Archives of Community Medicine and Public Health
Association between persistent high costs and chronic physical, mental and disability-related health conditions among community-dwelling Medicare-Medicaid dually eligible enrollees
Lirong Zhao1* Karyn Kai Anderson2 and Gerald Riley1
2Social Science Research Analyst, Medicare-Medicaid Coordination Office, Centers for Medicare & Medicaid Services,7500 Security Blvd, Baltimore, MD 21244, USA
Gerald Riley was with CMS Research and Evaluation Group at the time the study was conducted.
Cite this as
Zhao L, Anderson KK, Riley G (2018) Association between persistent high costs and chronic physical, mental and disability-related health conditions among community-dwelling Medicare-Medicaid dually eligible enrollees. Arch Community Med Public Health 4(2): 080-087. DOI: 10.17352/2455-5479.000043Background: The 11.4 million Americans who receive both Medicare and Medicaid benefits constitute one of the nation’s most vulnerable and costly populations.
Objectives: We examine the relationship between persistently high costs (PHC) and physical, mental, and disability-related conditions among community-dwelling dully eligible enrollees.
Research Design: Retrospective longitudinal study.
Subjects: Community-dwelling beneficiaries who were continuously enrolled in Medicare and Medicaid fee-for-service 2007 through 2009.
Measures: Beneficiaries in the top 10% of spending in all three study years were defined as having PHC. Chronic conditions were identified via CMS Chronic Condition Warehouse pre-defined variables.
Results: Medicare and Medicaid collectively paid $77.7 billion for 1.46 million beneficiaries in the study from 2007 through 2009. Of these total expenditures, 39.3% were attributable to the 6.9% of dually eligible enrollees who were PHC. Medicaid accounted for 44.5% of total spending. Of the total Medicaid spending on dual enrollees, 67.9% was incurred by those individuals identified as PHC. An overwhelming 83.8% of PHC dually eligible enrollees were younger than 65 years. Beneficiaries with at least one disability-related condition were more likely to be PHC. In particular, beneficiaries with “intellectual disabilities and related conditions” were found to be 17 times more likely to be PHC compared to those without this condition, though this cost may be attributable to other concomitant health issues.
Conclusion: Individuals with certain chronic conditions, especially disability-related conditions, tend to have persistently high costs over time. They may be particularly suitable candidates for interventions or payment models that promote more coordinated and efficient care. (250/250).
Introduction
Individuals who are simultaneously enrolled in Medicare and Medicaid (also called “dual enrollees” or “dually eligible beneficiaries”) are known to have significantly greater morbidity, comorbidity, and health care needs than those qualifying for Medicare or Medicaid alone. Not surprisingly, this group also accounts for a disproportionate share of Medicare and Medicaid expenditures [1].
Forty-one percent of Medicare-Medicaid dual enrollees have at least one mental health diagnosis, while 60 percent have three or more chronic conditions. The 27 percent of Medicare-Medicaid enrollees who receive institutional long term services and supports (LTSS) services accounted for 52 percent of total Medicare-Medicaid enrollee expenditures in 2011 [2]. More than $294 billion was paid for this group in Medicare and Medicaid health care benefits in the same year [3].
Medicare and Medicaid are the two major public health programs that pay for dually eligible beneficiaries’ health care services. In general, Medicare is responsible as primary payer and pays for most acute care services, such as inpatient care, outpatient, physician, skilled nursing facility services, home health care, prescription drugs, durable medical equipment, and hospice. Medicaid covers long term care services and serves as a supplement to Medicare coverage through the Medicare Savings Program. Dual enrollees are often classified as being “full benefit” in that they are eligible to receive full Medicaid services (including nursing home benefits) or “partial benefit” in that Medicaid only provides assistance with their Medicare cost-sharing obligations.
