Archives of Clinical Gastroenterology
Characterization of patients with primary biliary cholangitis and autoimmune hepatitis from a community hospital in East Harlem
Priyanka Yerragorla1#, Divya Nekkalapudi2#, Ahmed Shady3# and Nora V. Bergasa4*
Cite this as
Yerragorla P, Nekkalapudi D, Shady A, Bergasa NV (2020) Characterization of patients with primary biliary cholangitis and autoimmune hepatitis from a community hospital in East Harlem. Arch Clin Gastroenterol 6(1): 006-009. DOI: 10.17352/2455-2283.000068Background and objectives: Primary Biliary Cholangitis (PBC) and Autoimmune Hepatitis (AIH) are uncommon autoimmune diseases in the United States. There is limited information in regards to those two conditions in Black Americans and subjects of Hispanic ethnicity; thus, we conducted a study to characterize patients with these diseases in a community hospital that serves this type of population.
Methods: A retrospective review from 2001 to 2017 of all electronic medical records of patients with diagnoses of PBC or AIH according to the International Classification of Diseases (ICD 10) was conducted. This period was chosen because of feasibility.
Results: Fifteen patients with PBC were identified, one of whom was a man, all were of Hispanic ethnicity and all were in precirrhotic stages. The response to Ursodeoxycholic Acid (UDCA) was suboptimal, however, no complications from liver disease were identified during the study period.
Five women with AIH were identified, all were of Hispanic ethnicity, all were treated with prednisone and azathioprine with appropriate response.
Conclusions: Hispanic patients with AIH respond to treatment appropriately. However, patients with PBC exhibited a suboptimal response to UDCA.
Pharmacogenetic studies should be considered in Hispanic patients in regards to the use of UDCA.
Introduction
Primary Biliary Cholangitis (PBC) and Autoimmune Hepatitis (AIH) are uncommon immune mediated chronic liver diseases [1-3]. Most of the literature on the epidemiology of these two conditions is derived from Caucasian populations; in the United States, there is limited information in regards to PBC and AIH in Black Americans and in subjects of Hispanic ethnicit [4-11].
New York City Health+Hospitals/Metropolitan serves the community of East Harlem, populated mostly by black Americans, black Africans and subjects of Hispanic ethnicity; accordingly, the aim of this study was to characterize the patients with AIH and PBC attended at this institution, and to explore communalities between them and patients from the country that gave the Hispanic community its language, Spain.
Methods
A retrospective review of medical records coded as PBC or AIH by the ICD 10 classification from 2001-2017 was conducted. This time period was chosen because of feasibility to access electronic medical records. The study was approved by the institutional review board.
Results
One patient was diagnosed with AIH at hospitalization for acute hepatitis; all other patients with AIH or PBC were referred to the hepatology clinic because of abnormal liver profile (Tables 1,2). None of the patients from either group had end stage liver disease or hepatocellular carcinoma over the period of the study.
Fifteen patients had a diagnosis of PBC, one of whom was a man; the mean age was 65 years, with a range of 38-91. All were of Hispanic ethnicity. The most common symptom was documented as pruritus in eight patients, all of whom were treated with cholestyramine, associated with relief, and fatigue in one. The coexistent autoimmune diseases were scleroderma in three patients and hypothyroidism also in three patients. No stigmata of chronic liver disease were documented from any of the patients.
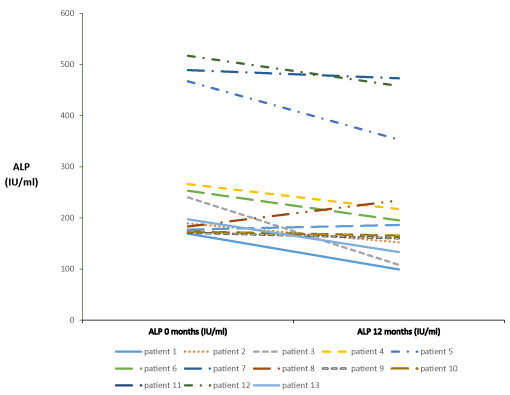
In the group of patients with PBC, fourteen patients had positive Anti Mitochondrial Antibodies (AMA) in serum and eleven had Anti-Nuclear Antibodies (ANA). The mean serum IgG concentration was 1,592 mg/dL with a range of 1,130-3,280 (normal 690-1,140), and the mean IgM was 281 mg/dL with a range of 64-626 (normal 40-240). Five patients had probable PBC (i.e. chronic cholestatic liver profile and positive AMA) [12] and one was AMA negative but, liver histology was consistent with the disease. Of the patients in whom liver histology was available, five had stage I, four stage II and one stage IV [13]; four of the patients had steatosis. All had been treated with Ursodeoxycholic Acid (UDCA) from the time of diagnosis (Table 1) [14]. According to the Barcelona criteria [15] and based on the serum Alkaline Phosphatase (ALP) activity, three patients exhibited complete response, ten patients did not respond, and in the two patients with initially normal serum activity of ALP, it remained the same. The mean reduction in serum ALP activity was 14% (Figure 1). The globe score [16] in three of the fifteen patients (20%) at the end of one year of treatment predicted a low transplant free survival.
