Annals of Circulation
New in the etiology, pathogenesis, prevention and treatment of atherosclerosis. The two different types of cholesterol plaques have nothing to do with each other?
Rusanov Sergey*
Cite this as
Rusanov S (2021) New in the etiology, pathogenesis, prevention and treatment of atherosclerosis. The two different types of cholesterol plaques have nothing to do with each other. Ann Circ 6(1): 004-011. DOI: 10.17352/ac.000018Copyright
© 2021 Rusanov S. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.The article is presented in the form of a review and analysis of the literature, which additionally helps to reveal the mechanisms of the pathogenesis of the development of atherosclerosis. This article provides a completely new understanding of the stages and sequence of atherosclerosis development. The modern vision is refuted, which states that all types of lesions in atherosclerosis are developed successively, one after another. The article sheds a light on a significant difference between type IV atherosclerotic lesions and between types V and VI atherosclerotic lesions. Type IV atherosclerotic lesions consists of one lipid core with molten extracellular lipid. Stretches the middle and outer layers of an artery from one side and protrudes beyond the anatomical artery dimensions over the years. In contrast, type V atherosclerotic lesions type is a long, concentric, soft, strong, elastic, yellow, uniform structure, in the form of a tube with a hole in the middle, located in the lumen, which is easily removed from the artery. This types V and VI atherosclerotic lesions - the author suggests calling “cylindrical cholesterol plaque”. Type V atherosclerotic lesions (cylindrical cholesterol plaque) has nothing to do with types I-V atherosclerotic lesions. There are many “coincidences” that make it impossible to see the difference between them. Type V atherosclerotic lesions (cylindrical cholesterol plaque) is an independent pathological structure that appears in a short period of time (few minutes) in the lumen of a healthy artery in case of artery spasm and appearance of a strong obstruction to blood flow. Low density lipoproteins are retained within the wall, in front of the site of arterial narrowing, and quickly create a CCP in the form of a hollow cylinder. All subsequent forms of types V and VI atherosclerotic lesions - concentric and eccentric, are the result of the destruction of the original concentric structure of the type V atherosclerotic lesions (cylindrical cholesterol plaque).
Abbreviations
ASL- atherosclerotic lesions;
ASL(I)- type I atherosclerotic lesions;
ASL(IV)- type IV atherosclerotic lesions;
ASL(I-IV)- types I-IV atherosclerotic lesions;
ASL(V)(CCP)- type V atherosclerotic lesions (cylindrical cholesterol plaque);
ASL(VI)- type VI atherosclerotic lesions;
ASL(V-VI)- types V and VI atherosclerotic lesions;
LC- lipid core with molten lipids;
LDL- low density lipoproteins;
CCP- cylindrical cholesterol plaque;
FC- fibrous cap;
FCCP- friable cylindrical cholesterol plaque;
SCCP- soft cylindrical cholesterol plaque;
DCCP- dense cylindrical cholesterol plaque;
OCCP- old cylindrical cholesterol plaque;
MFC- macrophage foam cells;
VV- vasa vasorum;
Introduction
The manuscript is presented in the form of a review and analysis of the literature, which additionally helps to reveal the mechanisms of the pathogenesis of the development of atherosclerosis. The article proposes a completely new theory on the emergence and development of Atherosclerosis (AS), which clarifies the questioned differences between type IV atherosclerotic lesions (ASL [IV]) and type V atherosclerotic lesions (ASL [V]). In classification of AS there is a description of six types Atherosclerotic Lesions (ASL) [1,2].
According to the generally accepted theory - all types of lesions develop successively, one after another - from type I atherosclerotic lesions (ASL [I]) to ASL (VI). They can be subdivided into 2 large groups: types I-V atherosclerotic lesions (ASL [I-IV]) and types V and VI atherosclerotic lesions (ASL [V-VI]).
ASL (IV) consists of one lipid core (LC) with molten extracellular lipid, stretches the middle and outermost layer of an artery and protrudes beyond the anatomical artery dimensions over the years [1] Figure 1 (Figure 1.4-1.6) .
