Archives of Clinical Gastroenterology
Unusual association of two rare entities: Primary rectal linitis and Klippel-Trenaunay syndrome
Haraki I1*, El Yazal S1, Ait Errami A1, Lairani FZ1, Jiddi S1, Samlani Z1, Krati K1 and Oubaha S2
Cite this as
Haraki I, El Yazal S, Ait Errami A, Lairani FZ, Jiddi S (2019) Unusual association of two rare entities: Primary rectal linitis and Klippel-Trenaunay syndrome. Arch Clin Gastroenterol 5(1): 001-002 DOI: 10.17352/2455-2283.000059Klippel-Trenaunay syndrome (KTS) is a rare congenital disorder, characterized by the triad of vascular malformations (angioma), venous and or lymphatic malformations and asymmetrical disturbed growth of soft tissues and/or bone. Primary rectal linitis is a rare digestive tumor with very poor prognosis. We report the case of a 41-year-old patient with Klippel trenaunay syndrome who was diagnosed with primary rectal linitis.
Introduction
Klippel-Trenaunay syndrome (KTS) is a rare congenital disorder, characterized by the triad of vascular malformations (angioma), venous and or lymphatic malformations and asymmetrical disturbed growth of soft tissues and/or bone [1]. The presence of two of these elements makes the diagnosis possible [2]. Rectal linitis is a rare digestive tumor, most often found in association with gastric localization [3]. Its primitive character is much rarer [3]. Often metastatic at the time of diagnosis, its treatment is a real issue [4]. We report the case of a 41-year-old patient with KTS who was diagnosed with primary rectal linitis (PRL).
Case Report
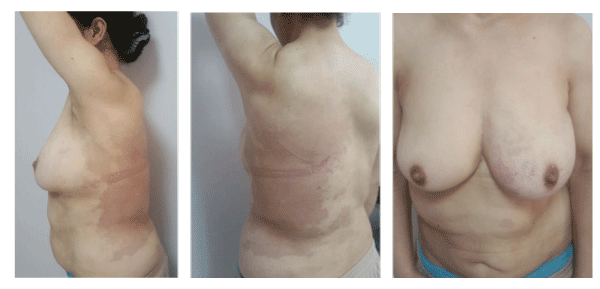
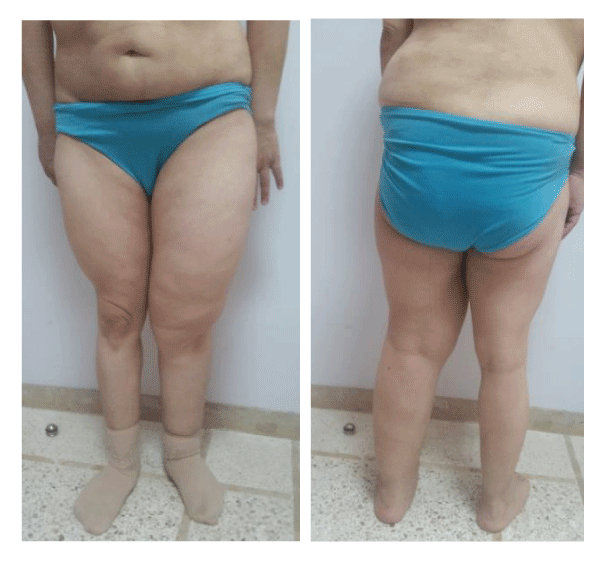
We report the case of Mrs. O.L., 41 years old, referred for recurrent hematochezia with chronic constipation and difficulties of exoneration. She reported no abdominal pain or weight loss. Flat angiomas of the left back, left breast, chest and abdomen were found, associated with hypertrophy of the left hemi-body responsible for asymmetry (Figure 1-5); which allowed us clinically to make the diagnosis of KTS. At rectal examination, a stenosis at 3 cm from the anal margin was found, partially admitting the finger pulp with pelvic shielding. A circumferential regular stenosis of the low rectum was impassable for the colonoscope. Biopsies showed a signet-cell adenocarcinoma. Upper endoscopy and echo-endoscopy showed no evidence of gastric primary tumor, breasts, gallbladder and bladder were normal). The diagnosis of PRL was made. Pelvic MRI found a circumferential rigid thickened tubular lumen of the lower rectum, measuring 20 mm in maximum thickness, spread over 100 mm in height, with infiltration of the mesorectum, loss of interface of separation with the cervical uterine region and regional lymph nodes. No distant metastases were found on the thoraco abdominal CT. It was classified T4N1 M0. Tortuous oblong formations of the costo vertebral angles of the apical region have been found, most probably related to vascular malformations completing the triad of KTS. Neoadjuvant radio-chemotherapy was proposed. In the meantime, the patient was admitted to the emergency department for an occlusive syndrome, for which a colostomy was performed. The patient was not controlled on treatment and developed pleural metastases. She died 6 months after the diagnosis.
