Archives of Clinical Gastroenterology
Non-surgical acute cholecystitis: 2 cases of gallbladder rupture after internal endoscopic or percutaneous diversion
Lorenzo Monfardini1*, Claudio Sallemi1, Nicolo’ Gennaro2 and Claudio Bna1
2Training School in Radiology, Humanitas University, Via R.L. Montalcini 4, 20090 Pieve Emanuele, Milan, Italy
Cite this as
Monfardini L, Sallemi C, Gennaro N, Bna C (2020) Non-surgical acute cholecystitis: 2 cases of gallbladder rupture after internal endoscopic or percutaneous diversion. Arch Clin Gastroenterol 6(2): 022-025. DOI: 10.17352/2455-2283.000073Gallbladder rupture is a rare but serious complication of acute cholecystitis. We describe two cases of acute cholecystitis in patients not candidate for surgery that underwent internal biliary drainage with endoscopic and percutaneous approach, respectively. Both experienced gallbladder rupture in the postoperative period. The complication occurred after percutaneous internal drainage was treated conservatively, whereas the latter occurred after the endoscopic maneuver required an external percutaneous approach. After a brief revision of the literature about the interventional management of acute cholecystitis, the Authors discuss the possible reasons of galbladder rupture.
Introduction
Gallbladder rupture is a rare but serious complication of Acute Cholecystitis (AC) [1]. Usually presenting as a consequence of a local uncontrolled inflammation, it has never been reported to occur after gallbladder drainage. We describe two cases of AC with contraindication to surgery that underwent internal biliary drainage with percutaneous and endoscopic approach, respectively. They both experienced rupture of the gallbladder in the post-treatment follow-up. The complication was managed conservatively in the case of the percutaneous treatment, whereas gallbladder rupture occurring after endoscopic treatment required an external percutaneous approach.
Case report 1
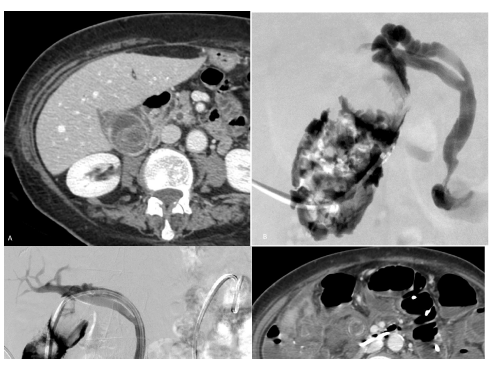
An 84-year old woman with previous lithiasis of the common bile treated with endoscopic sphincterotomy was admitted to ER for acute right flank pain. Laboratory, clinical and imaging findings suggested acute calculous cholecystitis (Figure 1). Because of the non-surgical profile (ASA score= 4), she underwent a percutaneous internal drainage of the gallbladder via the cystic and the common bile duct to the duodenum. Cholangiography showed opacification of the biliary tree without lithiasis of the cystic duct. A 26 cm 8F double J-ureteral stent was then advanced until the distal tip was lying in the II part of the duodenum (Figure 1c). After downsizing to 6F, the external drainage was removed with the unattended recommendation to undergo an endoscopic substitution not later than 3-4 months. The patient came again to our attention after 8 months with fever and hypogastrium pain. Contrast-enhanced CT scan did not reveal the the gallbladder but only hyperdense stones in the peritoneal cavity (Figure 1d). A medical treatment stabilized the patient and avoid further complications. The patient was discharged few days later to a nursing home where she kept healthy until the time of writing.