Figure 1:
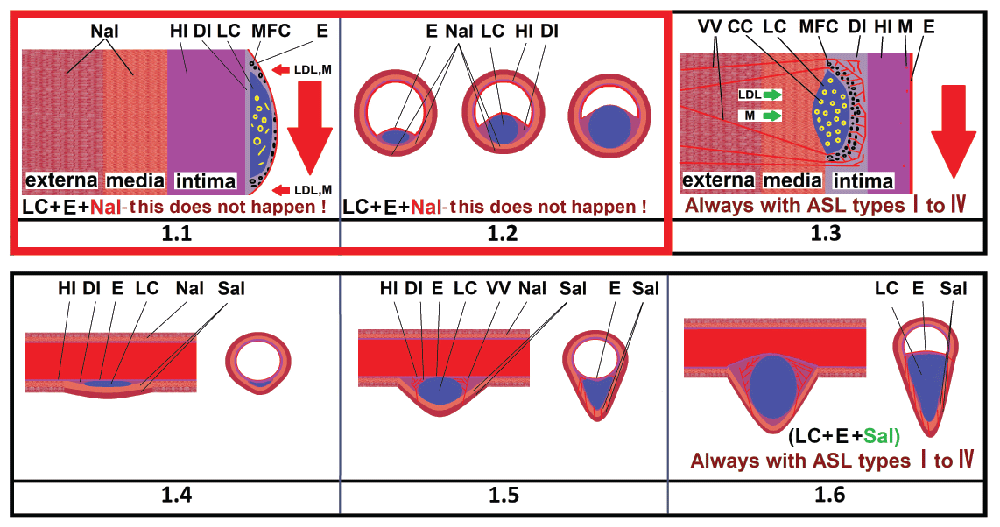
1.1) Arterial wall at the level of classic type IV atherosclerotic lesions (popular opinion). Does not correspond to the data specified in the 1995 classification. Many believe that LDL enters the “intima” through the damaged endothelium. The lipid nucleus is located just behind the damaged endothelium. The endothelium is stretched and damaged. The middle and outer layers of the artery are never stretched. The LC size increases only in the lumen of the artery. In practice, there is no situation when type IV atherosclerotic lesions has a “large lipid core under the stretched endothelium” and there are normal, non-stretched layers of the artery [3]; 1.2) Type IV atherosclerotic lesions cross-section (popular opinion). Similar to (paragraph 1.1) [3]; 1.3). The real location of the LC in intimate part. Type IV atherosclerotic lesions in coronary artery [1]. The LC is located far from the endothelium, close to the middle layer of artery. The MFCs are located close to the LC. There is an area of healthy intimate region (HI) without inflammation, without MFC, LDL, with a very small number of macrophages Between the MFC and the lumen of the artery. LDL and macrophages enter the lipid nucleus only from the outer layer of the artery, through the “vasa vasorum”[1]; 1.4-1.6) The longitudinal and transverse section of the types I-IV atherosclerotic lesions, according to the classification [1,2], looks like a tubercle that protrudes beyond the anatomical dimensions of the artery. Also looks like a tubercle protruding inward (into the lumen) of the artery in type IV atherosclerotic lesions. Always limited to a few millimeters LC length. Always contains liquid lipids in the lipid core. There is always an area of healthy intima near the endothelium. Always has a whole endothelium. Never has a fibrous cap. Always stretches the middle and outer layer of the artery. It always has blood vessels that start from the outer layer of the artery [5].
CC - cholesterol crystals; DI - damaged artery intima; E - endothelium; HI - healthy intima of the artery; LC - lipid core with molten lipids; LDL - low density lipoprotein; M - single macrophages; MFC - macrophage foam cells; Nal - normal artery layers; Sal - stretched artery layers; VV - vasa vasorum.
In contrast, ASL (V) is a long, concentric, soft, strong, elastic, yellow, uniform structure, in the form of a tube with a hole in the middle, located in the lumen, which is easily removed from the artery without damaging its walls. This cylindrical - the author suggests calling “cylindrical cholesterol plaque” (CCP) (Figures 2,3).
Figure 2:
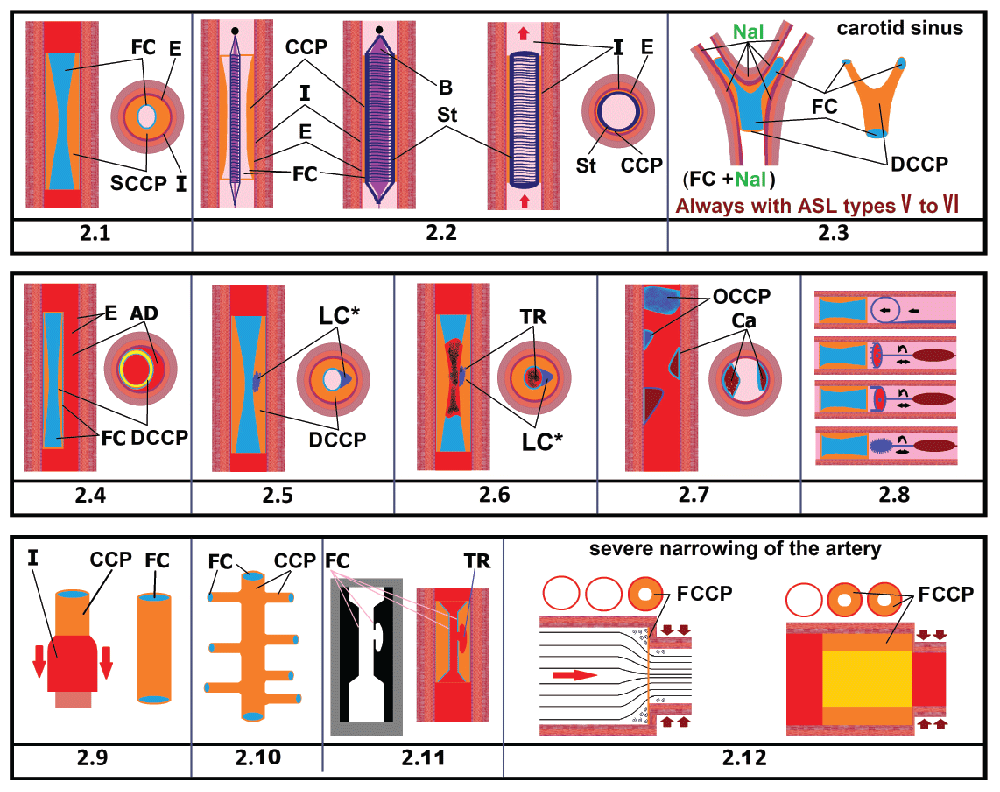
2.1) There is a long, soft, elastic, strong, solid, yellow tube in the form of a hollow cylinder located in the arterial lumen, have a concentric arrangement. Endothelium is located between “intima” and the external wall CCP. The blood passes through a narrow passage in the center of CCP. Always has FC [6,7]; 2.2) CCP has a concentric shape, is easily stretched in different directions with a balloon and fixed with a stent. The anatomical dimensions of the artery do not change [8]; 2.3) Branching of the CCP in the lateral branches of the artery in the carotid sinus. CCP follows the contours of the artery, is located on all sides, close to the artery wall. Blood flows inside the CCP and moves away from the artery walls. The anatomical dimensions of the artery do not change [6,9-11]; 