Discussion
99 % of linitis plastica occurs in the stomach while the rest occur in the breast, gall bladder, pancreas, urinary bladder and colon [5]. Primary colorectal linitis represents less than 0.1% of all colorectal tumors, 78% of them occur in the rectosigmoid segment [4]. Diagnosis is difficult since transanal biopsies may be too superficial [2]. Primary gastric linitis shouldn’t be missed and an upper endoscopy is systematic [2]. Typical imaging features include focal / circumferential wall thickening leading to luminal narrowing. Long segment involvement is common with lesions more than 10 cms not uncommonly found [6]. This tumor has a very poor prognosis and is most often metastatic at the time of diagnosis. Treatment options are not codified. Therefore we proposed with analogy to signet-cell stomach carcinoma, an adjuvant RCT. As far as we know, no case of PRL reported was associated to KTS. It is rare condition, with an unknown etiology and an incidence of approximately 1/100 000 live births [7]. 63% of patients with KLS have the manifestation of the complete triad (port-wine stain, varicose veins, and hypertrophy of soft tissues/bones)[8]. KTS could be either caused by embryonic mesodermal changes or sporadic polygenic mutations [2]. If there is a genetic background for PRL, the association we are reporting with KTS may open the discussion of common genes between these entities.
- Mneimneh S, Tabaja A, Rajab M (2015) Klippel-Trenaunay Syndrome with Extensive Lymphangiomas. Case Rep Pediatr 2015: 581394. Link: https://goo.gl/uFmZ1u
- Oduber CE, van der Horst CM, Hennekam RC (2008) Klippel-Trenaunay syndrome: diagnostic criteria and hypothesis on etiology. Ann Plast Surg 60: 217-223. Link: https://goo.gl/GzU86v
- Sabbagh C, Chapuis-Roux E, Chatelain D, Regimbeau JM (2015) Primary rectal linitis: a rare clinical condition. J Visc Surg 152: 73-75. Link: https://goo.gl/dfr9A2
- Hyngstrom JR, Hu CY, Xing Y (2012) Clinicopathology and outcomes for mucinous and signet ring colorectal adenocarcinoma:analysis from the National Cancer Data Base. Ann Surg Oncol 19: 2814-2821. Link: https://goo.gl/U9qPLj
- Chowdhary JR, Das K, Das KM (1975) Primary linitis plastics of the colon: Report of a case and review of the literature. Dis Colon Rectum 18: 332-338. Link: https://goo.gl/X9h7q6
- Prasad S, Patankar T, Zakaria TT, Patankar Z (1998) Primary linitis plastica of the rectosigmoid in a thirteen year old boy. J Postgrad Med 44: 40-42. Link: https://goo.gl/LTs6Cr
- Barbeiro S, Brásio R, Atalaia-Martins C, Marcos P, Gonçalves C, et al. (2016) Klippel-Trenaunay syndrome: endoscopic findings. Endoscopy 48: E355-E356. Link: https://goo.gl/ANAwFP
- Jacob AG, Driscoll DJ, Shaughnessy WJ, Stanson AW, Clay RP, et al. (1998) Klippel-Trenaunay syndrome: spectrum and management, Mayo Clinic Proceedings 73: 28-36. Link: https://goo.gl/SJvJaC
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.

 Save to Mendeley
Save to Mendeley
