Archives of Community Medicine and Public Health
How can we presume a kid is having risk factors for cardiovascular disease?
Fernando Aguirre Palacios1* and Gregory Celis2
2Maria Fernanda Aguirre Cts, Princess University Hospital, Madrid
Cite this as
Palacios FA, Celis G (2022) How can we presume a kid is having risk factors for cardiovascular disease? Arch Community Med Public Health 8(4): 118-119. DOI: 10.17352/2455-5479.000186Copyright License
© 2022 Palacios FA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Digital health has come into reality, thanks to the new technologies such as Artificial Intelligence and Deep learning, contributing in a transcendental way to advances in the prevention, diagnosis, treatment and monitoring of diseases; In addition, this occurs at a crucial moment, marked by the growing prevalence of chronic diseases and the increase in life expectancy. In this context, digital health is not only necessary but, according to experts, it is the key to guaranteeing the present and future of quality healthcare.
So, human health, from now on, will be related to Primordial prevention, preventing risk factors from disease developing. Although the opportunity for societal benefit is the greatest if this “time zero” before disease develops is preserved, this would require population-based strategies and systems-wide collaboration, which are difficult to achieve [1].
Obesity is a pandemic that tends to perpetuate itself because of a sedentary lifestyle, in the digital age, more and more early in the life of humanity. Its inception occurs in childhood. As a result, this will modify the normal growing process of the body and mind, resulting in early aging, hardly detected, due to the lack of clinical evidence. Dyslipidemia and insulin resistance, increase blood pressure, leading to cardiovascular disease with all its diverse expressions up to coronary disease, heart failure and death [2-5].
So, the consequence of this derangement will turn into the appearance of metabolic syndrome in kids over 12 years old. The screening time should start in the child’s developmental maturity, to achieve stability of the analytical results, that is, after 12 to 15 years on average, or the Tanner V period. The menarche in females will be the light that announces the beginning of the change in the hormonal cycle [3,4]. Before that, the body has gone through its natural growth cycle, and the hormones interact in the metabolic profiles generating unstable results [6,7].
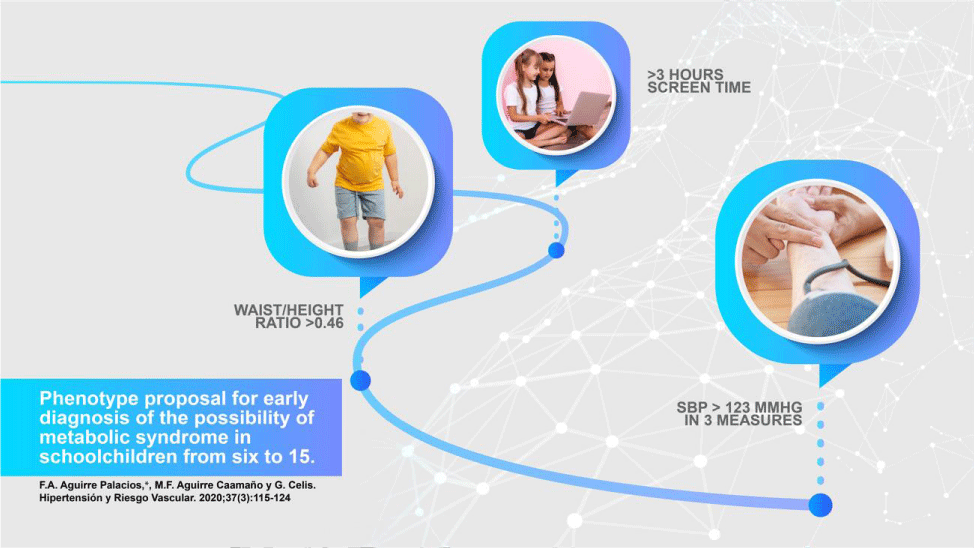
So, how can we presume at home, or in school, our Kids will develop such a disease? In a simple equation. Physical inactivity is the first feature. 3 hours of screening, is an arbitrary proposal, validated in our study. 2. With a cheap measuring tape, measure the Waist/height ratio, with a metric over 0,47. This ratio should be corrected in every population study; 3. Blood pressure measurement above the 90th percentile [8] (Figure 1).
Our study demonstrates the inflammatory process might have started in those kids with the 3-questions positive. The lipids test will be, < 45 mg HDL: or triglycerides > 100 mg/dl. In our study, CRP, and interleukin 6, were mathematically sensitive in the analysis of the ROC curve, as well as the values of baseline blood pressure above the 90th percentile in 3 consecutive measures9. 12.6% of our children tested positive for the Dx of metabolic syndrome in our sample, which is of great concern and encourages us to apply coordinated measures of lifestyle change in our city [10-12].
It is essential to replicate the present finding and validate it worldwide since a pattern of atherogenic dyslipidemia is very different from that we have seen in the North American population described in the PURE Study and is not the purpose of the present editorial.
