Annals of Environmental Science and Toxicology
Application of the standard case definition in the case of Congo-Crimean Hemorrhagic Fever (CCHF) in the Zhambyl region of Kazakhstan
Andrey M Dmitrovskiy1,2*, Pak YeА3, Syzdykov МS1, Ryabushko YeA1, Kamytbekova KZh4 and Iskakova FA5
2National Center for Biotechnology, Almaty Branch (CRL), Kazakhstan
3Health Department of Zhambyl Region of Kazakhstan, Kazakhstan
4International Kazakh Turkish University, Kazakhstan
5Kazakh National University, Almaty, Kazakhstan
Cite this as
Dmitrovskiy AM, Pak YeА, Syzdykov МS, Ryabushko YeA, Kamytbekova KZH, et al. (2022) Application of the standard case definition in the case of Congo-Crimean Hemorrhagic Fever (CCHF) in the Zhambyl region of Kazakhstan. Ann Environ Sci Toxicol 6(1): 050-051. DOI: 10.17352/aest.000053Copyright
© 2022 Dmitrovskiy AM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.In the presented case, a typical example of CCHF is described, a patient who lives in an endemic territory and had risk factors for infection – cattle keeping and tick bite. The patient sought medical help in a timely mannert, but his diagnosis of CCHF was made late, due to underestimation of the risk factors for CCHF infection and non-use of the standard case definition. The correct diagnosis was made only after the appearance of the hemorrhagic syndrome. The appearance of bleeding in patients with CCHF presents a high risk of infection for others. But timely isolation and intensive treatment allowed for the prevention of infection of contact persons and save the patient’s life.
Introduction
CCHF is endemic to three southern regions of Kazakhstan, where cases of this infection are registered annually. As a rule, infection occurs after the bite of an infected tick. In rural areas, there is significant tick contamination of livestock, therefore, according to the case standard definition of the CCHF adopted in the Republic of Kazakhstan, contact with cattle is a risk factor for infection [1,2].
Clinical diagnosis of CCHF at the beginning of the disease is complicated by the fact that there is no leading - hemorrhagic syndrome, so the diagnosis is often made late. This can lead both to the death of the patient, as a result of untimely and improper treatment, and to infection of others, as a result of the lack of isolation of the patient [3,4].
This article is aimed at improving the knowledge of medical professionals on the clinical manifestations of CCHF and emphasizes the importance of assessing the risk factors of this infection and applying a standard case definition.
Case report
A 62-year-old man, a villager, fell ill on 15.07.22, when a fever of up to 40C, weakness, lower back pain appeared, and later liquid stools joined. Only on the 3rd day - 18.07.22 he applied to the rural outpatient clinic, - treatment with anti-inflammatory drugs was prescribed; the next day - 19.07.22 I applied to the central district hospital, - where they continued treatment with antipyretic and anti-inflammatory drugs.
21.07.22 – on the 6th day of the illness, a nosebleed appeared, only after that did the doctor of the rural outpatient clinic suspect a case of CCHF. She isolated the patient and passed an emergency notice. The patient was evacuated by an ambulance team to the infectious diseases department of the central district hospital.
Data were collected on the risk factors of infection: the patient keeps livestock at home, some insect (tick?) was removed from the back on 11.07.22 and a probable case of CCHF has been determined.
Upon admission, there is a sharp weakness, nosebleed, headache, and pain in the lumbar region. Body temperature 36.0; blood pressure - 70/50 mmHg; pulse 110/min; breaths – 22/min.
The condition is extremely severe due to severe intoxication, and hemorrhagic syndrome. The patient is inhibited, sluggish, and adynamic. The skin is dry and pale, there were small hematomas at the injection sites and petechial rashes. The tongue is dry, densely covered with a dark coating. The gums are bleeding. There was hypotension, thready pulse.