2.4) Dissection of the artery. The strong outer wall of the CCP can break away from the inner artery wall so that blood can flow between the CCP and the artery wall, forming a pathology - an arterial dissection [12]; 2.5) FC damage and penetration of macrophages into the CCP wall, LC formation in the CCP wall. The LC is located only inside the CCP wall [13]; 2.6) Blood clot formation at the site of FC damage [14]; 2.7) calcium crystals deposition in the CCP wall. All subsequent forms of types V and VI atherosclerotic lesions, concentric and eccentric, are the result of the destruction of the original concentric structure of the CCP. The artery wall near CCP does not have inflammation, VV and LC, bleeding sites, protruding parts, sprain of the artery membranes, has a normal appearance of the inner and outer surfaces [15]; 2.8) Use of instruments having a form of ring and cylinder to remove CCP, in case of types I-V atherosclerotic lesions, there are no such instruments [16,17]; 2.9) The artery wall that is intact, without inflammation, without tubercles and necrosis, can be easily turned inside out [18,19]; 2.10) Branching of the CCP in the lateral branches in the arteries of the heart. The anatomical dimensions of the artery do not change [20,21]; 2.11) X-ray with contrast agent and longitudinal section of the artery with CCP. Bleeding in the LC. LC located in the CCP wall itself, immediately under the FC. The artery wall remains intact. CCP consists of LDL only. The anatomical dimensions of the artery do not change. When examining CCP it can be seen that CCP pinches the artery evenly on all sides of the artery. It can be seen that the blood passes through a narrow passage in the center of CCP [6,14,22]; 2.12) Formation of CCP in the vortex when a strong narrowing of the arterial lumen occurs. All blood cells easily pass into formed narrow opening, and only low density lipoproteins (LDL) are retained within the wall, in front of the site of arterial narrowing, and quickly create a CCP in the form of a hollow cylinder [23-25].
AD - Dissection of the artery; B- Balloon; Ca- Calcium crystals deposition; CCP- Cylindrical Cholesterol Plaque; DCCP- Dense Cylindrical Cholesterol Plaque; E- Endothelium; FC- Fibrous Cap; FCCP- Friable Cylindrical Cholesterol Plaque; I- Intimate area; LC*- the lipid core is located not within the arterial wall, but within the wall of the CCP itself; OCCP- Old cylindrical cholesterol plaque; SCCP- Soft cylindrical Cholesterol Plaque; St- Stent; TR- Blood Clot.
Figure 3:
3.1-3.10) There is a long, soft, elastic, strong, solid, yellow tube in the form of a hollow cylinder located in the arterial lumen, have a concentric arrangement. CCP follows all the contours of the artery. The blood passes through a narrow passage in the center of CCP. Always has FC. CCP can have any length - from a centimeter to tens of centimeters. The outer wall of the CCP is always smooth and does not depend on the presence of an LC inside the wall of the CCP [26-28]; 3.1-3.7, 3.9,3.10) The length of types V and VI atherosclerotic lesions in the carotid artery is more than 3 cm. CCP is located both in the central artery and continues in its branch. The LC is located only inside the CCP wall. 3.8) The length of the types V and VI atherosclerotic lesions in the arteries of the lower extremities more than 10 cm. CCP may appear after stent placement. The CCP was removed from the superficial femoral artery 2 weeks after stent implantation.