Case report 2
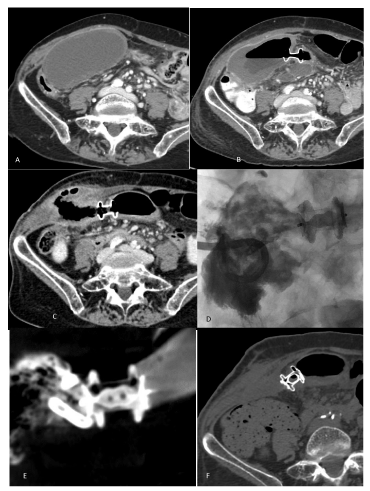
An 85-year old woman was admitted to ER for upper abdominal pain, jaundice and fever. She had previous history of common bile duct lithiasis treated with endoscopic sphincterotomy and stones retrieval. She underwent contrast-enhanced CT scan that showed gallbladder distention with thickened, enhanced walls and hyperdense material in both the common bile and cystic duct (Figure 2a). An endoscopic cleaning of common bile duct was conducted and in the same session an endoscopic ultrasound-guided internal gallbladder drainage (Hot AXIOS™, Boston Scientific, Marlborough, MA, USA) was placed with the intention to reduce the gallbladder distention by diverting the bile into the duodenum. 5 weeks later the patient was readmitted because of a right flank swelling and pain. Contrast-enhanced CT scan instead of gallbladder revealed a collection with air and fluid communicating with the duodenum (Figure 2c). Due to the risk of an external fistulisation, a percutaneous drainage was placed. In order to occlude the diversion to the digestive tract, a 12 mm Amplatzer plug II (St. Jude Medical, St. Paul, MN, USA) was delivered inside the AXIOS. An external drainage was left in situ until any fluid secretions ceased. 1 month later, the external drainage was removed and a contrast-enhanced CT scan confirmed the successful diversion occlusion and the disappearance of the collection (Figure 2e). Gastroscopy was eventually performed to assess the duodenal walls around the AXIOS system and the delivered Amplatzer plug, confirming no alterations in the mucosal layer.
Discussion
We described two cases of AC treated with percutaneous or endoscopic approach. The dissimilar therapeutic strategy was due to the different on-call physicians. However, in both cases the gallbladder underwent a complete rupture in the late postoperative period.
Gallbladder perforation is a well-known complication of chronic cholecystitis and is usually due to the obstruction of the cystic duct that starts a cascade reaction [1]. Retention of intraluminal secretions distends the gallbladder until the rise of the intraluminal pressure impedes venous and lymphatic drainage. The vascular compromise ultimately leads to ischemia, necrosis and perforation. Spontaneous gallbladder perforation and other causes of non traumatic gallbladder perforations have also been reported [2, 3].
The endoscopic and percutaneous internal biliary drainage have been described in the management of AC and represent established approaches in non-surgical candidates [4–10]. Jatrogenic gallbladder perforation during surgery have been also described [2], but perforation after non surgical management of AC has rarely been reported so far [4].
Hypomotility has been recognized as an important risk factor for biliary lithiasis and AC. The delay in emptying the lumen favours stasis with sludge formation and represent a risk factor for chronicization of the inflammation even in the presence of a patent cystic duct [11]. Chronic inflammation is a well-known risk factor for gallbladder perforation [12]. We postulate hypomotility to be the responsible mechanism of the evolution of the described cases even as possible cause of stent obstruction, regardless the technique. In fact, the success of internal biliary drainage, performed either with percutaneous (case #1) or endoscopic (case #2) approach, relies on the intrinsic capacity of the gallbladder to empty into the duodenum.
At this regard, an external percutaneous drainage may stand as the elective therapeutic strategy in non-surgical patients, since it overcomes gallbladder hypomotility and allows washing and emptying of the lumen. Even if these operations can be performed also after the placement of an endoscopic drainage, they are indeed more practical and better tolerated when performed through a percutaneous drainage rather than a nasoduodenal catheter, which is hardly tolerated and whose small caliber may hamper washing and emptying maneuvers. Moreover, a percutaneous external approach avoids invasive procedures like sphincterotomy whose complications like pancreatitis, local infections, can be barely tolerated by critical ill patients.
A novel method to interrupt the biliary-duodenal diversion was performed in case #2. To the best of our knowledge, using an Amplatzer vascular plug has never been described in this setting and resulted to be a successful therapeutic choice. Being most of vascular interventional radiologists familiar with, the Amplatzer vascular plug matches perfectly within the AXIOS system. This intrinsic feature should be known by operators and its use in this setting needs to be included among its possible off-label and non-routine use.
In conclusion, gallbladder rupture is a possible complication of AC treated with an internal bile diversion, being it performed either with an endoscopic or a percutaneous approach. Recognizing hypomotility as a risk factor for AC chroniziaction, external percutaneous drainage stands as the elective therapeutic strategy in non-surgical patients with hydropic AC. Amplatzer vascular plug may be used to occlude a biliary-duodenal diversion achieved with the AXIOS system.
Authorship contribution statement
First Author: Data curation, Formal analysis, Writing - original draft, review & editing.
Second third Authors: Methodology, Writing - original draft, submission advicer.
