Archives of Clinical Gastroenterology
A Case of Rapunzel Syndrome
Krisztina Csuzi1*, Orsolya Boda2, Robert Neumann2 and Gergely Peter Toth1
2Department of Surgery, Elisabeth Hospital, Sopron, Hungary
Cite this as
Csuzi K, Boda O, Neumann R, Toth GP (2020) A Case of Rapunzel Syndrome. Arch Clin Gastroenterol 6(2): 054-056. DOI: 10.17352/2455-2283.000079Trichobezoar is a concretion of chewing and swallowing hair or any other indigestible materials that accumulate in the gastrointestinal tract. Rapunzel syndrome refers to a rare condition when a gastric trichobezoar extends into the small bowel. We describe the case of a 16-year-old female who presented with chronic abdominal pain, loss of appetite and weight loss. Based on her past medical history, trichophagia has already been revealed at preschool age. Imaging tests indicated a large filling of the stomach. Upper gastrointestinal endoscopy showed a large trichobezoar in the stomach with prolonga on through the pylorus. The patient underwent exploratory laparotomy and the trichobezoar was removed. Upper gastrointestinal endoscopy is the preferred modality for diagnosis and in most cases the treatment is surgical.
Introduction
Bezoars are intraluminal accumulations of indigestible material. They have been classified into phytobezoars (comprised of vegetable and fruit residue), lactobezoars (comprised of milk residue), pharmacobezoars (comprised of pills and capsules) and trichobezoars (an accumula on of hair), according to their dominant composition [1]. Trichobezoars are common in patients with mental retardation, psychiatric disorders or personality disorders such as trichophagia and trichotillomania.
Rapunzel syndrome is a rare condition when a gastric trichobezoar extends into the small bowel increasing the risk of complications such as obstruction, perforation and peritonis [2]. The syndrome is named a er the heroine of a German fairy tale written by the Grimm Brothers and first published in 1812. The fairy tale is about a young princess with a long golden hair imprisoned by a witch in a tall tower with neither stairs nor a door [1]. One day, a prince rode through the forest and heard Rapunzel singing from the tower. After a while, they fell in love with each other, the princess lowered her long hair to the ground from her window, so the prince could climb up and rescue her.
Case report
A 16-year-old female was referred to our Paediatric Department with abdominal pain for two years, loss of appetite and weight loss for a month. Two years earlier the patient was treated with acute pancreatitis in another hospital. During the treatment abdominal ultrasound and MRI scan were taken showing a diffuse parenchymal enlargement. Other laboratory examinations could not clarify the aetiology. Three months later the patient visited the emergency department of the same hospital because of heavy epigastric pain. The examinations excluded acute pancreatitis, her pain was considered gastric hyperacidity and she was proposed to take proton-pump inhibitor. The patient’s condition did not improve during medication.
Over time, her complaints were associated with weight loss and loss of appetite. During an examination carried out by the family doctor a palpable firm mass was revealed in the epigastric region. The rest of the physical examination was unremarkable. After that the patient underwent the following investigations. Abdominal ultrasound showed a large-scale echogenic mass in the stomach with dense posterior acoustic shadow. Barium meal test showed intraluminal filling defect with a size of 13 × 5 cm. Based on her past history, trichophagia was present at preschool age.
