Archives of Community Medicine and Public Health
Is non-alcoholic steatohepatitis caused by alcohol?
Hubert E Blum*
Cite this as
Blum HE (2020) Is non-alcoholic steatohepatitis caused by alcohol? Arch Community Med Public Health 6(1): 081-083. DOI: 10.17352/2455-5479.000083Epidemiology
Obesity and the associated diseases such as the metabolic syndrome, hypertryglyceridemia and diabetes mellitus type 2 are the most frequent causes of Non-Alcoholic Fatty Liver Diseases (NAFLD) [1-5]. Over time NAFLD may show mixed lobular inflammatory infiltrates and a ballooning degeneration around hepatocytes, termed Non-Alcoholic Steatohepatitis (NASH) with the potential to develop a liver cirrhosis or a Hepatocellular Carcinoma (HCC), frequently without a preexisting cirrhosis.
Pathogenesis
NAFLD and NASH are diffuse parenchymal liver diseases defined by clinical parameters (daily alcohol-intake < 20g) and histopathologic features of steatohepatitis. Diagnosis is based on the exclusion of other known causes of liver diseases that are associated with steatosis, e.g., Wilson’s disease, autoimmune liver disease, galactosemia and most important hepatitis C and Alcoholic Liver Disease (ALD). Central to the diagnosis of NASH are histopathologic findings that meet the criteria of ALD. NASH is the most severe form of a larger spectrum of NAFLD, characterized by fat plus ballooning degeneration or ALD-like lesions, including sinusoidal fibrosis, polymorphonuclear infiltrates with or without Mallory hyalin. The natural course of NASH ranges from a clinically asymptomatic presentation to liver cirrhosis and its complications, including HCC.
While the factors determining the natural course and progression to NASH are not well defined, the clinical conditions underlying NAFLD are increasingly clear: obesity, rapid and profound weight loss in obese individuals, including Jejunoileal Bypass (JIB) surgery, hyperlipidemia, total parenteral nutrition, drugs, industrial toxins, and disorders characterized by extreme insulin resistance. Most patients with NASH have a good prognosis and it is uncertain whether NASH affects life expectancy. Nevertheless, in many patients with liver cryptogenic liver fibrosis or cirrhosis NASH appears to be the underlying cause.
Excessive importation of free fatty acids (FFA) can result from either increased delivery of triglycerides to the liver (as seen with obesity and rapid weight loss), or from excessive conversion of carbohydrates and proteins to triglycerides (e.g., secondary to overfeeding or total parenteral nutrition).
Insulin resistance has a key role in the development of hepatic steatosis and, potentially, steatohepatitis. Obesity and type 2 diabetes, conditions associated with peripheral insulin resistance, are frequently observed in patients with (NAFLD).
Resistin and leptin are adipose tissue-derived proteins that may have an important physiological role in the development of insulin resistance. Overexpression of resistin in a mouse model led to glucose intolerance, hyperinsulinemia, and impaired suppression of FFA levels. Further, leptin deficiency is associated with massive overweight in mice and humans.
Can nash be caused by alcohol
As opposed to ALD, the definition of NAFLD and NASH generally allows the daily use of <20 g alcohol. This definition - particularly in alcohol-sensitive patients - ignores the contribution of even low amounts of alcohol to the pathogenesis of NAFLD/ NASH and at the same time in somewhat relaxed attitude towards the recommended <20 g daily alcohol restriction. In fact, the recommendation of alcohol restriction in patients of NAFLD/ NASH should be an absolute alcohol abstinence. This view is strongly supported by a recent publication demonstrating that the moderate alcohol use of 10-19 g/ day doubles the risk of advanced liver disease as compared to a daily alcohol use of 0-9 g [6]. Therefore, only alcohol abstinence would scientifically justify the term NAFLD/ NASH.