FC- Fibrous Cap; LC*- the lipid core is located not within the arterial wall, but within the wall of the CCP itself; OWP - outer wall CCP; St - stent.
Figure 3.1-3.8 Images courtesy of Dr. Mikhaylov I. Ph.D. in medicine. Leading vascular surgeon. Clinical Hospital of the Academy of Sciences in St. Petersburg [26].
Figure 3.10 Image courtesy of Natus Medical Incorporated, natus.com [28].
The scientific and medical literature doesn’t provide a description of the “transitional state” between ASL (IV) (small tubercle) [1-5] and ASL (V)(CCP) (tube in the form of a hollow cylinder [6-22,26-28], often without a “lipid core” [6,8-14,16-21,25[).
In case of ASL (IV), according to the current theory, macrophages should meet with low density lipoproteins (LDL) immediately behind the single layer endothelium. And it is here, in the intima, just behind the endothelium, that macrophage foam cells (MFC) should form, which then form LC with extracellular lipids [3].
Real histological sections ASL (I-IV) show the opposite arrangement of the LC and healthy intima. LC is located on the side of the intima opposite to the endothelium, the border with the middle layer of the artery. There is a region with a completely healthy intima between the LC and the endothelium. There are no signs of inflammation, damage, accumulation of LDL and macrophages in this area [1] (Figure 1.3).
Long-term inflammation causes stretch of the middle and outer walls of the artery. The “vasa vasorum” (VV) allows inflammatory cells, erythrocytes, and lipoproteins to penetrate into the arterial wall from the outer layer (Figure 1.3-1.6) [29,30].
The presence of a normal, non-inflamed intima between the MFC and the endothelium suggests that there is no penetration of macrophages and LDL from the side of endothelium. The concept is defined as an “outside-in” movement [31].
Therefore, the development of ASL (I-IV) does not depend on any way of the state of the endothelium, which means that ASL (I-IV) cannot in any way be associated with the processes occurring in the arterial lumen and cannot be connected with the development of ASL (V-VI) , which develops only in the arterial lumen.
Features and characteristics that create a false impression that the ASL (IV) and ASL (V)(CCP) types are similar to each other.
Coincidence 1
ASL (IV) and ASL (V)(CCP) always appear in the same places - carotid artery, cerebral arteries, heart, aorta and the lower extremities, but at the same time look different.
ASL (IV) (Figure 1):
- Looks like a tubercle protruding from the one side of the arterial wall [1]
- Limited by the LC length of a few millimeters [1]
- Always has an eccentric arrangement in the artery, and always stretches the middle and outermost layer on one side of the artery, blood is always pressed only against the opposite arterial wall [1]
- Always located in the outer part of the intima, at the border with the middle layer of the artery [1]
- Always has endothelium and healthy intimate part from the side of the arterial lumen [1]
- Never has fibrous cap (FC) [2]
- does not have a rigid structure that could retain its shape when removed from the artery wall, since there is a molten mass of extracellular lipids [1]
- luminal narrowing of artery does not occur until the LC occupies up to 40% of the potential lumen area within the wall [32] or until an 80% increase in external arterial size is achieved [33]
- ctive germination of VV [29,30]
ASL (V) (CCP) (Figure 2,3) in contrast, looks different:
- there is a long, soft, elastic, strong, solid, yellow tube in the form of a hollow cylinder located in the arterial lumen, have a concentric arrangement [6-22,26-28]
- has yellow color of surface, both inside and outside [6, 8-10, 12,14,16-21,26-28]
- Often has a homogeneous elastic structure without impurities, inflamed areas, areas of necrosis, bleeding and VV [6,8-14,16-21,25]
- When removed from the artery, retain its cylindrical shape and looks like “solidified silicone” [6,9-11,16,18-21,26-28]
- can exactly copy the contours of the branching of the artery [6,9-11,18-21]
- can be easily separated from the arterial walls without causing damage to it. The walls of the artery are always smooth and clean, without tubercles and infiltrations [6,9,11,12,16-21]
- can have any length - from a centimeter to tens of centimeters: the length in the carotid artery and heart vessels is more than 5 cm [6,8-11,13,19-21], in the lower extremities more than 10 cm [16,26]
- can have several layers which are superimposed on each other [7]
- Never has single-cell endothelium in the arterial lumen [1]
- Always has FC [1]
- may contain calcium deposits that do not extend beyond the normal size of the artery on X-ray examination [15]
- can be separated from the arterial wall with the help of ring-shaped instruments [16,17]
- is easily stretched in different directions with a balloon and fixed with a stent [8,26]
- During surgery can exfoliate into parts identical in structure and color without inflammation and necrosis [17,18]
- Many doctors call the CCP - “altered artery intima”[6,16,19]
- can have a strong structure of the outer and inner surfaces due to the numerous fibrotic fibers that form the FC and the fibrous layer between ASL (V-VI) and the artery wall [1,6,9-12,16,19-21,26-28]
- the outer wall can break away from the inner artery layer so that blood can flow between the ASL (V-VI) and the artery inner layer, forming a pathology - an arterial dissection, in contrast to ASL (I-IV), in which cannot be detachment of intima, since the intima near the ASL (I-IV) and in other places has a very small thickness (0,3-0,5mm) and weak structure and cannot physically maintain the blood flow for a long time, and also cannot be seen during research [12]
- During the surgery to remove ASL(V-VI), its “predecessor” - ASL(IV) is completely absent [6-22,26-28].
