Archives of Depression and Anxiety
Maladaptive stress: Theoretical, neurobiological and clinical profiles
Giulio Perrotta*
Cite this as
Perrotta G (2021) Maladaptive stress: Theoretical, neurobiological and clinical profiles. Arch Depress Anxiety 7(1): 001-007. DOI: 10.17352/2455-5460.000057Stress is an adaptive response of the organism to an event that can be both internal and external, interfering at the endocrine, humoral, organic and biological levels: If the person reacts with all his resources, in a constructive and functional way, then we speak of "eustress", responding in an adaptive and functional way; if, on the other hand, the person fails to draw on his strategies, then we speak of "distress", giving rise to a more or less pervasive and serious form of maladaptation, which if reinforced with specific conditioning could give rise to one or more psychopathologies. It is therefore important to intervene on the person, according to a precise therapeutic plan, and on his mental and personality patterns, in order to remodel certain learned models that reinforce maladaptation and to support and assist the person in his process of awareness towards the invalidating and/or dysfunctional condition.
Contents of the manuscript
The General Concept of the "Stress"
Stress is a reaction that occurs when a person perceives an imbalance between the stresses received and the resources available to him or her, which has the function of re-establishing a new internal balance (homeostasis) as a result of external (e.g. a traffic accident) or internal (e.g. an illness) stressors that interfere at the endocrine, humoral, organic or biological level [1].
The term 'stress' was first introduced into biology by Cannon in 1935, but the syndrome was defined as such by Selye in 1936, and can be 'positive' (eustress) or 'negative' (distress), depending on a number of factors [2,3].
a) (Source) of stress: refers to the source of stress, but this factor alone does not explain the difference between eustress and distress, as it matters how one reacts to the stressful stimulus. Examples of stressors are organic sources (e.g., pain, hunger, thirst, physical trauma, and illness), environmental sources (e.g., outdoor temperature, noise, light, odour, and spatial uncertainty), psychological sources (e.g., fear, anxiety, boredom, value differences, and psychic trauma), and social-relational sources (e.g., interpersonal uncertainties).
b) (Typology) of the stressful stimulus: refers to the range of characteristics of the stimulus; when it is linked to a traumatic event, its repetition is experienced negatively.
c) (Intensity) of the stressful stimulus: refers to the perceived severity of the stressful stimulus; when it is particularly intense in severity and power, the person will experience it negatively.
d) (Frequency) of the stressful stimulus: refers to how many times in time the stressful stimulus occurs; when it is repeated and constant in time, even in a short period, the person will perceive it as threatening and dangerous and therefore negatively.
e) Adaptive reaction to the stressful stimulus (Coping): this refers to the defence mechanisms and strategies implemented by the person suffering the stressful stimulus; the more tools the person has, the more positive and constructive his/her reaction will be.
Let's take some examples to better understand the difference:
1) "I am in an isolated place and there is a large stray dog in front of me". The presence of the stray (source) large dog (type) is a stressogenic stimulus, as it instils fear and dread, regardless of the animal itself, because the external circumstances are one of isolation. This stressful stimulus in itself is capable of creating a disturbance in the psychophysical balance. The body reacts to the stimulus with stress. At this point, everything depends on the person's reaction: if he/she has sufficient coping strategies, he/she will react positively and thus find a solution to avoid the danger or damage; if not, he/she will react negatively and risk exposing him/herself even more to damage and danger. The intensity and frequency of the stimulus will partly condition the person's reaction, depending on the real danger, on the real strategies that could be implemented and on possible previous traumas linked to that stressful source (for example, a previous aggression by a big dog).
2) "I am a woman and I am alone in a dark alley in a town I do not know". The dark alley, being a woman, alone, defenceless, and in a place one does not know, are all stressors that can break the psychophysical balance; however, the person's reaction will depend on whether he/she can find solutions to avoid potential harm or danger, or whether he/she has been a victim of rape in the past.
In general, responses following exposure to stressors can be grouped in two ways [2,4].
a) Instantaneous responses, due to the nature and physiology of the nervous system (e.g. the sympathetic nervous system using already synthesised and stored neurotransmitters);
b) Delayed responses, due to the nature and physiology of the endocrine and neuroendocrine systems (e.g. stressor reception, activation of transcription of hormone-synthesising proteins and synthesis of hormones released into the humoral circulation).