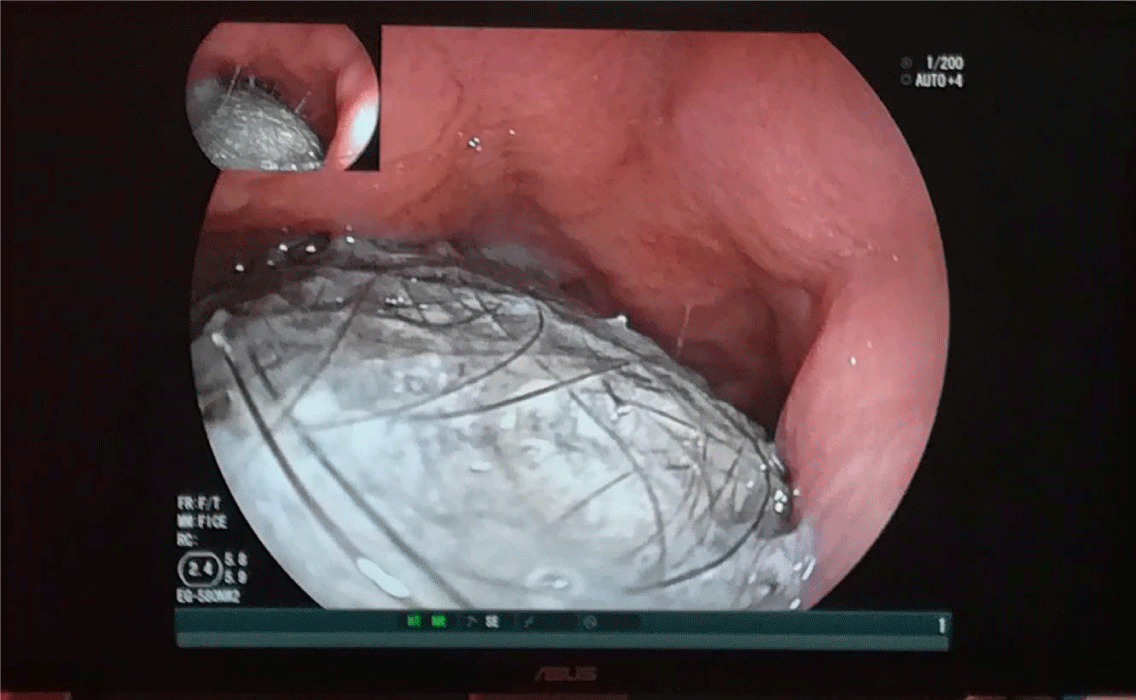
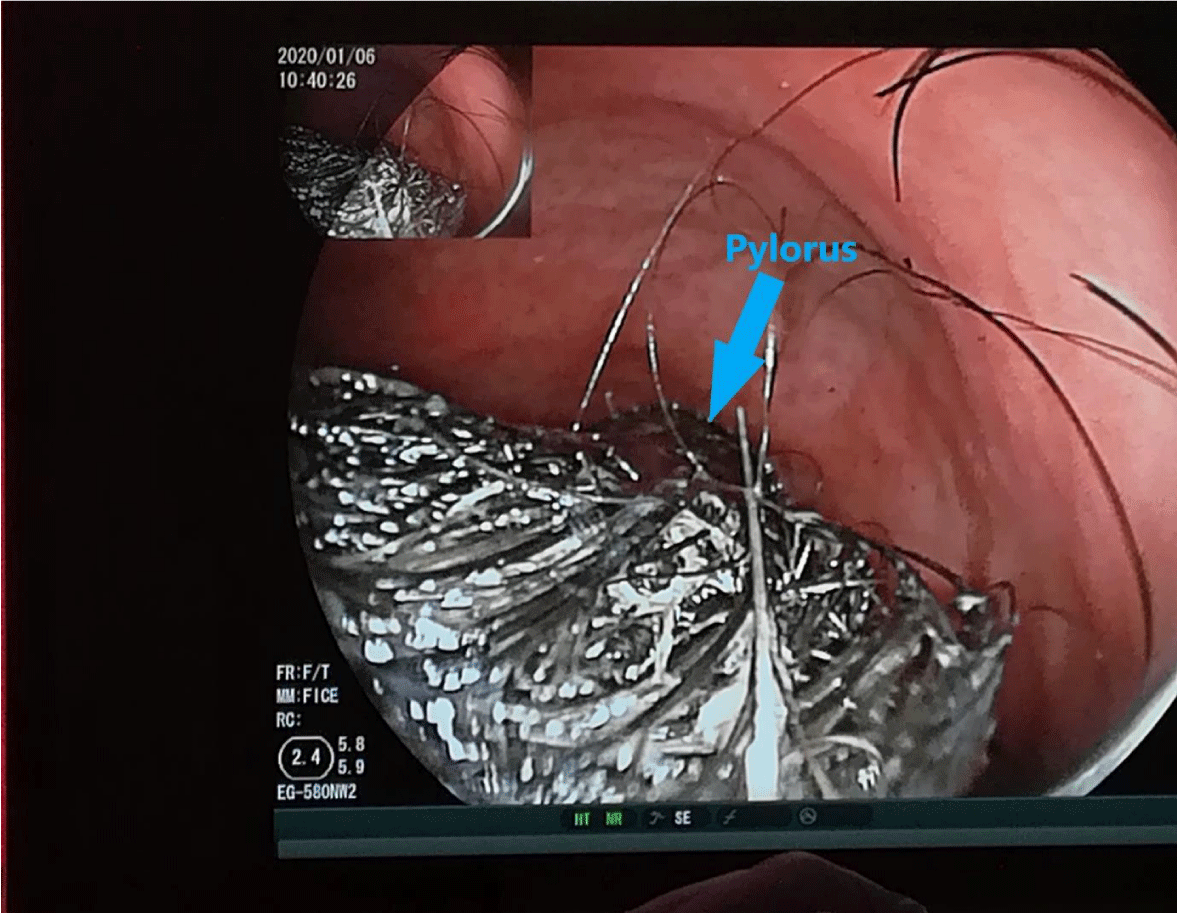
The patient was referred to our Department with the above-mentioned symptoms and examination results. In our Department gastroscopy took place and it revealed a huge gastric trichobezoar (Figure 1) with prolongation through the pylorus (Figure 2).