Coincidence 2
LDL are present in ASL (IV) and ASL (V) (CCP), but their quantity and distribution are different:
- ASL (IV) (Figure 1) there is a very small amount of LDL in the intima, close to the MFC. All LDL are absorbed by MFC. At the same time, there is no LDL between the MFC and the endothelium in the healthy intimate part [1]
- ASL (V) (CCP) (Figure 2,3) in contrast, is not connected with the intima, is located only in the arterial lumen, consists entirely of LDL. CCP, when it comes to the color and structure, looks like LDL in “xanthomas” with the familial hypercholesterolemia - dense, yellow, homogeneous mass [6,8-10, 12,14,16-21,26-28].
Coincidence 3
ASL (IV) and ASL (V)(CCP) always have macrophages, but their numbers and distribution are different:
- ASL (IV) (Figure 1), a small number of macrophages in the intimate part are located near the MFC. Macrophages that have become MFC are located near the LC. Only single macrophages are present in the healthy intima between the MFC and the whole endothelium (Figure 1.3) [1]
- ASL (V)(CCP) (Figure 2,3) in contrast, consists of LDL only. Macrophages accumulate in ASL (V)(CCP) wall only at the sites of random ruptures of the FC [13,14,26-28]. There is no presence of MFC in the artery wall in the area of ASL (V)(CCP) [6,9-11,16-19].
Coincidence 4
ASL (IV) and ASL (V)(CCP) might have LC, but in different places:
- ASL (IV) (Figure 1) - LC is located within the artery wall, in the intima, at the border with the middle layer. ASL (IV) always contains one LC - limited by length of a few millimeters (Figure 1.3) [1]
- ASL (V) (CCP) (Figures 2,3) in contrast, from the very beginning of ASL(V)(CCP) appearance LC may be completely absent. With “aging” and FC rupture, the lipid core is located not within the arterial wall, but within the of the CCP itself. The LC is removed together with ASL (V) (CCP) [13,26-28]. The artery walls near ASL (V) (CCP) doesn’t have LC [6,9-11,16-19].
Coincidence 5
ASL (IV) and ASL (V)(CCP) may mechanically overlap the arterial lumen, but ASL(IV) and ASL(V)(CCP) overlap the artery in different way:
- ASL(IV) (Figure 1), a dense tubercle, which has been growing for decades, is located on one side of the artery, has a limited length, is always eccentrically located in relation to the arterial lumen [1-5]
- ASL (V)(CCP) (Figures 2,3) in contrast, is a long, concentric in the form of a tube with a hole in the middle. the blood passes through a narrow passage in the center of ASL(V-VI) [6,8,11-14,16-19,26-28].
Coincidence 6
ASL (IV) and ASL (V)(CCP) may сover an artery due to blood clotting, but in different situations:
- ASL (IV) (Figure 1) do not cause blood clots in the arterial lumen - in case of ASL(IV), the unicellular endothelium is never damaged [1]
- ASL (V)(CCP) (Figures 2,3) in contrast, a blood clot is formed by rupture (erosion) of a thin TCFA (thin-cap fibroatheroma) above the LC [13,14,26-28].
Coincidence 7
ASL (IV) and ASL(V)(CCP) can theoretically be removed from the artery, but in practice only ASL(V-VI) are removed:
- While viewing the videos that were made during the removal of “ASL”, the author has never seen the removal of the ASL (I-IV)
- Absolutely all “ASL” removed during surgery refer to ASL (V-VI) type (Figures 2,3) [6,9-11,13,14,16-21].
The main conclusion that appears after conducting a study as to the difference between ASL (I-IV) and ASL (V-VI) is very simple: ASL (V-VI) have completely different structure and origin in comparison with ASL (I-IV).
Problems with etiology and pathogenesis
AS is considered a progressive chronic inflammatory disease [34,35] with systemic manifestations [36].