Factors modulating stress and its adaptive function
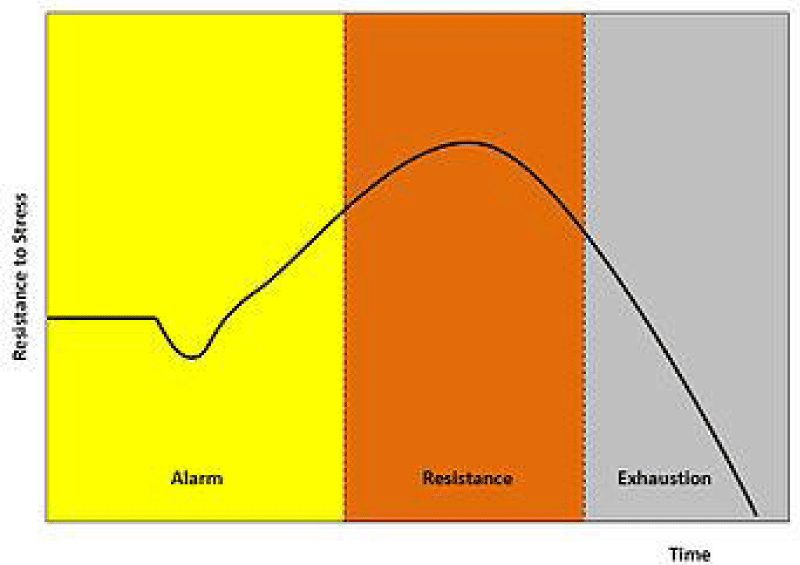
Each stressor immediately evokes neuropsychic, emotional, locomotor, hormonal and immunological regulatory reactions that form a general framework known as the General Adaptation Syndrome according to Selye's model, which he defined as the response the organism puts into action when subjected to the prolonged effects of multiple stressors, such as physical (e.g. fatigue), mental (e.g. work commitments), social or environmental (e.g. the obligations or demands of the social environment) stimuli [1] Figure 1.
Adaptation is a complex activity that involves the implementation of finalistic actions designed to change the internal balance of the organism (homeostasis) by generating a subjective emotional response, defending the organism from the stressor and implementing strategies to be elaborated in the event of future exposure to stressors, but also to change the balance outside the organism (environment), in order to adapt it to the needs of the subject. These two aspects may vary according to multiple factors, but in general the response in vertebrates is based on a constant and stereotyped pattern of action [5].
The greater or lesser success of the adaptive processes (adaptive capacity) is given by the balance between the qualitative and quantitative characteristics of the events that trigger them and the personal resources of the subject involved. As far as the "qualitative characteristics" are concerned, we consider temperamental and personality characteristics, cultural and intellectual level, socio-economic conditions and subjective resonance to the event; as far as the quantitative characteristics are concerned, we consider a time axis and therefore the age of the subject, his reaction time, the time required by the event to achieve effective adaptation and the duration of exposure to the stressor [6].
The evolution of General Adaptation Syndrome occurs in three stages [7,8].
1. Stage 1: Alarm reaction. Stage 1 can be subdivided into two phases: a) Shock phase: The organism receives the stressor and still has to work out a response to deal with it (e.g. it has to decide whether to change the internal or external environment). Adaptation is not yet present and therefore resistance against the stressor is minimal. b) Antishock phase: The body responds to stressors by implementing both physical and mental coping mechanisms. Examples are increased heart rate, blood pressure, muscle tone and arousal (psychophysiological activation). In general the physical response is activated: a) Instantaneously: the sympathetic system → medullary adrenal system; this allows the release of catecholamines into the bloodstream (thus explaining the tachycardia, muscle contraction and other factors typical of the attack or flight reaction). b) After a few hours and partially: the endocrine axis hypothalamus → pituitary → adrenal system; this allows the release of glycoactive hormones (e.g. corticosteroids) into the bloodstream.
2. Stage 2: Resistance. The body attempts to combat and counteract the negative effects of prolonged fatigue by producing specific hormonal responses from various endocrine glands, e.g. the adrenal glands. The delayed type response is the predominant response and its duration is related to the duration of exposure to the stressor and the amount of energy reserves in the body.
3. Stage 3: Exhaustion or Recovery. "Exhaustion", if the stressors continue to act, the subject may be overwhelmed and permanent adverse effects may occur in the psychic and/or somatic structure; "Recovery", if the body has managed to eliminate the effects of the stressor (modification of the internal environment, or of the homeostatic set-point) or the stressor itself (modification of the external environment). An example of a simple and stereotyped response is as follows: exposure to stressors or prediction of a stressor in the future (feed-forward mechanism); reception of the stressor and possible processing of the message; implementation of the adaptation syndrome and modification of the normal values ('set points') of various homeostatic systems; adaptation or resolution of the problem.