The present proposal looks for a digital software that introduces this simple equation (Ecuador Index) to validate the present Phenotype of metabolic syndrome which is a precursor of Diabetes Mellitus [13].
- Vaduganathan M, Venkataramani AS, Bhatt DL. Moving Toward Global Primordial Prevention in Cardiovascular Disease: The Heart of the Matter. J Am Coll Cardiol. 2015 Oct 6;66(14):1535-1537. doi: 10.1016/j.jacc.2015.08.027. PMID: 26429076.
- Aguirre P F, Coca A, Aguirre MF, Celis G. Waist-to-height ratio and sedentary lifestyle as predictors of metabolic syndrome in children in Ecuador. Hipertens Riesgo Vasc. 2017 Nov 4:S1889-1837(17)30079-X. doi: 10.1016/j.hipert.2017.09.002. Epub ahead of print. PMID: 29108814.
- Koskinen J, Magnussen CG, Sabin MA, Kähönen M, Hutri-Kähönen N, Laitinen T, Taittonen L, Jokinen E, Lehtimäki T, Viikari JS, Raitakari OT, Juonala M. Youth overweight and metabolic disturbances in predicting carotid intima-media thickness, type 2 diabetes, and metabolic syndrome in adulthood: the Cardiovascular Risk in Young Finns study. Diabetes Care. 2014 Jul;37(7):1870-7. doi: 10.2337/dc14-0008. Epub 2014 Apr 17. PMID: 24742659.
- de Ferranti SD, Gauvreau K, Ludwig DS, Neufeld EJ, Newburger JW, Rifai N. Prevalence of the metabolic syndrome in American adolescents: findings from the Third National Health and Nutrition Examination Survey. Circulation. 2004 Oct 19;110(16):2494-7. doi: 10.1161/01.CIR.0000145117.40114.C7. Epub 2004 Oct 11. PMID: 15477412.
- Singh Y, Garg MK, Tandon N, Marwaha RK. A study of insulin resistance by HOMA-IR and its cut-off value to identify metabolic syndrome in urban Indian adolescents. J Clin Res Pediatr Endocrinol. 2013;5(4):245-51. doi: 10.4274/Jcrpe.1127. PMID: 24379034; PMCID: PMC3890224.
- Marshall WA, Tanner JM. Variations in pattern of pubertal changes in girls. Arch Dis Child. 1969 Jun;44(235):291-303. doi: 10.1136/adc.44.235.291. PMID: 5785179; PMCID: PMC2020314.
- Marshall WA, Tanner JM. Variations in the pattern of pubertal changes in boys. Arch Dis Child. 1970 Feb;45(239):13-23. doi: 10.1136/adc.45.239.13. PMID: 5440182; PMCID: PMC2020414.
- Ball GD, Weigensberg MJ, Cruz ML, Shaibi GQ, Kobaissi HA, Goran MI. Insulin sensitivity, insulin secretion and beta-cell function during puberty in overweight Hispanic children with a family history of type 2 diabetes. Int J Obes (Lond). 2005 Dec;29(12):1471-7. doi: 10.1038/sj.ijo.0803044. PMID: 16077712.
- HILL AB. THE ENVIRONMENT AND DISEASE: ASSOCIATION OR CAUSATION? Proc R Soc Med. 1965 May;58(5):295-300. PMID: 14283879; PMCID: PMC1898525.
- Brambilla P, Bedogni G, Heo M, Pietrobelli A. Waist circumference-to-height ratio predicts adiposity better than body mass index in children and adolescents. Int J Obes (Lond). 2013 Jul;37(7):943-6. doi: 10.1038/ijo.2013.32. Epub 2013 Mar 12. PMID: 23478429.
- Aguirre PF, Morales S A, MF Aguirre, Coca A, Gregory Celis Can a Simple Physical Questionnaire Detect Metabolic Syndrome? EC Cardiology. 2018; 5:28-30.
- Coleman KJ, Tiller CL, Sanchez J, Heath EM, Sy O, Milliken G, Dzewaltowski DA. Prevention of the epidemic increase in child risk of overweight in low-income schools: the El Paso coordinated approach to child health. Arch Pediatr Adolesc Med. 2005 Mar;159(3):217-24. doi: 10.1001/archpedi.159.3.217. PMID: 15753263.
- Aguirre Palacios FA, Aguirre Caamaño MF, Celis G. Propuesta de fenotipo para diagnóstico temprano de posibilidad de síndrome metabólico en escolares de seis a 15 años [Phenotype proposal for early diagnosis of possibility of metabolic syndrome in school children aged 6 to 15 years]. Hipertens Riesgo Vasc. 2020 Jul-Sep;37(3):115-124. Spanish. doi: 10.1016/j.hipert.2020.05.004. Epub 2020 Jun 10. PMID: 32534888.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