In practice, not “all” vessels are inflamed. ASL appear only in certain places of the vascular bed, and at the same time there are arteries and veins without ASL. This arrangement of ASL refutes the systemic nature of the process in AS and shows that absolutely all systemic factors (in the form of systemic inflammation, type 2 diabetes, smoking, the consumption of fatty foods, sedentary lifestyle, increased weight body, increase in the level of LDL) - cannot have an impact on the appearance and development of CCP.
Difficult hemodynamic conditions also cannot be described as the main reason for the formation of ASL. Healthy people also have such places, and also in a patient while he was still absolutely healthy.
There is a single factor that can connect specific sites in the artery and the rapid response of the artery to this factor. This can only happen when a pathological electrical signal arrives from the autonomic nervous system (ANS).
Acute, extreme stress can provoke acute, lethal myocardial infarction [37] or cardiac arrhythmia in very short periods of time. Above-mentioned diseases cold arise in people because of earthquakes [38,39], missile strikes [40], and football penalties broadcasted on television [41].
Pathogenesis of CCP formation
Pathological commands coming from the ANS cause artery compression in specific areas. The arterial lumen is narrowed to such an extent that only a small opening for the blood passage remains.
Taking into account that the artery has a circular shape - an obstruction, in case of artery compression, looks like a ring inserted into the arterial lumen.
Almost all blood cells can pass into the formed narrow opening, and only LDL, which have certain physical properties, enter the vortex regions in front of the constriction, and retain in the form of a ring (Figure 2.12).
When the first ring from the LDL is formed, a new vortex zone is also formed, which triggers the formation of a new ring from the LDL. The ASL(V)(CCP) follows the artery contours, in a few minutes, in case of strong artery compression, ASL(V)(CCP) of any length can be formed, and most importantly, it always has cylindrical shape (Figures 2,3).
The pressure on the artery wall in a narrow section (inside the CCP) is significantly smaller than it was before the CCP appearance, according to hydrodynamics [23-25]. Baroreceptors determine the decrease in arterial pressure (AP) and transmit incorrect information. The presence of CCP in the carotid sinus area causes persistent AP elevations.
Classification of CCP
The author proposes the following classification:
- Friable cylindrical cholesterol plaque (FCCP);
- Soft cylindrical cholesterol plaque (SCCP);
- Dense cylindrical cholesterol plaque (DCCP);
- Old cylindrical cholesterol plaque (OCCP);
Friable cylindrical cholesterol plaque (FCCP): the original form of CCP, in which LDL are accumulated in the form of a tube in front of obstruction, in case of arterial compression, but not yet attached to each other. When the artery spasm stops, the LDLs from FCCP can easily return to the vascular bed, this and ensures a “pathological increase in the level of LDL” in the blood [42].
Soft cylindrical cholesterol plaque (SCCP): If the vasospasm continues for a long time - the FCCP has not destructed. LDL are glued together by fibrous filaments. SCCP becomes completely similar copy of the artery wall. FC gradually forms between the LDL and the vascular bed. Blood flows inside the CCP and evenly moves away from the artery walls (Figures 2,3);
Dense cylindrical cholesterol plaque (DCCP): When the YCCP is inside the artery for a long time, the fibrous connection between the LDL is strengthened, the connection with the artery intima is strengthened, and the FC becomes tighter. Separation of the outer layer of the CCP from the inner layer of an artery may cause the artery dissection (Figure 2.4).
Old cylindrical cholesterol plaque (OCCP): Gradually, the part of the DCCP in which no necrosis or inflammation has occurred can gradually dissolve. The rest of DCCP transforms into eccentric ASL (V-VI) - with foci of necrosis, bleeding, emboli and blood clots. Later calcium crystals are deposited in these places, instead of LDL. All subsequent forms of ASL (V-VI), concentric and eccentric, are the result of the destruction of the original concentric structure of the CCP - ASL (V).
Conclusion
New theory explains, why during the surgery to remove ASL, artery wall can be absolutely healthy, explains how a concentric, long, soft, elastic, firm CCP with no LC and other lesions appears inside the artery. Explains why CCP has yellow, solid color on all sides and why it can be easily separated from the artery wall without bleeding in the artery wall. Explains how a person who has “factors” and “risks”, for decades can be absolutely healthy but eventually get to the hospital with vascular problems only after a nervous tension. It also explains why healthy people, who lead a healthy lifestyle, without bad habits, without “factors” and “risks”, also end up in the hospital with ischemic disorders [43].
Understanding the mechanism of pathological LDL increase in blood can help restore LDL levels in blood, by restoring ANS function and controlling vasoconstriction.
Preventing the formation of CCP in the vessels can prevent calcium deposits in the arteries and provide adequate nutrition to the limbs.