Because of the differing mechanisms of the two programs’ operations, one challenge is the coordination of funding streams such that beneficiaries’ health care needs are satisfied while also controlling costs. Medicare Advantage special needs plans (SNPs) and the Program of All-Inclusive Care for the Elderly (PACE) are two approaches that have been used to reach these goals [4]. More recently, CMS initiatives, such as the Financial Alignment Medicare-Medicaid Plan (MMP) demonstrations, also aim to achieve the goal of improving quality of care and lowering costs for individuals who are dually enrolled in Medicare and Medicaid through efforts to partner with states [5]. Identifying the characteristics of those dually eligible individuals who have the highest costs can help in crafting more focused and effective responses to the challenges facing this population.
Dually enrolled beneficiaries tend to have multiple non-life threatening chronic conditions that may produce persistently high health care expenditures over time. The range of acute and long term care services required to manage their conditions in a community setting requires complex navigation and care coordination among different services and providers. If health care services can be provided in a more effective and efficient way it may be possible to prevent or delay costly institutionalization which could have a profound impact on improving health while reducing health care expenditures. In this paper, we analyze the characteristics of the community dwelling Medicare-Medicaid dual enrollee population to better understand which mental health, physical health, and disability-related conditions are most strongly associated with persistently high costs (PHC). According to a study in 2012, dually eligible beneficiaries residing in the community constitute a vulnerable population that may benefit from policy reforms and improved care coordination [1].
Among dual beneficiaries not enrolled in managed care, including both community- and institution-dwelling beneficiaries, prior research has found that 60 percent had at least three physical or mental health conditions. Forty-one percent had at least one mental health condition, with a 25 percent prevalence of depression and 12 percent prevalence of schizophrenia or another psychotic disorder [6]. Dually eligible enrollees who live in community environments need services including prescription drugs, psychiatric specialty care, rehabilitation, case management, housing, and employment [7].
Very few studies have focused on the community-dwelling dually eligible population to explore the relationship between persistently high costs and multiple chronic conditions, with an emphasis on mental health and disability-related conditions. Most previous studies employed short-term cross-sectional study designs, usually limited to one year [1]. Potential approaches to care coordination and cost control for persistently high costs dually enrolled beneficiaries are likely to be different for the community-dwelling population than for those who are institutionalized. Our study fills this gap by identifying the most vulnerable high-cost subgroup of community dwelling dually eligible beneficiaries over three years.
Methods
DATA: Two sets of data sources were used in the study. The Medicare-Medicaid Linked Enrollee Analytic Data Source (MMLEADS) is a suite of analytic research files for Medicare-Medicaid dual enrollees. This data source can be used to address research questions regarding beneficiaries’ eligibility, enrollment, health care utilization and cost, and chronic physical and mental health conditions as well as intellectual, developmental, and physical types of potentially disabling conditions [8]. We used MMLEADS to identify the study sample and measure study outcomes. The CMS Timeline files are a set of summary files with long-term care stay counts for Medicare beneficiaries. These Timeline files were used as supplemental criteria to exclude institutional stay beneficiaries.
SAMPLE SELECTION: Enrollment in Medicaid is not always continuous across years. Loss of Medicaid coverage could not only reduce access to medical services and increase out-of-pocket costs but it could also result in incomplete information on health services utilization and expenditures in program administrative information systems [9]. As an additional issue, both Medicare and Medicaid administrative data do not necessarily provide complete and accurate encounter data from managed care plans. Due to these challenges, we limited the sample to dual beneficiaries who were continuously enrolled in both Medicare and Medicaid fee-for-service from January 2007 to December 2009. Because we were interested in identifying beneficiaries who had persistently high costs throughout the three years of the analysis, we excluded from analysis those who died during the study period [10,11].
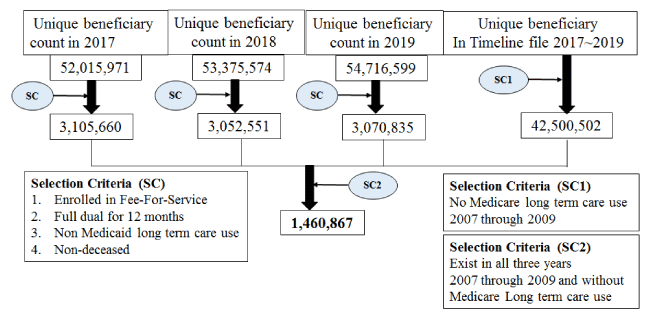
Finally, given that more than 27 percent of the full benefit dual population reside in an institutional long term care facility, accounting for 52 percent of full benefit expenditures [2], we excluded beneficiaries using long term care services, nursing home facilities, and other types institutional care services. Beneficiaries with short-term acute inpatient services use are still considered as community-dwelling and were not excluded from the study sample. Refer to chart 1 for a flowchart for final sample selection.