The neurobiological basis
Recent discoveries clarify both how the brain perceives and generates stressful stimuli, and the reactions that can occur when the body's defences against stress fail. The brain's response to stressful agents has changed little since early human ancestors either fought or fled for survival. In humans, as in animals, the basic physiological mechanisms of stress activation are always the same: the nervous pathway, with release of catecholamines, and the endocrine pathway, with secretion of corticosteroids. Moreover, in humans as in animals, the stress response is always non-specific, it is an attack/run response not differentiated according to the type of stressful event. The most important physiological processes that are activated in the stress condition therefore operate along these two paths. The first is the nervous pathway consisting of the orthosympathetic (i.e. the sympathetic nervous system, that part of the autonomic nervous system which regulates the essential functions of the body) and the medullary portion of the adrenal glands. When faced with a stressful stimulus and formulating an appropriate response, the brain promptly activates the nerve pathways from the control centres in the brainstem: this results in the release of catecholamines, noradrenaline at various sites and adrenaline from the adrenal glands (located just above the kidney). The dual release underlies the attack-escape response, the classic and prompt reaction needed in dangerous situations. Catecholamines enable us to deal with the event quickly and effectively. Due to the action of catecholamines, the heart speeds up its activity, supplying more blood to the brain and muscles; arteries and veins under the skin narrow and the blood clotting time shortens, removing the danger of profuse bleeding in the event of injury; breathing becomes rapid and deep, supplying more oxygen; the mucous membranes of the first airways dry up, making it easier for the air to travel to the lungs; sweating increases, refreshing the body; many muscles tense up strongly, preparing for rapid and vigorous action; finally, the mind becomes very alert, grasping the slightest clue and refining all intellectual capacities. Functions that could absorb energy and disturb this state of alertness, such as eating and digesting, are slowed down and suspended. Skin receptors then give rise to the straightening of hair (goose bumps) and intestinal receptors cause that uncomfortable abdominal sensation one experiences in stressful situations. These symptoms are preparatory to attack or escape and increase the blood supply to the vital organs, muscles and brain.
Usually, all these changes due to catecholamines are short-lived and when the alarm ceases, normal levels are quickly restored. The problems begin when the alarm continues over time and the activation becomes excessive. The same organic response triggered by catecholamines is at the basis of the syndrome which, in the 1920s, the physiologist Cannon called fight-or-flight syndrome: that is, the organic and psychic condition in which all a person's energies, when faced with an enemy or a danger, are mobilised to attack or to run for their lives. It is this condition that allowed primitive man to survive long enough to procreate. Today, however, things have changed and the open response of fight or flight is not always possible. If someone bothers us, hinders us in achieving a goal, or simply does not meet our expectations and needs (and as a 'nuisance' we consider him to be an 'aggressor') our body reacts quickly as it would have done thousands of years ago: it charges in to pounce on him with punches, kicks and bites. On the other hand, if our brain perceives that the intruder is bigger and stronger than us and it is not wise to challenge him, the energy in our body allows us to retreat and run away. These two behaviours, however, are neither allowed by the rules of social life, nor are they dignified; the good thing is that we should also sketch a small smile, take it in, and with savoir faire. But how can we use our catecholamines and energy for fight or flight? That is the problem of modern man. The accumulation of these charges is unhygienic and could sooner or later affect us in a variety of ways. Good manners are not always healthy. Repressed anger, for example, increases blood pressure in many cases. The second pathway along which the physiological processes of stress operate is the neuroendocrine pathway and consists of the activation of a cerebro-somatic circuit known as the HPA axis, which connects the hypothalamus, pituitary gland, adrenal cortex and hippocampus by transporting specialised hormones through the blood stream. The hypothalamic-pituitary-adrenal axis (HPA) is the central coordinator of neuroendocrine stress response systems. The amygdala also plays a crucial role in this system. Located in the phylogenetically 'old' part of the brain, the amygdala, a small, almond-shaped region at the front of the brain, plays an important role in the stress response. Information from the senses that can signal danger - visual perceptions and sounds - reaches the amygdala in a direct line, short-circuiting the cerebral cortex, the phylogenetically 'youngest' structure of the brain in which higher processes such as reasoning are processed. Sensory information also reaches the cerebral cortex, but the route to the amygdala is shorter and more direct, and therefore also less time-consuming.