Control over vasoconstriction can be provided with drugs that prevent compression of the arteries, and also, it is possible, that control over vasoconstriction can be provided with specialized psychological help and drugs that restore the normal functioning of the CNS and ANS.
Conflict of interest
I, Rusanov Sergey, am the sole author of the manuscript.
- Stary HC, Chandler AB, Dinsmore RE, Fuster V, Glagov S, et al. (1995) A definition of advanced types of atherosclerotic lesions and a histological classification of atherosclerosis. A report from the Committee on Vascular Lesions of the Council on Arteriosclerosis, American Heart Association. Arterioscler Thromb Vasc Biol 15: 1512-1531. Link: https://bit.ly/2YdcpIW
- Stary HC, Chandler AB, Glagov S, Guyton JR, Insull W, et al. (1994) A definition of initial, fatty streak, and intermediate lesions of atherosclerosis. A report from the Committee on Vascular Lesions of the Council on Arteriosclerosis, American Heart Association. Circulation 89: 2462-2478. Link:
https://bit.ly/3ol5AQi - YouTube [Internet]. [Place unknown]: doctor image. Inflammation In Atherosclerotic Plaque Formation. Link: https://bit.ly/3obSDs6
- YouTube [Internet]. [place unknown]: azicareindonesia. [Video], Atherosclerosis Link: https://bit.ly/3CW2k1T
- YouTube [Internet]. [Place unknown]: CardioTabs. [Video], what is Plaque? Link: https://bit.ly/3F3fmg3
- YouTube [Internet]. [place unknown]: The Neurosurgical Atlas by Aaron Cohen-Gadol, M.D. [Video], Carotid Endarterectomy: Technical Pearls and Pitfalls. Link: https://bit.ly/3iiARiZ
- YouTube [Internet]. [place unknown]: TAUVOD. [Video], Eradication of Atherosclerosis. Link: https://bit.ly/3kPQJLB
- YouTube [Internet]. [place unknown]: Dr. Sandeep Burathoki. [Video], Carotid Artery Stenting video. Link: https://bit.ly/3m5yJfH
- YouTube [Internet]. [place unknown]: Alvin Wang. [Video], Carotid endarterectomy. Link: https://bit.ly/2YaVC9B
- YouTube [Internet]. [place unknown]: NSPC Brain & Spine Surgery. [Video], Carotid surgery. Link: https://bit.ly/3kS6LVs
- YouTube [Internet]. [place unknown]: Covenant Health. [Video], Carotid Endarterectomy. Link: https://bit.ly/2XV8Q9V
- Rаsslаivаûŝаâ аnevrizmа аorty (translation - “Aortic dissecting aneurysm.”) g. Krasnodar 06 09 12. Link: https://bit.ly/39Mf6U9
- Brinjikji W, Huston J, Rabinstein AA, Kim G, Lerman A, et al. (2016) Contemporary carotid imaging: from degree of stenosis to plaque vulnerability. Journal of Neurosurgery 124: 27-42. Link: https://bit.ly/2Y7cBcR
- YouTube [Internet]. [Place unknown]: The Austin Diagnostic Clinic (ADCHealth). [Video], You and Your Stent: Link: https://bit.ly/3zLkZvv
- Diagnosis of calcinosis of coronary arteries by multispiral computed tomography. Link: https://bit.ly/3ulNQoR
- YouTube [Internet]. [place unknown]: Galina Skokova. [Video], Endarterectomy; Link: https://bit.ly/3AVsrp5
- YouTube [Internet]. [Place unknown]: Tech Insider. [Video], Devices ‘eat’ bad cholesterol. Link: https://bit.ly/3AT0rCD
- YouTube [Internet]. [Place unknown]: Nejrokhirurgiya. [Video], Operatsiya - karotidnaya ehndarterehktomiya 2 (translation - “Operation - carotid endarterectomy 2”); Link: https://bit.ly/3ihaGt4
- YouTube [Internet]. [Place unknown]: Surgery Department. [Video], 1 Аngioplastika: stentirovanie podklûčičnoj arterii 2. Karotidnaâ èndarterèktomiâ (translation - “1. Angioplasty: stenting of the subclavian artery 2. Carotid endarterectomy”); Link: https://bit.ly/39MfCkZ
- YouTube [Internet]. [place unknown]: CTSNetVideo. [Video], Triple Coronary Endarterectomy in a Patient Undergoing CABG 2019 Link: https://bit.ly/3kSyGVf
- YouTube [Internet]. [place unknown]: CTSNetVideo. [Video], Coronary Endarterectomy of the Left Anterior Descending Artery. Link: https://bit.ly/3ARPvVM
- YouTube [Internet]. [place unknown]: UCLA Health. [Video], Carotid Artery Disease & Stroke Angioplasty - Dr. May Nour | UCLAMDChat. Link:
https://bit.ly/3iiPa7n - Galdin NS (2006) Osnovy gidravliki i gidroprivoda. Uchebnoe posobie (translation - “Fundamentals of hydraulics and hydraulic drive. Textbook”). Omsk: Sibirskaja gosudarstvennaja avtomobil’no-dorozhnaja akademija (SibADI); 145.