In the group of AIH there were five women of Hispanic ethnicity with a mean age of 51 years (range 41-66). One patient reported transient pruritus, which was treated with cholestyramine, associated with documented relief and one had icterus on exam, which resolved on treatment. Two patients had systemic lupus erythematosus and one had psoriasis. Of the five patients, three were positive for anti-smooth muscle antibody and four had ANA in their serum. The mean serum IgG was 1,164 mg/dl with a range of 940-2,040 (normal 690-1,140). Three patients had grade II and one had grade III inflammation on liver histology [17]; one patient had stage I fibrosis and three had stage II [17]. All were treated with prednisone and azathioprine or 6-mercaptopurine after diagnosis (Table 2).
Discussion
In this retrospective study of patients with PBC or AIH, the majority of patients was of Hispanic ethnicity and was pre-cirrhotic, and the minority had other associated autoimmune diseases. Pruritus was the most common symptom in PBC. In association with treatment with UDCA at one year, only three patients (23%) exhibited complete response to the drug [15], with a small mean decrease in ALP activity. Liver profile normalized itself on immunosuppression in AIH.
The percentage of patients with PBC that reported pruritus was 53%, as compared to the 70% that has been consistently documented in the world literature [18]. In addition, only one patient (6%) reported fatigue, which is substantially lower than what has been reported in other studies, especially, in the recent literature [19]. This is an important observation because it has been proposed that most Hispanic patients with PBC report pruritus and fatigue in its majority [20]. We wonder if the absence of fatigue in our study group is a reflection of the need to survive in the challenging socio-economic situations that some of the patients from the community that the hospital serves may face, and that may not allow them to focus on lack of energy level.
In general, approximately 35% of patients do not experience a significant reduction in serum activity of ALP in association with UDCA [21,22]; these are patients who appear to have a decrease in survival free from liver transplantation [15,21-23]. In contrast to patients with AIH who responded well to the standard of care (i.e. immunosuppression), only three patients with PBC (23%) exhibited normalization in the serum ALP activity in association with UDCA. In fact, in our study the mean decrease in ALP activity at one year of treatment was only 14%; this finding may suggest that pharmacogenetics of patients of Hispanic ethnicity may play a role in their response to treatment with this medication [24].
The Globe score predicted a good transplant free survival in twelve of the fifteen patients (80%) at the end of one year of treatment. In this context, although the globe score predicted accurately in the majority of patients, it is worth noticing that this score was derived from data on the local population from eight European and North American countries, which are mostly comprised of non-Hispanic subjects, and, although some patients included in this derivation might have been of Hispanic ethnicity, the genesis of the score raises a question on the validity and applicability of the globe score on the Hispanic population in general.
Although the number of patients in this study is small, we would like to point out some similarities to those from the study from Spain. The prevalence of pruritus and fatigue from the study from Spain was 27 and 47 %, respectively [25], lower than what has been published by other groups [19], and also a finding in our study; this result may be the expression of the suggested genetic predisposition to be protected (or to have susceptibility) from pruritus [26,27] (and fatigue). In addition, the combined percent of subjects that had incomplete or no response to UDCA was 77% in our study and 56% in the one from Spain [25], both higher than the 35% reported from other studies [21]. By definition, Hispanics are a heterogeneous population and as a group, they are underrepresented in research studies [24,28,29]. There is interethnic and intraethnic variability in the genetics of metabolizing enzymes, which highlights the need to define the ancestries of the population studied in clinical trials, including patients of Hispanic ethnicity with PBC.
