Archives of Clinical Nephrology
Tunneled femoral catheters and tunneled jugular catheters, our experience, efficacy and complications
Iyad Abuward Abu-Sharkh*, Suleyka Puello Martinez, Luisa Janeiro Moas, Nisrine Arhda, Manuel Fidalgo Diaz, Anabertha del valle Narvaez Benitez, Rafael Alonso Valente and Candido Diaz Rodriguez
Cite this as
Abu-Sharkh IA, Martinez SP, Moas LJ, Arhda N, Diaz MF, et al. (2020) Tunneled femoral catheters and tunneled jugular catheters, our experience, efficacy and complications. Arch Clin Nephrol 6(1): 001-004. DOI: 10.17352/acn.000037Background: The replacement of the arterio-venous fistula with PTFE prostheses or central tunneled catheters is increasing due to the early exhaustion of autologous native accesses. The percentage of patients with tunneled catheters as vascular access for hemodialysis reaches between 15 to 25%, therefore, it is essential to improve the techniques used to avoid early and late complications, and to look for other possibilities due to early venous exhaustion. The use of tunneled femoral catheters is increasingly frequent due to the impossibility of using accesses of the superior venous axis. In this work we study and analyze the evolution and complications of tunneled catheters, both jugular and femoral, placed in the period from January 1, 2017 to May 30, 2018 in the Interventional Nephrology Unit, Nephrology Department of the Clinical Hospital of Santiago de Compostela. We also compared the evolution of femoral tunneled catheters with tunneled jugular catheters.
Results: Although the number of the sample is small, especially in the group of tunneled femoral catheters, and the results were not statistically significant, clinically it was seen that tunneled jugular and femoral catheters present similar results in the short-medium term. No significant differences were detected in both immediate and late complications between tunneled femoral catheters and tunneled jugular catheters, no differences were detected in catheter infections between the two groups.
Conclusion: Tunneled femoral catheters can be an effective and safe alternative in case of non-accessibility to the superior venous axis.
Introduction
Percutaneous vascular access can be used temporarily (temporary central venous catheters) or permanently (tunneled central venous catheters) [1].
Although percutaneous vascular access is considered inferior to native vascular access due to its shorter half-life and its more frequent complications, the use of percutaneous accesses has increased significantly in recent years. This is due to the fact that the renal patient has more cardiovascular complications, more morbidities and more advanced age, in addition to the waiting time until the AVF maturation which in some patients needs more time due to associated comorbidities such as diabetes mellitus, peripheral arteriopathy, smoking, obesity, advanced age and suboptimal vascular anatomy; even reaching the primary failure of the native access created. In addition to this the easy access to its placement and the immediacy of its use for hemodialysis, has allowed the abuse of its use as vascular access [2,3].
According to the published results of some studies, the use of central venous catheters has increased in many countries, with the percentage of patients dialyzing through tunneled catheters as high as 27.7% in Sweden, 35% in Belgium and 49.1% in Canada [3,4].
The ideal site for the placement of permanent catheters is the right jugular vein, but in some cases it is impossible to use due to the presence of some complication, both primary and secondary to other previous procedures, for example: right jugular vein thrombosis, stenosis of the jugular vein, malformations in the neck, vascular structural alterations or other anatomical structures of the neck.
Other vessels may be the target of percutaneous vascular access, such as the left jugular vein, the subclavian, femoral, iliac, or inferior cava vein.
The use of the subclavian vein for hemodialysis catheters is being set aside due to the high incidence of venous stenosis [4,5].
The use of the femoral, iliac or inferior vena cava is considered as a last resort before the exhaustion of other possibilities, always with a distal to proximal order relative to the heart. In the scientific literature, data have been provided that percutaneous accesses have a higher incidence of infections and dysfunctions, being higher in cases of percutaneous accesses of the inferior venous axis [5-9].
Procedures
All tunneled catheters were placed by interventional nephrologists. The catheter placement was performed under real-time ultrasound in the interventional nephrology unit.
We used 15.5F with lengths from 24cm to 28 cm for jugular catheters and 15.5 F TITAN HD with length of 55 cm for femoral catheters. The tip of the catheter was placed in the right atrium for jugular and femoral catheters. The skin exit site for tunneled femoral catheters was towards the side wall of the abdomen.
The administration of prophylactic antibiotic is usually with Cefazolin or in case of not being able to use it, with Vancomycin, single dose after intervention.
All catheters for hemodialysis are managed by nurses specialized in hemodialysis and with training in the management of vascular access.
Nursing care and catheter management is done completely sterile following hospital protocols that include both respiratory and contact isolation, and catheter locking is basically done with heparin except in case of infections, situation which requires locking in addition to heparin with antibiotics.
In the treatment protocol for dialysis patients’ infections, treatment is done on an outpatient basis without the need for hospitalization, except in cases of instability or severe infections.
Materials and methods
A descriptive, retrospective observational study was carried out in the nephrology department of the University Clinical Hospital of Santiago de Compostela. The study included 59 patients who underwent permanent vascular access in the Interventional Nephrology Unit between January 2017 and May 2018.