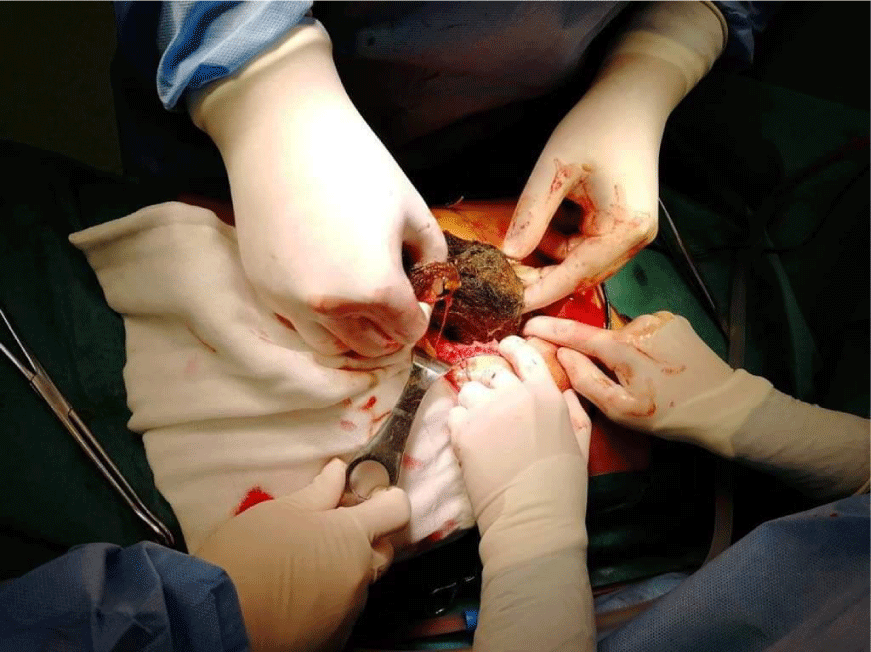
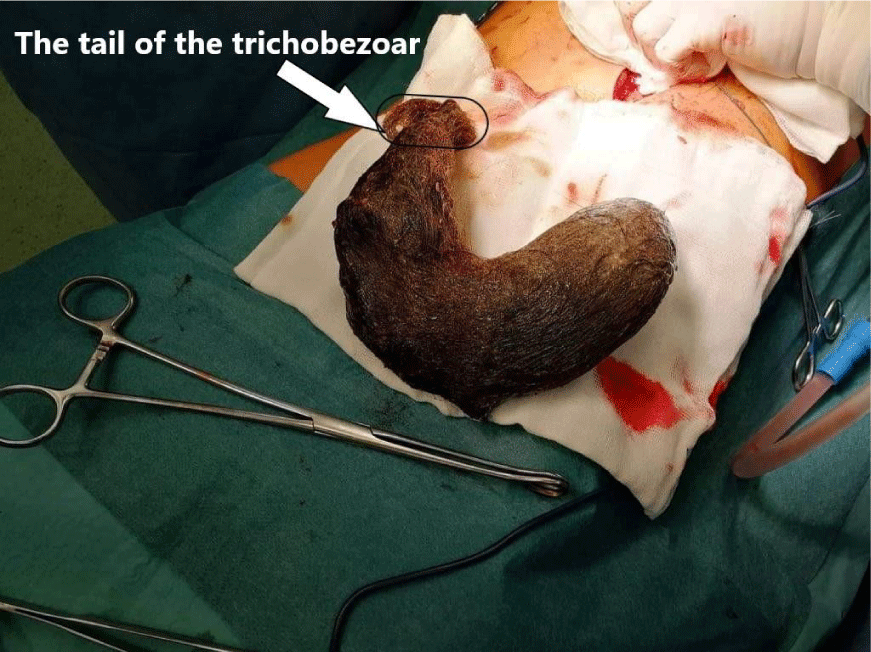
The patient underwent gastrostomy (Figure 3), with retrieval of the trichobezoar without any surgical complica tions. The stomach-shaped mass measured 20.0 × 5.0 × 5.0 cm (Figure 4) and had a tail of hair extending through the pylorus into the middle part of the duodenum.