In contrast to the patients with PBC, those with AIH who were also of Hispanic ethnicity and who were treated with immunosuppression medications, showed biochemical remission with the treatment, suggesting that ethnicity may not have an impact on the response to this type of drug.
This study is limited by its retrospective nature; however, we can conclude that PBC and AIH are not common in the community of East Harlem, consistent with their definition as rare diseases [2,3]. Liver disease was promptly recognized at referral, as suggested by the pre-cirrhotic stages at diagnosis. Biochemical response to treatment was appropriate in AIH; however, in PBC, the response was lower than what has been considered optimal. Although lack of adherence to treatment cannot be unequivocally excluded, the effects of ethnicity on response to UDCA cannot be ignored; thus, pharmacogenetic studies in patients of Hispanic ethnicity with PBC merit consideration.
- Imam MH, Lindor KD (2014) The Natural History of Primary Biliary Cirrhosis, Semin Liver Dis 34: 329-333. Link: http://bit.ly/38tYfmW
- Manns MP (2011) Autoimmune Hepatitis: The Dilemma of Rare Diseases. Gastroenterol 140: 1874-1876. Link: http://bit.ly/2UWWtXc
- Floreani A, Tanaka A, Bowlus C, Gershwin ME (2017) Geoepidemiology and Changing Mortality in Primary Biliary Cholangitis. J Gastroenterol 52: 655-662. Link: http://bit.ly/2uNarAi
- Levy C, Naik J, Giordano C, Mandalia A, O’Brien C, et al. (2014) Hispanics with Primary Biliary Cirrhosis Are More Likely to Have Features of Autoimmune Hepatitis and Reduced Response to Ursodeoxycholic Acid than Non-Hispanics. Clin Gastroenterol Hepatol 12: 1398-1405. Link: http://bit.ly/2USnqLF
- Heathcote J (1997) The Clinical Expression of Primary Biliary Cirrhosis. Semin. Liver Dis 17: 23-33. Link: http://bit.ly/3bESSmD
- Cholankeril G, Gonzalez HC, Satapathy SK, Gonzalez SA, Hu M, et al. (2018) Increased Waitlist Mortality and Lower Rate for Liver Transplantation in Hispanic Patients With Primary Biliary Cholangitis. Clin Gastroenterol Hepatol 16: 965-973.e2. Link: http://bit.ly/39u9ITi
- Poupon RE, Lindor KD, Cauch-Dudek K, Dickson ER, Poupon R, et al. (1997) Combined Analysis of Randomized Controlled Trials of Ursodeoxycholic Acid in Primary Biliary Cirrhosis. Gastroenterol 113: 884-890. Link: http://bit.ly/2SHkFdv
- Kim WR, Lindor KD, Locke GR, Therneau TM, Homburger HA, et al. (2000) Epidemiology and Natural History of Primary Biliary Cirrhosis in a US Community. Gastroenterol 119: 1631-1636. Link: http://bit.ly/38rUzlA
- Zolfino T, Heneghan MA, Norris S, Harrison PM, Portmann BC, et al. (2002) Characteristics of Autoimmune Hepatitis in Patients Who Are Not of European Caucasoid Ethnic Origin. Gut 50:713–717. Link: http://bit.ly/2OTi3Zb
- Toda G, Zeniya M, Watanabe F, Imawari M, Kiyosawa K, et al. (1997) Present Status of Autoimmune Hepatitis in Japan - Correlating the Characteristics with International Criteria in an Area with a High Rate of HCV Infection. J Hepatol 26: 1207-1212. Link: http://bit.ly/2uNaTyu
- Seki T, Kiyosawa K, Inoko H, Ota M (1990) Association of Autoimmune Hepatitis with HLA-Bw54 and DR4 in Japanese Patients. Hepatology 12: 1300-1304. Link: http://bit.ly/39JKe4P
- Metcalf JV, Mitchison HC, Palmer JM, Jones DE, Bassendine MF, et al. (1996) Natural History of Early Primary Biliary Cirrhosis 348: 1399-1402. Link: http://bit.ly/39CB4GT
- Scheuer P (1967) Primary Biliary Cirrhosis. Proc R Soc Med 60: 1257-1260. Link: http://bit.ly/39BQiMG