Recently, intestinal microbiota have been implicated as a potential source of hepatotoxic oxidative injury and changes in the microbiome have been shown to play a role in lipotoxicity and pathogenesis of NAFLD. Studies suggest that the specific composition of intestinal microbiota may play a role in both the inflammatory and fibrosis responses in patients with NAFLD [7]. Among 57 patients with biopsy-proven NAFLD, those with Bacteroides genus counts in the second and third tertile had a 2-fold increase in NASH compared with those with lower Bacteroides counts who were found to also have an abundance of Prevotella bacteria. With respect to fibrosis stage, those with Ruminococcus counts in the third tertile were found to have a 2-fold increase in stage 2 or greater fibrosis compared with those with lower levels of Ruminococcus. Specific gut microbiome signatures were linked to the severity of NAFLD and degree of fibrosis in additional studies [8,9]. A specific microbial metabolite, 3-(4-hydroxyphenyl) lactate, correlated significantly with hepatic fibrosis and specific bacterial species (Firmicutes, Bacteroidetes, and Proteobacteria) [8]. One proposed mechanism pertains to the endogenous production of alcohol and acetaldehyde. Colonic bacteria and yeast possess an enormous metabolic capacity for generating both ethanol and acetaldehyde, and can oxidize ethanol to high levels of acetaldehyde, even at low ethanol concentrations. Acetaldehyde is easily absorbed into the portal system,
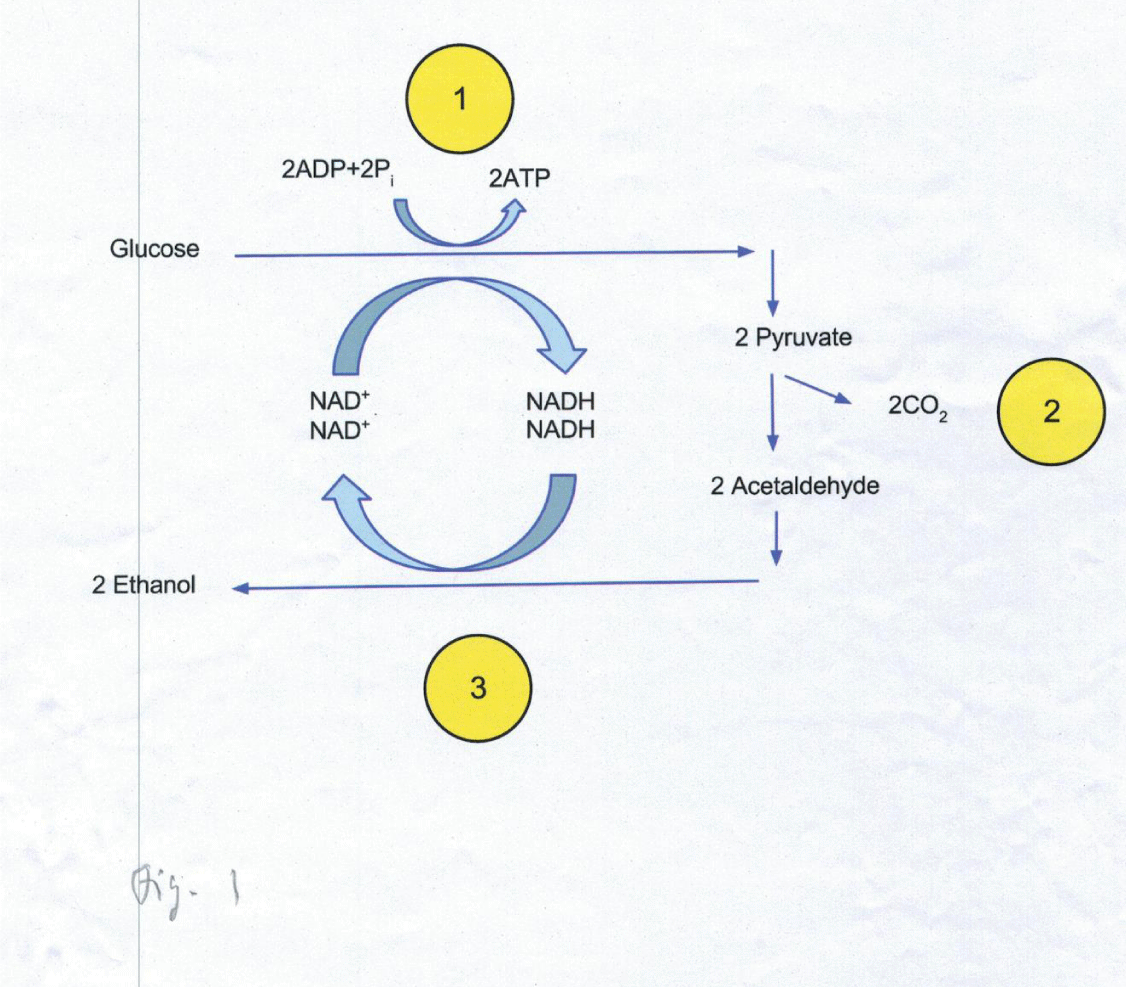
The most compelling evidence for a contribution of alcohol to NAFLD/ NASH has recently been provided by Yuan, et al. [10]. In an individual with a severe NASH the authors discovered an ultrahigh blood alcohol concentration (BAC) of about 400 mg/ L after the consumption of a high-carbohydrate, alcohol-free diet. Further analyses revealed the endogenous alcohol production by a Klebsiella pneumoniae (Kpn) strain through fermentation of glucose/ sucrose (glucose-fructose dimer). This clinical situation was termed‚ Autobrewing syndrome’ (ABB) caused by a high-alcohol (HiAlc) producing Kpn strain (Figure 1). The patient eventually recovered after dietary changes and antibiotic treatment.
