: 333-348. Link: https://bit.ly/3qLZ83s
- Wu Z, McGoogan JM (2020) Characteristics of and Important Lessons From the Coronavirus Disease 2019 (COVID-19) Outbreak in China: Summary of a Report of 72?314 Cases From the Chinese Center for Disease Control and Prevention. JAMA 323: 1239-1242. Link: https://bit.ly/3gxmBRg
- Yang J, Zheng Y, Gou X, Pu K, Chen Z, et al. (2020) Prevalence of comorbidities and its effects in patients infected with SARS-CoV-2: a systematic review and meta-analysis. Int J Infect Dis 94: 91-95. Link: https://bit.ly/2IClHqk
- CDC COVID-19 Response Team (2020) Severe Outcomes Among Patients with Coronavirus Disease 2019 (COVID-19) — United States, February 12–March 16, 2020. MMWR Morb Mortal Wkly Rep 69: 343-346. Link: https://bit.ly/3n8l5HV
- Garg S, Kim L, Whitaker M, O’Halloran A, Kambhampati A, et al. (2020) Hospitalization Rates and Characteristics of Patients Hospitalized with Laboratory-Confirmed Coronavirus Disease 2019 - COVID-NET, 14 States, March 1-30, 2020. MMWR Morb Mortal Wkly Rep 69: 458-464. Link: https://bit.ly/2Kb1U1G
- McMichael TM, Currie DW, Clark S, Pogosjans S, Kay M, et al. (2020) Epidemiology of Covid-19 in a Long-Term Care Facility in King County, Washington. N Engl J Med 382: 2005-2011. Link: https://bit.ly/39ZtREC
- Blackman C, Farber S, Feifer RA, Mor V, White EM (2020) An Illustration of SARS-CoV-2 Dissemination Within a Skilled Nursing Facility Using Heat Maps. J Am Geriatr Soc 68: 2174-2178. Link: https://bit.ly/3gFimDy
- Mas Romero M, Avendaño Céspedes A, Tabernero Sahuquillo MT, Cortés Zamora EB, Gómez Ballesteros C, et al. (2020) COVID-19 outbreak in long-term care facilities from Spain. Many lessons to learn. PLoS One 15: e0241030. Link: https://bit.ly/39WV8qZ
- Telford CT, Onwubiko U, Holland DP, Turner K, Prieto J, et al. (2020) Preventing COVID-19 Outbreaks in Long-Term Care Facilities Through Preemptive Testing of Residents and Staff Members - Fulton County, Georgia, March-May 2020. MMWR Morb Mortal Wkly Rep 69: 1296-1299. Link: https://bit.ly/2JRVzYX
- Rolland Y, Lacoste MH, de Mauleon A, Ghisolfi A, De Souto Barreto P, et al. (2020) Guidance for the Prevention of the COVID-19 Epidemic in Long-Term Care Facilities: A Short-Term Prospective Study. J Nutr Health Aging 24: 812-816. Link: https://bit.ly/2VZNu79
- Abrams HR, Loomer L, Gandhi A, Grabowski DC (2020) Characteristics of U.S. Nursing Homes with COVID-19 Cases. J Am Geriatr Soc 68: 1653-1656. Link: https://bit.ly/37WFUzU
- Van den Brink AM, Gerritsen DL, Voshaar RC, Koopmans RT (2013) Residents with mental-physical multimorbidity living in long-term care facilities: prevalence and characteristics. A systematic review. Int Psychogeriatr 25: 531-548. Link: https://bit.ly/2JI5xMM
- Strausbaugh LJ, Sukumar SR, Joseph CL (2003) Infectious disease outbreaks in nursing homes: an unappreciated hazard for frail elderly persons. Clin Infect Dis 36: 870-876. Link: https://bit.ly/3m2A3Oj
- Lee MH, Lee GA, Lee SH, Park YH (2020) A systematic review on the causes of the transmission and control measures of outbreaks in long-term care facilities: Back to basics of infection control. PLoS One 15: e0229911. Link: https://bit.ly/3oxScoO
- Applegate WB, Ouslander JG (2020) COVID-19 Presents High Risk to Older Persons. J Am Geriatr Soc 68: 681. Link: https://bit.ly/37TSY95
- WHO () Preventing and managing the COVID-19 pandemic across long-term care services in the WHO European Region. Link: https://bit.ly/3naGzEg
- CDC (2020) Preparing for COVID-19: Long-term Care Facilities, Nursing Homes. Link: https://bit.ly/33ZqqKi
- Yen MY, Schwartz J, King CC, Lee CM, Hsueh PR (2020) Society of Taiwan Long-term Care Infection Prevention and Control. Recommendations for protecting against and mitigating the COVID-19 pandemic in long-term care facilities. J Microbiol Immunol Infect 53: 447-453.