MEASURES: Total annual payment was calculated by aggregating Medicare and Medicaid fee-for-service expenditures. A beneficiary was defined as “high-cost” if his/her total annual cost was within the top ten percent of our sample. If a beneficiary was a high-cost individual for all three years from 2007 through 2009, he/she was defined as having “persistent high-cost” (PHC).
Chronic conditions were measured from existing variables within the Chronic Condition Warehouse (CCW) that had originally been developed from algorithms applied to Medicare and Medicaid claims’ ICD-9 and ICD-10 codes [12,13]. These conditions were classified into three categories. The first category comprised mental health conditions; the second category included intellectual, developmental and physical disability-related conditions; and the third category pertained to chronic physical health conditions. Table 1 for a full list of fifty-nine studied chronic conditions across these three groups. We created three summary dichotomous variables for each of the three sub-class condition groups from 2007 through 2009. The fifty-nine specific conditions were all studied as distinct dichotomous variables as well.
ANALYSIS: We first examined beneficiaries’ demographic characteristics and dual eligibility status. We then calculated the total annual Medicare and Medicaid combined costs. This measurement was used to create persistent high-cost indicators for each beneficiary. We compared the difference in frequency distributions between the persistent high-cost (PHC) group and the non-PHC group for each condition. To examine the cost by health services type and identify the most costly services, we calculated the costs by services type.
Medicare and Medicaid programs report service use differently in the administrative claims. MMLEADS data adapted service types that are classified according to a hierarchical information method from its source data. To calculate the breakdown percentage of total Medicare spending, we used four primary types of Medicare service: 1) institutional services (hospital inpatient, post-acute care, skilled nursing facility, hospice, and home health services); 2) hospital outpatient (outpatient, ESRD facility, outpatient clinic, outpatient therapy, and community mental health center); 3) non-hospital outpatient (carrier and durable medical equipment); and 4) prescription drugs.
Thirty-nine types of service in the Medicaid Analytic eXtract (MAX) research database were used in the development of MMLEADS’ three hierarchical types of service categories. Because the study sample is community dwelling FFS beneficiaries, we analyzed the program payments using only the following three specific Medicaid services types in MMLEADS: 1) acute care (hospitalization, outpatient hospital services, physician or other practitioner treatment services, laboratory tests or imaging services); 2) non-acute care (non-institution-based, including rehabilitative services, home health services, personal care services, and durable medical equipment and supplies); and 3) prescription drugs. These service types were used to calculate payment percentage distribution for total Medicaid cost.
We used three different multivariate logistic regression models to examine the association between PHC and chronic physical, mental, and potentially disabling health conditions, adjusting for demographic factors. Model #1 includes individual condition indicators to calculate the odds ratio of being PHC in the presence of each condition; Model #2 includes three condition-summary dichotomous flags for having: 1) at least one mental health condition, 2) at least one disability-related condition, and 3) at least one physical health condition; Model #3 is same as Model #2 with exclusion of the two conditions with highest adjusted odds ratios from Model #1, intellectual disabilities and HIV/AIDS, in order to determine the extent to which these conditions were driving the results of Model #2. Both Models #2 and #3 were run with three interaction terms: mental health and potentially disabling conditions; mental health and physical health conditions; and potentially disabling conditions with physical health conditions.