Joseph LeDoux has called this pathway of stress response the inferior pathway, travelled in those crucial milliseconds before the stressful event becomes apparent. While the cerebral cortex is still analysing the stressful stimulus, the amygdala is already in action, sending chemical messages that trigger a cascade of reactions both in the brain and in the body in general. In response to the stressful stimulus, the amygdala sends signals to the hypothalamus. The hypothalamus is the key area for regulating hormonal balance: it receives fibres from the areas of the brain that process emotional information, including the amygdala, and from the regions of the brainstem that control sympathetic nerve responses, and integrates the information to produce a hormonal response, the release of Corticotropin-Releasing Hormone (CRH), which stimulates the next station, the pituitary gland. CRH stimulates the production and release of Adrenocorticotropin (ACTH) from the anterior pituitary gland. ACTH, in turn, stimulates the release of glucocorticoids, primarily cortisol, from the cortex of the adrenal glands. Cortisol is the key steroid hormone for understanding the next phase of the stress response. It raises blood levels of both sugars, stimulating the liver to release more sugar into the blood, and of other metabolites such as fatty acids and amino acids, often at the expense of proteins, which are broken down into readily available energy substances (a sort of instant 'energy bar' for muscles and brain). Cortisol, like adrenaline, raises blood pressure and, in simple terms, makes you feel better: more toned up and performing, less likely to feel fatigue and pain, and less likely to be distracted by worries or distractions. Cortisol also inhibits other phenomena such as growth, digestion, inflammation and even wound healing and sexual urges, things that can be done better at other times. Pain receptors are repressed. Selye called these corticosteroid hormones 'adaptive hormones' because they help us adapt to stressors. They are comparable to the oil that lubricates the engine of a car, keeping it running at its best. There is therefore a synergism of the effect of catecholamines (adrenaline and noradrenaline) and corticosteroids: the combination of these hormones helps to load the body in the best way possible to cope with stressful agents. The emergency response system continues to pump powerful hormones into the body until the brain perceives that the danger has passed. When it is effectively over, the system deactivates and hormone levels return to normal. If the system is well regulated, it switches on and off according to the body's needs. If, on the other hand, its functioning is disturbed, the stress response can generate disturbances in the brain as well as in other parts of the body, such as the heart or the immune system. All these substances, catecholamines and corticosteroids, are in fact an excellent source of energy, but their excessive production due to strong and prolonged stress becomes harmful. If too much sugar is released, it is difficult for it to be fully utilised, which can lead to diabetes-like conditions. Releasing too much fat leads to an increase in cholesterol and triglycerides and possibly to atherosclerotic disorders. When too many amino acids are mobilised from various organic structures in a process of disintegration, muscle mass is reduced, the skin thins and lymphoid tissue volumes decrease, the latter leading to a weakening of the immune system. This suggests the atrophy of the thymus, spleen, lymphatic ganglia and all other lymphoid tissues observed by Selye in his early research. Selye's third symptom, gastric and duodenal ulcers, was also due to the large quantities of corticosteroids in his system. These substances damage the cells of the gastric mucosa, leading to gastritis, ulcerative lesions and bleeding. The last stage of the HPA circuit is the feedback mechanism of cortisol on the brain, in particular on the hippocampus and the amygdala. The normalisation of hormone levels depends in fact on the hippocampus, a key structure for learning, memory and the cognitive aspects of emotions, located in the temporal lobe. The highest density of receptors for cortisol is in fact located in the hippocampus. The receptors are of two types: low MR and high GR. Low MR is activated by normal levels of circulating cortisol in the HPA axis and maintains normal general metabolism and brain processes. However, when cortisol levels start to rise, especially in the morning, the high GR gradually starts to be activated. In stressful situations, cortisol levels rise sharply and activate these receptors, while the hippocampus is inhibited by a genetically controlled program. The hippocampus moderates the system's reaction and detects the amount of stress hormone present in the blood and orders the thalamus to curb the hormone cascade. At the same time the amygdala, which lacks the cognitive capabilities of the cerebral cortex, can sense that danger is still present, and send inputs to the hypothalamus to maintain the flow of hormones. In the meantime, cortisol also continues to act on the amygdala, which processes fear and anxiety (with the effect of activating it to enable fear learning), and deactivating the hippocampus (to ensure that resources are not wasted on unnecessary aspects of learning). If this cascade persists - as it can under the influence of numerous somatic or psychic factors - the function of the hippocampus risks being impaired. Under continuous pressure, the hippocampus cannot perform its normal function and a vicious circle is created.