According to these symptoms and examination results we expected to find a large bezoar during the gastroscopy but we could not expect that it extended through the pylorus. Because of the large size it was certain that surgical intervention was needed. So the actual outcome of the treating plan was similar to our expected outcome. Since then the patient has been under gastroenterological control.
This case report has been written with the patient consent and institutional approval.
Discussion
We have described a rare cause of chronic abdominal pain among children by introducing the case of a 16-year-old female who had a history of trichophagia. The diagnosis was based on the patient’s medical history, physical examination, imaging tests and upper gastrointestinal endoscopy. The bezoar was removed by exploratory laparotomy. Rapunzel syndrome is a rare condition in paediatric population. During the differential diagnosis of chronic abdominal pain, we have to think about Rapunzel syndrome if there is a history of trichotillomania or trichophagia.
Trichobezoar is a concretion of chewing and swallowing hair that accumulates in the stomach and fails to pass through the intestines. If it extends into the small intestine, it is referred to as Rapunzel syndrome. The syndrome was first described by Vaughan, et al. in 1968 [3,4].
It is a very rare entity in paediatric population, most commonly affecting women under the age of 30, mainly associated with psychiatric conditions [5].
Symptoms could include abdominal pain, loss of appetite, nausea/vomiting, and weight loss. Patients can be asymptomatic until the bezoar reaches the point of obstruction. The following complications may occur: gastric ulceration, acute pancreatitis, gastric perforation, obstructive jaundice, complete intestinal obstruction, severe peritonitis [6,7].
Small bezoars can be extracted via endoscopy using various disintegrating techniques, but in most cases a surgical management is needed because of the large size [8,9]. Rou tine endoscopy, ultrasonography can be used for detection of recurrence.
- Kim JS, Nam CW (2013) A Case of Rapunzel Syndrome. Pediatr Gastroenterol Hepatol Nutr 16: 127-130. Link: https://bit.ly/2WRhFxZ
- Nieto JO, Suárez JV, Vergara JJV, Molina JMT (2011) Rapunzel Syndrome. A case report and literature review. Rev Col Gastroenterol 26: 58-60. Link: https://bit.ly/32UDUaq
- Vaughan ED, Sawyers JL, Sco HW (1968) The Rapunzel syndrome: An unusual complication of intestinal bezoar. Surgery 63: 339-343. Link:
https://bit.ly/2WPm3xJ - Finale E, Franceschini P, Danesino C, Barbaglia M, Guala A (2018) Rapunzel syndrome: how to orient the diagnosis. Pediatr Rep 10: 7689. Link:
https://bit.ly/30NxxTs - Lyons D (2019) Large gastric trichobezoar causing failure to thrive and iron deficiency anaemia in an adolescent girl: a case report emphasising the imaging findings and review of the literature. BJR Case Rep 5: 20180080. Link: https://bit.ly/2OVEoER
- Jensen AR, Trankiem CT, Lebovitch S, Grewal H (2005) Gastric outlet obstruction secondary to a large trichobezoar. J Pediatr Surg 40: 1364-1365. Link: https://bit.ly/3hwIIqv
- Lalith S, Gopalakrishnan KL, Ilangovan G, Jayajothi A (2017) Rapunzel Syndrome. J Clin Diagn Res 11: TD01-TD02. Link: https://bit.ly/30NXx0S
- Gupta A, Kaur J, Wadhwa N (2017) Rapunzel syndrome in a seven year old female. Turk J Pediatr 59: 598-600. Link: https://bit.ly/2WRgE99
- Fallon SC, Slater BJ, Larimer EL, Brandt ML, Lopez ME (2013) The surgical management of Rapunzel syndrome: a case series and literature review. J Pediatr Surg 48: 830-834. Link: https://bit.ly/3eT6c7u
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