Results
Nationally, from 2007 through 2009, 1,460,867 community-dwelling beneficiaries were enrolled in both fee-for-service Medicare and Medicaid programs continuously. Among this group, 6.94 percent (101,432) were individuals with PHC whose total program payments were among the top 10 percent for each calendar year. Within the entire sample, more than half (54.7 percent) of beneficiaries were under sixty-five years of age, and the percentage was much higher among the PHC group versus the non-PHC group (83.8 percent versus 52.6 percent). Those who were male (53.1 percent in PHC group versus 39.3 percent in non-PHC group) and Non-Hispanic White (73.0 percent versus 58.6 percent) were more likely to be a persistent high-cost beneficiary. While the majority of this Medicare-Medicaid dual enrollee sample was entitled to full Medicaid benefits (74.9 percent) as opposed to assistance with Medicare cost-sharing only (i.e., “partial benefits”), this was particularly pronounced in the PHC group at 98.1 percent. (Table 2).
From 2007 through 2009, $77.7 billion in Medicare and Medicaid expenditures were paid on this sample of community dwelling, fee-for-service, dually enrolled, non-deceased beneficiaries. Of this total, $43.1 billion (55.5%) were Medicare program payments and $34.6 billion (45.5 %) were Medicaid program payments. In total, $30.5 billion (39.3%) of total Medicare and Medicaid payments went to PHC beneficiaries. Among the 6.94 percent of beneficiaries with PHC, 77 percent of expenditures were paid by Medicaid and 23 percent were paid by Medicare. Additionally, 67.9 percent of total Medicaid costs were paid on behalf of the PHC group, while 16.2 percent of the total Medicare costs were expended on the PHC group. (Table 2).
Among all dually eligible beneficiaries in the sample, nearly half of Medicare payments were expended on prescription drugs (48.0%), with institutional outpatient services costs being the second highest category in payments (22.5%). The distribution was similar for both the PHC and the non-PHC groups (Figure 1).
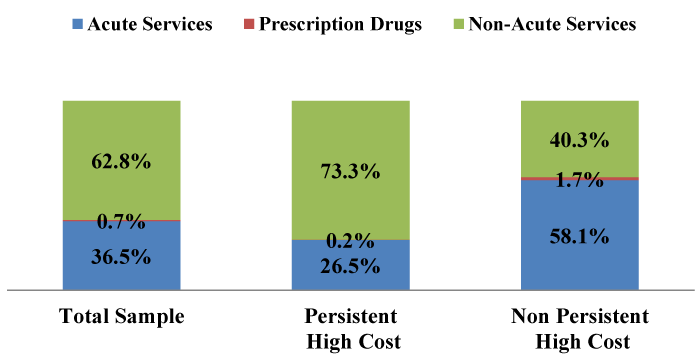
Medicaid expenditures for beneficiaries with persistent high costs showed a high percentage (73.3%) going to non-acute care, primarily consisting of rehabilitative services, home health services, and DME. In contrast, only 40.3% of Medicaid expenditures among non-PHC beneficiaries went to such services. Because dually eligible beneficiaries receive the vast majority of their prescription drugs under Medicare Part D, it is not surprising that Medicaid only paid a small proportion of the total prescription drug expenditures (0.7% for the full sample, and only 0.2% for the persistent high-cost group) (Figure 2).
Among the total sample of dually enrolled beneficiaries, 94.1 percent had at least one of the 59 studied chronic conditions in at least one of the three years. On average, 5.8 chronic conditions were found for all beneficiaries; the persistent high-cost group had higher average condition counts than non-PHC beneficiaries (7.5 versus 5.6). The prevalence of mental health and disability related conditions differed significantly between the PHC and the non-PHC group. For example, in the PHC group, 78.7 percent of beneficiaries had at least one of the 15 studied disability related conditions, while in the non-PHC group, only 17.8 percent had the same (Table 1).