The result is a persistent state of activation and alertness that renders the body's natural defence system uncontrollable. This prolonged state comes at a high cost. It places a strain on the entire organism, which in the long term can lead to very negative consequences. A graphic representation of the process shows a bell curve that relates stress to brain function: little stress is good, a little more is better, but too much is bad. Since the reaction to stress is controlled by the brain, researchers have long believed that stress can directly damage its structure. It is now clear that the amount of stress hormones an individual is exposed to during his or her lifetime is a determining factor in diseases of the brain and the body in general. Genetic and somatic factors play a significant role, as does the environment in which development takes place before and after birth. Lifestyle choices (diet, physical activity, smoking or alcohol consumption) can also indirectly exacerbate the harmful effects of stress. Environmental factors, in particular, can change the genome of organisms and thus directly affect the development and evolution of species. Animal experiments have provided convincing evidence in this regard, and new brain imaging of survivors of high-stress episodes confirms these effects in humans. Studies carried out on mice and primates show that severe and prolonged stress has a detrimental effect directly on cells in the hippocampus and beyond. Scientists have observed a deterioration of the dendrites, structures comparable to 'arms' through which these cells receive signals from neighbouring cells. Over time, this leads to significant atrophy of the hippocampus. More recently, researchers have used magnetic resonance imaging to document changes in the hippocampus observed in people suffering from post-traumatic stress-related disorders, such as veterans or war victims, or people who were abused in childhood. Observations in several laboratories, including Dr McEwen's, provide significant evidence that moderate and prolonged stress can cause damage to the hippocampus. The growing number of results demonstrating the consequences of moderate stress, as experienced daily by many individuals, raises important and inescapable questions about the health and behaviour of modern man. In the cardiovascular system, this mechanism has been well understood: stressful experiences can exacerbate heart disease and an acute stress episode can trigger a cardiac crisis. Stress also plays a role in depression, gastroduodenal ulcers and diseases with an immune component, such as rheumatoid polyarthritis, viral infections and cancer. In some chronic brain diseases, excessive plasma cortisol levels are present. In particular, in severe depression, there is an overproduction of cortisol. Recent studies indicate that the hippocampus also appears to be reduced in size. These findings have led psychiatrists to regard major depression as a condition of prolonged stress. We do not know at the moment whether the increase in cortisol is the primary cause of this disease rather than the consequence of severe psychological decompensation and the resulting stress. Patients do, however, benefit from inhibiting the production or action of cortisol, especially in cases where classic antidepressants are ineffective. Antidepressants often serve to normalise the overactivity of the HPA axis, in part by regulating the density of MR and GR receptors in the brain, especially in the hippocampus. Neuroscientists hope to develop more effective treatments for stress disorders that work by readjusting the retroactive control system and reducing the excessive hormonal response. Brain ageing is accompanied by a general decline in higher functions that varies greatly from individual to individual: some (good ageing), retain good cognitive abilities while others do not (bad ageing). Is it possible to provide an explanation at the molecular level? Cortisol levels are only higher in bad ageing than in good ageing. The increase in cortisol precedes the decline in mental abilities, which are associated with a decrease, observed in brain scans, in the size of the hippocampus. Experiments on guinea pigs have shown that keeping the level of the stress hormone low from birth, or even from an intermediate age, prevents the onset of memory disorders typical of untreated subjects. It appears that individuals with an excessive hormonal response to stress (not the most stressed, but those who respond most to stressful stimuli) are those who show greater memory impairment and other cognitive disorders with age [8-14].
Neuropathological and psychopathological profiles
A maladaptive response to a stressful event may lead to the onset of a pathological picture. In the case of a psychological disorder, the clinical picture will mimic the expression of a major disorder from a symptomological point of view. Maladaptive behaviour may be of clinical interest if it consists of emotional or behavioural symptoms that cause subjective suffering and a significant impairment in the subject's social and work functioning. The subject's characteristics of fragility or rigidity play an important role when the subject has to produce strategies to respond appropriately to a change in the environment. The characteristics of the stress syndrome are: a) symptoms preceded by an identifiable stressful event, whether positive or negative; b) occurring within the three months preceding the development of the symptoms; c) must be more intense than the corresponding normal reactions; d) have a tendency to resolve spontaneously within a defined period of time (6 months); e) the syndrome must not represent an exacerbation of the symptoms of an underlying mental disorder, whether or not linked to the stressful event; f) must be associated with a mental illness; g) must be associated with a mental disorder, whether or not linked to the stressful event; h) must be associated with a mental disorder, whether or not linked to the stressful event [2].
The diagnosis of the level of chronic stress to which an individual is subjected is neither simple nor unambiguous, given the generality of the phenomenon and the subjectivity in reacting to different stress factors. The most classic method for measuring stress levels, which is purely psychological, is based on filling in questionnaires that investigate either the presence in the patient's life (in the present or near past) of stress factors (such as the loss of loved ones or of work), or the occurrence of stress-related symptoms or psychophysical pathologies [1]. In particular: [1] In particular: a) in "neurotic states", the maladaptive response involves a fear of not being able to cope with negative consequences, leading to chronic conditions such as anxiety, panic, depression and sleep-wake rhythm disorders; b) in "borderline states", the maladaptive response involves a progressive but constant disruption of the reality plane, linked to the loss of control and circumstances beyond one's control; c) in "psychotic states", the maladaptive response is completely absorbed by the impairment of the reality plane [15-50]. In the theoretical model at the basis of PICI-1 there is precisely the concept of stress (and trauma): the basis of all psychopathologies is in fact the inability of the subject to adapt in a functional way to a stress that according to its severity, intensity and frequency has become a real trauma (the origin of every psychopathology) [51,52].
