Archives of Clinical Gastroenterology
Dieulafoy’s Lesion Associated with Megaesophagus
Valdemir José Alegre Salles1,2*, Rafael Borges Resende3, Gustavo Seiji3, and Rodrigo Correia Coaglio2,4
2General Surgeon at the Regional Hospital of Paraíba Valley, Taubaté, Brazil
3Endoscopist Physician at the Regional Hospital of Paraíba Valley, Taubaté, Brazil
4Assistant Profesor, Department of Medicine, University of Taubaté, Brazil
Cite this as
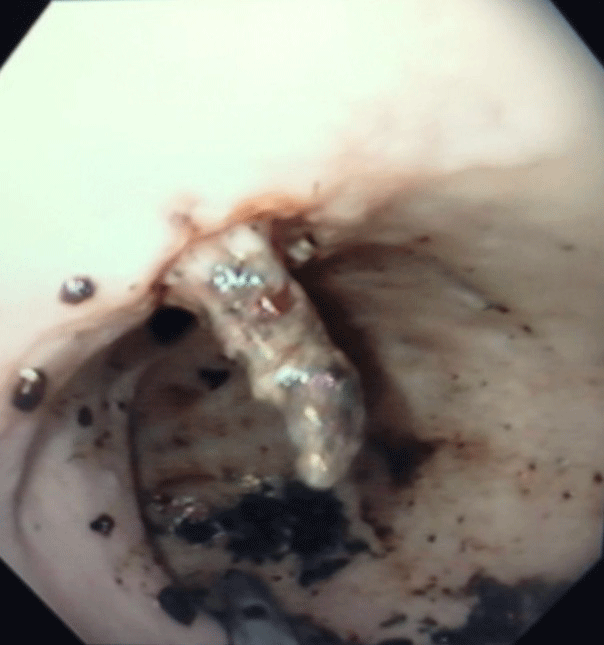
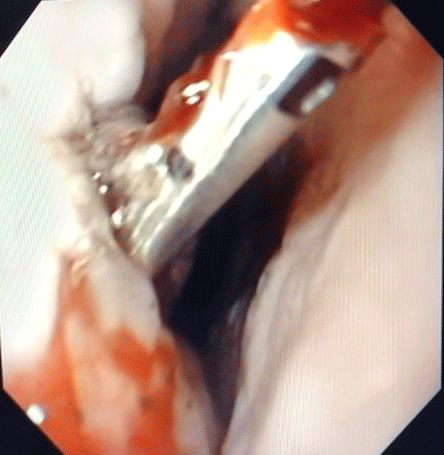
Alegre Salles VJ, Resende RB, Seiji G, Coaglio RC (2020) Dieulafoy’s Lesion Associated with Megaesophagus. Arch Clin Gastroenterol 6(3): 067-068. DOI: 10.17352/2455-2283.000083A 31-years-old male patient, with no previous symptoms, admitted to the ER with massive hematemesis that started about 2 hours ago and already with hemodynamic repercussions. After initial care with clinical management for compensation, and airway protection (intubation) he underwent esophagogastroduodenoscopy (EGD), which was absolutely inconclusive due to the large amount of solid food remains and clots already in the proximal esophagus with increased esophageal gauge. After a 24 hours fasting, and 3 inconclusive EGD, since we don’t have the availability of an overtube, we decided to use a calibrated esophageal probe (Levine 22) and to maintain lavage and aspiration of the contents, until the probe returned clear. In this period, the patient presented several episodes of hematimetric decrease and melena, maintaining hemodynamic stability with intensive clinical support. Only after 04 days, it was possible to perform a new EGD that showed diffusely increased esophageal gauge, tortuous in distal third and still with food stasis and blood remains that could be aspirated. On the middle esophagus was found a calf vascular stump with attached clot and fibrin (Figure 1). Endoscopic clipping and sclerotherapy (5 cc of ethamolin and hypertonic glucose solution) were then successfully performed, without further episodes of bleeding (Figure 2).
There are few cases in the literature reporting esophageal Dieulafoy`s lesions, since it`s rare incidence, being more frequently found in the stomach, especially in the small curvature of the gastric body [1]. The megaesophagus has as main symptomatology dysphagia, depending on its degree of involvement, may also be associated with vomiting, regurgitation and pneumonia due to reflux. Esophageal bleeding due to megaesophagus is also extremely rare, and when present, usually comes from a food stasis ulcer [2]. It is known that the frequency of upper gastrointestinal bleeding caused by Dieulafoy`s lesion is about 1.5% of the cases, being of gastric origin almost in its entirety [3]. These lesions have their origin in the anomalous formation of a vessel in the submucosa layer, of increased caliber and that sometimes is subject to bleeding when it suffers an ulceration over its mucosa and becomes exposed [4]. Dieulafoy esophageal lesions are very rare, especially when related to patients with megaesophagus. Another peculiar aspect of the case is the diagnosis of megaesophagus in an accentuated degree, already with tortuosity, in a previously asymptomatic patient. It is also known that megaesophagus is a rare entity, with annual incidence of approximately 1 / 100.000 inhabitants, and its main origin is idiopathic achalasia. Which leads us to think whether the formation of Dieulafoy was related to megaesophagus or not. While bleeding is most likely due to the peak of esophageal dysmotility with significant food stasis [5]. The relationship between esophageal Dieulafoy and megaesophagus is still unknown. Perhaps because of its very low incidence or even the absence of relation, this being only an intriguing case and keeping us in doubt if the formation of the Dieulafoy was related to the megaesophagus, or only food stasis caused ulceration over the existing vessel. The report draws attention to other possible associations published in the future.
- Malliaras GP, Carollo A, Bogen G (2016) Esophageal Dieulafoy’s lesion: an exceedingly rare cause of massive upper GI bleeding. J Surg Case Rep 6: 1-2. Link: https://bit.ly/36DKwf9
- Senjer JK, Kanthan R (2012) The evolution of Dieulafoy’s lesion since 1987: Then and now – a journey trough the lens of a pediatric lesion with literature. Rev Gastro Res Prac 2012: 432517. Link: https://bit.ly/3jJwOew
- Timmapuram J, Shah M, Srour J (2011) Esophageal dieulafoy lesion: an unusual case of GI bleeding. Gastrointestinal Endosc 73: 1055-1056. Link: https://bit.ly/3jDW99z
- Francis DL, Katzka DA (2010) Achalasia: update on disease and its tratment. Gastroenterology 139: 369-374. Link: https://bit.ly/3iCtlgl
- Eckardt AJ, Eckardt VF (2009) Current clinical approach to achalasia. World J Gastroenterology 28: 3969-3975. Link: https://bit.ly/2SAg9he
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