Fourth Author: Conceptualization, Supervision, Clinical setting.
Ethical approval: This study was not submitted to the Ethics Committee but only Written informed consent was obtained from the two participants.
Competing interest: No benefits in any form have been received or will be received from a commercial party related directly or indirectly to the subject of this article.
Novelty of work: images of fig 2 have already been published in a letter to Editor (Cardiovasc Intervent Radiol. 2020 Apr;43(4):652-654. doi: 10.1007/s00270-020-02419-3. Epub 2020 Jan 27.)
Journal pertinence: Non-surgical acute cholecystitis is an open issue for surgeons. This short report underline the rising role of IR’s in his management mostly in cases in which gallbladder motility can be compromised and percutaneous approach could be worthwhile rather than endoscopic one
Thank you for receiving our manuscript and considering it for peer review process. We appreciate your time and looking forward to here backs you.
Please contact me at the below address for your correspondence.
- Derici H, Kara C, Bozdag AD, Nazli O, Tansug T, et al. (2006) Diagnosis and treatment of gallbladder perforation. World J Gastroenterol 12: 7832-7836. Link: https://bit.ly/2WnuoaH
- Morrin MM, Kruskal JB, Hochman MG, Saldinger PF, Kane RA, et al. (2000) Radiologic features of complications arising from dropped gallstones in laparoscopic cholecystectomy patients. AJR Am J Roentgenol 174: 1441-1445. Link: https://bit.ly/3dbhELe
- Subasinghe D, Udayakumara EAD, Somathilaka U, Huruggamuwa M (2016) Spontaneous perforation of common bile duct: A rare presentation of gall stones disease. Case Rep Gastrointest Med 2016: 5321304. Link: https://bit.ly/2WrK5Op
- Anderloni A, Leo MD, Carrara S, Fugazza A, Maselli R, et al. (2018) Endoscopic ultrasound-guided transmural drainage by cautery-tipped lumen-apposing metal stent: exploring the possible indications. Ann Gastroenterol 31: 735-741. Link: https://bit.ly/2SAX6Ea
- Walter D, Teoh AY, Itoi T, Pérez-Miranda M, Larghi A, et al. (2016) EUS-guided gall bladder drainage with a lumen-apposing metal stent: a prospective long-term evaluation. Gut 65: 6-8. Link: https://bit.ly/2WtWkKm
- Khan MA, Atiq O, Kubiliun N, Ali B, Kamal F, et al. (2017) Efficacy and safety of endoscopic gallbladder drainage in acute cholecystitis: Is it better than percutaneous gallbladder drainage? Gastrointest Endosc 85: 76-87.e3. Link: https://bit.ly/3dhrbAx
- Bundy J, Srinivasa RN, Gemmete JJ, Shields JJ, Chick JFB (2018) Percutaneous Cholecystostomy: Long-Term Outcomes in 324 Patients. Cardiovasc Intervent Radiol 41: 928-934. Link: https://bit.ly/3bWBTfo
- Ahmed O, Rogers AC, Bolger JC, Mastrosimone A, Lee MJ, et al. (2018) Meta-analysis of outcomes of endoscopic ultrasound-guided gallbladder drainage versus percutaneous cholecystostomy for the management of acute cholecystitis. Surg Endosc 32: 1627-1635. Link: https://bit.ly/2zVDkg4
- Hatzidakis A, Venetucci P, Krokidis M, Iaccarino V (2014) Percutaneous biliary interventions through the gallbladder and the cystic duct: What radiologists need to know. Clin Radiol 69: 1304-1311. Link: https://bit.ly/3d4ZT06
- Raymond CJ, Khayat M, Chick JFB, Srinivasa RN (2019) Endoscopy as an Adjunct to Image-Guided Interventions: A New Frontier in Interventional Radiology. Tech Vasc Interv Radiol 22: 119-124. Link: https://bit.ly/2ygVIQa
- Behar J, Mawe GM, Carey MC (2013) Roles of cholesterol and bile salts in the pathogenesis of gallbladder hypomotility and inflammation: cholecystitis is not caused by cystic duct obstruction. Neurogastroenterol Motil 25: 283-290. Link: https://bit.ly/2W0uu9m
- Stinton LM, Shaffer EA (2012) Epidemiology of gallbladder disease: cholelithiasis and cancer. Gut Liver 6: 172-187. Link: https://bit.ly/2yo6DHH
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