It is clear that subjectivity in reacting to stress factors, or in the evaluation of symptoms themselves, is the main problem with this methodology, which is however widely adopted in the state of the art. In an attempt to make the assessment as objective as possible, the last few decades have seen a shift to studying the physiological alterations of stress, which mainly depend on sympathetic hyperactivation and inhibition of the parasympathetic compartment, mainly affecting cardiac effectors. As the sympathetic system is activated by the secretion of noradrenaline, the flow/level of this neurotransmitter can be measured by blood analysis. Alternatively, the level of ACTH and cortisol, an immunosuppressant and potentially diabetic-releasing hormone released during stress, can be measured in blood, urine or saliva. Stress has the same effect on oxytocin (also due to cortisol) [53]. A completely different method is based on the study of cardiac and blood pressure activity in the subject, since heart rate and blood pressure depend essentially on the balance of sympathetic-vagal activity. By monitoring the subject by means of the electrocardiogram and a Holter pressure monitor in an environment carefully prepared to be devoid of any stimuli (white walls, adequate air and room temperature, silence) one can, with relative accuracy, measure the patient's vegetative state. Stress can then be quantified instrumentally as the variation of three factors: skin impedance, pressure pattern, Heart Rate Variability (HRV). It was found that, in the case of a stressed subject, there is an increase in skin impedance, as well as a stable increase in blood pressure at rest of 10mmHg, both in clinostatism and in orthostatism. But the indices that have proved most indicative are the frequency study of the variation in the length of heartbeats, an analysis carried out from a tacogram, a graph obtained from a normal ECG by placing the sequence of heartbeats on the abscissa and their length on the ordinate (normally calculated from the peak of the R wave taken into consideration to the next peak of the R). The distribution of power at different frequencies changes in a peculiar way depending on the level of stress: in particular, an activation of the sympathetic system decreases the power distributed at higher frequencies. [8] There are also pathological physical conditions that can negatively interfere with the ability to react positively to stressful events, by depressing the immune system: this occurs in autoimmune, rheumatoid and hyperhistamine diseases [54].
Una forma particolare di stress: Stress da lavoro
A particular form of stress: Work-related stress (burn-out), which is not a pathology in itself but a cause for which the worker may be absent due to the state of malaise caused by overwork, the compression of his rights, insufficient rewards, lack of fairness, conflicting values, poor remuneration or, more generally, even personal harassment received from colleagues or superiors, which is so intense and frequent as to induce the worker into a real state of continuous anxiogenic stress characterised by specific psychophysical symptoms [55,56].
Conclusion
Stress, as we can see, is a precise adaptive response of the organism to one or more events that can be both internal and external, capable of interfering at an endocrine, humoral, organic and biological level. If the person reacts with all his resources, in a constructive and functional way, then we speak of 'eustress', responding in an adaptive and functional way; if, on the other hand, the person is unable to draw on his strategies, then we speak of 'distress', giving rise to a more or less pervasive and serious form of maladaptation, which if reinforced with specific conditioning could give rise to one or more psychopathologies. It is therefore important not to demonise stressful events per se, as they are functional to overcoming one's difficulties and personal growth, but rather to intervene on the person's psychic processes, according to a precise therapeutic plan, and on his mental and personality patterns, in order to remodel certain appressed models that reinforce maladaptation, supporting and assisting the person in his process of awareness towards the resolution of the invalidating and/or dysfunctional condition [57-59].
- Perrotta G (2019) Psicologia generale, Luxco Ed, 1st ed.
- Perrotta G (2019) Psicologia clinica, Luxco Ed, 1th ed.
- Perrotta G (2019) Psicologia dinamica, Luxco Ed, 1th ed.
- Pancheri P (1983) Stress, emozioni, malattia, Mondadori ed.
- Di Nuovo S, Rispoli L, Genta E (2000) Misurare lo stress. Il Test M.S.P. e altri strumenti per una valutazione integrata, Franco Angeli.
- Lucini D, Riva S, Pizzinelli P, Pagani M (2007) Stress management at the worksite: reversal of symptoms profile and cardiovascular dysregulation. Hypertension 49: 291-297. Link: http://bit.ly/3q6qRef
- Selye H (1956) The Stress of life. McGraw-Hill (Paperback), New York.
- Kandel ER (2017) Principi di Neuroscience, Casa Editrice Ambrosiana.