The results from the multivariate logistic regressions revealed that certain chronic conditions were observed to be strongly associated with the persistent high-cost status of beneficiaries. For instance, intellectual disabilities and related conditions exhibited the strongest association with PHC status (Adjusted Odds Ratio=16.94), adjusting for all other conditions and demographic variables. HIV/AIDS, with an AOR of 3.63, demonstrated the second strongest association. Other conditions with AORs over 2.00 include: ADHD and other conduct disorders, autism spectrum disorder, cerebral palsy, learning disabilities and other developmental delays, mobility impairments, multiple sclerosis and transverse myelitis, muscular dystrophy, deafness and hearing impairment, blindness and visual impairment, spinal cord injury, traumatic brain injury and nonpsychotic mental disorders due to brain damage, other developmental delays, and chronic kidney disease. Some mental and physical chronic conditions were negatively associated with PHC status, such as tobacco and alcohol use disorders, hypertension, migraine and other chronic headache.
When the conditions were summarized by group (mental health, disability-related, and physical health), as three separate dichotomous variables in the same model (Model #2), we found that those with at least one of the disability-related conditions were 11.37 times more likely to be a beneficiary with PHC as compared to those without a disability-related condition. Having one or more mental health condition increased the likelihood of PHC by 1.50 times, while possessing one or more of the studied physical chronic health conditions was only weakly associated with being a PHC (AOR=1.14).
Finally, we reran Model #2 with removal of two conditions with the highest adjusted odds ratios, intellectual disability and HIV/AIDS, in order to ascertain the extent to which these two conditions were independently driving the results. This new Model #3 resulted in a significantly reduced, albeit still notably high, AOR for disability-related conditions (AOR=3.02). Similarly, the AOR for the mental health condition group was slightly reduced (AOR=1.22). For the physical chronic health group, however, the association with PHC was slightly elevated in this new model (AOR=1.31) (Table 3).
Discussion
Prior to the development of MMLEADS, few single data resources were available to researchers and policymakers to make data-driven, cost-saving policy recommendations about dually enrolled beneficiaries on a national scale [14]. However, some studies have found a clear relationship between high program payments and mental health and disability-related conditions, especially among dually enrolled beneficiaries younger than age 65 [15-17]. The results provided in this study expand upon these findings by examining a broad range of chronic conditions associated with persistently high costs among a nationwide sample of community-dwelling Medicare-Medicaid dually enrollees.
While 55 percent of community-dwelling dual beneficiaries in our study cohort were younger than 65 years old, the percentage under 65 in the PHC group (84 percent) was disproportionately higher than the non-PHC group (53 percent). This is consistent with other studies that suggest that younger dually eligible beneficiaries possessing mental health and disability-related conditions are in need of greater levels of attentive care and financial support [15].
Different health services may require different strategies for improving care and optimizing care coordination. Our results indicate minor differences in the proportions of Medicare prescription drug payment, institutional services, and institutional and non-institutional outpatient services between community-dwelling dually eligible enrollees with and without persistent high costs. However we found that under Medicaid, non-acute services (i.e., rehabilitative services, home health services, personal care services, and durable medical equipment and supplies) accounted for 73.3 percent of expenditures for PHC dually eligible beneficiaries, while these services accounted for only 40.3 percent of expenditures for non-PHC dually eligible beneficiaries. Efforts to reduce persistent high-costs might start with these non-acute care services, most of which are paid for by Medicaid. Better coordination of these services, with acute care services covered by Medicare, may produce a strategy for reducing persistently high costs. Cost reduction programs, such as case management with coordinated medical, mental health, substance abuse treatment, and psychological rehabilitation services, could focus on this population.
The Medicare Modernization Act of 2003 (MMA) expanded the health plan options available through the MA program by authorizing Special Needs Plans (SNPs) to better coordinate benefits for beneficiary populations with special needs (i.e., dually eligible individuals, institutional enrollees, or beneficiaries with certain chronic conditions). More recently, through the Financial Alignment Initiative, ten states began testing an integrated delivery-payment model to improve coordination of care and align financial incentives for dually eligible individuals. In this model, available only to full-benefit dually eligible individuals, participating health plans known as Medicare-Medicaid Plans (MMPs) enter into a three-way contract with the state and CMS, to receive a prospective blended payment and provide integrated services [5].