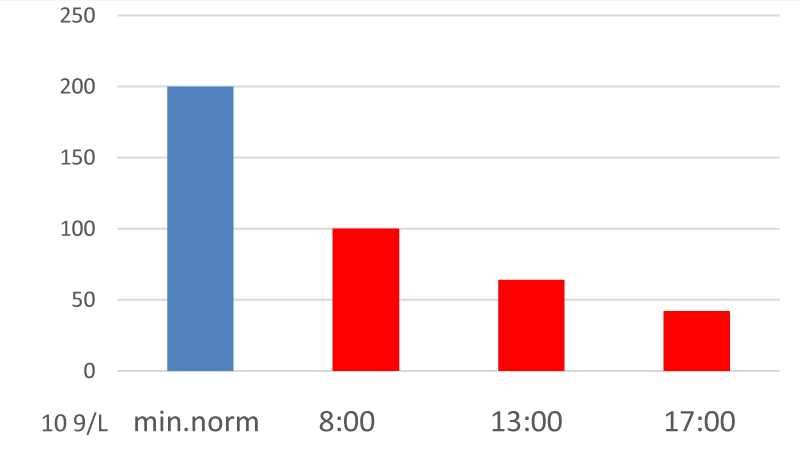
In the blood - a decrease in the dynamics of the number of platelets 100 – 64 - 42 × 10 9/L during the day (Figure 1), leukopenia - 2.8 × 10 9/L, hemoglobin 152 - 132 g/l. Coagulogram: PTI 84%; fibrinogen 3.79 g/l.
During the examination for CCHF - in the PCR test, the RNA of the CCHF virus was detected; in the ELISA test for antigens,- the antigen of the CCHF virus was detected; the ELISA test for antibodies was positive for IgM.
A confirmed case of CCHF was exposed.
The diagnosis was: “Congo-Crimean hemorrhagic fever, confirmed case, severe course. Complications: Infectious-toxic shock of 2 - 3 degrees; DIC syndrome”.
Treatment has begun: ribavirin, immune plasma, hemostatic therapy, infusion therapy with crystalloids, and the fight against DIC and shock.
As a result of the therapy, the patient recovered.
The patient was discharged in the third week after the appearance of clinical symptoms with normal coagulation parameters. The patient was taken on dispensary registration at the place of residence for further treatment and rehabilitation.
Clinical observation and laboratory testing revealed no cases of CCHF among the contact persons.
Discussion
All cases of fever in a territory endemic to CCHL, if there are risk factors for infection with CCHF in the history, should be treated as suspicious for CCHL Clinical diagnosis of CCHF in the pre-hemorrhagic period is difficult. Differential diagnosis in the presence of intestinal syndrome should be carried out with a group of intestinal infections, primarily salmonellosis; in the presence of respiratory syndrome - with a group of respiratory infections, currently, primarily with COVID-19. Also, the differential diagnosis should be carried out with other tick-borne infections, such as rickettsioses and borreliosis.
Conclusion
Clinical diagnosis of CHF at the beginning of the disease is difficult, for diagnosis it is necessary to take into account the risk factors of infection - living in an endemic area, tick bite, and the presence of livestock at home [5,6].
In the described case, unfortunately, the standard definition of the case was not applied in a timely manner and the diagnosis was made only on the 6th day of the illness, fortunately, the patient recovered and none of the people around him fell ill.
Thus, the presented case clearly demonstrates the need to identify the risk factors of infection with CCHF, and the application of the existing standard case definition, also demonstrates the need for medical workers to use PPE that is appropriate to the risk assessment when working with infectious patients.
- Dmitrovskiy АM, Sherrmetova MB, Egemberdiyeva RA, Shapiyeva JZh, Kuzmina AR, Utepbergenova GA. CCHF natural foci appearance and development dynamics in Turkestan region. Abstract book of XII international Jena Symposium on Tick-borne Diseases 21-23 March, Weimar, Germany. 2013; 80.
- Shapiyeva J, Kyraubaev K, Egemberdiyeva R, Dmitrovskiy A, Utegenova E, Usenov U, Shermetova M, Kuzmina A, Pak E. Epidemiological manifestations of CCHF in Kazakhstan. Abstract book of the Medical Biodefense Conference 2013, Munich, Germany, 2013; 39.
- Order of the Acting Minister of Health of the Republic of Kazakhstan No. 623 of December 15, 2006.
- Order of the KGSEN of the Ministry of Health of the Republic of Kazakhstan No. 84 dated March 28, 2013. "On improving the system of epidemiological surveillance and prevention of CCHF in Zhambyl, Kyzylorda and South Kazakhstan regions".
- Dmitrovskiy A, Shermetova M, Yegemberdiyeva R, Yeraliyeva L, Abdiyeva K, Shapiyeva J, Utepbergenova G, Kuzmina A, Pak E. Nosocomial Crimean-Congo hemorrhagic fever outbreak in Southern Kazakhstan // Abstract book of the Congress of Clinical Microbiology and Infectious Diseases, Barcelona, Spain, 2014; 227.
- Yegemberdiyeva R, Shapiyeva Z, Dmitrovskiy A, Tureberkov N. Spectrum of Tick-Borne disease patogenes in Kazakhstan. In materials of Connecting the Dots on Vector-borne Diseases, Oslo 2015; 32.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