- LeDoux J (1996) The Emotional Brain. The Mysterious Underpinnings of Emotional Life, New York, Simon & Schuster. Link: http://bit.ly/35w61gm
- McEwen BS, Morrison JH (2013) Brain on stress: vulnerability and plasticity of the prefrontal cortex over the life course. Neuron 79: 16-29. Link: http://bit.ly/3bqNrtW
- Heim C, Nemeroff CB (2009) Neurobiology of posttraumatic stress disorder. CNS Spectr 14: 13-24. Link: http://bit.ly/3sdkOXa
- Shin LM, Liberzon I (2010) The neurocircuitry of fear, stress, and anxiety disorders. Neuropsychopharmacology 35: 169-191. Link: https://go.nature.com/39qxKAy
- Khosrowabadi R (2018) Stress and Perception of Emotional Stimuli: Long-term Stress Rewiring the Brain. Reza 9: 107-120. Link: https://bit.ly/35vseLD
- Dragos D, Tănăsescu MD (2010) The effect of stress on the defense systems. J Med Life 3: 10-18. Link: http://bit.ly/2LnJ6gz
- Perrotta G (2019) Anxiety disorders: definitions, contexts, neural correlates and strategic therapy. J Neur Neurosci 6: 046. Link: https://bit.ly/2WSmiaT
- Perrotta G (2019) Neural correlates in eating disorders: Definition, contexts and clinical strategies. J Pub Health Catalog 2: 137-148. Link: https://bit.ly/3mWmf8s
- Perrotta G (2019) Post-traumatic stress disorder: Definition, contexts, neural correlations and cognitive-behavioral therapy. J Pub Health Catalog 2: 40-47. Link: https://bit.ly/3rvaCc6
- Perrotta G (2019) Autism Spectrum Disorder: Definition, contexts, neural correlates and clinical strategies. J Neurol Neurother 4: 136. Link: https://bit.ly/2L0pNcK
- Perrotta G (2019) Sleep-wake disorders: Definition, contexts and neural correlations. J Neurol Psychol 7: 09. Link: https://bit.ly/3hoBiGO
- Perrotta G (2019) Depressive disorders: Definitions, contexts, differential diagnosis, neural correlates and clinical strategies. Arch Depress Anxiety 5: 009-033. Link: https://bit.ly/2KADvDm
- Perrotta G (2019) The phenomenon of demoniac possession: definition, contexts and multidisciplinary approaches. J Psychology and Mental Health Care 3: 1-019. Link: https://bit.ly/3mYYSLz
- Perrotta G (2019) Panic disorder: definitions, contexts, neural correlates and clinical strategies. Current Trends in Clinical & Medical Sciences 1. Link: https://bit.ly/38IG6D5
- Perrotta G (2019) Obsessive-Compulsive Disorder: definition, contexts, neural correlates and clinical strategies. Cientific Journal of Neurology 1: 08-16. Link: https://bit.ly/3pxNbNu
- Perrotta G (2019) Behavioral addiction disorder: definition, classifications, clinical contexts, neural correlates and clinical strategies. J Addi Adol Beh 2. Link: https://bit.ly/3rAT9ip
- Perrotta G (2019) Alzheimer's disease: definition, contexts, neural correlates, strategies and clinical approaches. J Aging Stud Ther 1. Link: https://bit.ly/2KMINeK
- Perrotta G (2019) Parkinson's disorder: definition, contexts, neural correlates, strategies and clinical approaches. J Neurosci Neurol Surg 4. Link: https://bit.ly/3bmsGj8
- Perrotta G (2019) Delusions, paranoia and hallucinations: definitions, differences, clinical contexts and therapeutic approaches. Cientific Journal of Neurology (CJNE) 1: 22-28.
- Perrotta G (2019) The acceptance in the elaboration of mourning in oncological diseases: definition, theoretical models, and practical applications. Needs analysis and subjective oncological reality. Biomed J Sci Tech Res 21.
- Perrotta G (2019) Paraphilic disorder: definition, contexts and clinical strategies. J Neuro Research 1: 4. Link: https://bit.ly/3oxAHFL
- Perrotta G (2019) Attention Deficit Hyperactivity Disorder: definition, contexts, neural correlates and clinical strategies. J Addi Adol Behav 2. Link: https://bit.ly/3aQyWiU
- Perrotta G (2019) Tic disorder: definition, clinical contexts, differential diagnosis, neural correlates and therapeutic approaches. J Neurosci Rehab 1-6. Link: https://bit.ly/3rEagQm
- Perrotta G (2019) Internet gaming disorder in young people and adolescent: a narrative review. J Addi Adol Behav 2.