The data source was the patient’s medical history, from which the necessary data was collected anonymously. The variables studied were age, weight, sex, time in hemodialysis on the day of catheter placement, cause of CKD, antiplatelet intake after placement, anticoagulants intake after placement, type of catheter, side of catheter placement, placement date, date of first infection, type of first infection, germ causing the infection, total infections during the time of the study, catheter removal date, reason for removal, immediate complications and late complications.
A descriptive analysis of the analyzed variables was carried out using the frequency and percentage for the qualitative variables, and the mean, median, standard deviation and range for the quantitative one. For the comparison of qualitative variables, the Chi-square test was used. The analysis was performed with an IBM SPSS Statistics v20 statistical package.
Results
22 (37.3%) of the patients studied were women, and 37 (62.7%) men (Table 1).
The median age was 71 years and the median weight was 70 kg. The causes of end stage kidney disease are shown in the (Table 2), the most frequent being diabetic nephropathy (30.5%), followed by those of unknown cause 15.3% and Nephroangiosclerosis 10.2%.
The Mean time in HD was 17.95 months. The median time in HD was 8 month; This includes patients who initiate HD through the tunneled catheter without having other previous venous access.
In 48 patients (81.4%) the type of catheter used was through the jugular vein while 11 patients had a tunneled femoral catheter. The most used access side was the right (93.2%).
After the placement of the catheter, 7 of the 59 patients had anticoagulant treatment, while 26 patients had anti-platelet therapy, of which 3 were dual anti-platelet treatment. Two patients who had venous thrombosis, 1 was anti-coagulated and the other had no anticoagulant or anti-platelet treatment.
Catheter infection was observed in 16 patients (27.1%), 5 women (22.7%) and 11 men (29.7%), 9 tunnel infections, 6 sepsis and 1 combined case of tunelitis complicated with sepsis. There were 2 cases of infections in femoral catheters (18%) and 14 cases of jugular catheters (29%) during the follow-up period.
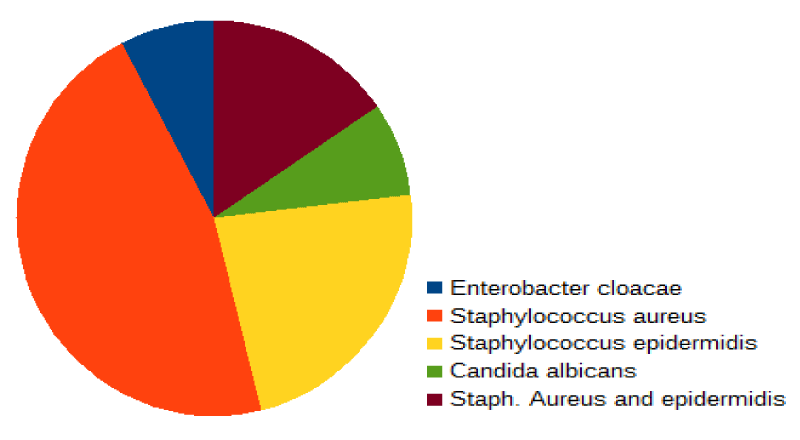
The most frequent type of infection was from the tunnel, confirmed in 7 patients (43.8%), and the most frequently isolated microorganism was Staphylococcus Aureus. The type of infection, isolated microorganism and time from placement to the first infection according to the type of catheter are shown in the corresponding Graph 1.
The mean time from insertion to the first infection was 138 days, interquartile range (205-101), and although in the case of femoral catheters the time is shorter, with a median of 32, it lacks statistical significance since the infections they have occurred in 2 femoral cases versus 14 jugular catheters.
Catheter removal occurred in 32 patients (54.2%), the mean time from insertion to removal was 244 days, interquartile range (363-118).
27 jugular catheters (56%) and 5 femoral (45%) have been removed during the study period.
The cause of removals in the jugular group was 10 of 27 (37%) due to AVF creation, 8 due to dysfunction (29.6%), 4 (14.8%) due to recovery of renal function, 4 (14.8%) due to death, 1 (3.7%) by transfer to PD.
On the other hand, in the femoral group 2 of the 5 (40%) it was due to AVF creation, 2 (40%) due to dysfunction and (10%) due to deep vein thrombosis.
Bleeding after implantation was considered an immediate complication and was observed in 3/59 patients (5.1%),1 in femoral group and 2 in jugular group, of whom 1 patient did not take any type of anti-platelet treatment, 1 was with acetylsalicylic acid and another patient was anticoagulated with low molecular weight heparin.
Only two patients had venous thrombosis (3.4%) of which one patient was anticoagulated with acenocoumarol and another was not receiving any antithrombotic treatment
Discussion
We start from the basis that patients who have had a femoral catheter are not having adequate access to the jugular axis, either due to exhaustion or complications, for this reason it is understood that the femoral catheter group would have more complications, comorbidities and less quality of the vascular system.