The ongoing CMS Medicaid Innovation Accelerator Program (IAP) aims to improve the health and health care of Medicaid beneficiaries and to reduce costs by supporting states’ ongoing payment and delivery system reforms. One of the key program areas is to improve care for Medicaid beneficiaries with complex care needs and high costs and support physical and mental/behavioral health integrations. The successful implementation of IAP may provide an effective additional guidance for persistent high cost Medicare-Medicaid dually enrollees [18].
Among community dwelling Medicare-Medicaid enrolled beneficiaries, the presence of a disability-related condition is a primary factor that was associated with persistently high health expenditures. Since a large proportion of beneficiaries with PHC are relatively young (under 65), innovative management of psychiatric services payment models that focus on disability and mental health related conditions may have the potential to achieve significant cost savings. It is possible that such coordinated management would also improve the quality of care and outcomes for this population [4].
Our study has some limitations worth mentioning. First, due to state variations in service delivery and administrative data collection, the study findings may not apply consistently for all states. In addition, disability-related conditions and mental health conditions can be underestimated when using administrative data sources alone [12]. These conditions can be under-diagnosed and under-reported due to stigma and the simple fact that beneficiaries cannot be identified as having a particular condition unless he/she has a medical bill processed through the Medicare or Medicaid data system with the relevant ICD code included on the claim. This means that there is the possibility of selection bias if those with identifying ICD codes have greater medical needs and therefore may be more expensive than individuals with intellectual disability who may be higher functioning and/or have fewer medical needs. Finally, as with chronic condition count measures, the results of the three chronic condition groups, included in this study, were a function of which conditions were included in each group. While our intent was to be as thorough as possible, it is possible that we neglected to include a given chronic health condition in its appropriate group. For example, the variable “Alzheimer’s disease and related dementia” was included in the physical health condition group. However, one could also argue that Alzheimer’s and dementia are either mental health conditions or even disability-related conditions. Therefore, the results of this study may have differed if these conditions were to have been included in either of these other groups rather than the physical health condition group.
Our study has generated some additional potential study topics to explore. As seen in figure 1, Medicare prescription drugs accounted for a large proportion of total expenditures across all services. Because MMLEADS data has more granular information on drug class, further studies can be conducted to differentiate the payment amount by medication categories to identify the most costly drug classes as targeted areas for program payment reform (e.g., prescribing generic medications, reducing excessive prescribing of opioid medications, prescribing less-costly preventative medications to avoid more costly downstream adverse health care events and associated costs).
In conclusion, innovative payment model reform efforts involving dually eligible beneficiaries may find it particularly effective to devote attention to certain subpopulations within the different categories of potentially disabling conditions. More specifically, care coordination interventions that focus on those high-PHC associated conditions, such as intellectual disability, HIV/AIDS, autism, mobility impairments, multiple sclerosis and transverse myelitis, have the potential to improve beneficiaries’ health and quality-of-life as well as the efficiency and effectiveness of spending by program payers over time.
Authors sincerely acknowledge Dr. David Bott, Dr. Sophia Chan, and Dr. Gregory Boyer for their inputs on research analysis and paper development. Authors also sincerely acknowledge Mr. William Clark and Mrs. Renee Mentnech in the initial and final completion of the paper development.
Authors’ contributions and approval
Mrs. Lirong Zhao is a quantitative Social Science Research Analyst working in Research and Evaluation Group of Centers for Medicare & Medicaid Services. Mrs. Zhao contributed in the study conception and design, data analysis and interpretations, drafted and collectively finalized the manuscript. Mrs. Zhao has final approval of the article version to be published.
Dr. Anderson is a senior Social Science Research Analyst working in Medicare-Medicaid Coordination Office of Centers for Medicare & Medicaid Services. Dr. Anderson contributed to the study design, interpretations of data and statistical analysis results, revised critically for important intellectual content. Dr. Anderson has final approval of the article version to be published.
Mr. Riley is a senior health services researcher working in this study before he retired from Research and Evaluation Group of Centers for Medicare & Medicaid Services. Mr. Riley contributed to the study conception and design, revised the draft for important intellectual content. Mr. Riley has final approval of the article version to be published.
Conflicts of interests
The authors have no conflicts of interests to disclose.