- Perrotta G (2019) Bipolar disorder: definition, differential diagnosis, clinical contexts and therapeutic approaches. J Neuroscience and Neurological Surgery 5. Link: https://bit.ly/34SoC67
- Perrotta G (2019) The reality plan and the subjective construction of one's perception: the strategic theoretical model among sensations, perceptions, defence mechanisms, needs, personal constructs, beliefs system, social influences and systematic errors. J Clinical Research and Reports 1. Link: https://bit.ly/3b34baH
- Perrotta G (2020) Psychological trauma: definition, clinical contexts, neural correlations and therapeutic approaches. Curr Res Psychiatry Brain Disord: CRPBD-100006. Link: https://bit.ly/37UD3bz
- Perrotta G (2020) Human mechanisms of psychological defence: definition, historical and psychodynamic contexts, classifications and clinical profiles. Int J Neurorehabilitation Eng 7: 1. Link: https://bit.ly/2L0I5dJ
- Perrotta G (2020) Suicidal risk: definition, contexts, differential diagnosis, neural correlates and clinical strategies. J Neuroscience Neurological Surgery 6: 114. Link: https://bit.ly/3aMqcu5
- Perrotta G (2020) Pathological gambling in adolescents and adults: definition, clinical contexts, differential diagnosis, neural correlates and therapeutic approaches. ES J Neurol 1: 1004. Link: https://bit.ly/34RmUlj
- Perrotta G (2020) General overview of “human dementia diseases”: definitions, classifications, neurobiological profiles and clinical treatments. Journal of Gerontology & Geriatrics Studies 6. Link: https://bit.ly/39d8zkw
- Perrotta G (2020) The concept of altered perception in "body dysmorphic disorder": the subtle border between the abuse of selfies in social networks and cosmetic surgery, between socially accepted dysfunctionality and the pathological condition. J Neurol Neurol Sci Disord 6: 001-007. Link: https://bit.ly/3hrVNCD
- Perrotta G (2020) Dysfunctional attachment and psychopathological outcomes in childhood and adulthood. Open J Trauma 4: 012-021. Link: https://bit.ly/2Mi2ThB
- Perrotta G (2020) Neonatal and infantile abuse in a family setting. Journal of Pediatrics and Child Health. Open J Pediatr Child Health 5: 034-042. Link: https://bit.ly/2KApVQo
- Perrotta G (2020) Alien Abduction Experience: definition, neurobiological profiles, clinical contexts and therapeutic approaches. Ann Psychiatry Treatm 4: 025-029. Link: https://bit.ly/37W6j1T
- Perrotta G (2020) Sexual orientations: A critical review of psychological, clinical and neurobiological profiles. Clinical hypothesis of homosexual and bisexual positions. Int J Sex Reprod Health Care 3: 027-041. Link: https://bit.ly/38DtEVa
- Perrotta G (2020) Pedophilia: definition, classifications, criminological and neurobiological profiles and clinical treatments. A complete review. Open J Pediatr Child Health 5: 019-026. Link: https://bit.ly/38Jzggz
- Perrotta G (2020) Gender dysphoria: definitions, classifications, neurobiological profiles and clinical treatments. Int J Sex Reprod Health Care 3: 042-050. Link: https://bit.ly/2L0hLk6
- Perrotta G (2020) Cuckolding and Troilism: definitions, relational and clinical contexts, emotional and sexual aspects and neurobiological profiles. A complete review and investigation into the borderline forms of the relationship: Open Couples, Polygamy, Polyamory. Ann Psychiatry Treatm 4: 037-042. Link: https://bit.ly/3mVRoZP
- Perrotta G (2020) Borderline Personality Disorder: definition, differential diagnosis, clinical contexts and therapeutic approaches. Ann Psychiatry Treatm 4: 043-056. Link: https://bit.ly/3hx2B1N
- Perrotta G (2020) Narcissism and psychopathological profiles: definitions, clinical contexts, neurobiological aspects and clinical treatments. J Clin Cases Rep 4: 12-25. Link: https://bit.ly/2KCwxOa
- Perrotta G (2020) Dysfunctional sexual behaviors: definition, clinical contexts, neurobiological profiles and treatments. Int J Sex Reprod Health Care 3: 061-069. Link: https://bit.ly/3hxT4aU
- Perrotta G (2020) Perrotta Integrative Clinical Interview. LK ed., I ed., pag 270, formato A5.
- Perrotta G (2020) The structural and functional concepts of personality: The new Integrative Psychodynamic Model (IPM), the new Psychodiagnostic Investigation Model (PIM) and the two clinical interviews for the analysis of personality disorders (Perrotta Integrative Clinical Interview or PICI) for adults and teenagers (1TA version) and children (1C version), Psychiatry Peertechz, E-book.
- Perrotta G (2020) Oxytocin and the role of “regulator of emotions”: definition, neurobiochemical and clinical contexts, practical applications and contraindications. Arch Depress Anxiety 6: 001-005. Link: https://bit.ly/2JqvAYr
- Perrotta G (2020) The clinical and psychopathological implications in the forms of hyperhistaminosis. Online J Neuro Br Disord 4: 12. Link: https://bit.ly/3rBIh40
- Roy I (2019) Burnout Syndrome: definition, typology and management. Soins Psychiatr 39: 12-19. Link: http://bit.ly/3ozLuiv
- Mauranges A (2018) Symptoms and characteristics of burnout. Soins 63: 28-32.
- Perrotta G (2020) The strategic clinical model in psychotherapy: theoretical and practical profiles. J Addi Adol Behav 3: 5. Link: https://bit.ly/3rALHUG
- Perrotta G (2020) Accepting "change" in psychotherapy: from consciousness to awareness. Journal of Addiction Research and Adolescent Behaviour 3.
- Bienertova-Vasku J, Lenart P, Scheringer M (2020) Eustress and Distress: neither good nor bad, but rather the same? Bioessays 42: e1900238. Link: https://bit.ly/3q7YNHj
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