As can be seen in the results obtained, the percentage of male patients is higher than female patients, male patients formed 63% of the sample studied, while women 37%, on the other hand, the patients who required placement of the femoral catheter were more female (63,6%). In some studies, elderly patients have been associated with the increased possibility of AVF failure, although in other studies no differences have been detected between young patients and elderly patients. In our study, it was seen that the mean age is 71 years, and we consider that other factors have more influence on the determination of the type and the survival of vascular access. Approximately 30% of patients who acquire catheter implantation had diabetic nephropathy as a cause of chronic kidney disease.
In our study, anticoagulant or anti-platelet therapy intake was not relevant. No relationship has been found between anticoagulation / anti-platelet therapy and the incidence of early or late complications, the two complications related to the procedure detected were venous thrombosis and bleeding, with equal incidences in jugular catheters and femoral catheters.
There were no differences in the incidence of infections between men and women, (22.7%) in women and (29.7%) in men, nor was there a correlation with age since the distribution of infections was homogeneous at all ages.
Tunnelitis was the most frequent infection, observed of equal incidence in the two groups studied, both jugular and femoral, and although the mean time of onset of the first infection was shorter in the femoral group, it was not stylistically significant because of the low frequency number of infections.
In addition they were treated with antibiotherapy and did not require any catheter removal.
There have been 32 catheter removals of the 59 inserted catheters, and the most important reason was the creation of a native vascular access, with the same percentage in the two groups studied. While in the femoral group there was 1 removal because of deep femoral vein thrombosis, in the jugular group 8 catheters have been removed due to dysfunction compared to 2 in the femoral group.
Conclusion
Due to the advanced age of the patients and the associated pathologies especially cardiovascular pathology, the use of non-native vascular access is increasing, for this reason we must improve the techniques of vascular catheters placement in order to optimize its viability [7-9].
We consider that we must investigate further to find easy and safe alternatives to guarantee vascular access, in addition to individualizing the type of access for each patient.
The use of the femoral vein for the creation of percutaneous vascular access, allows to have good alternative in case of depletion of the superior venous axis, and although in the literature there has been repeated talk about the increased risk of infections and complications of this type of access [10], our retrospective study shows that there is no increased risk of infections or complications in relation to jugular catheters, and also shows no inferiority in efficacy and evolution. Even in patients with high risk to use the superior venous axis while waiting for the creation of autologous access, we could consider the use of the femoral axis until the creation of autologous vascular access.
- Raja RM (1996) El acceso vascular para la hemodialisis. En: Daugirdas JT, Ing TS, editors. Manual de Dialisis. Barcelona: Masson-Little Brown 51-74.
- Polo JR, Echenagusıa A (2006) Accesos vasculares para hemodialisis. En: Jofre R, Lopez-Gomez JM, Luno J, Perez-Garcia R, Rodrıguez-Benıtez P, editors. Tratado de Hemodialisis. 2.a ed. Barcelona: Editorial Medica Jims 213-241.
- Malovrh M (2011) How to increase the use of native arteriovenous fistulae for haemodialysis. Prilozi 32: 53-65. Link: http://bit.ly/2t0qkTb
- Hinsdale JG, Lipcouvirtz GS, Hoover EL (1985) Vascular access in the elderly: results and perspectives in a geriatric population. Dial Transplant 14: 560-562. Link: http://bit.ly/2t1ZtX1
- Miller LM, Clark E, Dipchand C, Hiremath S, Kappel J, et al. (2016) Hemodialysis Tunneled Catheter-Related Infections. Can J Kidney Health Dis 3: 2054358116669129. Link: http://bit.ly/36toFn0
- Miller LM, MacRae JM, Kiaii M, Clark E, Dipchand C, et al. (2016) Hemodialysis Tunneled Catheter Noninfectious Complications. Can J Kidney Health Dis 3: 2054358116669130. Link: http://bit.ly/2vhV9n5
- Molina Alfonso S, Orret Cruz D, Pérez Rodríguez A, Gutiérrez García F (2012) Supervivencia de las Fístulas Arteriovenosas en Pacientes en Hemodiálisis. Rev Cub Cir 51: 307-317. Link: http://bit.ly/2uzBY88
- Zhai S, Zhao Q, Feng Y, Yu Y, Zhou L, et al. (2017) Placement of tunneled cuffed vascular catheter through superior vena cava puncture. Journal of Vascular Surgery: Venous and Lymphatic Disorders 5: 547-552. Link: http://bit.ly/38Jadc4
- Wang L, Wei F, Sun G, Chen H, Yu H, et al. (2016) Use of iliac vein tunneled cuffed catheters in elderly hemodialysis patients: a single-center retrospective study. J Nephrol 29: 105-110. Link: http://bit.ly/2sZoQIP
- Maya ID, Allon M (2005) Outcomes of tunneled femoral hemodialysis catheters: Comparison with internal jugular vein catheters. Kidney International 68: 2886-2889. Link: http://bit.ly/2vra9PJ
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