The further investigation of a cohort of patients with NAFLD identified a strong association between disease severity and the existence HiAlc Kpn isolates. In a HiAlc-Kpn-induced mouse model of fatty liver disease (FLD) the authors demonstrated that HiAlc-Kpn might be an important cause for NAFLD via the induction of endogenous alcohol production. Finally, transplant of HiAlc-Kpn into mice was shown to cause NAFLD. Taken together, these data provide compelling evidence that HiAlc-Kpn exist in humans and can be associated with the development of NAFLD/ NASH (Figure 2).
Summary and recommendations
In NALFD/ NASH alcohol abstinence is to be recommended because the intake of even low daily amounts of acohol (< 20 g) can carry the risk of an advanced liver disease [6] while 10-19 g alcohol per day doubles the risk of advanved liver disease as compared to 0-9 g daily alcohol inake,
Recent data further suggest that the intestinal microbiome can play a major role inthe pathogenesis of NAFLD/ NASH through an excess endogenous alcohol production [10]. While the study demonstrates that HiAlc-Kpn is a primary causative agent of NAFLD it represents only one type of etiology among other mechanisms, presumably including further roles of the microbiota that need to be investigated (Geographical Abstract, 10).
Dedication
Dedicated to the 50th birthday of Prof. Dr. med. Robert Thimme. Medical Director, Clinic of Internal Medicine II, University Hospital Freiburg.
The excellent technical assistance of Mrs. Mariette Gutgsell is gratefully aknowledged.
- Rinella ME (2015) Nonalcoholic fatty liver disease: a systematic review. JAMA 313: 2263-2273. Link: https://bit.ly/3efRhUT
- Younossi ZM, Koenig AB, Abdelatif D, Fazel Y, Henry L, et al. (2016) Global epidemiology of nonalcoholic fatty liver disease-Meta-analytic assessment of prevalence, incidence, and outcomes. Hepatology 64: 73-84. Link:https://bit.ly/2XukBAe
- Younossi Z, Tacke F, Arrese M, Chander Sharma B, Mostafa I, et al. (2019) Global perspectives o nnonalcoholic fatty liver Disease and nonalcoholic steatohepatitis. Hepatology 69: 2672-2682. Link: https://bit.ly/2ZyHvt1
- Chalasani N, Younossi Z, Lavine JE, Charlton M, Cusi K, et al. (2018) The diagnosis and management of nonalcoholic fatty liver disease: Practice guidance from the American Association for the Study of Liver Diseases. Hepatology 67: 328-357. Link: https://bit.ly/3bXptmR
- Collaborators GBDD (2019) Health effects of dietary risks in 195 countries, 1990-2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet 393: 1958-1972. Link: https://bit.ly/2WZL2yH
- Aberg F, Puukka P, Salomaa V, Mannisto S, Lundqvist A, et al. (2020) Risks of light and moderate alcohol use in fatty liver idisease: follow-up of population cohorts. Hepatology 71: 835-848. Link: https://bit.ly/3d7p02U
- Boursier J, Mueller O, Barret M, Machado M, Fizanne L, et al. (2016) The severity of nonalcoholic fatty liver disease is associated with gut dysbiosis and shift in the metabolic function of the gut microbiota. Hepatology 63: 764-775. Link: https://bit.ly/3goUS58
- Caussy C, Hsu C, Lo MT, Liu A, Bettencourt R, et al. (2018) Link between gut-microbiome derived metabolite and shared gene-effects with hepatic steatosis and fibrosis in NAFLD. Hepatology 68: 918-932. Link:https://bit.ly/2Xmt8VW
- Loomba R, Seguritan V, Li W, Long T, Klitgord N, et al. (2017) Gut microbiome-based metagenomic signature for non-invasive detection of advanced fibrosis in human nonalcoholic fatty liver Disease. Cell Metab 25: 1054-1062. e5. Link: https://bit.ly/3bZSUoh
- Yuan J, Chen C, Cui J, Lu J, Yan C, et al. (2019) Fatty Liiver disease caused by high-alcohol-producing Klebsiella pneumoniae. Cell Metab 30: 675-688 e677. Link: https://bit.ly/2ZBtElE
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