- Shterenliht DV (1984) Gidravlika (translation - “Hydraulics”). Moskva: Jenergoatomizdat 640.
- Chugaev RR (1982) Gidravlika (Tehnicheskaja mehanika zhidkosti) (translation - “Hydraulics (Technical fluid mechanics)”). Moskva: Jenergoizdat 672.
- YouTube [Internet]. [place unknown]: Surg Spot. [Video], Karotidnaya endarterektomiya: hirurgicheskoe lechenie kak profilaktika ishemicheskogo insulta (translation-“Carotid endarterectomy: surgical treatment as prevention of ischemic stroke”); Link: https://bit.ly/3ii9NAn
- File: Carotid Plaque.jpg Link: https://bit.ly/3igKkaq
- YouTube [Internet]. [place unknown]: Natus Neuro. [Video], Natus TCD Webinar: TCD Continuous Monitoring during Carotid Endarterectomy Surgery. Link: https://bit.ly/3BpPHfh
- Kockx MM, Cromheeke KM, Knaapen MW, Bosmans JM, De Meyer GR, et al. (2003) Phagocytosis and macrophage activation associated with hemorrhagic microvessels in human atherosclerosis. Arterioscler Thromb Vasc Biol 23: 440-446. Link: https://bit.ly/3og6U72
- Kolodgie FD, Gold HK, Burke AP, Fowler DR, Kruth HS, et al. (2003) Intraplaque hemorrhage and progression of coronary atheroma. N Engl J Med 349: 2316–2325. Link: https://bit.ly/2YczpI5
- Maiellaro K, Taylor WR (2007) The role of the adventitia in vascular inflammation. Cardiovasc Res 75: 640-648. Link: https://bit.ly/3unpWcL
- Glagov S, Weisenberg E, Zarins CK, Stankunavicius R, Kolettis GJ (1987) Compensatory enlargement of human atherosclerotic coronary arteries. N Engl J Med 316: 1371-1375. Link: https://bit.ly/3iiBrNH
- Zarins CK, Weisenberg E, Kolettis G, Stankunavicius R, Glagov S (1988) Differential enlargement of artery segments in response to enlarging atherosclerotic plaques. J Vasc Surg 7: 386-394. Link: https://bit.ly/2Y7cVs5
- Lucas AR, Korol R, Pepine CJ (2006) Inflammation in atherosclerosis: some thoughts about acute coronary syndromes. Circulation 113: e728-e732. Link: https://bit.ly/3id89zV
- Libby P, Theroux P (2005) Pathophysiology of coronary artery disease. Circulation 111: 3481-3488. Link: https://bit.ly/39LkxT8
- Fuster V, Moreno PR (2005) Atherothrombosis as a systemic, often silent, disease. Nat Clin Pract Cardiovasc Med 2: 431. Link:
https://go.nature.com/3CMCBsK - Connelly KA, MacIsaac AI, Jelinek VM (2004) Stress, myocardial infarction, and the “tako-tsubo” phenomenon. Heart 90: e52. Link: https://bit.ly/2Y16LsU
- Lowenstein CJ, Dinerman JL, Snyder SH (1994) Nitric oxide: a physiologic messenger. Ann Intern Med 120:227–237. Link: https://bit.ly/3kR2dhX
- Leor J, Poole WK, Kloner RA (1996) Sudden cardiac death triggered by an earthquake. N Engl J Med 334: 413-419. Link: https://bit.ly/2XWbw7o
- Kark JD, Goldman S, Epstein L (1995) Iraqi missile attacks on Israel. JAMA 273: 1208-1210. Link: https://bit.ly/3ARPIIy
- Witte DR, Bots ML, Hoes AW, Grobbee DE (2000) cardiovascular mortality in Dutch men during 1996 European football championship: longitudinal population study. BMJ 2000 321: 1552-1554. Link: https://bit.ly/3m7nAuX
- Rusanov SE (2017) The affection of the disturbance of the hydrodynamics of blood in case of stress on pathological increase of level of low density lipoproteins in blood. The formation of cylindrical plaques, and their participation in the development of acute ischemic disorders of heart and brain. Med Hypotheses 106: 61-70. Link: https://bit.ly/3m7B6yx
- Vernon ST, Coffey S, Bhindi R, Soo Hoo SY, Nelson GI, et al. (2017) Increasing proportion of ST elevation myocardial infarction patients with coronary atherosclerosis poorly explained by standard modifiable risk factors. Eur J Prev Cardiol 24: 1824-1830. Link: https://bit.ly/3F07ZWq
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