- Parés A (2014) Old and Novel Therapies for Primary Biliary Cirrhosis. Semin Liver Dis 2014; 34: 341-351. Link: http://bit.ly/37jAzjG
- Pares A, Caballeria L, Rodes J (2006) Excellent Long-Term Survivalin Patients with Primary Biliary Cirrhosis Andbiochemical Response to Ursodeoxycholic Acid. Gastroenterol 130: 715–720. Link: http://bit.ly/37m04AJ
- Lammers WJ, Hirschfield GM, Corpechot C, Nevens F, Lindor KD, et al. (2015) Development and Validation of a Scoring System to Predict Outcomes of Patients with Primary Biliary Cirrhosis Receiving Ursodeoxycholic Acid Therapy. Gastroenterol 149: 1804-1812 E4. Link: http://bit.ly/37svs0s
- Ishak K, Baptista A, Bianchi L (1995) Histological Grading and Staging of Chronic Hepatitis. J Hepatol 22: 696-699. Link: http://bit.ly/39yYVr2
- Bergasa NV (2014) Pruritus of Cholestasis.In: Carstens E, Akiyama T, Editors. Itch: Mechanisms and Treatment. Boca Raton (FL): CRC Press/Taylor & Francis. Chapter 6. Link: http://bit.ly/2uyqTEJ
- Lee JY, Danford CJ, Trivedi HD, Tapper EB, Patwardhan VR, et al. (2019) Treatment of Fatigue in Primary Biliary Cholangitis: A Systematic Review and Meta-Analysis. Dig Dis Sci 64: 2338-2350. Link: http://bit.ly/2USoyPp
- Peters MG, Di Bisceglie AM, Kowdley KV, Flye NL, Luketic VA, et al. (2007) Differences Between Caucasian, African American, and Hispanic Patients with Primary Biliary Cirrhosis in the United States. Hepatology 46: 769-775. Link: http://bit.ly/3byqgvo
- Corpechot C, Abenavoli L, Rabahi N (2008) Biochemicalresponse to Ursodeoxycholic Acid and Long-Termprognosisin Primary Biliary Cirrhosis. Hepatology 48: 871-877. Link: http://bit.ly/2URJ1UO
- Kuiper EM, Hansen BE, de Vries RA (2009) Improvedprognosis of Patients with Primary Biliary Cirrhosis Thathave a Biochemical Response to Ursodeoxycholic Acid. Gastroenterol 136: 1281-1287. Link: http://bit.ly/2ORj6c3
- Kumagi T, Guindi M, Fischer SE, Arenovich T, Abdalian R, et al. (2010) Baseline Ductopenia and Treatment Response Predict Long-Term Histological Progression in Primary Biliary Cirrhosis. Am J Gastroenterol 105: 2186-2194. Link: http://bit.ly/2HoRhDy
- Claudio-Campos K, Duconge J, Cadilla CL, Ruaño G (2015) Pharmacogenetics of Drug-Metabolizing Enzymes in US Hispanics. Drug Metab Pers Ther 30: 87-105. Link: http://bit.ly/31UNF5C
- Pares A (2018) Cholangitis Biliar Primaria En Espana. Resultados de Un Studio Delphi Sobre Su Epidemiologia, Diagnostic, Seguimiento y Tratamiento. Link: http://bit.ly/37o0GWM
- Wei LX, Floreani A, Variola A, El Younis C, Bergasa NV (2008) A Study of the Mu Opioid Receptor Gene Polymorphism A118G in Patients with Primary Biliary Cirrhosis with and without Pruritus. Acta Derm Venereol 88: 323-326. Link: http://bit.ly/31Q7T0A
- Floreani A, Carderi I, Variola A, Rizzotto ER, Nicol J, et al. (2006) A Novel Multidrug-Resistance Protein 2 Gene Mutation Identifies a Subgroup of Patients with Primary Biliary Cirrhosis and Pruritus. Hepatology 43: 1152-1154. Link: http://bit.ly/3bHecrZ
- Fashoyin-Aje LA, Fernandes LL, Keegan P, Sridhara R, Pazdur R (2018) Enrollment of Hispanics in Cancer Clinical Trials: An FDA Analysis. Journal of Clinical Oncology. Link: http://bit.ly/2SM1U8G
- Naranjo CM (2018) Special Populations Underrepresented in Oncology Research: Challenges and Solutions to Engage the Hispanic Population. Applied Clinical Trials. Link: http://bit.ly/39zP1pi
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