- European Centre for Disease Prevention and Control.Surveillance of COVID-19 at long-term care facilities in the EU/EEA. Link: https://bit.ly/2Lok3tr
- Stone SP, Cooper BS, Kibbler CC, Cookson BD, Roberts JA, et al. (2007) The ORION statement: guidelines for transparent reporting of outbreak reports and intervention studies of nosocomial infection. Lancet Infect Dis 7: 282-288. Link: https://bit.ly/39ZK8cu
- Kimball A, Hatfield KM, Arons M, James A, Taylor J, et al. (2020) Asymptomatic and Presymptomatic SARS-CoV-2 Infections in Residents of a Long-Term Care Skilled Nursing Facility - King County, Washington, March 2020. MMWR Morb Mortal Wkly Rep 69: 377-381. Link: https://bit.ly/2LfuMGm
- Arons MM, Hatfield KM, Reddy SC, Kimball A, James A, et al. (2020) Presymptomatic SARS-CoV-2 Infections and Transmission in a Skilled Nursing Facility. N Engl J Med 382: 2081-2090. Link: https://bit.ly/3owyREC
- Min L, Galecki A, Mody L (2015) Functional disability and nursing resource use are predictive of antimicrobial resistance in nursing homes. J Am Geriatr Soc 63: 659-666. Link: https://bit.ly/3oCE0Ll
- Jing QL, Liu MJ, Zhang ZB, Yuan J, Zhang AR, et al. (2020) Household secondary attack rate of COVID-19 and associated determinants in Guangzhou, China: a retrospective cohort study. Lancet Infect Dis 20: 1141-1150. Link: https://bit.ly/3qJovmD
- Luo L, Liu D, Liao X, Wu X, Jing Q, et al. (2020) Contact Settings and Risk for Transmission in 3410 Close Contacts of Patients With COVID-19 in Guangzhou, China: A Prospective Cohort Study. Ann Intern Med 173: 879-887. Link: https://bit.ly/3oEOGZX
- Chiu S, Black CL, Yue X, Greby SM, Laney AS, et al. (2017) Working with influenza-like illness: Presenteeism among US health care personnel during the 2014-2015 influenza season. Am J Infect Control 45: 1254-1258. Link: https://bit.ly/3n6UTxj
- Tartari E, Saris K, Kenters N, Marimuthu K, Widmer A, et al. (2020) Not sick enough to worry? "Influenza-like" symptoms and work-related behavior among healthcare workers and other professionals: Results of a global survey. PLoS One 15: e0232168. Link: https://bit.ly/3oEjIB1
- Widera E, Chang A, Chen HL (2010) Presenteeism: a public health hazard. J Gen Intern Med 25: 1244-1247. Link: https://bit.ly/374G48W
- Zimmerman S, Gruber-Baldini AL, Hebel JR, Sloane PD, Magaziner J (2002) Nursing home facility risk factors for infection and hospitalization: importance of registered nurse turnover, administration, and social factors. J Am Geriatr Soc 50: 1987-1995. Link: https://bit.ly/3gxgPiy
- Lin H, Ng S, Chan S, Chan WM, Lee KC, et al. (2011) Institutional risk factors for norovirus outbreaks in Hong Kong elderly homes: a retrospective cohort study. BMC Public Health 11: 297. Link: https://bit.ly/2LkhM2h
- Shiao JS, Koh D, Lo LH, Lim MK, Guo YL (2007) Factors predicting nurses' consideration of leaving their job during the SARS outbreak. Nurs Ethics 14: 5-17. Link: https://bit.ly/37TRfR9
- Woodhead EL, Northrop L, Edelstein B (2016) Stress, Social Support, and Burnout Among Long-Term Care Nursing Staff. J Appl Gerontol 35: 84-105. Link: https://bit.ly/37Jj4LG
- Spencer SP, Karsies T (2019) Audit-and-Feedback and Workflow Changes Improve Emergency Department Care of Critically Ill Children. Pediatr Qual Saf 4: e128. Link: https://bit.ly/2IzCoTb
- Ellis G, Gardner M, Tsiachristas A, Langhorne P, Burke O, et al. (2017) Comprehensive geriatric assessment for older adults admitted to hospital. Cochrane Database Syst Rev 9: CD006211. Link: https://bit.ly/2Kbksi2
- Mitja O, Ubals M, Corbacho M, Alemany A, Suner S, et al. (2020) A Cluster-Randomized Trial of Hydroxychloroquine as Prevention of Covid-19 Transmission and Disease. Link: https://bit.ly/39Y8kvR
- Lee SH, Son H, Peck KR (2020) Can post-exposure prophylaxis for COVID-19 be considered as an outbreak response strategy in long-term care hospitals? Int J Antimicrob Agents 55: 105988. Link: https://bit.ly/3m46lZd
- Center for Disease Control and Prevention, Considerations for Use of SARS-CoV-2 Antigen Testing in Nursing Homes. Link: https://bit.ly/3lZZJv7
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