- Coughlin TA, Waidmann TA, Phadera L (2012) Among Dual Eligibles, Identifying the highest-Cost Individuals Could Help in Crafting More Targeted And Effective Responses. Health Affairs 31: 1083-1091. Link: https://goo.gl/dDQ1X7
- Dual-Eligible Beneficiaries of Medicare and Medicaid: Characteristics, Health Care Spending, and Evolving Policies (2013) Congressional Budget Office. Link: Available at: https://goo.gl/ZtGtvQ
- Medicare-Medicaid Enrollee Information National, 2011. Centers for Medicare & Medicaid Services. Link: Available at: https://goo.gl/ffsd11
- Report to Congress: Medicare and the health care delivery system Chapter 5: (2011) Coordinating Care for Dual-Eligible beneficiaries. Medicare Payment Advisory Committee. Link: https://67.59.137.244/chapters/Jun11Ch05.pdf
- Financial Alignment Initiative (2017) Centers for Medicare and Medicaid Services. Link: https://goo.gl/23VGL5
- Physical and Mental Health Condition Prevalence and Comorbidity among Fee-for-Service Medicare-Medicaid Enrollees (2014) Centers for Medicare & Medicaid Services. Link: https://goo.gl/DLPRJs
- Mental Health: A Report of the Surgeon General, U.S. (1999) Department of Health and Human Services Substance Abuse and Mental Health Services Administration and National Institutes of Health. Link: https://goo.gl/vcsr4m
- Introducing a New Linked Medicare and Medicaid Database from the Federal Coordinated Health Care Office (FCHCO). Centers for Medicare & Medicaid Services, 2013. Link: https://goo.gl/AE97TC
- Riley G, Zhao L, Tilahun N (2014) Understanding Factors Associated With Loss Of Medicaid Coverage Among Dual Eligibles Can Help Identify Vulnerable Enrollees. Health Affairs 33: 147-152. Link: https://goo.gl/YtsenM
- Hogan C, Lunney J, Gabel J (2001) Medicare Beneficiaries’ Costs Of Care In The Last Year Of Life. Health Affairs 20: 188-195. Link: https://goo.gl/8DdqBL
- Zainulbhai S, Goldberg L, Ng W (2014) Assessing Care Integration for Dual-Eligible Beneficiaries: A Review of Quality Measures Chosen by States in the Financial Alignment Initiative. The Commonwealth Fund. Link: https://goo.gl/8DdqBL
- Gorina Y, Kramarow KE (2011) Identifying chronic conditions in Medicare claims data: evaluating the Chronic Condition Data Warehouse algorithm. Health Services Research 46:1610-1627. Link: https://goo.gl/vjwZu9
- Chronic Conditions Data Warehouse: Your source for national CMS Medicare and Medicaid research data: Condition Categories. 2015. Centers for Medicare & Medicaid Services Chronic Condition Warehouse. Link: Available at: https://goo.gl/w1GFp4
- Gold MR, Jacobson GA, Garfield RL (2012) There Is Little Experience And Limited Data To Support Policy Making On Integrated Care For Dual Eligibles. Health Affairs 31: 1176-1185. Link: https://goo.gl/ZuM9AX
- Frank RG, Epstein AM (2014) Factors Associated With High Levels Of Spending For Younger Dually Eligible Beneficiaries With Mental Disorders. Health Affairs 33: 1006-1013. Link: https://goo.gl/dLWV8v
- Foote SM, Hogan C (2001) Disability Profile And Health Care Costs Of Medicare Beneficiaries Under Age Sixty-Five. Health Affairs 20: 242-253. Link: https://goo.gl/mtn1Z4
- Oliveira C, Cheng J, Vigod S (2016) Patients With High Mental Health Costs Incur Over 30 Percent More Costs Than Other High-Cost Patients. Health Affairs 35: 36-43. Link: https://goo.gl/DhKXvF
- Medicaid Innovation Accelerator Program (2018) CMS Centers for Medicare & Medicaid Innovation. Link: https://goo.gl/aJTfRX
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
